Glaucoma: Changing mindsets
Summer 2025
by Liz Hillman
Editorial Co-Director
James T. Murphy, MD, began using virtual visual fields in his glaucoma practice in 2020 as a pandemic necessity. Lori Provencher, MD, incorporated virtual visual fields over a year ago when she switched practices.
“I can’t imagine going back,” Dr. Provencher said, noting that when she joined Vance Thompson Vision in Omaha, Nebraska, the practice already had a standard Zeiss Humphrey Visual Field Analyzer but had decided to invest in three Radius VR headsets. The latter are now her preference. “Clinically, Radius has a testing strategy, RATA, that is similar to SITA, and it has excellent correlation with HFA when staging disease. It has also been studied in all ranges of disease severity, which gives me confidence using it in a diverse glaucoma practice. The background luminance is also the same as the HFA, an important detail that is missed with other virtual field devices. For patients, the headset is light, comfortable, ergonomically superior to bowl perimetry, and easy to use. Patients don’t have to shuffle from room to room. My team loves Radius as well. They find it easy to use, and they love that it eliminates the bottleneck waiting for an HFA. From a practice perspective, educational videos, billing data, and easy software updates are also a value add.”
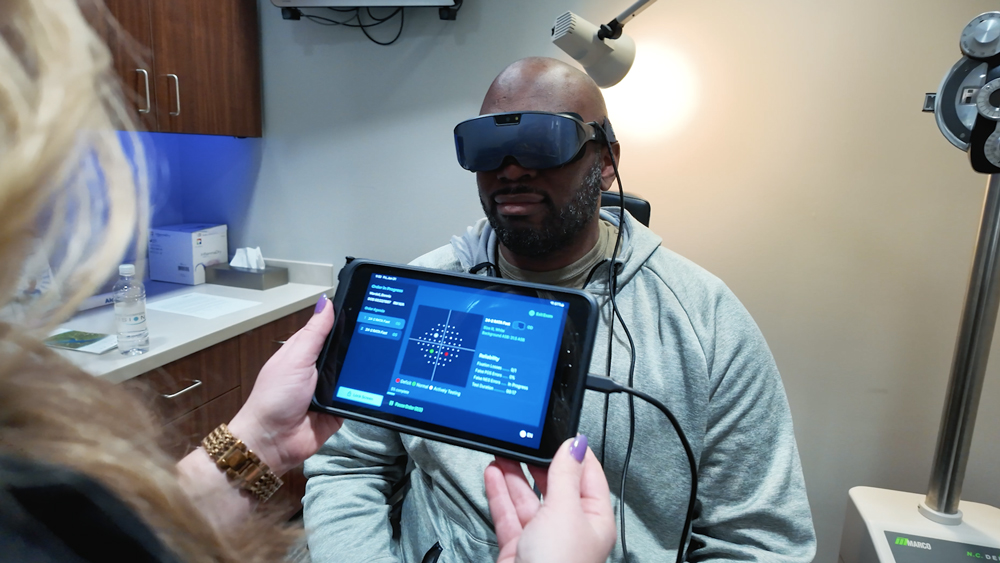
Source: RadiusXR
Dr. Murphy said his practice brought in the technology because it allowed them to conduct virtual visual fields with patients in their car when pandemic social distancing measures were in place. “We handed it to them outside in the parking lot,” he said. “It worked really well to continue to monitor glaucoma patients. Then we thought, ‘We could use these forever.’”
Dr. Murphy said he’s found virtual visual fields versatile and well-liked by patients. There is also an audio coaching aspect with different languages, which he has found useful. Dr. Murphy said the ergonomic features of virtual visual field technology are an advantage as well. Whether it’s a patient who is wheelchair bound, one who has neck issues, or one who just cannot maintain the position required for taking visual fields with a tabletop device accurately and reliably, virtual visual fields have come to the rescue.
Dr. Murphy said he has demoed various virtual visual field devices, such as Radius and Olleyes. “I’ve dabbled over the years because I’ve been curious about how the technology is evolving and improving,” he said.
While virtual visual field use is not ubiquitous within ophthalmology practices, Dr. Murphy said he thinks 5 years from now it will “100% be standard of care.”
“I liken virtual field testing to when Humphrey superseded kinetic Goldmann field testing,” he said. “Nowadays it is impossible to find a technician who can run a Goldmann. Inevitably, new, better, more efficient technology replaces the old. At first, there are always skeptics, but eventually practicality wins, and the standard of care evolves.”
Dr. Murphy thinks there will be a gradual shift in the market, and an HFA will become less common to find in private practice, and more so one will see virtual reality wearable devices administering automated perimetry. As this shift occurs, he thinks that research standards will evolve to accommodate this change in technology prevalence.
For those who have not yet switched to virtual visual fields, Dr. Murphy said they have to try it, and he noted that it is billable the same as HFA or any automated perimetric device that tests and maps sufficient isopters or performs similar quantitative analysis of the field of vision.
“Virtual devices perform the same testing as an HFA, but they are a fraction of the size and are more user-friendly when it comes to connecting to your EHR. Unlike larger, tabletop devices, wearable devices can be mailed in for service, immediately replaced, and often remote WiFi-based troubleshooting can solve problems; software updates come automatically over WiFi. Larger devices cannot be shipped, so when they require service, a service technician has to travel to your office, often taking weeks, which is a big hit to a practice’s workflow and bottom line, Dr. Murphy said.
From an efficiency standpoint, Dr. Murphy said completing a virtual visual field with a wearable takes between 2–3 minutes.
Yvonne Ou, MD, is currently studying virtual reality visual fields but not making any clinical decisions based on them.
“Through an originally unfunded collaboration and now an NEI-sponsored project, we are working with Vivid Vision to study Vivid Vision Perimetry (VVP) and its ability to accurately monitor glaucoma progression,” Dr. Ou said. “I do not think there is any clinical evidence (as of yet) that virtual reality visual fields can be used for monitoring glaucoma progression, and I hope to be part of the team that generates that evidence.”
Dr. Ou said the potential benefits of virtual reality visual fields are numerous: easier test taking, more efficient use of clinic resources, lower cost, portability, and home testing. In addition, the Vivid Vision test is easier to take for patients as it does not require patients to maintain steady fixation and suppress their foveation reflex. Instead, the test is designed so that patients look at each stimulus as it is being presented, making for a more intuitive test taking experience.
Artificial intelligence in glaucoma
While none of the physicians interviewed for this article use artificial intelligence directly in the clinic to inform their glaucoma practice currently, they do envision a future where it will be helpful.
“I think AI will continue to grow in all areas of medicine, but for glaucoma in particular, generative AI could help clinicians synthesize the immense amount of data we use to make decisions (e.g., family history, pachymetry, vision, corneal hysteresis, optic nerve exam, IOP, OCT, visual fields, etc.) to risk stratify patients and support more efficient decision making. It could also monitor for progression in testing, either in person or even remotely,” Dr. Provencher said.
She added that if AI could someday screen patients and accurately triage them to a primary eyecare provider or a surgeon, this would be a huge win for the aging population and stretched medical system.
“Also, we spend a large proportion of our time counseling and educating patients. AI could help with this to make the doctor more efficient, but it must not come at the expense of the patient experience and the personal connection a patient needs with their surgeon,” Dr. Provencher said.
Dr. Ou is excited to see the potential of AI identifying patients at risk for glaucoma, making screening programs more efficient and widespread. “I am also interested in the potential of AI to identify and predict high-risk progressors, as these are the patients who need timely intervention,” she said. “But diagnosing glaucoma and identifying its progression is not always easy even for the most experienced glaucoma specialist, thus great care must be taken as we adopt AI into clinical practice.”
Dr. Murphy said there is already an FDA-approved AI-based tool for glaucoma screening, Alris AI. He said this tool, which he doesn’t have experience with, crunches numbers like corneal thickness, visual field, retinal nerve fiber layer, and IOP over time to provide a glaucoma risk assessment.
Other technologies in the pipeline that will be helpful for glaucoma include handheld/mobile OCT. The theme here is smaller, faster, cheaper is better, Dr. Murphy said. “AI-based analytic tools have already demonstrated that they are capable of distinguishing glaucomatous versus non-glaucomatous field defects with accuracy as good as or better than trained subspecialists, and the potential is only growing. It’s already smarter than we are, it’s just a matter of how practices leverage that potential to their benefit and the benefit of patients,” he said.
Dr. Murphy said he would love for AI technology to be able to help him compare apples to oranges of 20+ years of visual field analysis from an older proprietary progression analysis system to newer wearable systems.
“AI has such a wide-ranging number of applications, and we’re just scratching the surface of what it can do for us,” Dr. Murphy said.
About the physicians
James T. Murphy, MD
Scarsdale Ophthalmology Associates
Scarsdale, New York
Yvonne Ou, MD
Professor, Vice Chair for Postgraduate Education
Department of Ophthalmology
University of California, San Francisco
San Francisco, California
Lori Provencher, MD
Vance Thompson Vision
Omaha, Nebraska
Relevant disclosures
Murphy: None
Ou: NEI-funded Vivid Vision
Provencher: Radius
Contact
Murphy: jamestmurphyiiimd@gmail.com
Ou: Yvonne.Ou@ucsf.edu
Provencher: lorrainemprovencher@gmail.com