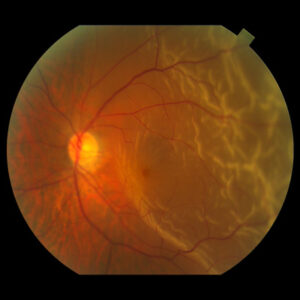
Cataract
Spring 2026
by Liz Hillman
Editorial Co-Editor
Oral sedation for cataract surgery has been used in some capacity for at least the last 20 years in the U.S. With the recent increase of office- based cataract surgery, which almost exclusively uses oral sedation, and general success seen with what’s considered an efficient, cost-saving, and, at times, safer sedation option, discussion has begun on whether oral sedation options could become the primary care model even within ambulatory surgical centers (ASC) or hospital settings where IV sedation is currently most common.

Source: Philadelphia Eye Associates
“This is important because it’s a change from the way most cataract surgeons have traditionally done cataract surgery. We’re used to IV sedation, and when you’re comfortable with something in a surgical setting, it’s hard to break out of your rut,” said Mark Lobanoff, MD, adding that he had a mild panic attack when he opened his office-based surgery suite, which just uses oral sedation, in addition to a topical or intracameral anesthesia to prevent pain. “I had never done cataract surgery with just oral sedation before. To my pleasant surprise, it works, and for the vast majority of patients, oral sedation is a superior method of sedation to IV.”
Reasons cited by Dr. Lobanoff include:
- The patient experience: With oral sedation there are no IV sticks, no need for a separate doctor visit to ensure physical health for safety of IV sedation, and no need for a 6–10 hour fast prior to surgery.
- Patient safety: Several studies support the safety of oral sedation in cataract surgery for the right patient.1–3 “A patient who’s calm, relaxed, pain-free but still in control of their cognitive functions, in my opinion, so far has been safer,” Dr. Lobanoff said.
- Efficiency: There are fewer preop logistics with oral sedation and a shorter postop recovery period. “With IV sedation, they have to be in recovery for a half hour. That slows the whole center down,” Dr. Lobanoff said.
- Cost: IV sedation and all that it entails is a greater cost to the medical system, he said.
Dr. Lobanoff is not alone in these opinions. Shahzad Mian, MD, also acknowledged benefits to oral sedation, including the fact that time can be saved in avoiding a pre-anesthesia health assessment. “We use a checklist of questions that helps us determine whether the patient can have the low-risk anesthesia and doesn’t have to go through a detailed evaluation, which was a precursor to transitioning over to oral sedation from IV because it is a lower-risk type of anesthesia for the patient, and therefore we don’t need as detailed of an evaluation,” he said.
There is also the benefit of not being dependent on availability of an anesthesiologist or certified registered nurse anesthetist (CRNA). “There’s a shortage of anesthesiologists and CRNAs.4 There’s not adequate coverage available for performing procedures,” Dr. Mian said.
Brad Feldman, MD, said he operates 50% of the time in an office-based surgical suite with oral sedation and the other 50% of the time in an ASC. When in the ASC, 99% of the time, he’s using IV sedation with an anesthesiologist or CRNA monitoring. The other 1% of the time, he’s using oral sedation for reasons like the patient forgetting to skip breakfast that day, inability to get IV access, or other reasons where oral sedation is simply deemed safer by the surgical team. “It’s gotten us out of trouble where we would have had to cancel cases,” Dr. Feldman said. “And the patients have all done well.”
Dr. Feldman said there doesn’t seem to be anything negative about the use of oral sedation in the right patient. “From a patient perspective, it’s easier, more comfortable, there are less hoops they have to jump through. They don’t need to see a primary doctor to be cleared for surgery unless that’s requested. There’s no preoperative testing besides what’s done in the ophthalmologist’s office. The day of surgery, the time that they’re there is shorter. It’s less invasive. The thing that hurts the most for cataract surgery is the IV needle being placed, so that doesn’t happen. From an insurance perspective, the insurer is not paying an anesthesiologist, a primary care physician, and a cardiologist for clearance. There’s a lot less cost to the system.”
But the question of whether oral sedation will become more mainstream is not just a matter of efficacy or economics. “In my ASC, we’re torn between competing forces,” Dr. Feldman said. Most ASCs employ an anesthesiologist and/or CRNAs, and they need to have enough cases to keep them busy, he said. “We have a minimum number of cases per day that we have to schedule in order to have an anesthesiologist. If we don’t meet it, they might cancel the day.”
In addition, for an ASC to switch from an IV-sedation model to a primarily oral sedation model would not be easy, Dr. Feldman said. Everything from the financial structure to the layout of the building, with multiple large staging areas, is geared toward a more costly, less efficient, and staffing heavy IV-sedation model in ASCs, he said.
Dr. Mian described a study that he was involved in that compared oral sedation to intravenous sedation in a large academic, hospital setting, evaluating efficiency and patient satisfaction for “simple” cataract surgery. The study, which was presented at major medical meetings but is not yet published in peer review, enrolled 188 patients, 54 of whom received the oral sedation.
According to Dr. Mian, there was no difference in procedure time or PACU time, though he noted there was a trend toward it being “a little bit shorter” for patients who received oral sedation. In terms of patient expectations, patient comfort, and nausea, there was no difference between the two groups. Dr. Mian also said there was no difference in patients saying they felt “out of it” in the postop period.
“The patients who got oral sedation did feel overall that they were a little more anxious than the ones who got IV sedation because they were more aware of what was happening. So there was a small difference there,” he added.
Patients were happy with both types of sedation, and Dr. Mian reported patients saying the most uncomfortable part of the entire surgical process was receiving an IV. In the study all patients received an IV, even if they were given oral sedation.
“Our results showed that, at least in our system, there was no downside to switching to oral sedation,” Dr. Mian said. “Patients felt just as safe, and they felt that they were comfortable during the procedure. In fact, there was the opportunity to get rid of the IV, which was the most uncomfortable part of the procedure.
“We also established that, for our system, it was an efficient process. It did not take more time, which was what we’re trying to show to our team—that it is a safe, effective, and efficient process, that IV sedation is not necessarily required for all patients,” Dr. Mian said.
Special considerations
While oral sedation in many cases does not require a CRNA or an anesthesiologist, Dr. Lobanoff said it’s incumbent on the surgeon administering the sedation and performing the procedure to make sure several things are monitored. “In preop we check everyone’s pulse, blood pressure, temperature. We make sure they’re within safe parameters. During the procedure itself, we’re monitoring heart rates. We’re watching the patient, making sure they’re breathing,” he said. “The patient is awake during the procedure, so you can communicate with them, ask how they’re doing. This is better for understanding what their medical condition is at that moment.”
If you’re operating in an office-based surgical suite with oral sedation, Dr. Lobanoff said the facility will have advanced cardiac life support (ACLS) available, and staff members will have passed ACLS training.
“You should be able to run a crash cart. A lot of docs say, ‘I haven’t done that in many years.’ But you can learn it. The number of times we’ve used it? Zero. But you need to be ready in the rare case it ever does occur,” Dr. Lobanoff said.
Even if there is a surprise during surgery, where a routine cataract procedure becomes complicated, Dr. Lobanoff said he’s still been able to manage the case with oral sedation. He described a case that ended up with a posterior capsule tear, requiring an anterior vitrectomy and other measures. The case took about an hour.
“What did we do? At the half-hour mark, the nurse put another half MKO Melt [midazolam, ketamine, and ondansetron, Imprimis] under their tongue, and we continued on as if nothing happened,” he said. “You certainly want to assess the patient, make sure they need it, but that’s the situation where you say, ‘I know the half-life of this drug. I know its time course. I know when we gave the first dose, and I know how the patient responded to that dose. Let’s give half the first dose,’ and that often covers the issue.”
Regardless of where you practice, Dr. Mian said patient safety comes first. There needs to be a system to screen patients and determine if they are truly routine and thus eligible for oral anesthesia. He also said that basic life support and airway management training is important. “Whether it’s due to the anesthesia or not, it’s imperative that you’re prepared to take care of them. Any member of the team who’s in the room should be familiar with the medications that the patients are getting and how to reverse the effects of those medications,” Dr. Mian said.
Also of note are global sedation practices, many of which don’t include any sedation for cataract surgery. Dr. Feldman said throughout his years working outside the U.S., he’s observed and participated in cataract surgery being safely practiced with limited to no anesthesia and without anesthesiologists or CRNAs.
“We’ve always had a traditional way of doing it in the U.S., which is anesthesiologists or CRNA and IV sedation. That’s been the model here for a long time,” he said. “But the experience and data from abroad shows that outcomes can be excellent without IV anesthesia.”
Types of oral sedation
Dr. Feldman said much of the oral sedation he’s using for cataract surgery is based on what he uses for refractive surgery: alprazolam or diazepam. These medications generally take 15–45 minutes to take effect, which Dr. Feldman said is convenient because that matches the timeframe for pupillary dilation.
There is also the MKO Melt. The ondansetron acts as an anti-nausea, and the ketamine acts as a dissociative, taking away perception of pain and relieving anxiety, Dr. Feldman said.
Younger patients, such as those in the refractive lens exchange group, Dr. Lobanoff said, usually require a full MKO Melt, while older patients having cataract surgery are generally given about 10 mg of diazepam. If a patient is still anxious after diazepam, Dr. Feldman said they will consider the addition of an MKO Melt.
Dr. Feldman said he’s done around 2,000 cases using oral sedation and hasn’t had to cancel a single case due to inadequate sedation. In addition, Dr. Feldman said he hasn’t had any complications due to over sedation with an oral sedative, while he has had complications occur during cases at the ASC due to over sedation with IV anesthesia.
When IV sedation is still necessary
The surgeons interviewed for this article all said there are cases where IV sedation is still preferred. These include the highly anxious patient, patients with more advanced medical problems, such as morbid obesity or respiratory issues, and patients whose cataract surgery is likely to be more complex.
Practicing at an academic medical center, Dr. Mian said a lot of their patients are not routine. “They have a history of trauma, or they have other health risk factors,” he said. “There are many different reasons why we need the ability to have more careful monitoring, more careful evaluation prior to surgery, and monitoring for their health overall during the surgery. The cases may also be longer.”
In addition to a more complicated medical history, Dr. Mian said more complex cases may need IV sedation. “But for routine cases, it certainly is reasonable to consider oral sedation, hopefully in the future sublingual sedation, which could have a faster onset and quicker recovery.”
“Do you need IV sedation for [routine cataract surgery]? You don’t. We’ve just been accustomed to it. Just because it’s what was offered before doesn’t necessarily mean it’s the best way forward,” Dr. Lobanoff said.
“Overall, oral sedation is a safe way to provide care, not just based on our small study, but based on other published studies and how people are practicing,” Dr. Mian said. “Again, I think making sure that we have appropriate training for the medications that are being used and appropriate screening for patients is important.”
About the physicians
Brad Feldman, MD
Philadelphia Eye Associates
Philadelphia, Pennsylvania
Mark Lobanoff, MD
OVO LASIK + Lens
St. Louis Park, Minnesota
Shahzad Mian, MD
Chair, Professor
Department of Ophthalmology and Visual Sciences
University of Michigan
Medical School
Ann Arbor, Michigan
References
- Chen M, et al. Oral diazepam versus intravenous midazolam for conscious sedation during cataract surgery performed using topical anesthesia. J Cataract Refract Surg. 2015;41:415–421.
- Hanna A, et al. Intravenous vs nonintravenous sedation for cataract surgery: systematic review and meta-analysis. J Cataract Refract Surg. 2025;51:723–730.
- Peeler CE, et al. Patient satisfaction with oral versus intravenous sedation for cataract surgery: a randomized clinical trial. Ophthalmology. 2019;126:1212–1218.
- Menezes J, Zahalka C. Anesthesiologist shortage in the United States: a call for action. J Med Surg Pub Health. 2024;100048.
Relevant disclosures
Feldman: None
Lobanoff: Alcon, Bausch + Lomb, iOR, Tracey Technologies
Mian: None
Contact
Feldman: bfeldman@phillyeye.com
Lobanoff: mlobanoff@gmail.com
Mian: smian@med.umich.edu