ASCRS News: ASCRS/EyeWorld Journal Club
September 2021
by Hetal Ray, MD, Wendy Linderman, MD, and Jessica Chow, MD

Residency Program Director
Yale Eye Center
New Haven, Connecticut
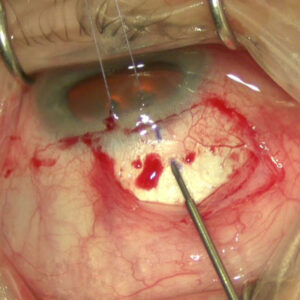
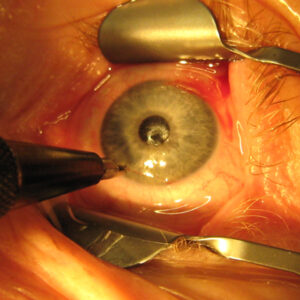
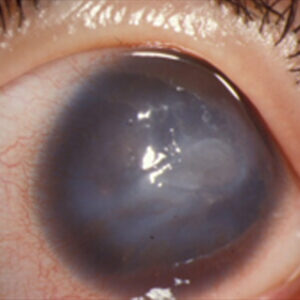
Glaucoma is a leading cause of blindness worldwide.1 Adequate lowering of IOP remains the mainstay of glaucoma treatment. Prior to 2012, surgical management of glaucoma consisted primarily of trabeculectomy and glaucoma drainage implants. Since 2012, minimally invasive glaucoma surgeries (MIGS) have been developed to lower IOP by bypassing the trabecular meshwork for mild to moderate glaucoma. MIGS boasts faster recovery, lower impact on leisure activities, and a greater safety profile compared to traditional glaucoma filtering surgeries. However, reported complications of MIGS include decreased vision, IOP elevation, hyphema, corneal edema, device movement, and need for reoperation. This paper is the first of its kind to describe short-term postoperative complications in eyes after minimally invasive glaucoma surgery.
Design

Ophthalmology Resident
Yale Eye Center
New Haven, Connecticut
This was a retrospective case series studying postoperative complications in the 90 days following MIGS procedures. Data was collected at a single tertiary care center over a 6-month period. The procedures included in the study were iStent (Glaukos), iStent inject (Glaukos), Hydrus (Ivantis), OMNI (Sight Sciences), gonioscopy-assisted transluminal trabeculotomy (GATT), and XEN (Allergan). The primary outcomes of the study were reoperation rates and indications within a 90-day period following MIGS procedure. Additional data included details of intraoperative and postoperative complications, time to reoperation, and outcomes at 1 month following reoperation.
Results
There were 448 MIGS procedures included in the study. Twenty-three eyes underwent reoperation. Patients who underwent reoperation had a mean age of 70, were predominantly female, and most often had moderate to severe glaucoma.

Ophthalmology Resident
Yale Eye Center
New Haven, Connecticut
Sixteen of the 23 eyes that underwent reoperation had the XEN, 4 iStent/iStent inject, and 3 goniotomy/GATT/OMNI. Therefore, all types of MIGS except Hydrus were represented in the group of eyes that required reoperation, though the sample size of patients undergoing Hydrus was small (8 patients).
There was a statistically significant higher rate of reoperation in the XEN group. Eleven of the 16 eyes that required reoperation after XEN were implanted in an ab interno fashion.
The most common indication for reoperation was elevated IOP. The XEN group also had bleb-related indications for reoperation including exposure, wound leak, and early encapsulation. The most common reoperation performed in the XEN group was needling with an antifibrotic agent. A few eyes required major procedures such as a second XEN, trabeculectomy, or glaucoma drainage device. In the iStent group, 2 eyes required IOL repositioning or secondary IOL implantation related to cataract surgery complications and 2 eyes required XEN. In the angle-based group, 3 eyes required trabeculectomy. In all groups, average time to reoperation was 39 days, with a range of 4 to 82 days.
Postoperative results following reoperation were encouraging. Following reoperation, there was a statistically significant reduction in IOP, improvement in visual acuity, and decrease in number of IOP-lowering drops at postoperative month 1. Across groups, there were no visually devastating complications in the 90-day postoperative period.
Summary
The 90-day reoperation rate for MIGS in this study was 5.3%. The most common indication for reoperation was elevated IOP. If elevated IOP is excluded as an indication for reoperation as in prior studies, the reoperation rate for MIGS in this study was 1.6%. This rate is lower than the 90-day reoperation rate of 2.5–3.1% for traditional glaucoma surgeries reported by Chu et al.2
The XEN group had a statistically significant higher rate of reoperation rate of 10.5%. Reoperation was more common with the ab interno approach. The most common indication for reoperation with XEN was high IOP, which is similar to other MIGS, but this group also had bleb-related indications for reoperation. Of these, 2.6% required reoperation for implant exposure or wound leak. This can be compared to a rate of tube exposure of 1.6% and rate of wound leak of 1.8% in the immediate postoperative period.2

Source: Yale Eye Center
Discussion
The ASCRS Journal Club panelists highlighted the large number of MIGS procedures performed by a diverse group of surgeons as two great strengths of this study.
Given this study’s retrospective nature, there was no standardized protocol among the study groups. Medical and surgical decisions were individualized to each patient and surgeon. Only interventions performed in the operating room were included in this study. In particular, this study excluded in-office needling and likely underestimated the rates of needling in the XEN group.
This study’s focus was on the 90-day postoperative period, and therefore did not offer insight into late-term complications that may occur. Other studies have also looked at longer-term outcomes following MIGS. In a retrospective study, eyes were followed 1 year after XEN implantation, and 6% had transient hypotony, 10% had 2 or more Snellen lines lost, and 16% required a second glaucoma procedure regardless of ab interno or ab externo approach.3 In a prospective study of eyes with cataract and mild to moderate primary open angle glaucoma, Hydrus implantation reduced the probability of incisional glaucoma surgery from 3.9% to 0.6% in a 3-year period as compared to cataract surgery alone.4 One large randomized study of 152 eyes compared Hydrus and iStent and found a statistically significant decreased reoperation rate (0 versus 3.9%) and reduced medication use in the Hydrus group.5
The panelists in the ASCRS Journal Club pointed out that even in cases of recently diagnosed, mild glaucoma, a percentage of patients will progress to severe disease. This is exemplified by the LiGHT study, in which 1.8% of ocular hypertension patients required a traditional glaucoma surgery within 3 years despite no evidence of glaucomatous damage at presentation.6 In the future, MIGS may be offered to ocular hypertensives as early surgical options to decrease risk of progression to advanced disease. More long-term outcomes data is needed to further analyze the safety profiles among the MIGS procedures and compared to traditional glaucoma surgery.
The authors published the first study of short-term reoperation rates after MIGS. True to its definition, MIGS has a favorable safety profile compared to traditional glaucoma surgery. The XEN group had the highest rate of reoperation. MIGS continues to emerge as an important surgical option for eyes with glaucoma.
Reoperation for complications within 90 days of minimally invasive glaucoma surgery
Wesam Shamseldin Shalaby, MD, Joseph Bechay, BS, Jonathan Myers, MD, Daniel Lee, MD, Reza Razeghinejad, MD, Natasha Nayak Kolomeyer, MD, L. Jay Katz, MD, Aakriti Garg Shukla, MD
J Cataract Refract Surg. 2021;47(7):886–891.
Purpose: To describe reoperations that occurred within 90 days of minimally invasive glaucoma surgery (MIGS) at a single institution over a 30-month period.
Setting: Tertiary care hospital.
Design: Retrospective case series.
Methods: Charts of adult patients who underwent trabecular microbypass stents, gel microstents, and goniotomy procedures (including gonioscopy-assisted transluminal trabeculotomy) from October 1, 2017 to March 15, 2020 at Wills Eye Hospital were examined. Outcome measures were unanticipated reoperations within the first 90 days after MIGS procedures and the complications that led to these reoperations.
Results: 448 MIGS procedures were performed on 436 eyes of 348 patients over a 30-month period by 6 glaucoma surgeons. Of these, 206 (46.0 %) were trabecular microbypass stents (198 iStent/iStent inject [Glaukos], 8 Hydrus [Ivantis]), 152 (33.9%) were gel microstents, 90 (20.1%) were goniotomy procedures. Combined phacoemulsification took place in 256 (58.7%) eyes. Reoperation within 90 days took place in 23/436 eyes (5.3%), including 16/152 eyes in the gel microstent group (10.5%), 4/198 eyes in the iStent/iStent inject group (2.0%), 3/90 eyes in the goniotomy group (3.3%). Indications for reoperation were elevated intraocular pressure (IOP) in 16/23 eyes (69.6%), gel microstent tip exposure with wound leakage in 3/23 eyes (13%), and early gel microstent encapsulation without elevated IOP in 1/23 eye (4.3%). 2/23 eyes (8.7%) required reoperation for lens complications while 1/23 eye (4.3%) had elevated IOP and aphakia requiring reoperation.
Conclusion: The rate of reoperation within the first 90 days after MIGS was low. Elevated IOP and complications associated with gel microstents were the main indications for reoperation.
ARTICLE SIDEBAR
The ASCRS Journal Club is a virtual, complimentary CME offering exclusive to ASCRS members that brings the experience of a lively discussion of two current articles from the Journal of Cataract & Refractive Surgery to the viewer. Co-moderated by Nick Mamalis, MD, and Leela Raju, MD, the July session featured a presentation by Jake McMillin, MD, author of “Accuracy of intraocular lens calculation formulas for flanged intrascleral intraocular lens fixation with double-needle technique.” The second manuscript, “Reoperation for complications within 90 days of minimally invasive glaucoma surgery” was presented by Hetal Ray, MD, resident, Yale Eye Center. To view the July Journal Club session, visit ascrs.org/clinical-education/journal-club/schedule/july-2021.
References
- Tham YC, et al. Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology. 2014;121:2081–2090.
- Chu CK, et al. Reoperations for complications within 90 days after glaucoma surgery. J Glaucoma. 2020;29:344–346.
- Tan NE, et al. Comparison of safety and efficacy between ab interno and ab externo approaches to XEN Gel Stent placement. Clin Ophthalmol. 2021;15:299–305.
- Ahmed IIK, et al. Three-year findings of the HORIZON trial: a Schlemm canal microstent for pressure reduction in primary open-angle glaucoma and cataract. Ophthalmology. 2021;128:857–865.
- Ahmed IIK, et al. A prospective randomized trial comparing Hydrus and iStent microinvasive glaucoma surgery implants for standalone treatment of open-angle glaucoma: the
COMPARE study. Ophthalmology. 2020;127:52–61. - Gazzard G, et al. Selective laser trabeculoplasty versus eye drops for first-line treatment of ocular hypertension and glaucoma (LiGHT): a multicentre randomised controlled trial. Lancet. 2019;393:1505–1516.
Contact
Ray: hetal.ray@yale.edu
Chow: jessica.chow@yale.edu