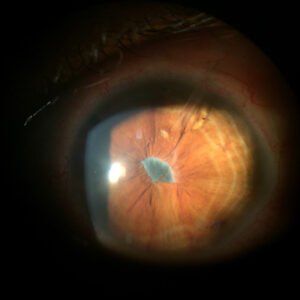
Glaucoma: Strike!
Fall 2024
by Liz Hillman
Editorial Co-Director
Various patient scenarios, combined with surgeon preferences and comfort with the procedures, dictates tube shunt placement for glaucoma patients. The different placement options allow the surgeons to knock down challenges in order to set the patient up for the greatest likelihood of tube shunt success.
“I will do all three locations in different circumstances,” said Jacob Kanter, MD.
“Where you choose to place the tube is multifactorial,” said Poonam Misra, MD.
Anterior chamber placement
Dr. Misra said that anterior chamber is her preferred location for tube shunts.
“Normally we prefer to put them in the anterior chamber. It’s a large enough space and the tube is visible when you examine the patient to confirm no obstruction of the lumen,” Dr. Misra said.
Dr. Kanter said that anterior chamber placement is the only choice for phakic patients and those who have not had retina surgery.
“If they still have their lens, technically, it’s possible to fit it in the sulcus, but it’s very risky,” Dr. Kanter said. “If you have someone who is a young patient, a steroid responder, or a young primary open angle glaucoma patient who has a clear lens and you decide to do a tube instead of a trabeculectomy, you have to put it in the anterior chamber.”
Dr. Kanter said procedurally anterior chamber placement is simpler because you can see the needle the whole time as you’re making a track for the tube, and there is not a lot of risk for bleeding in this space.
The biggest con for anterior chamber placement is the increased risk for corneal decompensation potentially leading to corneal failure. “Even in some cases, it might look perfect, but the cornea decompensates, and we have to remove the tube or keep it but move it to the sulcus more posterior,” Dr. Kanter said.
To avoid this, Dr. Misra said to make sure the tube is closer to the iris than the cornea (or at least midway between the two structures). She said the bevel should be up, facing away from the iris. Dr. Misra said that with this placement, it’s important to perform careful gonioscopy preop to make sure there is enough space in the area where you intend to place it and you are aware of any peripheral synechiae or scarring. It’s also important to make sure your tube entry site is positioned posterior enough from the limbus to limit tube exposure risk in the future.
Ying Han, MD, PhD, said anterior chamber placement is not her preferred location, but she will use this space if 1) the patient is phakic and young or 2) if the tube could get blocked by vitreous when placed at sulcus, such as with loose zonules.
Sulcus placement
Dr. Han said sulcus placement is her preferred location for tube shunts, primarily because of its protective effect on the corneal endothelium. She acknowledged that sulcus placement may be trickier, but the learning curve is not steep. All her fellows and residents are able to perform sulcus tube placement during training.
Dr. Han said she enters 4 mm from the limbus using a 20-gauge MVR blade, which is bigger than the diameter of the tube, to make tube insertion easier. She finds there is almost no leakage because the tube is inserted through the ciliary body, and the ciliary body muscle constricts to prevent leaking. She doesn’t find bleeding to be an issue due to the use of the sharp MVR blade to get through the ciliary body and use of viscoelastic to create space, smooth the path for the tube, and tamponade any bleeding.
Dr. Han emphasized the importance of creating a bevel-down configuration for the sulcus tube placement. This is to prevent the tube being plugged by the iris tissue, which occurs if a bevel-up tube is placed in the sulcus. She dilates the patient for sulcus tube placement to help with visualization.
Dr. Kanter said sulcus placement is trickier from a visualization and space standpoint. For precise placement, he recommended using one of the guidewire techniques, which he and colleagues published about earlier this year.1
Another pearl Dr. Kanter offered is to use viscoelastic to deepen the sulcus (as he would with anterior chamber placement as well). Dr. Kanter said bevel direction is traditionally posterior for sulcus placement to avoid iris clogging the tube, but some surgeons still bevel anteriorly as they would for anterior chamber placement. An anterior bevel helps the tube go into the sclerotomy a little easier, Dr. Kanter said. He said he’s never seen iris block a sulcus tube that was beveled anteriorly, unless it was actually sticking into the iris. “As long as it’s parallel to the iris, you can get away with an anterior bevel in the sulcus,” he said.
Pars plana placement
Dr. Han will use pars plana placement when she wants the tube to be even farther away from the cornea or in the setting of anterior segment dysgenesis when there is limited space in the anterior chamber or sulcus.
If a patient is at high risk for corneal damage or if they’ve had prior corneal surgery, Dr. Misra said the sulcus or pars plana are options for tube placement, but she personally sees benefits to pars plana. “Sometimes with the sulcus, you don’t have a sense of what happened there (what their cataract surgery was like, if there is any scarring, etc.).”
Dr. Misra said she finds the pars plana also a bit safer if a patient has already had tube exposure episodes because the tube entry into the eye is farther back from the limbus. “Tube exposure risk is a big reason why we decide to place the tube in the posterior chamber,” she said.
The physicians interviewed for this article emphasized the importance of a thorough vitrectomy by retina colleagues prior to pars plana tube placement to avoid vitreous clogging the tube. Dr. Misra also said leaving the tube a little bit longer into the posterior cavity could help for postop visualization.
Tube management
Dr. Han said for sulcus tube placement, she sees postoperative patients at 1 day, 1 week, and 1 month postop. Most of the time she doesn’t need to see the tube postop in exams.
“The key point is during surgery, you need to see the tip of the tube clearly before you finish the case. I had one case where we were not sure if the tube was clearly visualized in the sulcus intraoperatively. The next day the patient had an IOP spike, and the tube was stuck in the ciliary body. Since then, I know I need to clearly see the tip of the tube before I close the case. That’s intraoperatively. Postop, if you don’t see the tube, that’s fine, it’s behind the iris,” she said, adding that she thinks in sulcus placement, the tube should be bevel down, away from the iris. An indentation in the iris postop combined with an IOP spike could indicate that the iris has been sucked into the tube.
Dr. Han said she uses a long-term steroid postop for a few months. This prevents scar formation. She also uses mitomycin-C at 1 week and sometimes 1 month to prevent scar formation. “In general, tube management is easier than trabeculectomy. The key to success of the tube shunt surgery is to prevent scar formation, including controlling the inflammation to prevent the hypertensive phase,” Dr. Han said.
Dr. Misra said she watches out for how quickly a patient encapsulates the bleb over the plate itself. If IOP starts to increase early, she suspects early encapsulation and utilizes aqueous suppression early.
“I think that’s probably the biggest tube failure—in a lot of these patients, their pressure starts creeping up and we don’t address it early enough and suddenly their pressure is back to their preoperative range. I’m not afraid to start suppression if I think the pressure is beginning to creep up and discuss this possibility with patients preoperatively,” she said. Dr. Misra also said it’s important to watch out for hypotony, especially with Baerveldt tubes (Johnson & Johnson Vision), when using a wick or fenestrations.
“As soon as I see anything relevant to clinical hypotony—corneal lens touch or persistent shallowing—I use cycloplegics or even reform the eye in the office with a viscoelastic, if they’re having severe shallowing after tube placement. I think all of this is prevented by close monitoring in the postoperative period,” she said.
Article Sidebar
DECLARE trial
It’s unknown whether sulcus placement of tubes actually results in less endothelial cell loss compared to anterior chamber placement, but the Glaucoma Drainage Device and Endothelial Cell Loss Compare Trial (DECLARE) aims to provide some data for this debate. The prospective, multicenter, outcome-masked, randomized clinical trial is enrolling patients who will be randomized 1:1 to receive either sulcus or anterior chamber tube placement. Endothelial cell density and IOP will be measured at 12 months and 24 months of follow up.
“Because we don’t know which tube placement is better, we’re conducting the DECLARE trial. We’re hoping it will provide more information about endothelial cell count and outcomes, so stay tuned,” Dr. Han said.

Article sidebar
Mary Qiu, MD, Glaucoma Editorial Board member, shared how she has knocked down clinical and surgical challenges:
I started using a 3-0 Prolene guidewire to assist with sulcus tube placement if there is a tricky case where the tube does not want to easily go into the sulcus.
About the physicians
Ying Han, MD, PhD
Vice Chair for Clinical Services and Medical Director
Department of Ophthalmology
University of California, San Francisco
San Francisco, California
Jacob Kanter, MD
Assistant Professor
Johns Hopkins University
Baltimore, Maryland
Poonam Misra, MD
Assistant Clinical Professor
Department of Ophthalmology
Glaucoma Center at Manhattan Eye, Ear & Throat Hospital, Northwell
Zucker School of Medicine
New York, New York
Reference
- Shah A, et al. Three techniques for guidewire-assisted sulcus glaucoma tube shunt placement. Am J Ophthalmol Case Rep. 2024;34:102009.
Relevant disclosures
Han: None
Kanter: None
Misra: None
Contact
Han: Ying.Han@ucsf.edu
Kanter: jkanter2@jh.edu
Misra: Pmisra1@northwell.edu