ONLINE EXCLUSIVE
Glaucoma
March 2023
by Liz Hillman
Editorial Co-Director
The first-in-human trial and data for suprachoroidal outflow enhancement using a novel micro-interventional technology and first-in-class biostenting approach developed by Sean Ianchulev, MD, MPH, was published online in January.
The study by Ianchulev et al. published in the British Journal of Ophthalmology described the use of “acellular scleral allograft bio-tissue microtrephined into a shaped supraciliary biostent.”1 Ten patients with open-angle glaucoma and cataracts underwent combined phacoemulsification cataract surgery with supraciliary biostent implantation intended to create reinforced and durable micro-interventional supraciliary outflow, the authors wrote.

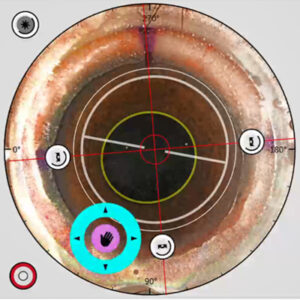
Source: Sean Ianchulev, MD, MPH
There are currently no MIGS devices or approaches physicians can use in clinical practice to address the suprachoroidal outflow after the voluntary withdrawal of CyPass (Alcon) from the market in 2018. At the 2022 Eyecelerator @ AAO meeting, Iqbal “Ike” Ahmed, MD, presented early information about Iantrek’s micro-interventional technology and supraciliary biostent approach. At that time, Dr. Ahmed, who is a co-author of this current study, said that the field learned from experience with first-generation MIGS devices and the importance of minimizing hardware risk to the endothelium—an advantage of the flexible, homologous bio-tissue matrix, which is soft, porous, non-lubricious, and conforms to surrounding ocular tissues by design. This addresses the key corneal health concern with “a soft implant with flexibility and appropriate, stable placement in the anterior chamber,” as EyeWorld Onsite reported from the meeting.
From the Ianchulev et al. published data, 12-month mean IOP was lowered 40% from baseline (24.2±6.9 mm Hg) to 14.6±3.2 mm Hg with the biostent, with 80% of patients achieving at least a 20% reduction in IOP. Glaucoma medication use went from 1.3 drops at baseline to 0.5 glaucoma drops at the 12-month postop visit—a 62% reduction, according to the study authors.
The investigators noted the anticipated phaco-associated 11% endothelial cell loss at 12 months. The implant was well tolerated, and vision with the combined cataract surgery improved from a mean BCVA of 20/130 to 20/36 at 12 months postop.
“We are encouraged by the results of this study and the potential of this new approach to provide viable and compelling solutions to surgeons and glaucoma patients,” Dr. Ianchulev, professor of ophthalmology, New York Eye and Ear Infirmary of Mount Sinai, New York, New York, and founder of Iantrek, said in the company’s blog post about the results. “We will continue to invest in research and development to leverage our micro-interventional technologies for ophthalmic surgery.”
Reference
- Ianchulev T, et al. Biotissue stent for supraciliary outflow in open-angle glaucoma patients: surgical procedure and first clinical results of an aqueous drainage biostent. Br J Ophthalmol. 2023. Online ahead of print.