Glauoma: Complicated cases
December 2021
by Liz Hillman
Editorial Co-Director
Malignant glaucoma is a rare complication, but it’s still something surgeons need to be on the lookout for after surgery, especially in the early postoperative period.
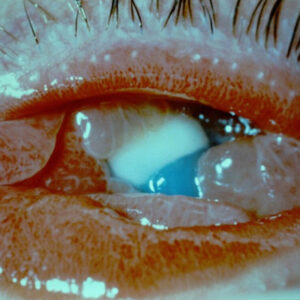
Amenze Oriaifo, MD, defined malignant glaucoma as “uniform shallowing or flattening of both the central and peripheral anterior chambers in an eye with normal to elevated intraocular pressure despite one or more patent iridotomies.”
“It’s also known as aqueous misdirection, ciliary block glaucoma, and lens block angle closure,” she said.


Source: Amenze Oriaifo, MD
Lindsay Foley, MD, and Joseph Panarelli, MD, said in an email to EyeWorld that “malignant glaucoma involves an alteration in the normal anatomic relationship among the lens, ciliary body, anterior hyaloid face, and vitreous.”
“Whether aqueous is actually misdirected into the posterior chamber is still being debated,” they said. “However, all proposed mechanisms seem to involve abnormal vitreous fluid flow, resulting in fluid buildup behind the vitreous and creation of a significant posterior to anterior pressure gradient. This gradient drives the vitreous, lens, and iris forward, which further reduces vitreous permeability, creating a vicious cycle resulting in angle closure.”1,2,3
Dr. Oriaifo estimated that this complication occurs in 2% to 4% of eyes undergoing surgery for angle closure glaucoma. Drs. Foley and Panarelli cited published research that estimated prevalence of malignant glaucoma after angle closure surgery between 0.6% and 4%.1,4,5 Dr. Oriaifo said she’s only seen it a handful of times during training and her years in practice. Dr. Oriaifo said that while malignant glaucoma can happen at any time in the postoperative period, most cases occur shortly after the incisional surgery. Drs. Foley and Panarelli noted that it’s most commonly associated with trabeculectomy and tube shunts (the latter less commonly), but it has also been reported after cataract surgery, surgical iridectomy, pars plana vitrectomy, diode laser cyclophotocoagulation, bleb needling, and even laser iridotomy.
“Trying to get ahead of it by recognizing risk factors early and planning out the surgery accordingly is key,” Dr. Oriaifo said.
Know the risk factors
First and foremost, Drs. Foley and Panarelli said that if a patient developed malignant glaucoma in one eye, they’re likely to have it happen in the other.
“Therefore, if a patient presents with poor vision in one eye due to complications from surgery, it is critical to get old records before proceeding with surgery in the better eye,” they said.
Factors that increase the risk of malignant glaucoma occurring, according to Dr. Oriaifo, include hyperopia, chronic angle closure with plateau iris configuration, nanophthalmos, or a history of malignant glaucoma in the fellow eye. She also said women are three times more likely than men to develop malignant glaucoma due to smaller eyes.
Drs. Foley and Panarelli offered similar risk factors: history of angle closure with peripheral anterior synechiae, axial hyperopia, small eyes, and female gender.6,7
Mitigating the risk
Drs. Foley and Panarelli said there are a few ways to try to prevent malignant glaucoma.
“The simplest and most conservative approach is to immediately start an agent such as 1% atropine sulfate and continue it for several weeks to months after the surgical procedure,” they wrote.
In eyes with an axial length less than 20 mm, which Drs. Foley and Panarelli said are at especially high risk, they will perform prophylactic iridozonulohyaloidectomy from an anterior or posterior approach. They said the patient in this case should be pseudophakic or undergoing concurrent cataract surgery.
Dr. Oriaifo said approaches to get ahead of malignant glaucoma, in order of effectiveness, are prophylactic vitrectomy, prophylactic iridozonulohyaloidectomy, anterior vitrectomy, sclerotomies, posterior capsulorhexis, ECP, and goniosynechialysis.
Malignant glaucoma occurs—now what?
Drs. Foley and Panarelli said that in order to diagnose malignant glaucoma, the patient must already have a peripheral iridotomy. “This allows the clinician to rule out angle closure due to pupillary block,” they said.
From there, the next step is to start medical therapy with mydriatic-cycloplegic agents. These, they explained, tighten the zonules to pull the lens posteriorly. Drs. Foley and Panarelli noted aqueous suppressants, hyperosmotic agents, and topical steroids as helpful to reduce aqueous production, decrease the volume of the vitreous, and reduce inflammation.
“Medical treatment alone has been shown to be effective in about 50% of patients within 5 days (though some of these patients may actually have annular choroidal effusions and not true MG),” they said.
If medical treatment is not successful, the next step would be laser treatment, according to Drs. Foley and Panarelli, explaining that the idea is to create a passageway between the anterior chamber and the vitreous space. An Nd:YAG laser can disrupt the anterior hyaloid face, they said, noting that it’s often most successful if the laser is placed outside the optic of the IOL, where the anterior and posterior capsular leaflets are fused.
Laser photocoagulation of the ciliary processes is another potential option, Drs. Foley and Panarelli said. This can help reduce the abnormal anatomic relationship between the ciliary processes and the anterior hyaloid face.
If both medical and laser treatments fail at resolving the issue, they said iridozonulohyaloidectomy with core vitrectomy is required. This procedure would create an uninterrupted passageway from the anterior chamber to the vitreous cavity that is needed to truly make the eye unicameral. Drs. Foley and Panarelli advised use of a depot steroid injection in these patients because they often develop significant intraocular inflammation.
“The prognosis of malignant glaucoma depends on the severity of the attack and is often guarded, but if diagnosed and treated early, the prognosis can be good,” Drs. Foley and Panarelli said.
About the physicians
Lindsay Foley, MD
Resident
Department of Ophthalmology
New York University Langone Health
New York, New York
Amenze Oriaifo, MD
Central Texas Eye Center
San Marcos, Texas
Joseph Panarelli, MD
Associate Professor
Department of Ophthalmology
New York University Langone Health
New York, New York
References
- Chandler PA, et al. Malignant glaucoma. Medical and surgical treatment. Am J Ophthalmol. 1968;66:495–502.
- Quigley HA. Angle-closure glaucoma—simpler answers to complex mechanisms: LXVI Edward Jackson Memorial Lecture. Am J Ophthalmol. 2009;148:657–669.
- Shahid H, Salmon JF. Malignant glaucoma: a review of the modern literature. J Ophthalmol. 2012;2012:852659.
- Simmons RJ. Malignant glaucoma. Br J Ophthalmol. 1972;56:263–272.
- Lowe RF. Malignant glaucoma related to primary angle closure glaucoma. Aust J Ophthalmol. 1979;7:11–18.
References continued - Debrouwere V, et al. Outcomes of different management options for malignant glaucoma: a retrospective study. Graefes Arch Clin Exp Ophthalmol. 2012;250:131–141.
- Razeghinejad MR, et al. Lesser anterior chamber dimensions in women may be a predisposing factor for malignant glaucoma. Med Hypotheses. 2005;64:572–574.
Relevant disclosures
Foley: None
Oriaifo: None
Panarelli: Aerie, Allergan, CorneaGen, Glaukos, New World Medical, Santen
Contact
Foley: Lindsay.Foley@nyulangone.org
Oriaifo: amenzeosa@gmail.com
Panarelli: Joseph.Panarelli@nyulangone.org