Cornea
Spring 2024
by Ellen Stodola
Editorial Co-Director
Identifying and treating patients with limbal stem cell dysfunction or deficiency can be a challenging process. Several physicians discussed how they handle these patients, including which techniques are available for mild to more severe disease.
Bennie H. Jeng, MD
The first thing to know is the difference between deficiency and dysfunction, Dr. Jeng said, because limbal stem cell deficiency means there are no more cells left, or at least not in certain areas. Dysfunction could mean that there are cells, but they just aren’t working, he said. “I make that distinction because there are cases, for example, in contact lens-associated limbal stem cell dysfunction, if you give patients a contact lens holiday, they could recover, or other cells nearby could recover or repopulate.”
While Dr. Jeng said it’s hard to give an actual incidence or prevalence, the concept of limbal stem cell dysfunction or deficiency is underdiagnosed in general because if you don’t look for it, you won’t find it. If you look carefully, 5–10% of people with chronic contact lens wear have some mild degree of limbal stem cell deficiency or dysfunction, he said.
Dr. Jeng said that contact lens intolerance and taking a contact lens holiday is the first rung of treatment for this condition. Severity escalates when the stem cells are wiped out from disease or inflammation. It becomes a problem, Dr. Jeng said, when there is more than 4–6 contiguous clock hours of deficiency because then the surface can’t re-epithelialize correctly. The cells that then populate the surface are conjunctivalized epithelial cells rather than clear corneal cells, he said. Many of these things—like chemical burns, Stevens-Johnson syndrome, and autoimmune disorders—that lead to LSCD are already being managed by corneal specialists.
Dr. Jeng said treatment of every individual patient is different. It depends on the degree and how active the disease is. “I actually had a patient who had 11 clock hours of stem cell deficiency from a chemical insult in the past,” he said. “That 1 clock hour allowed him to re-epithelialize in the very center of his cornea, and I had him in a scleral lens to protect the rest of stem cells, and for years he managed just fine with that.”
Dr. Jeng said scleral lenses are usually his first go-to if there is some degree of stem cell issue, though this may not work for every patient.
By understanding the pathophysiology of limbal stem cell dysfunction or deficiency, Dr. Jeng said that doing a penetrating keratoplasty (PK) or any sort of keratoplasty does not fix the problem because the problem is the stem cells, not the cornea itself. “If it’s an isolated stem cell issue, then keratoplasty doesn’t have a role.”
So, if scleral lenses don’t work, you’re left with really two options, Dr. Jeng said. One is a keratoprosthesis, and the other is a stem cell transplant.
Dr. Jeng has used keratoprosthesis for stem cell deficiency. “You have to be very careful about who you choose because, even though it’s an indication for doing the procedure, they have to still be able to epithelialize,” he said. “If they can’t, doing a KPro, you’re asking for trouble. If it can’t epithelialize up to the optic, then you can’t do it because they’ll melt and have a bad outcome.” For this reason, Dr. Jeng is very conservative when choosing a KPro to treat patients with limbal stem cell deficiency and said he wouldn’t generally recommend this option.
That leaves stem cell transplantation, of which there are several options. One is transplanting from one eye to the other. In the case of a unilateral chemical burn, for example, you could do that, Dr. Jeng said. If the unaffected eye is completely unaffected, then you can take either four small clock hour blocks from the other eye and move to the diseased eye or you could do simple limbal epithelial transplant (SLET). “While I personally haven’t had success with [SLET], others definitely have,” he said.
The second option is a living, related donor, which is very similar to using cells from a cadaveric donor. Use of cadaveric donors, described by Edward Holland, MD, and his group, requires systemic immunosuppression for a year, Dr. Jeng said. “I think that a lot of ophthalmologists are uncomfortable with that, and if you don’t do it right, you either have a failure of surgery or you could make the patient very sick. He added that ophthalmologists alone should not be managing these transplant medications. These are at the level of a kidney or heart transplant, he said, so you need to have the infrastructure with a transplant team that’s in place. He noted that Dr. Holland’s Cincinnati Protocol has this infrastructure.
“I’ve had a few patients ask about that [option], and we have sent them to Cincinnati to do it because we don’t have an infrastructure set up for it,” Dr. Jeng said, adding that one other obstacle is that he really doesn’t see the surgical volume necessary to set up a program like this. Dr. Jeng said that he has personally used this technique. “But I felt that I didn’t do a high enough volume that makes me the best person to do this,” he said. “It makes sense, but we need to make sure any center set up has the appropriate volume to serve the patients.”
In terms of surgeons being trained to treat limbal stem cell deficiency or dysfunction, Dr. Jeng said he believes new fellows are well versed in when someone needs a scleral lens, and they’re probably trained in KPros, as well. They are most likely not trained in stem cell transplants because many centers don’t do them, he said, emphasizing that the surgery itself is not the difficult thing, but it’s managing the patients postoperatively.

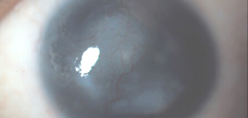
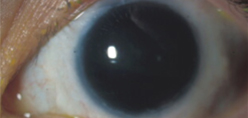
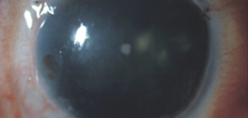
Source (all): Edward Holland, MD
Sophie Deng, MD, PhD
Dr. Deng sees patients for limbal stem cell deficiency very frequently in her practice. “We have established a center for limbal stem cell deficiency (LSCD), so we get referrals from the region and sometimes from across the country,” she said, adding that she often sees several of these cases per week.
She said the first step, even before treatment, is to stage the disease. She uses live imaging to evaluate the stem cell function in these eyes. “We do anterior segment OCT first to look at the epithelial thickness in these eyes to make sure we don’t misdiagnosis the stem cell deficiency,” she said. “Subsequently, we will perform in vivo confocal microscopy on these eyes to look at the microstructure of limbus and cornea.” We come up with a formula to quantify the stem cell function, she said.
“After we’ve done all [this] testing, then we determine the stage of LSCD,” she said. “Based on the severity of the LSCD, we treat the patients accordingly.”
Often, Dr. Deng said these patients have other comorbidities, such as ocular surface inflammation, dry eye disease, or eyelid abnormalities. In many of these eyes, their stem cell function improves as a result of removing the insulting agents, she said. As a majority of eyes with LSCD still have residual LSCs, once the health of the ocular surface improves, many of these eyes can recover quite well and subsequently, their vision improves.
The choice of treatment, Dr. Deng said, will depend on the stage of LSCD. If the patient does not recover by the optimization of the ocular surface—for example taking a holiday from contact lens use in LSCD induced by soft contact lens wear—Dr. Deng said she might proceed with a scleral lens, which can protect the cornea and can improve the vision. “This is a really good device for eyes with severe dry eyes in addition to LSCD,” she said.
Dr. Deng said she has had success treating LSCD resulting from prior glaucoma surgeries with scleral lenses.
For more severe cases of LSCD, Dr. Deng will move to surgery.
She has performed the SLET procedure as the preferred option if the disease affects only one eye. Another option, she said, if the patient has bilateral severe disease, is to use the Boston KPro. “If they have contact lens intolerance or have a severe cornea scar that a contact lens wouldn’t improve the vision, then KPro would be a good option,” she said.
Dr. Deng is also currently recruiting for a Phase 1 clinical trial investigating cultivated autologous limbal stem cells. If patients meet inclusion criteria, a tiny limbal tissue is removed from one eye, and the limbal stem cells are grown on a dish. Once there are enough stem cells, they are transplanted back to the diseased eye, she said.
Dr. Deng also has experience and success with using allogeneic stem cell transplantation with systemic immunosuppression for these patients with severe bilateral disease. However, she noted that she doesn’t employ this option as often because of a lack of interest in her patient population. “Our patients mostly are elderly patients, and they are not very keen on immunosuppression,” she said.
She noted that stem cell transplantation with immunosuppression is an option, adding that it has been shown to be safe by Dr. Holland and others. “I think it’s patient’s selection and whether the center has the expertise to do that,” she said. “I did collaborate with a team of renal transplant surgeons and internists to manage those patients. I have to congratulate Dr. Holland on their success because it’s very labor intensive, and it takes commitment on him, the renal transplant team, and the patient to manage the postoperative care and immunosuppression properly. It is a matter of disseminating the knowledge and protocol to other ophthalmologists so that they can adapt the protocol.”
Dr. Deng said that we want our trainees to be exposed to various procedures and therapies. “The fellows and residents are here to get exposed to how we make the diagnosis, stage the disease, using multimodal in vivo imaging. First, the fluorescein straining pattern is carefully examined to detect stippling staining in a whorl-like pattern, Next, an anterior segment optical coherence tomography is performed to detect whether a hyporeflective epithelial layer is present on the cornea and limbus. Lastly, in vivo confocal microscopy is performed to evaluate whether corneal and limbal epithelial cells are present in high density.” These in vivo imaging tests are a fast way to make the correct diagnosis of LSCD, she said. “We also perform impression cytology to confirm presence of conjunctival cells on the cornea, which is the hallmark of limbal stem cell deficiency,” Dr. Deng said. “The trainees are exposed to the surgical techniques of limbal stem cell transplantation and amniotic membrane graft for partial deficiency. Our trainees here have well rounded exposure to the diagnosis and management of limbal stem cell deficiency.”
Dr. Deng stressed the importance of not jumping into limbal stem cell transplant for these patients before ensuring that you’ve made the correct diagnosis and staged the disease. “Without knowing whether the eye has limbal stem cell deficiency or at what degree of severity, the treatment selection might not be appropriate,” she said. “It’s very important that the disease is correctly diagnosed and staged so the appropriate treatment can be given to the patient with the least invasive way to treat this disease.”
Marjan Farid, MD
Dr. Farid has found the best approach for severe cases of LSCD to be ocular surface stem cell transplantation with systemic immunosuppression, and her practice at UC Irvine is a site that’s set up to perform these procedures and manage them postoperatively.
Limbal stem cell deficiency occurs when the limbal stem cells of the ocular surface are diseased, Dr. Farid said. Patients might have mild early disease, she said, which can be caused by chronic contact lens wear resulting in chronic hypoxic damage to the limbal stem cells. “Those early stem cell deficiency patients, where part of their limbus is affected, some of these can be medically managed,” she said. This could include things like removing the offending agents from ocular surface, using preservative free eye drops, and decreasing the inflammation of the ocular surface. Early disease can also be caused by chronic exposure to preservatives in drops, such as long-term use of glaucoma medications, Dr. Farid said.
Then, she said, you have patients who have very severe ocular surface disease and severe limbal stem cell deficiency, and it may be combined with significant conjunctival scarring. These are patients who may have had chemical or thermal burns, patients with severe autoimmune-related disease (i.e., Stevens-Johnson syndrome), or patients with congenital aniridia who develop full LSCD because they genetically have abnormalities with the limbus. These patients will often need surgical intervention, Dr. Farid said. “These patients respond very poorly to primary keratoprosthesis, for example. They do much better when ocular surface is transplanted, restored with healthy limbal stem cells first, but it does require a whole process.”
Dr. Farid said that the process is similar to solid organ transplantation. These patients need systemic immunosuppression just like kidney transplant patients and they need monitoring for blood levels while on those medications, she said. “We have a nurse coordinator who helps manage immunosuppression, manage for toxicity, and so on. Unlike kidney transplant patients who are often very sick to begin with, our patients are relatively healthy. They do really well on these systemic immunosuppressive medications, and then we maintain those for several years, and they can be tapered off slowly over several years,” Dr. Farid said.
She called this treatment option “the only really successful way of managing these severe ocular surface disease patients.” Other treatment options, like primary corneal transplants or primary keratoprosthesis transplants on these eyes lead to corneal melts, infection, and failure at a very high rate, she said.
Dr. Farid added that management of these patients takes a whole team, and you really need a center that will support having that team, which includes a nurse transplant coordinator and a nephrology team/kidney transplant doctors who are available to consult with when their help is needed in managing the systemic immunosuppression. Because of this, Dr. Farid said there are only a handful of centers that have the ability, the training, the expertise, and the multidisciplinary approach to manage these patients. The ophthalmology team includes not only the corneal surgeon but often requires oculoplastics and glaucoma surgeons to manage other ocular co-morbidities in these patients.
Dr. Farid hopes that more large centers that have access to transplant services will begin to offer this option to patients. “It’s really the right way of doing it and decreases the risk of long-term failures,” she said. “If patients get treated the wrong way or have multiple transplants that they fail, it also primes their body to be at a higher risk of rejection. So even down the road, if we want to do things the right way, their body has been primed to be a higher rejection risk.”
In terms of learning how to use this technique of transplantation with systemic immunosuppression, Dr. Farid said there are a lot of resources in the literature on the procedure, techniques, and management. “If someone is at a center where they want to incorporate this, there’s a channel now, and several experts who are committed to helping their peers start this program,” she said. “We don’t want to be the only ones doing it. There’s a commitment to educate our corneal colleagues on this procedure.”
One of the big fears from ophthalmologists and cornea specialists is when treatment goes beyond the eye and patients have to be put on systemic therapies. She said it’s important to approach transplant colleagues to help with this and to glean from the knowledge from those doing these in massive numbers and who have had success.
About the physicians
Sophie Deng, MD, PhD
Professor
Walton Li Endowed Chair in Cornea and Uveitis
Co-Chief, Cornea Division
Stein Eye Institute
University of California, Los Angeles
Los Angeles, California
Marjan Farid, MD
Director of Cornea, Cataract, and Refractive Surgery
Gavin Herbert Eye Institute
University of California, Irvine
Irvine, California
Bennie H. Jeng, MD
Harold G. Scheie Chair and Professor
Chair, Department of Ophthalmology
Director, Scheie Eye Institute
University of Pennsylvania Perelman School of Medicine
Philadelphia, Pennsylvania
Relevant disclosures
Deng: None
Farid: None
Jeng: None
Contact
Deng: deng@jsei.ucla.edu
Farid: mfarid@hs.uci.edu
Jeng: Bennie.Jeng@Pennmedicine.upenn.edu