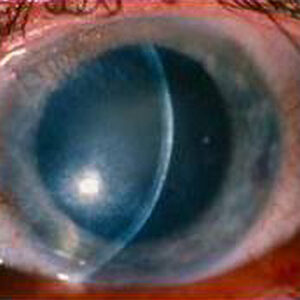
Cataract
Spring 2025
by Liz Hillman
Editorial Co-Director
Regardless of surgical experience level, Richard Tipperman, MD, said iris prolapse is something that happens to all surgeons occasionally. As such, knowledge of the risk factors that could predispose a patient for iris prolapse, how to handle the event should it occur, and postop considerations are an important refresh from time to time.
“There are a lot of different ways to manage it and mitigate it, but it is something that everyone will see on occasion, and one certainly needs to know how to manage,” Dr. Tipperman said.
Article Sidebar
Marisa Schoen, MD, Wills Eye Hospital, presented a case at the 2024 ASCRS Annual Meeting that Dr. Tipperman called “a neat trick.” In this video she takes an iris hook, makes an incision in the sclera posterior to the main incision, and hooks the prolapsed iris, pulling it out of the way. Watch the video!
Predisposition and prevention
Both Dr. Tipperman and Beeran Meghpara, MD, cited intraoperative floppy iris syndrome (IFIS) as the most common risk factor that increases a patient’s chance of iris prolapse during cataract surgery. There are a number of medications that can cause IFIS, they both said, and situations that can lead to iris prolapse, such as certain ocular anatomies, and wound construction. Medications include most notably tamsulosin/alpha blockers, though Dr. Meghpara said other medications can contribute to IFIS.
“The list keeps growing and growing,” Dr. Meghpara said of medications that can cause IFIS. “There are certain anti-psychotic medications that do it, certain blood pressure medications that have been reported, certain blood thinners. When you’re in a busy cataract practice, it’s often hard to keep track of what the different medications are that a patient is taking that is on this ever-growing list.”
Dr. Tipperman said that even if a patient is not currently on tamsulosin but had taken it in the past, it could still affect their iris.
“Some patients could have been on tamsulosin 15 years ago for a month then stopped it. They forget that they were on it, but their iris will still act like they’ve been on it the entire time,” Dr. Tipperman said. “Some patients come in for cataract surgery and they’ve been on tamsulosin for some time, and they say, ‘Should I stop it for my surgery?’ but there is no benefit in stopping it. Some patients’ irises on tamsulosin act completely normal and others very abnormal with a lot of iris prolapse.”
Dr. Tipperman said too shallow or too posterior of a phaco entry could entice iris prolapse, as could eyes with a smaller axial length or anterior chamber depth, according to Dr. Meghpara. “Even something as simple as a thin blue iris … if I see a thin or pale blue iris, that makes me worry a little bit,” he said.
Dr. Meghpara said poor dilation can clue surgeons into IFIS. “If they don’t dilate well, that is also something that will get your radar up,” he said.
If you have a known IFIS case that could be at risk for iris prolapse, Dr. Meghpara said it’s important to dilate the patient as much as you can ahead of time. He said if he’s worried about proper dilation, he’ll increase the phenylephrine dose to as high as 10%. He also said the patient could be started on an atropine drop 1–3 days preoperatively to improve dilation. “There have been reports of using a topical NSAID 1–3 days before surgery also helps improve dilation. Just [try to] get as much dilation as you can ahead of time,” he advised.
Maintaining that dilation intraoperatively can be achieved with intracameral injections of epinephrine or phenylephrine/ketorolac (Omidria, Rayner) in the irrigating solution. The latter, he said, is helpful if you have access to it from a coverage standpoint.
Dr. Meghpara said it’s important with some of these cases to place incisions a little more anterior and make them a bit longer to get them farther away from the limbus so the iris is less likely to prolapse out.
Intraoperatively, Dr. Tipperman said overfilling with viscoelastic, overly aggressive hydrodissection, or even a speculum that’s putting too much pressure on the globe can lead to iris prolapse.
Prolapse management
Dr. Tipperman said prolapse is most likely to occur early in the case when you have made the incision and you put in viscoelastic. In some cases, it occurs when you make the paracentesis, which is a sign “you’re going to be battling it all day,” he said, though this is less common. “It’s more common that the iris will come out of the main incision.”
At this point, Dr. Tipperman said to pause and assess the situation. Say to yourself, “Why is this occurring?”
“If it’s pharmacologic, a lot of people, myself included, think that putting some sort of agent in the anterior chamber like epinephrine will stiffen the iris and prevent some of the billowing and the prolapse. Some people will use iris hooks also,” he said. “If it’s coming from positive pressure, are you putting too much pressure on the eye with the way the speculum is? Did you put in too much viscoelastic; do you need to burp some out? Or is it your incision—did you happen to enter a little too posteriorly, or is your incision a little too shallow and the iris is coming out?”
Dr. Tipperman said when the iris keeps coming out of the main incision due to wound construction, one option is to place a sheets glide through the incision over the iris to push it back and protect it from the phaco. Another option is to sweep the iris back in, suture the incision, and move a few clock hours away. The latter, he said, takes a little bit more time, but it makes the case easier in the long run.
Dr. Meghpara said when prolapse occurs, “don’t panic.”
“You don’t want to turn something that is fairly easy to manage, do the wrong things, and turn it into a much bigger situation,” he said. “The first thing is avoid trying to push it back in or trying to fill up the anterior chamber with more viscoelastic to push it back in. You want to decrease the pressure in the anterior chamber. The way you do that is you shallow it through a paracentesis; try not to touch the iris as your first reaction.”
Once the pressure is lower, he said to use a blunt instrument through a paracentesis to sweep the iris back into the eye. “We’re not pushing it in but sweeping it from inside and sweeping it out of the incision back into the anterior chamber,” he explained.
After one prolapse, Dr. Meghpara said the iris tends to want to do it again, so he’ll adjust his phaco settings to low flow, decreasing the bottle height and lowering the vacuum and aspiration rates so there is less fluid going behind the iris.
“Sometimes once you get it in the eye, you can put a very small amount of high viscosity viscoelastic on top of the iris by the incision to push it backward. You don’t want to overfill the anterior chamber with viscoelastic completely because then you’ll prolapse out again because you’ve created too much pressure in the anterior chamber, but a very selective amount right in the area of prolapse will help,” he said.
If it keeps prolapsing out despite these efforts, Dr. Meghpara will employ iris hooks (usually four in a diamond shape to keep the iris taut) or a Malyugin ring. “What you can also try to do is put in iris hooks or the Malyugin ring and constrict the pupil, with an intracameral miotic. … You need the pupil dilated to finish up the surgery, but if you have the pupil contracting against a Malyugin ring, it’s going to be more taut. It may make it less floppy,” he said.
Another option Dr. Meghpara offered, if the iris keeps prolapsing out, to avoid damaging the tissue, is to leave it out of the wound, finish the cataract portion of the case, and sweep the iris back into the eye at the end of the case.
“It’s out of the eye but at least you’re manipulating it less. That’s the last-ditch effort to finish the case because every time you touch it, you’re creating defects in the iris and you could have a bigger issue after the fact trying to repair that,” he said.
Postop, if there are not significant iris defects caused by the prolapse and subsequent manipulation to get it back into the eye, the patient should not experience any issues. If there are significant iris defects, both Dr. Tipperman and Dr. Meghpara said they tell the patient that the case was difficult and that if they experience visual disturbances due to the iris defect, they can fix it.
Dr. Meghpara added that with the extra manipulation in these cases, patients who experienced iris prolapse can be more prone to CME, so he advised an NSAID postop.
Article Sidebar

Rom Kandavel, MD, EyeWorld Cataract Editorial Board member, shared what he is excited for at the ASCRS Annual Meeting:
“My favorite part about the ASCRS Annual Meeting is walking away with that little nugget of information that makes a meaningful change in my practice. Sometimes it’s clinical, sometimes it’s administrative, but each time it makes a difference.”
About the physicians
Beeran Meghpara, MD
Co-Director of Refractive Surgery
Wills Eye Hospital
Philadelphia, Pennsylvania
Richard Tipperman, MD
Attending Surgeon
Wills Eye Hospital
Philadelphia, Pennsylvania
Relevant disclosures
Meghpara: None
Tipperman: None
Contact
Meghpara: bmeghpara@willseye.org
Tipperman: rtipperman@mindspring.com