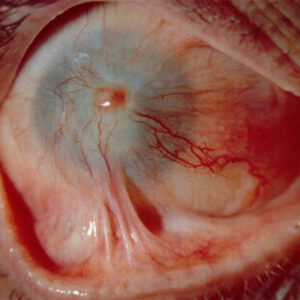
Refractive: Complicated cases
December 2021
by Liz Hillman
Editorial Co-Director
A patient unhappy after LASIK—thankfully, as Neda Nikpoor, MD, put it, there are not many. LASIK was established by the PROWL studies1 as safe and effective with a high level of satisfaction, but there are patients who are unhappy with their outcomes, though rarely. Why this happens and how to best manage these patients is what Dr. Nikpoor, Ella Faktorovich, MD, and Thomas Clinch, MD, shared with EyeWorld.
More than 95% of participants in the PROWL study were satisfied with their vision after LASIK. According to analysis by the FDA, some patients developed problems after the procedure, including visual disturbances such as starbursts, glare, halos, or severe dry eye. The studies found that less than 1% of patients had difficulty performing their usual activities due to any symptoms that developed postop.
Source: Neda Nikpoor, MD
Reasons for unhappy patients
Dr. Nikpoor said she could think of less than a handful of patients who were unhappy after LASIK. One was a man in his early 40s who was beginning to experience the symptoms of early presbyopia. She had offered to leave him a little myopic in his non-dominant eye, but he chose to see perfectly at distance in both eyes. His distance vision postop was good, and he could still read J1-plus uncorrected, but he said it felt more difficult to see near. “You could tell that he was struggling to deal with the fact that he was 40 now, and this was unmasking that,” she said.
Dr. Nikpoor said she has had a couple of patients experience “rainbow glare.” Evidence suggests that the majority of these cases diminish with neuroadaptation over time, and Dr. Nikpoor and her partner Alan Faulkner, MD, have found that to be true in their experience. Dr. Clinch said he has had this experience, too, and time resolves most cases of rainbow glare. He also said pulsed doses of topical steroids can be effective.
Another side effect that could result in an unhappy patient is dryness. Dr. Clinch said patients with dryness preoperatively should be treated and counseled that it could get worse during the postop period, as should patients who spend a significant amount of time looking at screens. He said physicians should look for lagophthalmos and counsel these patients about the potential for greater dry eye and the need for postop artificial tears.
If a patient were to have higher order aberrations, which Dr. Clinch identifies with the WaveLight Topolyzer Vario Diagnostic Device (Alcon), he has performed Contoura (Alcon) treatments on post-LASIK patients to reduce aberrations. The physician needs to explain to the patient that treating higher order aberrations can have variable outcomes. He usually advises against treating higher order aberrations if the patient’s procedure was done a long time ago and they’re functioning reasonably well. Dr. Nikpoor noted that she will set the appropriate expectation by telling patients it may take two or three treatments to achieve the final result.
“Time tends to heal a lot of the aberrations in both that the cornea will respond and the brain tends to neutralize some of the aberrations,” Dr. Clinch said.
Dr. Faktorovich shared the reasons she finds for unhappy post-LASIK patients. There are patients whose outcomes don’t align with their expectations. A good example of this is when a patient with mixed astigmatism also has significant accommodation, she said.
“We can operate on MRx, but their vision will worsen over the years as they lose their accommodation. Or we can operate on CRx and they will be nearsighted initially. In this case, they may need to do vision therapy,” Dr. Faktorovich said.
Dr. Clinch said he’s a big proponent of mild monovision in the pre-presbyopic, myopic patient. From an expectations standpoint, he said hyperopic patients need to be counseled preop that their convalescent period might be longer and they might experience nighttime visual disturbances for a longer period of time compared to their myopic peers. Highly myopic and/or myopic astigmats also could have a longer convalescent period, and they should be told they might need a touch-up.
Other unhappy patients, Dr. Faktorovich said, are those who feel like the surgeon doesn’t have time for them or is dismissive or defensive. There are also patients who may need help understanding what’s normal during the healing process, she added.
“If they don’t understand, it could be upsetting. If they do, they are reassured. If there is a plan of action to maintain a good healing process, that’s even better. Some symptoms are a normal part of the postoperative healing. With modern screening, techniques, and technologies, they are unlikely to persist. Be supportive, systematic, caring,” she said.
Dr. Nikpoor agreed and shared a particularly challenging case. She had a patient with severe neuropathic pain after PRK and saw her frequently for several months. “I reiterated at every visit that her pain was real and that I was committed to helping her get through this. She joined a Facebook support group and thanked me for taking her pain seriously. She shared that many members of the group were frustrated by their experience with their surgeons who dismissed them,” she said.
What do you do?
If you do find an unhappy post-LASIK patient in your chair, Dr. Nikpoor said she starts with a data collecting phase where she’s trying to figure out what they’re happy and unhappy about with their vision.
“I repeat back what I hear to make sure I’m understanding them correctly. Then I’ll go through the possible solutions for each thing they’re unhappy about,” she said. “At the end of that conversation I’ll ask, ‘If you did this again, would you make the same decision?’ A lot of times they say, ‘Oh, yes.’ I try to leave it on that positive note. They’ll usually say that in spite of the negatives, it has made their life better. I also want to know for my own sake that they would have chosen the same procedure.”
The unhappy patient is the one whose calls you should be returning right away, Dr. Faktorovich said. After listening to them, she says, “I can totally understand what you’re saying” and “I am committed to helping you.”
Once you’ve identified what’s causing their discontent, spend time explaining what’s going on so they understand. Dr. Faktorovich said she doesn’t dumb down her explanations; she finds patients understand and appreciate when she takes the time to explain what’s going on in technical terms. If a patient’s vision is blurry,
do a refraction and demo even the smallest prescription in a trial frame. Dr. Faktorovich said this will reassure the patient, even if they don’t decide to do a touch-up procedure.
Dr. Faktorovich advised involving a significant other in conversations with the patient, if the patient agrees, and she gives her cell phone number to all patients.
Ensuring happy patients
Dr. Nikpoor said her practice has a lot of capital equipment for preop testing that she finds helpful in assessing and optimizing the ocular surface. Her practice doesn’t require a contact lens holiday before screening, but if at screening there are signs of an abnormality, scans are repeated at their preop appointment. Dr. Nikpoor said they put patients on loteprednol 3 days before their preop appointment because it cleans up the ocular surface for good refractions and topography. If there is any question about epithelial conditions, she’ll get an epithelial map. If the topography is suspicious for subclinical keratoconus, she’ll do PRK.
Dr. Nikpoor advised ICLs for patients who are higher myopes, in cases where the stromal bed would be pushed to less than 300 microns, and where there would be more than 40% tissue altered with a cornea-based procedure.
Preoperatively, Dr. Faktorovich looks for things like slight inferior steepening on the topography that could be a sign of either forme fruste keratoconus or epithelial basement membrane dystrophy (EMBD). She performs epithelial thickness mapping with widefield OCT to help differentiate between the two conditions. She steers patients with forme fruste keratoconus toward a lens-based procedure and patients with EBMD toward PRK.
Dr. Faktorovich said she’s not afraid of steering patients away from surgery altogether. These patients often have good vision with contact lenses or glasses, and they expect great vision without these aids after. She tells these patients preoperatively about the healing process and what that could entail as well as the rare complications that could happen.
Dr. Faktorovich said to not rush the preop process, tailor it to the patient’s specific prescriptions and ocular findings, and consider having them come in for several visits.
About the physicians
Thomas Clinch, MD
Eye Doctors of Washington
Washington, D.C.
Ella Faktorovich, MD
Pacific Vision Institute
San Francisco, California
Neda Nikpoor, MD
Aloha Laser Vision
Honolulu, Hawaii
Reference
- Eydelman M, et al. Symptoms and satisfaction of patients in the Patient-Reported Outcomes With Laser In Situ Keratomileusis (PROWL) studies. JAMA Ophthalmol. 2017;135:13–22.
Relevant disclosures
Clinch: Alcon
Faktorovich: None
Nikpoor: None
Contact
Clinch: Thomas.Clinch@edow.com
Faktorovich: ella@pacificvision.org
Nikpoor: drneda@alohalaser.com