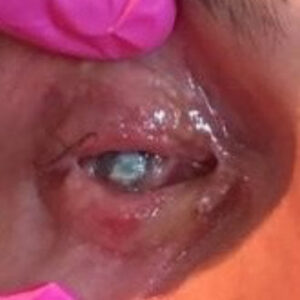
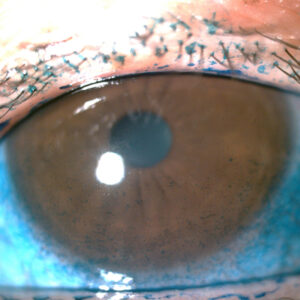
Cornea
Summer 2024
by Julie Schallhorn, MD
Cornea Editor

“My doctor told me I have dry eye.” I hear this statement multiple times a day in clinic. It is often followed by a litany of trialed therapeutics and a narrative of their effect. I sit quietly until the patient has unburdened themselves of this history. “Let’s start from the beginning—tell me exactly how you feel.”
I have to start from the beginning because the diagnosis they have been given often means nothing. “Dry eye” is a symptom, not a disease. A diagnosis of “dry eye” is like telling someone they have vision loss. The symptomatic result of vision loss is loss of vision. The symptomatic result of dry eye is … a feeling of dryness.
There are numerous conditions that manifest as a feeling of dryness in the eye, and these have been lumped together as “dry eye disease.” The ocular surface is an incredibly complex and dynamic structure that we are constantly learning more about. Dysfunction of our meibomian glands manifests with the same symptoms as dysfunction of the lacrimal gland which in turn can have the same symptoms as issues with orbicularis oculi—all of them can leave a patient feeling dry.
We have advanced to a point in our understanding of ocular surface disease that we can stop describing the condition as a symptom and instead start to discuss the underlying pathophysiology of the patient’s condition.
Julie Schallhorn, MD
We have advanced to a point in our understanding of ocular surface disease that we can stop describing the condition as a symptom and instead start to discuss the underlying pathophysiology of the patient’s condition. Rather than dry eye, it should be meibomian gland dysfunction, lagophthalmos, ocular rosacea, ocular surface inflammation, Demodex, etc. By looking for the root cause and naming it, we can then select the therapeutic with the correct mechanism of action.
Two of this issue’s Cornea articles focus on the therapeutic options we have available for ocular surface disease. As you read the articles, note how the experts discuss the therapeutic classes of the agents, discussing mechanism of action rather than a blanket treatment for “dry eye.” Knowing the mechanism and the target action will help you deliver these therapeutics where they will have the most effect and avoid treatment failures that are frustrating both for the patient and the doctor.
As we continue to see progress in ocular surface therapeutics, we need to continue to evolve our vocabulary surrounding ocular surface disease. I challenge you to start differentiating your “dry eye” patients as you see them in clinic. Think about the root cause and name the real disease. As our options for treatment increases, this will be the key to efficient and targeted therapy.
Article Sidebar
I wish I had …
W. Barry Lee, MD, Cornea Editorial Board member, shared what he wishes he had:
I wish for endothelial cell injections to get a quick approval from the FDA for the treatment of corneal endothelial disease. Patients in the FDA studies have done amazing thus far.