Glaucoma: Complicated cases
December 2021
by Ellen Stodola
Editorial Co-Director
A patient may be at risk for a bleb leak after trabeculectomy, either in the early postop period or years after surgery. Meenakshi Chaku, MD, shared considerations for this potential complication, how she monitors patients, and what to do if a bleb leak does occur.
Dr. Chaku noted that the likelihood of a bleb leak occurring varies. Management of this issue would depend on when it occurs and if an infection is present at the time of occurrence. One of the most important things to do, she said, is to watch the patient for infection.
Occasionally, bleb leaks can occur early in the postoperative period, especially if the patient has poor tissue healing.
However, she noted that any glaucoma specialist could encounter a late onset bleb leak. It can happen for any patient with prior trabeculectomy, especially if the tissue is more ischemic and thinner over the surgery site. Thus, it’s important to check for evidence of a bleb leak each time patients with a previous trabeculectomy come into the clinic.

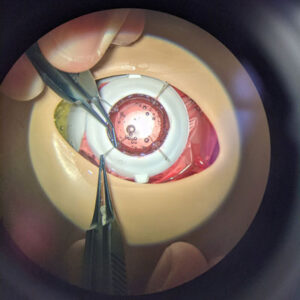
Source: New York Eye and Ear Infirmary of Mount Sinai
Comorbidities and considerations
In terms of specific comorbidities to be aware of that could increase the instance of a bleb leak after surgery, Dr. Chaku said to be cautious of patients with a thinner conjunctiva. Other risk factors include older age, previous history of inflammation, or long-term use of topical hypotensive medications, which can decrease tissue quality over time. When performing the trabeculectomy, Dr. Chaku said the way you open the conjunctiva also plays a role. A limbus-based approach tends to have less chance of a bleb leak than a fornix-based approach because it’s more posterior.
Additionally, she mentioned that the use of an antimetabolite, like mitomycin-C, could increase the risk of poor healing and bleb leak, but it is necessary to help in the success of the surgery. The problem, she said, is “we want patients to heal at their surgery site, but we don’t want them to scar down. We want a functioning bleb; that’s why we use mitomycin-C, but using it puts them at a higher risk later on for bleb leaks.”
Dr. Chaku said that if surgeons are using sponges for mitomycin-C administration, she recommends making sure they’re more posterior and not touching the edge of conjunctiva that you’re going to close with at the limbus. Dr. Chaku has experience using sponges for mitomycin-C administration but also uses injection of mitomycin-C to administer the antimetabolite more posterior.
Physicians should make sure to have a good conjunctival closure to prevent any leak. Dr. Chaku likes to use a running mattress suture when she closes a trabeculectomy to make sure the closure is tight. She also suggested using a thinner vascular needle so it doesn’t create a suture track during the closure. This is especially helpful if the conjunctiva is delicate and thin.
Making sure to educate patients about this potential complication and advising them to do their best not to rub their eyes is key. “You can’t always identify a patient who may have poor wound healing later on, but it is important to make sure they know what to look out for,” Dr. Chaku noted. She will educate patients to look for redness, tearing, pain, and their vision getting worse.
Management of leaks
Dr. Chaku said management of a bleb leak can be complicated in some cases. “Any time you have a bleb leak, make sure you’re covered with antibiotics,” she said, adding that you want to make sure there is no risk of infection.
If you see this in the early postop period, depending on how big the leak is, it may be possible to manage conservatively to help in conjunctival scarring. If the patient is on topical steroids, you could decrease the frequency to aid in scarring down the trabeculectomy sooner. A bandage contact lens or an older generation antibiotic that can cause scarring are other conservative measures that can be used. “The problem with a bleb leak early postop after surgery is that we want [the patient] to scar faster because of the leak, but you don’t want them to scar too much where they’re not going to function well later on,” Dr. Chaku said. Some patients may need a revision in the OR if the leak is significant, if the pressure is low, or if there is concern for infection. Dr. Chaku noted that other approaches include using autologous blood to help with scarring or tissue glue.
Often a bleb leak in the later postop period may need a revision back in the operating room. However, it is possible to handle these cases conservatively, Dr. Chaku said, referencing a case she handled where the patient didn’t want to go back to the OR, and he finally healed with a conservative approach and never developed an infection.
But if it’s a big leak and a thin, ischemic bleb, it’s better to consider a surgical revision. “Surgical revision of a late bleb leak can be difficult because it depends on how big the bleb is,” Dr. Chaku said. “You have to excise all the ischemic tissue and advance the healthy tissue to close it. If it’s a large area involved, it can be hard to get enough tissue to close it.”
This requires a broad dissection because you have to take away all the tissue that is leaking and try to find as much healthy tissue as possible. There are a number of approaches if you need to pull down the conjunctiva if additional tissue is needed.
Additionally, Dr. Chaku said that a patch graft may be used if the ischemic tissue is removed and the scleral flap has melted. “Sometimes I have placed a scleral patch graft on certain patients and always have one available for my revisions in case it is needed.”
While Dr. Chaku noted that she’s been fortunate enough to be able to close the tissue in all of her cases of bleb leaks, others have used amniotic membrane as a potential solution. It is always good to have additional tissue readily available when returning to the operating room in these cases.
Dr. Chaku stressed the importance of speaking to the patient about the potential for intraocular pressure rising after surgery, requiring treatment. They may need surgical intervention again, so it’s important to warn all patients.
Dr. Chaku advised monitoring patients for infection and to act quickly if there is a concern for an active process. When an infection occurs, these patients are at high risk for vision loss and blindness so it’s always important to have high surveillance. Until trabeculectomies are no longer done, there will always be a risk for this complication, she said.
About the physician
Meenakshi Chaku, MD
Associate Professor of Ophthalmology
Loyola University Medical Center
Maywood, Illinois
Relevant disclosures
Chaku: None
Contact
Chaku: MEENAKSHI.CHAKU@lumc.edu