Cataract
April 2023
by Ellen Stodola
Editorial Co-Director
Even with a successful cataract surgery, there are a variety of issues that can pop up postoperatively that can be problematic for patients, warranting further follow-up from the physician. Kevin M. Miller, MD, and Richard Tipperman, MD, discussed some of the most common issues that they see following cataract surgery and how to address them.
“While we may consider them minor nuisances, the patient’s perception is ‘What went wrong with my surgery?’” Dr. Tipperman said. “Surgeons should realize that the first thing they need to do is reassure and explain to the patient what’s going on and what we’ll do or not do about it.”
On a busy day, when you’re seeing a lot of patients and one of them tells you that their eye feels scratchy or they’re only 20/25 instead of 20/20, surgeons might discount everything as fine, while from the patient’s perspective, something went wrong with the surgery.

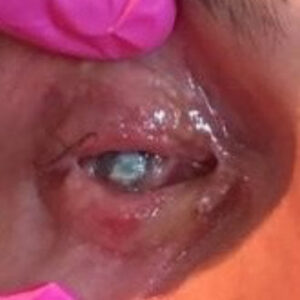
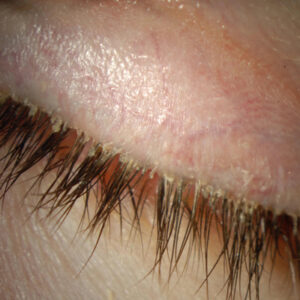
Source: Kevin M. Miller, MD
Of the issues that can come up postop, Dr. Tipperman said one of the most common he sees is corneal neuralgia and general complaints that “the eye doesn’t feel normal.” That could mean it feels big, small, uncomfortable, etc. After cataract surgery, the eye is irritated, and patients worry that there’s something wrong, even though for other surgeries, it’s normal to have swelling and postop effects.
Dr. Tipperman said that cataract surgeons recognize dry eye and the difference it can make. “I think 100% of patients get surface irritation that’s related to the betadine prep on the eye before surgery,” he said. “I tell them that this helps reduce risk of infection, but it also irritates goblet cells and the surface of the eye.” This short discussion helps calm the patient’s worries, he said.
Dr. Miller said another common source of dissatisfaction is small refractive errors. It’s not possible for surgeons to guarantee 20/20, but it’s important to tell patients you’ll do everything in your power to get the best result. “We can’t control where a lens will sit inside the eye; we can’t determine exactly how incisions will heal. But patients will wonder what went ‘wrong’ if their vision doesn’t turn out perfectly,” he said.
If there’s a small refractive error, the options for fixing it include glasses, contact lenses, and additional surgery. The additional surgery in Dr. Miller’s practice, in the cataract age range, is usually PRK, although sometimes he performs LASIK. “Less commonly, but for larger refractive errors, one might consider a lens exchange or a piggyback lens,” he said.
When addressing small refractive errors, timing is also a big factor. For example, he said that you don’t want to do PRK too soon because you want there to be refractive stability. He suggested waiting 3–6 months after surgery. But by that time, another problem is often kicking in, which is that the capsule starts wrinkling. Now you have a dilemma, Dr. Miller said, of how much of the problem is refractive error and how much is the capsule.
He will often wait to do a refractive touch-up until he’s opened the capsule. There are different challenges and expectations depending on which lens the patient had implanted. “When you implant a multifocal lens, you can be pretty sure the patient does not want to wear glasses,” he said. “Their expectations and the bar you have to exceed are higher.” Monofocal patients have often resigned themselves to wearing reading or computer glasses. “With a multifocal, it’s a little harder sell to put them into glasses, but I tell patients that if all you need is a little help for nighttime driving, let’s just do glasses.” It’s a much simpler option than more surgery.

Source: Kevin M. Miller, MD
Dr. Miller finds that a portion of his multifocal patients admit that they need a little help at nighttime and will use glasses, but there are some who don’t want to wear glasses for any scenario. “For those, we do laser vision correction,” he said. “In my location, among our premium services, we offer postop refractive enhancement as a service a patient can opt for.” He noted that patients do not have to sign up for this option, but it’s like an insurance policy. “Our standard cost for laser vision correction is $2,500 per eye,” he said. “If someone signs up for this insurance service, they pay $500. If they need or want laser vision correction after a cataract operation, they get it for $500.”
Dr. Miller noted that there are some surgeons who start to build a premium practice not thinking about what they are going to do when they encounter their first unhappy postoperative patient. They often feel they’ve been burned and don’t think it’s worth the effort. This is one reason why the device industry isn’t seeing much growth in the premium lens market, he said. If you have a strategy to deal with postoperative refractive errors and can get good results using that strategy, there’s no reason not to forge ahead.
Dr. Tipperman added that small residual refractive error can be incredibly frustrating to deal with for the surgeon and the patient. “The new generation formulas are good, and our techniques are good, but not every person gets to plano 20/20, and patients often cross cover each eye and compare them.”
There are some patients who you know preoperatively are going to be very particular, Dr. Tipperman said. “Those are people with whom I’ll have a more prolonged discussion about biological systems, healing, the lenses only coming in half D steps. … I tell them that ophthalmologists hate the word ‘perfect’ because it can’t always be achieved,” Dr. Tipperman said. He thinks those are patients in which the Light Adjustable Lens (RxSight) is a technology that you can offer them.
Other issues that can come up after surgery are capsular striae, wrinkles, and unwanted optical images. “The classic one is someone who has a capsular fold, and they see a light of 90 degrees to where the fold is,” he said, noting that he tells patients that this often resolves on its own. But if the patient is 12 weeks or so postop and still bothered, Dr. Tipperman will use a YAG laser.
Other patients might undergo cataract surgery and everything looks perfect, but they have significant glare and streaks of light in all directions postop, Dr. Tipperman said. “I see those patients treated with a YAG capsulotomy, and they’re always worse after that. I don’t think it’s well understood what causes the glare and streaking in otherwise perfect surgery.” Those patients are frustrated and think there’s some sort of defect with their lens, so it’s important to spend a lot of time with them. “I think if you do a YAG on those patients, you can make things worse because dysphotopsias become worse, and exchanging them becomes a bigger problem,” he said.

Source: Kevin M. Miller, MD
When having a discussion preoperatively with the patient, Dr. Tipperman noted it’s impossible to mention every single problem that can occur. However, for those patients who say they want to have “perfect” vision, Dr. Tipperman will reiterate that “we can only make it so good,” and if they’re not happy, there are ways to make it better.
Dr. Tipperman said he doesn’t normally discuss unwanted optical images unless the patient brings them up.
Depending on anterior chamber depth, you will see a much more obvious reflection off the IOL than off a natural eye, and Dr. Tipperman said patients often ask about this. Many have heard about this from a friend or relative. The reflection off someone’s eye after cataract surgery is different, and we can’t control it, he said, but if patients are concerned from an appearance standpoint, silicone IOLs are an option.
Dr. Miller agreed that he doesn’t discuss every problem that can occur with patients. “One of the pieces of the psychology puzzle in complication management is that every patient after surgery wants to know why you didn’t spend more time talking to them about the complication they experienced,” he said. “They don’t care about the ones they didn’t experience. All they care about is the one they did.” Dr. Miller mentions halos around lights for patients getting EDOF and multifocal lenses. He will describe what it looks like. Halos can be bothersome in the first month or two, but patients may stop noticing them after a few months. “When I see patients a year later, virtually no one complains of halos, and almost all can drive well at night and see street signs,” he said.
A pesky problem for ophthalmologists is when a patient comes into the office complaining of halos 3–4 months after surgery and there are wrinkles in the posterior capsule. You have to figure out if it’s the wrinkles or the lens design that’s causing the vision problem, he said, cautioning not to jump immediately to a lens exchange in these situations. Most times, opening the capsule fixes the problem.
Dr. Miller mentioned several other problems that he sees after cataract surgery, including EBMD, CME, ptosis, corneal neuralgias, multifocal IOLs that are not centered in the pupil, and irregular astigmatism.
He called CME “one of those things that haunts cataract surgeons.” It happens not infrequently in diabetics and patients with epiretinal membranes, but sometimes it happens in eyes that are totally normal. “When someone with any lens comes in a month after surgery saying, ‘My vision is blurry,’ and you look at the anterior segment and everything is clean, then you have to get an OCT or fluorescein angiography to see if there is CME,” he said.
Dr. Miller noted the importance of documenting ptosis prior to surgery. “I can’t tell you how many times patients don’t see themselves well in the mirror before surgery, and they don’t know they have a droopy eyelid or wrinkles on their face. If you don’t mention ptosis or wrinkles before surgery and they discover it after, they will wonder what went wrong,” he said.
Corneal neuralgias are an under appreciated problem. “The patient comes in saying they have an irritation or foreign body feeling,” he said. “You look carefully and everything seems perfectly normal, then they come in again and again complaining of the exact same thing.” Patients with this issue often go from doctor to doctor. Sometimes the neuralgias resolve on their own, he said, adding that he usually waits about a year to treat. “I’ll have them massage the area where the incision is to see if this helps to get the cut nerve or nerves to stop misbehaving. If it doesn’t after a year, I’ll take them back to the operating room and recut the incision,” he said. “I’ll recut the incision proximal to the original incision, deeper and wider so I make sure I transect every nerve that went through the original incision, and it’s like magic.” Dr. Miller called this issue a “diagnosis of exclusion,” adding that “you have to make sure nothing else is going on.”
When dealing with irregular astigmatism, Dr. Miller said it’s possible that there may be more irregularity to the cornea than previously known. You hope you pick this up ahead of time, he said, but it’s hard to predict the effect corneal irregularity will have on someone’s vision. “The 800-pound gorilla in the room is the cataract,” he said, adding that when you take the cataract out this could also impact the astigmatism, regular and irregular.
In terms of when he addresses some of these issues after cataract surgery, Dr. Tipperman said for refractive errors, he tells patients to wait for the prescription to be stable (around 12 weeks). If the patient is complaining that their eye is uncomfortable, irritated, or doesn’t feel right, Dr. Tipperman will do a normal staircase approach to dry eye.
People don’t realize that cataract surgery is surgery, he said, adding that it’s important to stress to patients that they’re still going through a healing phase following the procedure. “I think the most important thing is to maintain a good therapeutic relationship with the patient so that they know that you think their problems are important,” he said. “If they know that you’re going to stick with them and do everything you can to make them comfortable, it gives you a lot of mileage and time for most of this to get better.”
In terms of new technologies to help with some of these issues, Dr. Tipperman said the biggest improvement has been to IOL power formulas. It’s impressive how much better the newer formulas are than some of the older ones, he said, adding that this is an important message because some physicians are still using the older formulas in their practices.
About the physicians
Kevin M. Miller, MD
Kolokotrones Chair in Ophthalmology
David Geffen School of Medicine at UCLA
Los Angeles, California
Richard Tipperman, MD
Attending Surgeon
Wills Eye Hospital
Philadelphia, Pennsylvania
Relevant disclosures
Miller: None
Tipperman: None
Contact
Miller: kmiller@ucla.edu
Tipperman: rtipperman@oppdoctors.com