Browse articles on EyeWorld.org. EyeWorld is the award-winning member publication of ASCRS. The magazine provides news and updates from the Society as well as clinical features in the areas of cataract, refractive, cornea, glaucoma, and practice management. It publishes quarterly with editorial direction from its medical editorial board and staff.
It’s important to address underlying conditions prior to cataract surgery, and dry eye is one such condition. Physicians must identify and treat it to ensure the tear film is optimized and measurements are correct.
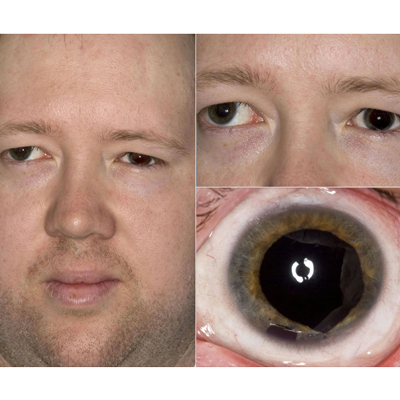
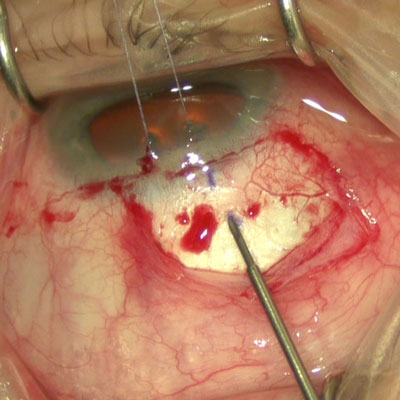
There are several companies in the field of artificial irises. Kevin M. Miller, MD, and Sathish Srinivasan, MD, discussed the available products and important considerations when working with artificial irises.
With the COVID-19 pandemic temporarily closing practices around the country, many ophthalmologists had to figure out how to still communicate with and treat their patients. Several physicians commented on how the pandemic has affected their dry eye patient population and trends they have seen.
A retrospective study based on insurance claims data is giving real-world insights into prescribing/treatment patterns for two dry eye medications—cyclosporine ophthalmic emulsion (Restasis, Allergan) and lifitegrast ophthalmic solution (Xiidra, Novartis).1 In doing so, researchers can make inferences on adherence, discontinuation, and more.
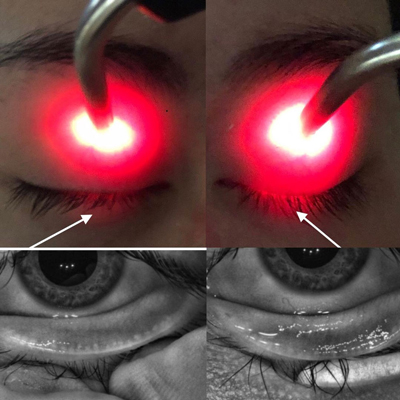
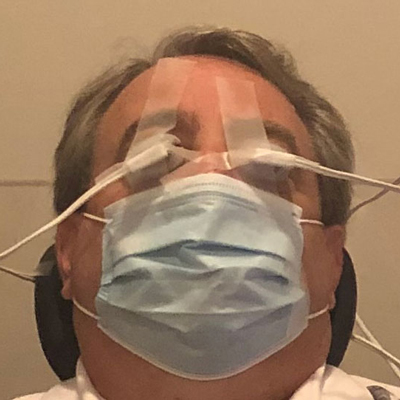
This 20-year-old college student with meibomian gland dropout and lid seal insufficiency had dry eye complaints. The student reported long computer hours, poor sleep, poor nutrition, excessive contact lens wear, and use of multiple over-the-counter and prescription acne treatment products.
Source: Laura Periman, MD
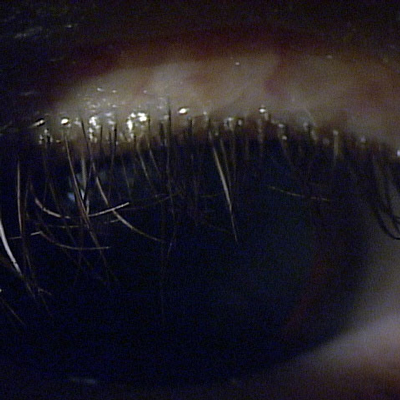
When teens come into the clinic, it’s important to consider that they might have dry eye or meibomian gland disease. Investigators in a recent study found that among minors coming in for eye exams, 15% were experiencing dry eye discomfort and 9% had signs of meibomian gland dropout, according to lead investigator Anna Tichenor, PhD.1
The COVID-19 pandemic has affected all areas of medicine, including eye banking. While much more is known about SARS-CoV-2 and the illness it causes, there are still several unknowns that continue to be investigated as they pertain to the safety of donor tissue.

Nathan Radcliffe, MD
Glaucoma Editor
As I write this, we are in the ninth month of the COVID pandemic, and each day brings a record number of new cases in the third wave of the virus. As a glaucoma specialist in New York City, my practice has surely seen some ups and downs over the past year. We have had to adapt tremendously, and perhaps now is a good time to reflect on some of these changes.
Where do drops fit in the era of interventional glaucoma—a time when there are new technologies, new drug delivery systems, and several MIGS options?
Depending on what you define as a microinvasive glaucoma surgery (MIGS), you might think it first became available several decades ago with endocyclophotocoagulation (ECP), but many define the MIGS era beginning with the iStent (Glaukos), the first ab interno trabecular microbypass device approved by the FDA in 2012.
Difficult patient conversations—frequent or few and far between—are a part of any medical career, but preparing for those conversations is not generally part of medical training.