Cornea
December 2013
by Frederik Raiskup, MD, PhD, FEBO
The success of any surgical intervention depends as much on postoperative care and management as it does on the surgical procedure itself. This undoubtedly also holds true for corneal crosslinking. At our hospital, we have been performing corneal crosslinking with the IROC illumination system (IROC Innocross, Zug, Switzerland) since the development of the first prototype and continue to use the latest UV-X 2000 crosslinking device. Through my experience with this system, I have come to understand that careful management of ocular surface health after surgery is essential for the successful and rapid visual rehabilitation of the patient and to minimize complications. Patient counseling is also equally important to prepare the patient for the potential side effects of the procedure and ensure that he/she is receptive to the postoperative management protocol and any interventions that may be necessary in case of side effects and eventual complications.
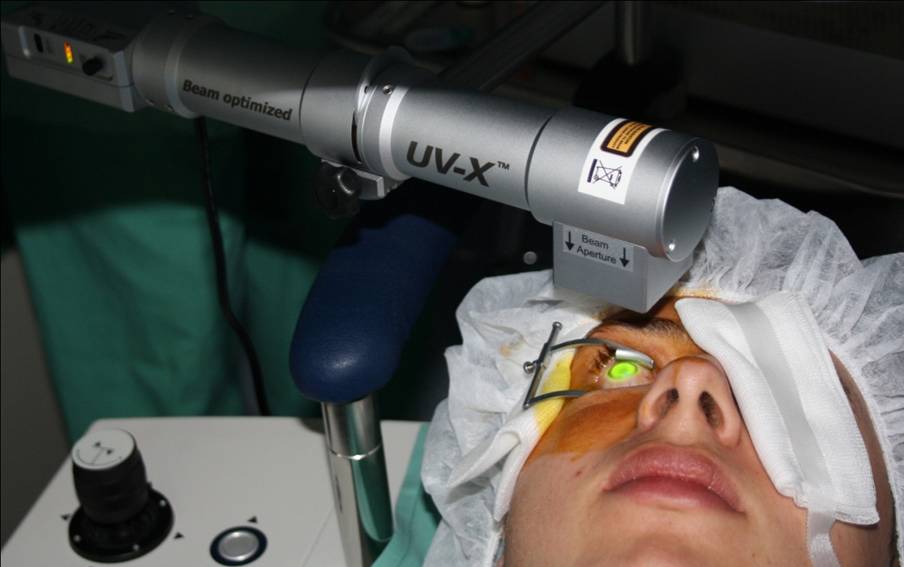
Source: Frederik Raiskup, MD
The essentials of postoperative management
The focus of postoperative management after corneal crosslinking is to restore a healthy ocular surface as quickly as possible. There are three main aspects to post-crosslinking patient management: 1) hastening re-epithelialization, 2) preventing infection, and 3) reducing pain.
The first of these, re-epithelialization, is the most important. The current crosslinking standard protocol requires de-epithelialization of the cornea before the administration of riboflavin solution. This is done in order to ensure that a sufficient amount of riboflavin enters the stroma. Therefore, it is important to restore this protective barrier of the ocular surface as quickly as possible after surgery. This not only helps to improve the patient’s comfort and visual acuity more rapidly after surgery, but it also reduces the risk of infection.
The epithelial layer serves to protect the cornea from micro-organisms and other environmental factors that could damage the stroma. Even small lesions in the epithelium can increase the risk of infection or melting, the consequences of which can be serious. There have been reports in the literature of microbial keratitis and stromal melting leading to the development of deep stromal scars and loss of visual acuity postoperatively, or in the worst cases, corneal perforation necessitating a corneal graft. Therefore, controlling infection after crosslinking is a priority.
Pain management is also an important aspect of postoperative management that ensures patient’s comfort. De-epithelialization of the cornea, a densely innervated and hence very sensitive tissue, causes some amount of pain. However, proper counselling of patients about the level of pain that can be expected after surgery and the use of common analgesics is an effective strategy to control pain.
Postoperative management protocol
We use a standard protocol in our department for the postoperative management of all corneal crosslinking patients. Soon after surgery, all patients receive a soft contact lens. The function of this lens is two-fold. First, it supports epithelialization, and second, it reduces pain. We also put all patients on topical antibiotics to prevent infection. We prescribe preservative-free quinolones (ofloxacin) three times a day until epithelialization is complete. At the same time we use preservative-free ocular surface lubricants to promote epithelialization.
Once re-epithelialization is complete, we remove the contact lens and discontinue the antibiotics and begin a steroid regimen for three weeks. I prescribe dexamethasone three times a day, however, fluorometholone is also commonly used. The steroid serves primarily as an anti-inflammatory agent and prevents the development of corneal scars. In treating crosslinking patients it is important to use preservative-free eye drops as preservatives can interfere with re-epithelialization.
If a patient complains of mild pain, I recommend using a non-steroidal anti-inflammatory drug, such as ibuprofen. In rare cases, patients whose pain threshold is very low or who are particularly sensitive to pain may complain of severe pain after crosslinking. In such cases I prescribe a strong painkiller from the group of centrally acting opioid analgesics.
Complications of and special considerations for corneal crosslinking
Although corneal crosslinking is a relatively safe procedure, some side effects and complications have been reported after the procedure. These range from minor side effects such as haze and sterile infiltrates to more serious complications such as corneal infection, stromal melting leading to perforation, or the development of deep stromal scars.
Among my patients, the most major complication has been infection. However, in my experience, severe infections tend to occur in patients who have other concomitant debilitating conditions (e.g., neurodermitis and diabetes mellitus) that predispose their ocular surface to infections and a prolonged epithelial healing process or in patients who suffer from diseases demanding long-term systemic steroid therapy (e.g., neurodermitis, asthma). For instance, one of the more severe complications that I have seen involved a patient who showed a prolonged delay in epithelial healing; the epithelium did not heal for several weeks following surgery, and he developed a secondary central microbial infiltrate. However, this patient also had neurodermitis that was being treated with systemic steroids. This likely increased his risk for prolonged healing and infection. In this case, I used several antibiotics to treat the infection. Even after the infection was treated and the inflammation had subsided, the epithelial defect was still present, for which I had to apply an amnion membrane. The lesion healed with a deep stromal scar. Therefore, ophthalmologists may need to take special precautions with patients who have neurodermitis or dry eyes, those who are taking systemic steroids because of other concomitant diseases, as well as those who are diabetic as they may have slower epithelial healing and be more prone to infection.
Another consideration that ophthalmologists should take into account when performing crosslinking is with respect to pregnant women, who are at risk of progression of keratoconus during this period. An experience with a patient of mine who was pregnant at the time of crosslinking and who developed an infection postoperatively alerted me to the potential risks of performing crosslinking in such patients. Fortunately, in this case I was able to control the infection with topical antibiotics; in cases of severe infections, systemic antibiotics or further surgical procedures, possibly under general anaesthesia, may become necessary to rescue the eye. However, these interventions can harm the fetus. Therefore, pregnant women with keratoconus should be well counselled about the possibility of keratoconus progression during pregnancy and the risk of prolonged epithelial healing, infection, and stromal melting following crosslinking and perhaps be advised to undergo surgery after delivery.
Another potential complication that can occur in some patients is a deep corneal scar. Again this tends to occur more commonly in patients with a predisposition, such as those with thin corneas and high keratometry readings. We have found that treating these patients with hypo- osmolar riboflavin solution instead of iso-osmolar riboflavin solution can reduce the risk of developing corneal scars.
I have seen sterile infiltrates as a sign of an immunological reaction in some of my patients. They are usually found subepithelially in the corneal periphery, separated from the limbus by a clear zone of the cornea. However, they often disappear within a few weeks of topical steroid treatment.
Haze has been reported as a minor side effect of crosslinking. However, this haze needs to be differentiated from the haze that is seen after refractive excimer laser surface ablation. Haze after corneal crosslinking is very faint and usually disappears with topical steroid treatment. Yet in some patients, even several months after surgery, fine haze can persist but usually only affects the crosslinked area. Such haze does not interfere with visual acuity and most likely occurs as a result of structural changes in the crosslinked tissue.
Ensuring good outcomes after crosslinking
We have found that the new optimized beam profile in the latest UV-X 2000 device achieves better outcomes and more efficient flattening than other UV illumination systems. Whereas with the previous top-hat beam profile most of the effect of crosslinking is seen at the center of the treated corneal tissue, with the new optimized beam profile we are able to achieve a greater volume of crosslinked tissue at the periphery of the irradiated area, and thus more uniform flattening across the cornea. We have verified with anterior segment optical coherence tomography that the demarcation line is parallel to the epithelial surface of the crosslinked area even in the periphery when using this new optimized beam profile.
Patient counseling is essential for successful treatment
An essential factor in helping patients follow their postoperative regimen is patient counseling, both before and after surgery. The majority of my patients do not have much difficulty following their postoperative regimen. However, this is because I spend time with them both before and after surgery to ensure that they have reasonable expectations from the procedure. It is important to inform patients that they will likely experience some pain, photophobia, tearing, and red eye after the procedure and that they will have to follow a course of antibiotics, ocular surface lubricants, and steroids so that they are not taken by surprise after surgery. Recommendations as simple as wearing sunglasses for the few days following surgery to counter photophobia can also go a long way in the postoperative management of crosslinking patients.
Good postoperative patient care and management are indispensable for achieving good treatment outcomes and patient satisfaction after corneal crosslinking. Awareness of the potential side effects and complications of corneal crosslinking, a strong focus on re-establishing ocular surface health, and patient counseling both before and after surgery are key strategies for improving visual outcomes, patient recovery, satisfaction, and comfort after crosslinking.
Editors’ note
Dr. Raiskup is a senior consultant, cornea, external diseases and refractive surgery unit, Department of Ophthalmology, Carl Gustav Carus University Hospital, Dresden, Germany, and associate professor of ophthalmology, Department of Ophthalmology, Faculty of Medicine, Hradec Králové, Charles University, Prague, Czech Republic. He has no financial interests related to this article.




