Glaucoma: Beyond the routine
Fall 2025
by Ellen Stodola
Editorial Co-Director
The DSLT laser (Voyager, Alcon) became commercially available in the U.S. earlier this year, and many surgeons are beginning to incorporate this into their glaucoma treatment paradigm. Several physicians discussed this new technology, how it compares to SLT, and how they’re using it in their practices.
Christine Funke, MD, is already using DSLT frequently in her high-volume practice. “I started using DSLT in clinical practice right after it was launched,” she said, adding that she’s been using it for about a year.

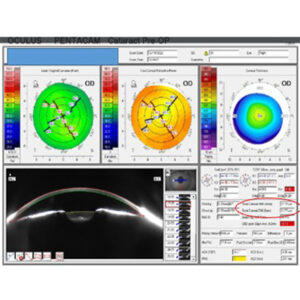
Source: Christine Funke, MD
“The reason I was excited about it is because I do such a high volume of laser that I am always looking for a way to increase efficiency and maximize my time in the operating room,” she said. “When I sit down to do laser procedures, I’ll do 70–80 patients in a half day. It used to be I would do 40–45. [With] the adoption of DSLT, as I got used to the device and my staff got better at the flow, I’ve been able to increase the volume of patients that I can take care of.”
Given that there is the LiGHT trial1 and evidence to support that SLT should be first line, we know the volume will increase, she said. “Patient volume is rising, and we need to be able to accommodate that volume. I think this is a good way to increase access of care when it comes to SLT technology.”
Shamik Bafna, MD, also cited the LiGHT trial, which demonstrated that SLT as a first-line therapy is better than drops. “The SLT group had less progression on visual fields, less need for additional glaucoma surgery, and tended to have better pressure compared to drops,” he said.
But even with this data, he said the question is, “Why haven’t we as doctors been advocating SLT as first line?” Dr. Bafna thinks the reason is that the “manual” SLT procedure is a bit cumbersome. “Traditional SLT is a procedure that’s been around for 25 years, but if you talk to most ophthalmologists, they don’t enjoy doing it,” he said.
“This is where I think DSLT has made a huge impact and has been revolutionary in terms of being able to offer something that we initially did not enjoy doing, but it’s more intuitive to do,” he said. Overall results in his hands with DSLT and traditional SLT are similar, but the main difference is it’s better accepted by both patients and surgeons.
Jella An, MD, said she works at one of the few academic centers in the U.S. that adopted DSLT early this year. “One of my longtime glaucoma patients, who had a great response to traditional SLT, was so enthusiastic about the technology that he generously donated the DSLT device to our clinic after learning about its potential to improve treatment delivery,” she said. “The early experience has been promising; patients appreciate the speed and comfort of the procedure. That said, it’s still relatively new and not yet widely available in most practices.” Dr. An noted that her institution is working on a randomized clinical trial to directly compare the efficacy, safety, and patient-reported experiences among DSLT and traditional SLT.
Dr. An said DSLT is especially helpful for patients who have difficulty being positioned at the slit lamp or tolerating prolonged gonioscopy or who have a poor gonioscopic view; this includes patients with neck/back issues, mobility challenges, anxiety during in-office procedures, or those who have hazy corneas.

Source: Jella An, MD
Comparisons to manual SLT and other treatments
Dr. Funke noted some differences between the manual SLT and DSLT procedures. There’s some comfort to the manual SLT because you can see exactly where you’re lasering. “Now we’re using something that’s automated where we’re trusting the technology to do the work because you don’t see the physical results that we’re used to seeing, the champagne bubbles in the angle,” she said, adding that DSLT offers the assurance that you’re doing the exact same thing every time. “I think the automation is good because we become more streamlined in the approach of how we’re taking care of people.”
She expects DSLT to be more accepted as well. With SLT, you need to use the goniolens. Gonio prisms can be hard for people who don’t use them very often, and the anatomy can sometimes be difficult to see.
Major pros of DSLT, she said, are that it’s simpler in terms of time, and it’s simpler in terms of how you’re able to use the laser (how it’s performed, not as many steps, and you don’t need as much experience with angle structure). For this reason, she said it will likely be more acceptable to a wider variety of non-glaucoma specialists.
“The thing about DSLT that is different is you need to have the lid speculum placed,” Dr. Funke said. “I find that helpful for most patients. I’ve learned I need the assistance of someone around me to place this, so there are some training components that need to be done with the staff.” She added that with the orientation of the DSLT, it is easier to not go back and forth to adjust the patient, so having a second person who is comfortable adjusting is helpful.
The footprint in the OR is comparable to SLT, and she said one added benefit is that patients may stand. It’s also high enough to accommodate both tall and shorter patients.
The IOP-lowering efficacy of DSLT appears comparable to traditional SLT, both in the literature and in Dr. An’s anecdotal experience. “The major advantage is its efficiency—DSLT can be completed quickly and does not require a gonioscopy or coupling gel. Patients commonly describe the sensation during treatment as ‘staticky,’ but it’s generally well tolerated,” she said.
Dr. An thinks DSLT is the most compelling first-line treatment currently available for patients with ocular hypertension or mild open-angle glaucoma. “I often offer it before initiating or escalating topical therapy,” she said. “In the worst-case scenario, insufficient IOP reduction, we can easily pivot to additional medications before surgery. Importantly, SLT offers an early, non-invasive intervention that can delay or avoid medication burden and progression to more invasive treatment.”
One main difference, Dr. Bafna said, is there’s no contact lens. DSLT is automated, as opposed to manually trying to find where to apply the laser energy, and it has an eye tracker on it to follow the limbus. It’s applying it externally by the sclera as opposed to internally to get to the trabecular meshwork.
With manual SLT, you have to put a contact lens on the eye, which blurs vision, Dr. Bafna said, so patients may not be as comfortable driving home the same day.
Many patients are being treated with drops for glaucoma, he said, so the question is if you’ll offer this instead of drops. What Dr. Bafna finds interesting is he often asks patients how they’re doing with drops, and they might say, “Great,” and the conversation ends. Now, he has changed his approach; instead of asking patients about any difficulties they’re having with the drops, he likes to ask patients how frequently they use drops, keeping the bar low to ensure he can get a clear picture if they’re missing days. “Once I find out they’re missing drops, that opens the door to discussing this technology and why I think it’s better,” he said.
Limitations and learning curve
Dr. An said, as with traditional SLT, DSLT should not be offered to patients with angle-closure glaucoma and may have limited efficacy in cases of angle recession or low tension glaucoma. Additionally, she advised caution in patients with uveitic glaucoma due to the potential risk of inflammation and secondary glaucoma in which the response to SLT can be erratic.
“DSLT can have difficulty detecting the limbus in patients with heavily pigmented limbal tissue, arcus senilis, very dry eyes, or those who cannot maintain steady fixation for 1–2 seconds,” Dr. An said. “An irregular iris or high corneal astigmatism may also affect limbal detection. For those with arcus, pigmented limbus, or very light irises, shining a muscle light from the temporal side with external room lights off and LED ring light set to 7–8 can significantly improve limbal detection. For patients with PAS, I prefer traditional SLT to better target the open trabecular meshwork and avoid treating scarred areas.”
Dr. An stressed that accurate limbal detection is critical. “Misfiring on the iris or ciliary body can lead to complications such as iridoplasty or cyclophotocoagulation, resulting in inflammation, pain, or IOP spikes,” she said. “I recommend avoiding manual adjustment of the limbal detection until you’ve gained more experience with the procedure.”
She also recommends checking IOP 30–60 minutes post-procedure and offering NSAIDs or a short course of steroids for photophobia or discomfort. In addition, it’s important to set expectations, especially in advanced cases; have a clear plan B, including escalation to urgent surgery, if the patient’s baseline IOP is high or poorly controlled on maximal medical therapy, Dr. An said.
She noted that there may be a learning curve with DSLT. “Although the procedure itself is straightforward to perform, integrating it into clinic flow required some trial and error,” she said. “Patient coaching is critical, ensuring they understand the need to stay still and look straight during treatment. We also found that pre-treating with tetracaine 10 minutes before followed by proparacaine immediately prior to the procedure significantly improved comfort.”
She also said that optimizing technician support and setup logistics is key for seamless integration. “The Alcon representatives provided outstanding support in training our technicians and surgeons, ensuring we were confident adopting novel technology that differs significantly from conventional tools in glaucoma management.”
Dr. Bafna also mentioned one limitation with DSLT is that it has to be able to identify the limbus of the patient. If there’s something going across the limbus, it won’t be able to find the limbus or perform the procedure, he said, noting the example of a patient having a pterygium or if there’s some type of a corneal scar that’s peripherally located and it’s hard for the machine to identify that. “There’s nothing from a medical perspective that’s a contraindication,” he said. “Now, I line up all these procedures one after the other, and it’s almost like performing a YAG capsulotomy.”
Dr. Bafna said the “main drawback” is the fact that you receive the same reimbursement as with manual SLT, and every time you do the procedure, there’s a click fee. However, he thinks it’s worth it because of the efficiency.
He said it’s important for physicians to know the capital cost to purchase this technology. It becomes an easier discussion if someone has an SLT device that they’re looking to replace. But if you have a perfectly working SLT machine, you wonder if it makes sense to put forth the capital expense and click fee. “In our clinic setting, I would do it hands down. It’s a much nicer procedure than what we had before. It’s completely revolutionized how we do SLT,” Dr. Bafna said.
Dr. Funke noted that there are some patients where DSLT can be more challenging than manual. One is patients who have small openings to their eyes. You need to have a 360-degree view of the sclera. “If someone is very deep set and small eyed, sometimes you can’t get the view you need,” she said. “The more I’ve done this, the more I’m finding patients anatomically where it might be hard to get the entire view of the peripheral limbus.”
In terms of the interface, Dr. Funke said it’s very user friendly. “Within a handful of patients, I felt comfortable,” she said. “By the end of my first day, which I did a larger number than average, I was already changing how I wanted my flow to go.”
Updates and future implications
Dr. Bafna said DSLT has changed his mindset in terms of interventional glaucoma. “I used to see patients who were on drops, and I had manual SLT available, but I wouldn’t have much of a discussion with patients about it,” he said. “Now that I have DSLT, I’m pushing to have patients do it.”
Dr. Funke said she’s still using manual SLT if she wants to do 180 degrees instead of a whole 360-degree treatment. Those are more targeted toward pigment dispersion, she said. “In the U.S., we don’t have the capability to change the treatment algorithm in the machine, but that’s coming and it’s already available in other countries.” In addition to that feature, Dr. Funke said she’s looking forward to other updates like manual override, which she said could help if you know where the limbus is (even if the machine doesn’t) and can automatically adjust.
Dr. Funke is also interested in being able to treat either 180 degrees or 360 degrees or in being able to skip areas. In Europe, they can skip area of treatment zone, for example if the patient has a stent. She added that there’s no known impact if you treat over that area, but it will be an option in the future to bypass this area.
“It’s wonderful to be in glaucoma right now because we have so many options,” Dr. Funke said. “These options need to be done earlier. We all emphasize this because we know that the trabecular meshwork and beyond is best remodeled and rejuvenated if we touch it early. If we wait until we’ve inundated the eye with medication, especially all the problems we see with additives and preservatives associated with those medications and we give this disease time to ravage all that tissue, the potential for rejuvenation is going to be lower. If we can get in there earlier with laser, MIGS, or drug-eluting pharmaceuticals, we see these positive benefits earlier.”
Dr. Funke thinks DSLT is going to open the door for more patients. “Right now, there’s a limited amount of people who want to do it. It does take time,” she said. DSLT has the potential to cut down on the time for the procedure, improve access for patients, and offer an improved/more comfortable procedure for the surgeon as well.
Dr. An said DSLT has the potential to increase access and efficiency while maintaining efficacy. “I see it playing a major role in reducing medication dependence, improving adherence, and offering early intervention, especially for patients who might otherwise go undertreated due to compliance issues or limited access to specialists,” she said.
Article Sidebar
Mary Qiu, MD, EyeWorld Glaucoma Editorial Board member, shared how she goes “beyond the routine”:
“In eyes with quiescent NVG with open or partially open angles, I offer angle-based surgeries that incise the trabecular meshwork, such as goniotomy and GATT, to try to surgically restore the conventional outflow pathway instead of immediately implanting a tube shunt.”
About the physicians
Jella An, MD
Storm Eye Institute
MUSC Health
Charleston, South Carolina
Shamik Bafna, MD
Cleveland Eye Clinic
Brecksville, Ohio
Christine Funke, MD
Barnet Dulaney Perkins
Eye Center
Phoenix, Arizona
Reference
- Gazzard G, et al. Selective laser trabeculoplasty versus eye drops for first-line treatment of ocular hypertension and glaucoma (LiGHT): a multicentre randomised controlled trial. Lancet. 2019;393:1505–1516.
Relevant disclosures
An: Alcon
Bafna: Alcon
Funke: AbbVie, Alcon, Elios, Glaukos, New World Medical, Nova Eye Medical, Sight Sciences
Contact
An: anjel@musc.edu
Bafna: sbafna@midwestvision.com
Funke: christine.funke@bdpec.com