Cataract: YES Connect
Spring 2025
by Ellen Stodola
Editorial Co-Director
The landscape of surgical training is evolving at an unprecedented pace. While in-person residency remains a critical foundation for skill development, the rise of digital tools has expanded the way ophthalmologists learn and refine surgical techniques. Social media and online platforms have broadened access to education, bringing world-class training within reach for surgeons everywhere. Advanced simulation tools, virtual reality operating rooms, and artificial intelligence (AI) are redefining how trainees gain experience and confidence. With a blend of traditional and virtual methods, the next generation of ophthalmologists can now access comprehensive, immersive training that was once unimaginable.
As a surgeon, I rely heavily on the foundation I obtained during my residency and fellowship training. Yet, I continue to grow and evolve by learning from other skilled surgeons online, exploring innovative techniques, and staying current with the latest advancements in our field.
Ashraf Ahmad, MD, YES Connect Guest Editor
New tools in surgical training are constantly improving teaching methods. In this YES Connect column, several physicians discussed digital tools for surgical training and how these fit in with more traditional training approaches.
Surgical training is undergoing a revolution, said Omar Krad, MD. “While residency remains the cornerstone, the landscape is expanding beyond traditional programs to publicly accessible platforms like YouTube and Instagram. The internet has democratized higher education, making specialized surgical skills more accessible than ever before,” he said. “Previously, aspiring surgeons often had to travel long distances, even internationally, for advanced training. Today, the internet has effectively placed the world’s expertise into a single, global classroom, transforming how surgeons learn and develop their craft.”
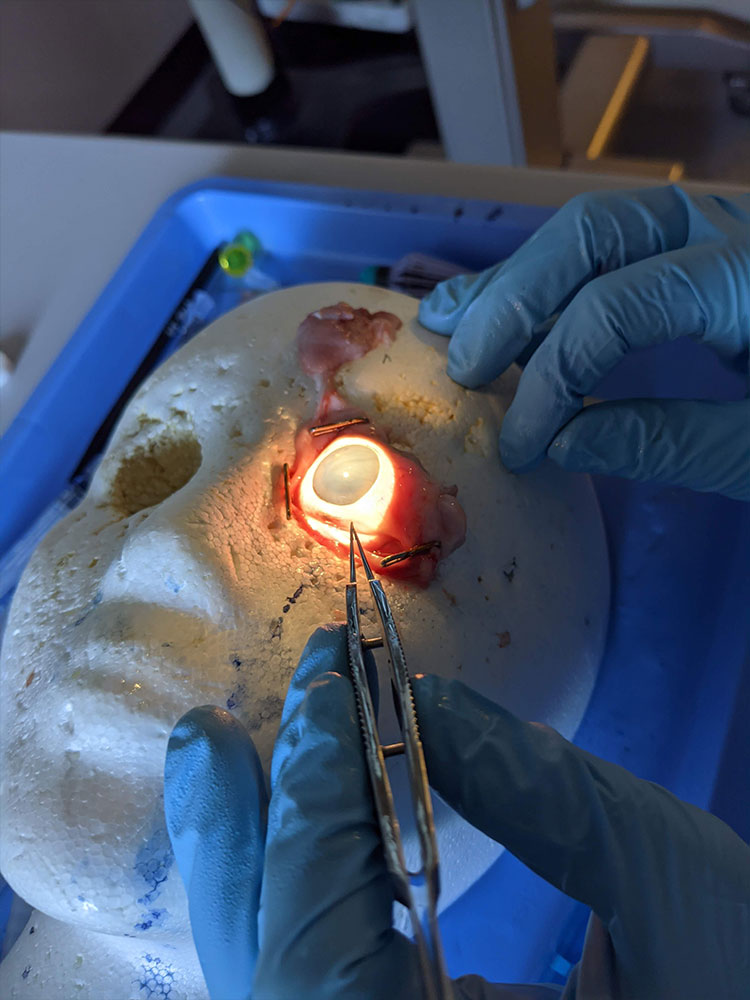
Source: Anthony Chung, MD
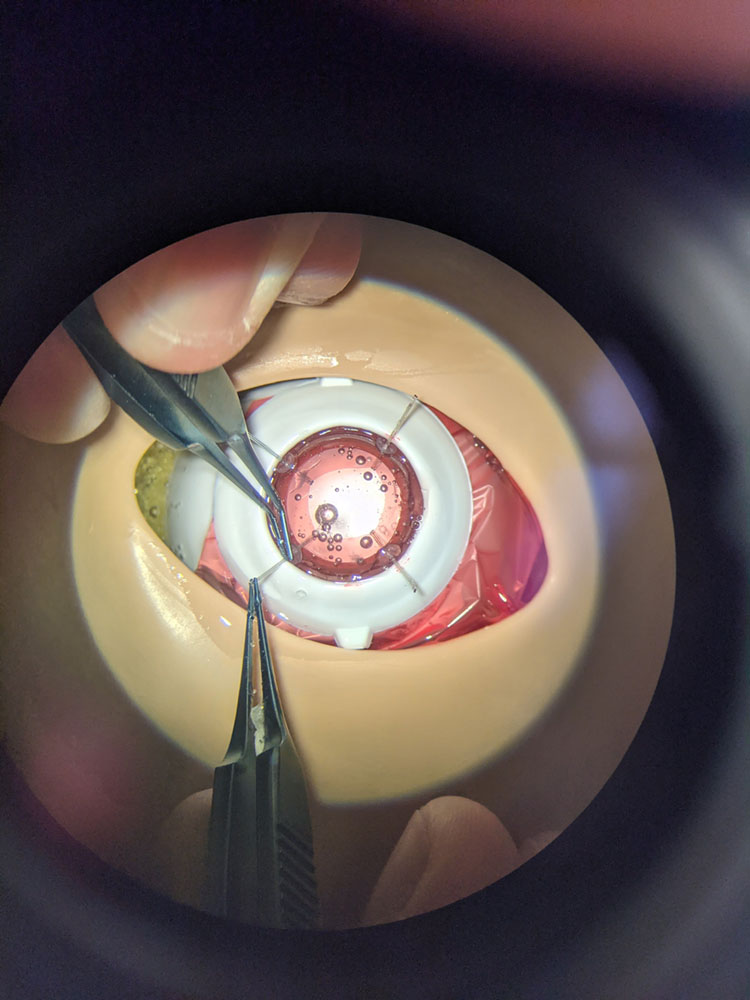
Source: Anthony Chung, MD
He added that although the necessary technology has been available for years, its impact on surgical training was initially limited by a scarcity of online content. “Fortunately, this landscape is shifting dramatically,” he said. “More and more surgeons are embracing online platforms to share educational content, enriching the learning experience for their peers.”
Anthony Chung, MD, said there are a number of simulation tools available in ophthalmology. He noted the Eyesi (Haag-Streit). “We’ve integrated these types of technologies thoroughly in the field,” he said.
Since Dr. Chung has been in practice, he said that the recent trend has been to get more immersive and use virtual reality headsets to create a 3D world that you’re sitting in virtually.
“I trained at a time when this has been commonplace for residents to have virtual reality,” Dr. Chung said. The extent to which these tools are integrated in each program is varied quite a bit, he said, but he added that many programs have these simulators as part of the curriculum to gain experience.
Jaclyn Haugsdal, MD, also noted some of the available virtual simulators. She mentioned that the Eyesi has been around the longest, and there are newer simulators being developed, such as those from HelpMeSee, Fidelis (Alcon), and FundamentalVR. Some of these are manual small incision cataract simulators, such as HelpMeSee and FundamentalVR, whereas Eyesi and the Fidelis are more in line with phacoemulsification simulation.
One of the best features of virtual simulators is the repetition, Dr. Haugsdal said. “They usually are easy to set up and clean up, and it’s easy to get in many repetitions in a short timeframe without using additional resources or supplies. For beginners, the simulators provide realistic enough feel to help develop the basics of surgical techniques. With the benefit of easy repetition, they can be an excellent resource.” Simulators are also great at teaching hand positioning, moving in the eye, and maintaining centration.
Dr. Krad said that in-person residency training is essential for establishing a strong foundation in ophthalmology. “However, my attendings emphasized the importance of lifelong learning, noting that many procedures they currently perform weren’t part of their own residency training,” he said. “While a solid foundation is crucial, digital tools can be incredibly effective for skill development post-residency. Without that strong initial foundation, though, there’s a greater risk of misinterpreting online content and potentially hindering one’s growth.”
Dr. Krad said the journey to becoming a proficient surgeon involves building procedural familiarity, developing muscle memory, and gaining confidence. Each repetition, whether in a wet lab, online, or in a virtual environment, helps to reduce a trainee’s anxiety and bolster their confidence, ultimately leading to improved performance under pressure, he said. “A comprehensive training strategy that integrates these diverse learning modalities is essential for supporting the growth of future surgeons.”
Dr. Chung said that digital tools like this are more of a self-directed learning option. “Because it’s self-directed, it can be like a video game,” he said. “You learn on your own and learn how to play the system, but whether or not that system is creating good habits for surgery is another thing.” He said that using these simulators also requires proper guidance when you’re first learning to ensure you’re using the right techniques.
Speaking about the pros and cons of virtual simulators vs. traditional simulation, Dr. Haugsdal again mentioned that virtual simulators are easy to set up and clean and allow for repetition. They are also good at teaching hand positioning, moving in the eye, and maintaining centration. But they may come with a cost or space issue and could be missing a more realistic feel. A more traditional simulation approach (like with pig/cow eyes or with artificial eye models) could be more realistic and could use actual surgical equipment and instrumentation. But resources could be limited, making repetition difficult, and the use of biological material requires proper handling and cleaning.
Many surgical simulators focus on cataracts, but Dr. Chung added that some have vitreoretinal modules on them, too. While these are unique ways to learn, Dr. Chung also believes in the combination of both virtual and traditional learning methods working together. “You need to be in front of patients and learning from the patients while doing your due diligence and practicing outside the OR,” he said. “I think all of these simulation techniques out there are supplemental to the traditional method of operating with the attending.” Anecdotally, Dr. Chung said he will often tell residents that the motion they use when performing the procedure is not terribly different from what he uses, but the difference he notices is the time taken in between each motion.
Dr. Chung added that the wet lab is a passion of his, and he hopes there comes a time when wet lab curriculum is more standardized among programs. This will help define the progression and place of where these tools fit together with other training, he said.
When commenting on whether virtual training options could grow to replace traditional ophthalmic training, Dr. Krad again stressed that traditional in-person training is crucial for establishing a solid foundation in surgery. “Without this foundational training, the effectiveness of virtual learning is significantly diminished. Only with a strong foundation can one fully leverage the benefits of virtual training resources,” he said.
The rapid growth in virtual and augmented reality technologies holds immense potential for surgical training and collaboration, Dr. Krad continued. “These advancements could enable trainees and practicing physicians worldwide to participate remotely in training sessions, experiencing them as if they were physically present. Imagine being able to virtually assist in any surgery from your home office. During a lunch break, for instance, one could virtually scrub in and observe a retina, cataract, or cornea specialist through the assistant scope. Interactive features, such as live Q&A with the surgeon, could further enhance the learning experience. This technology has the potential to dramatically improve access to specialized surgical training, benefiting both ophthalmologists and patients worldwide.”
Training programs equipped to provide top-tier surgical education have a unique opportunity to elevate the standard of care within their communities, Dr. Krad said. “By extending their educational resources virtually to practicing ophthalmologists, they can foster a culture of continuous learning and collaboration. The technology to livestream or post recordings of grand rounds and notable cases is readily available. Embracing this opportunity to share knowledge will ultimately translate to improved patient outcomes.”
Dr. Haugsdal finds that these newer simulation options complement the more traditional training approach. “The virtual simulators and traditional simulation models each have their benefits,” she said. “The simulators may be better for more beginner level education of a technique, whereas traditional approaches could be more helpful for advanced techniques.”
She added that some newer technology that is in development is the use of AI to analyze recorded surgical videos to assist with surgical education. “This could be used to determine inefficiencies in surgery or track trends in surgical time of individual steps or whole surgeries, or even to compare trainee videos to expert videos to determine areas that deviate from expert level,” she said. “This technology could be used as an additional surgical teacher or mentor to help provide feedback to the trainee on their actual surgical videos.”
In terms of new and future technologies and applications, Dr. Chung noted the quest to try to get more objective data from surgery itself. This will help to show the steps and where there’s room for improvement, he said, adding that AI/machine learning could potentially help evaluate objective data in the future.
About the physicians
Anthony Chung, MD
Assistant Professor
University of Washington School of Medicine
Seattle, Washington
Jaclyn Haugsdal, MD
Clinical Assistant Professor
University of Iowa
Coralville, Iowa
Omar Krad, MD
Eye Associates of Orange County
Mission Viejo, California
Relevant disclosures
Chung: None
Haugsdal: None
Krad: None
Contact
Chung: atchung5@uw.edu
Haugsdal: jaclyn-haugsdal@uiowa.edu
Krad: omarkrad@gmail.com