Glaucoma
April 2022
by Ellen Stodola
Editorial Co-Director
With many expanding technologies in ophthalmology, it makes sense that teaching modalities in the field would expand as well. Anuradha Khanna, MD, created the OcuSim virtual reality training, designed to be used specifically with the Oculus headset, to help teach some of the anatomy and knowledge needed in ophthalmic training. Dr. Khanna explained how she developed this technology and how it’s used at her university. Meenakshi Chaku, MD, discussed how she’s finding it particularly useful in glaucoma education and training.
Dr. Khanna noted that she was getting commendations for her teaching, and this motivated her to look at how adults learn and what educators need. When deciding what to pursue, Dr. Khanna said she came upon virtual reality and in 2010 decided that she was going to write a 3D book in ophthalmology. In 2014, she was able to create the first prototype, and she introduced it in the ophthalmology department at Loyola University, where they began to use it for medical students and residents.
Dr. Khanna created a 3D model of the eye with anatomy and was able to correlate clinical pathology as well. In virtual reality, there is the capability of instant dissection that is color coded and easily understandable, she said, and students can practice what’s going on clinically and how to diagnose the patient. Dr. Khanna was in the middle of expanding content for this model when the COVID-19 pandemic hit, and the hardware and learning center she was using became inaccessible.
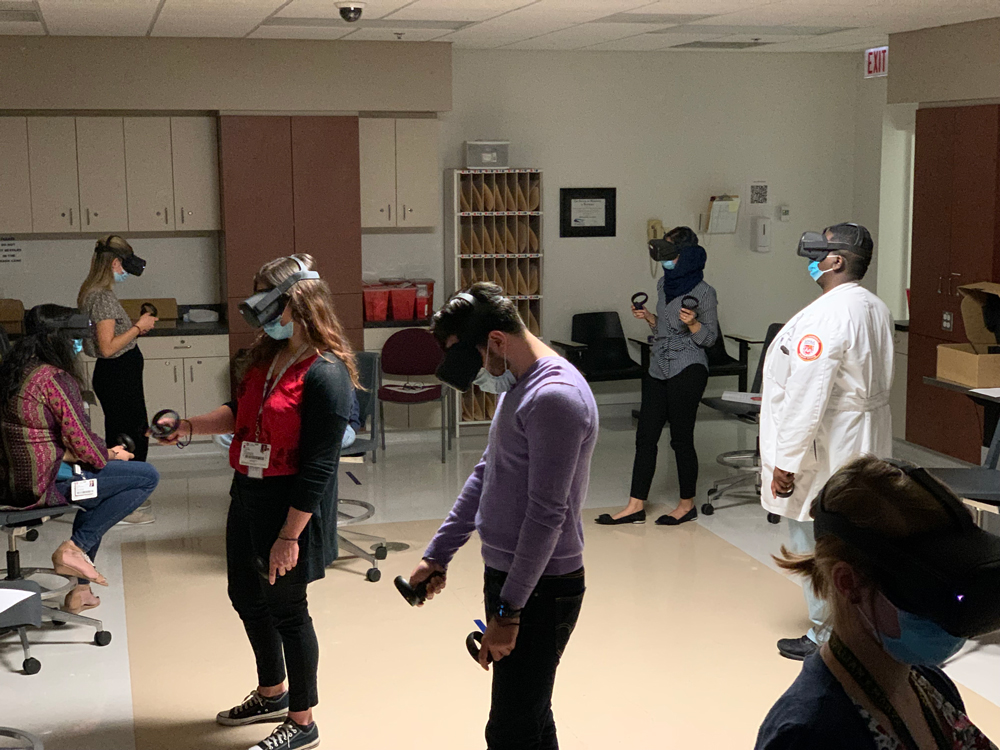

Source: Anuradha Khanna, MD
“I had more time, so I thought maybe we needed something more mobile,” she said, adding that this is how she began to develop the module now known as OcuSim. Dr. Khanna made the technology compatible with the Oculus headset and found the option was well received. The company donated a number of headsets to her university.
Immersing students in the eye can help prepare them with the fundamental concepts, Dr. Khanna said. “They can go in and look at every structure,” she said. “Then when they read [ophthalmology textbooks], they garner a lot more information in the first read of the book, and they’re understanding more than just the basics in a lecture and can get concept clarity.”
In terms of others who have developed similar technology, Dr. Khanna said there has been some success in surgical procedures. But her aim is to take a step back to examine the anatomy, physiology, and what the disease looks like clinically.
OcuSim allows residents to review structures of the angle, which offers experience prior to surgical wet labs. They can use the technology in the classroom on their own, she added.
Dr. Chaku teaches the glaucoma curriculum to residents at Loyola University and said she is excited about OcuSim. She noted the importance of understanding the mechanism of action of the disease and how to decide which treatment option to use.
Having the connection between seeing and understanding the concept so they know how to treat what’s going on in the eye is important, she said. “I review the Basic and Clinical Science Course Glaucoma textbook from the American Academy of Ophthalmology with the first-year classes, and I always tell them to look at the pathway and [understand] the anatomy and pathophysiology behind the specific disease. Now, using OcuSim, they can immerse themselves and go into the eye, into the angle, and understand why patients have glaucoma,” Dr. Chaku said. MIGS is an exciting space, she added, and it’s important to understand why we’re in the angle and why we’re getting lower pressures with new devices and treatments. “It gives them that concept clarity on why to choose specific treatments for different patients.
“It puts things together in a different way that we haven’t been able to do before,” Dr. Chaku said.
Dr. Khanna added that at Loyola, the simulation training is embedded into the curriculum. Dr. Khanna said that she often finds herself learning from trainees about the technology, and students are eager to continue on past individual modules that they’re working on. This teaching option incorporates visual, tactical, and audio learning. “As I’m creating it, I’m learning what these VR headsets are capable of and slowly introducing more interactivity,” Dr. Khanna said. “The more we do it, the more the residents use it, the more ideas come up.” The main limiting factor is money, she added.
Dr. Khanna said she does not have information on the specific procedures, like MIGS, in her lessons yet but she would be open to working with companies in the future. “Their product, they know best, and how to teach the residents, the educators know best, so we can merge the two worlds,” she said.
Dr. Khanna noted that there are many potential applications for her technology in the future as new procedures are developed. She thinks it could be valuable not just to trainees but also for those trying to keep their skills fresh. She has plans to develop a retina module as well.
The way she has designed the simulation is as if the participants are in a virtual study room, with the ability to teleport themselves into different parts of the room and look at the eye from different angles. In the future, she intends for them to be able to transport to different subspecialties and to the clinic.
With the advent of MIGS, the secondary effect is people are paying more attention to the angle, and from an educational standpoint, that has exploded the learning curve in that space, Dr. Chaku said.
“The reason I was so excited about OcuSim is because [it] gives a higher level of understanding and clarity to the residents that you can’t always draw out from a book,” she said.
Dr. Chaku added that this makes a difference because many people think that glaucoma is all about the pressure. But glaucoma is trying to figure out the right diagnosis and why we’re instituting this therapy, what’s the next step, and why will it work in this patient. “If you don’t understand that from a basic science/anatomy level, you’ll never give the patient the full treatment value,” she said.
In the future, Dr. Khanna hopes to expand the technology even more. For example, she said the next phase is to be able to incorporate individual case presentations.
Dr. Chaku added that since there are different training modules in glaucoma, it will be helpful to gives trainees different scenarios that they can examine in OcuSim and understand what’s happening and determine treatment plans. “We’ve been so excited about this technology,” she said. “We’re such a high-tech field and pushing the education envelope is exciting, and it allows us to do the best we can to get the next generation trained.”
About the physicians
Meenakshi Chaku, MD
Glaucoma Service Director
Loyola University Medical Center
Maywood, Illinois
Anuradha Khanna, MD
Vice Chairperson of Education
Department of Ophthalmology
Loyola University
Chicago, Illinois
Relevant disclosures
Chaku: None
Khanna: OcuSim
Contact
Chaku: MEENAKSHI.CHAKU@lumc.edu
Khanna: anuradha_khanna@hotmail.com




