Cataract
Fall 2025
by Liz Hillman
Editorial Co-Director
Asignificant number of patients presenting for cataract surgery have signs or symptoms of dry eye.1 In recent years, there has been a concerted education effort on the importance of ocular surface optimization to ensure accurate IOL calculations and candidacy for advanced-technology IOLs, when desired. In addition, there are now more treatments available for dry eye and ocular surface conditions.
With an increase in education and treatment options, however, some questions can arise. Who really needs surface optimization vs. who is essentially ready to schedule for surgery now? What’s reasonable in terms of treatment? When is a patient who needed ocular surface optimization ready for surgery?

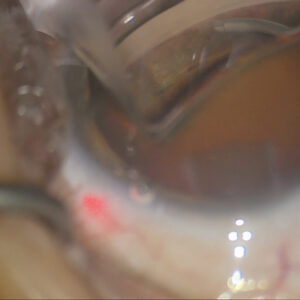
Source: William Trattler, MD
Targeting optimization
Tal Raviv, MD, said about a decade ago he began to practice based on refractive cataract surgery. It was a time when the impact of the ocular surface on refractive outcomes became widely publicized. At that time, he said, the practice was performing surface optimization measures on 70% of their patients.
“We were bringing them back for any abnormality,” Dr. Raviv said of putting patients on a surface optimization protocol before repeating biometry for IOL calculations. Over time, however, the practice found that for many patients, this aggressive optimization didn’t move the needle in terms of outcomes.
“We did (and still do) dry eye screening questionnaires for any new patient,” he said. “We empowered our staff members to do further diagnostic tests, such as osmolarity or MMP-9 testing or meibomian gland imaging. Then we would do the slit lamp examination and other diagnostic cataract devices. With all that, I used to find just about everyone had something off. Whether they had symptoms of dry eye on the SPEED questionnaire or signs of dry eye, one of their point-of-care tests was a little off.”
As such, the practice began patients on a protocol that could include a range of surface optimization therapies—over-the-counter tears, supplements, heat and massage therapy, prescription eye drops, or even in-office procedures—before seeing them back several weeks later for repeat measurements. “We did this for a few years,” he said. “I was just getting my practice going, so we had the capacity to do it, but I did notice that a large majority of these patients came back, we repeated the biometry, and it was the same.”
Dr. Raviv said that perhaps the testing paradigm for ocular surface disease was a “little too sensitive” for what was needed to proceed with cataract surgery for most patients. So, as his practice matured, he started to figure out which patients actually needed optimization vs. which ones didn’t.
As in the ASCRS Preoperative OSD Algorithm, which separates dry eye into visually significant vs. non-visually significant, Dr. Raviv said visually significant dry eye cases were the ones where keratometry measurements improved after surface optimization therapies.
“The ones that were not visually significant, meaning patients may have had some symptoms, some blepharitis, or some abnormal point-of-care testing, but they did not have corneal staining, we found a way to be more specific,” he said. “The topography looked normal, and there were multiple keratometries that we did on biometric devices lined up. Those patients did just fine going with those initial measurements for surgery.”
Dr. Raviv clarified that this doesn’t mean he didn’t discuss or treat dry eye with these patients, it just didn’t delay the patients’ surgeries.
Dr. Raviv said he uses three keratometric devices and reflection topography (Placido disc) or an LED light topography. “We obtain two late generation biometries, an auto-K, and the Cassini topographer [Cassini Technologies], and that gives us four sets of Ks to look at, four sets of astigmatic axis of certain magnitude and direction. If those are variably off, we know that something’s up on the ocular surface; we can’t go forward,” he said. “If they all line up nicely and the topographic picture looks regular, either bowtie astigmatism or spherical, I am comfortable proceeding typically without further optimization of the surface.”
If a patient is optimized for severe or even moderate dry eye and they improve, Dr. Raviv said he still might avoid a diffractive multifocal IOL for this patient in favor of blended or monovision. “If it’s just a mild dry eye, and they come back and look pretty good, I might use one of the newer generation multifocals,” he said. “But if they’re pretty dry and it took a while to get them to be optimized, I’m going to recommend a monofocal.”
With the number of cataracts going up, Dr. Raviv said efficiency is key. He has found that focusing optimization on only visually significant dry eye patients is more efficient. “I find that focusing on the more critical subset of dry eye patients that I mentioned, the visually significant dry eye patients, those are the ones we really don’t want to miss, and we want to be able to bring those people back. For the ones who may have mild symptoms but they don’t have visually significant dry eye, we want to address it, we want to know about it, but we’re a little more confident in our biometry and those patients. The whole point is you’re not delaying your surgery because of this.”
Finally, he said it’s important to note that there are patients with conditions that typical surface optimization won’t fix. There are many conditions that can result in irregular topography that are not dry eye. “You treat them like crazy, they come back, and it looks the same.” This is where he finds OCT epithelial thickness mapping helpful. Their tear film is fine but their epithelium is not. Dr. Raviv said this is subclinical EBMD that may not be seen on slit lamp exam. He performs a superficial keratectomy on these patients and waits 3 months for the re-epithelialization and smoothing before proceeding with measurements for IOL calculations.
“I’m really looking for a regular ocular surface with repeatable biometry on multiple devices to be comfortable that we can get close to the refractive outcome that the patient and I are desiring,” Dr. Raviv said.
Homework up front reduces postop work
William Trattler, MD, said he brings back a lot of patients for surface optimization and repeat measurements. Patients in his practice, he clarified, are not counseled or pre-treated with anything prior to their first exam.
If patients were advised, when they called in for their initial consultation, to use hypochlorous acid and artificial tears prior to their in-person exam, Dr. Trattler said it would result in better readings and reduce the need for bringing patients back after surface optimization measures. “Is the dry eye going to be solved for everyone, no … but it might be that only 20% of patients need a second set of readings,” he said.
Dr. Trattler said he obtains three measures of astigmatism prior to cataract surgery: a Cassini, a Pentacam (Oculus), and an IOLMaster 700 (Zeiss). If the astigmatism axis and power measurements align, he knows the readings are good. “As Dr. Raviv shared, in the presence of dry eye, if the three astigmatism results align, we can be confident that the measurements will provide reliable information for calculating our IOL power as well as our astigmatism power and axis,” he said. “However, when there are significant differences in the three astigmatism measurements, I will initiate therapy for the ocular surface and have the patient return for repeat measurements.” If you’re only using one device for your astigmatism readings you can potentially miss these inconsistencies.
Dr. Trattler emphasized that ocular surface optimization is important even for patients receiving basic monofocal IOLs. “These patients may not be selecting a premium IOL, but they’re still undergoing surgery and have high expectations,” he said. “Our goal is to deliver the best refractive outcomes possible. While they understand they may need glasses afterward, it’s critical to avoid leaving them significantly off target. Every patient we treat becomes an ambassador for our practice, so we strive to achieve the best results for every case.”
He added that patients who initially decline an advanced-technology lens can sometimes reconsider and call back to explore more advanced options. Dr. Trattler’s threshold for optimization and measurement quality does not differ if the patient is seeking a monofocal or advanced-technology lens. “Not only is it important to address dry eye preoperatively, but patients often experience dry eye symptoms after surgery. If their condition wasn’t treated prior to surgery, they may return complaining that their eyes are irritated and/or their vision is blurry, due to an exacerbation of their underlying dry eye. These patients may think that these symptoms are related to complications from their surgery, when in reality these symptoms are caused by their pre-existing dry eye that was not effectively treated.”
Dr. Trattler explained that topography is most helpful for assessing corneal irregularity and evaluating measurement repeatability. “If the irregularity is consistent across scans, that indicates it is a true anatomical issue, such as EBMD or Salzmann’s nodules,” he said. “If the corneal irregularity is not repeatable, and if it improves after treatment, that points to dry eye/ocular surface disease as the source of the inconsistent readings.”
Dr. Trattler said focusing on surface optimization preop is like doing your homework ahead of time vs. having to work harder on the back end. “Doing the work ahead of time has a payoff—happier patients, better outcomes, and more comfortable patients postop,” he said. Dr. Trattler said he does everything he can to improve a patient’s ocular surface rapidly without delaying surgery. “I get my patients scheduled for surgery on the first visit, but I bring them back in between for their final measurements,” Dr. Trattler said. “It’s pretty rare that I have to reschedule surgery.”
About the physicians
Tal Raviv, MD
Eye Center of New York
New York, New York
William Trattler, MD
Director of Cornea
Center for Excellence in Eye Care
Miami, Florida
Reference
- Trattler WB, et al. The Prospective Health Assessment of Cataract Patients’ Ocular Surface (PHACO) study: the effect of dry eye. Clin Ophthalmol. 2017;11:1423–1430.
Relevant disclosures
Raviv: Johnson & Johnson Vision
Trattler: AbbVie, Alcon, Bausch + Lomb, BVI, Cassini Technologies, Harrow, Oculus, Sun Pharma, Zeiss
Contact
Raviv: talraviv@eyecenterofny.com
Trattler: wtrattler@gmail.com