Refractive: Complicated cases
September 2023
by Liz Hillman
Editorial Co-Director
A patient who elected years ago to have refractive surgery is no longer seeing as well and learns they have ectasia. In many cases their vision can be preserved and/or improved. EyeWorld spoke with Steven Greenstein, MD, William Trattler, MD, and Blake Williamson, MD, about how they address corneal and refractive issues for these patients.
Dr. Trattler said the biggest determiner for these patients still being able to see well is catching their ectatic condition early. “The earlier you catch these patients, the better because they will have less vision loss when diagnosed, and treatments can stabilize and often improve vision,” he said.

Source: Steven Greenstein, MD
Dr. Trattler said he recently saw a patient with post-LASIK ectasia who was 20/60 uncorrected in their better eye when ectasia was diagnosed in 2020. This patient, now 3 years after undergoing crosslinking, had improved to 20/25 without glasses.
“Crosslinking improves the corneal shape in the majority of patients,” Dr. Trattler said. “If ectasia is not identified until it is quite advanced, even after crosslinking and other procedures, patients likely will need to use advanced contact lenses to achieve their best vision.”
If a patient’s uncorrected or best corrected vision with spectacles is not satisfactory after crosslinking, Dr. Trattler said scleral contact lenses are often the first line of visual correction. He said scleral contact lenses are a “very reliable and highly successful method for improving vision in patients with irregular corneal shape due to ectasia.”
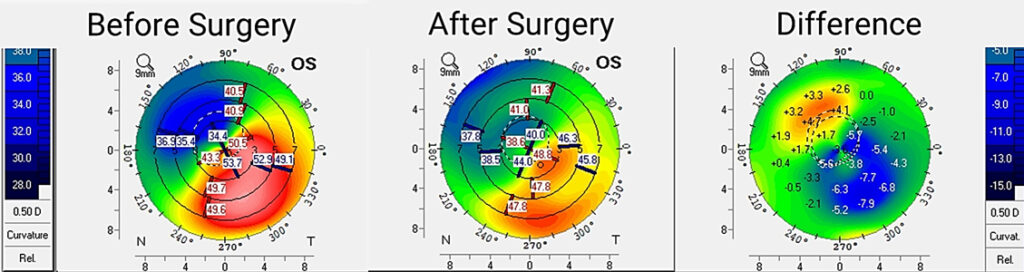
Source: Steven Greenstein, MD
Dr. Greenstein said the approach for the patient with ectasia after refractive surgery is similar to that for a patient with keratoconus. “It starts with establishing corneal stability through crosslinking, addressing corneal curvature, then visual improvement,” he said.
“We try to address all three of those things, set a plan for the patient moving forward, and create the realistic expectations about what we can do for their vision,” Dr. Greenstein said.
He said that depending on the thickness of their cornea and severity of the disease, topography-guided PRK could be an option. A literature review published in 2019 described studies that found crosslinking combined with or followed by topography-guided PRK or transepithelial PRK were effective at “providing corneal stability as well as significantly improving functional visual acuity.”1 At the time, the authors wrote that more data was needed on the long-term stability of the combined technique, as well as long-term studies on endothelial cell counts.
Other methods to regularize the cornea include Intacs (CorneaGen) and corneal tissue addition keratoplasty (CTAK, CorneaGen). Dr. Greenstein said he primarily does the latter. It uses sterilized corneal tissue that is shaped and placed into a laser channel to reshape the cornea. If the patient’s disease is too severe or if they have too much scarring, a corneal transplant (hopefully lamellar) is an option, he said.
If the patient is eligible for cataract surgery, there are lens-based options that could improve their vision (again after crosslinking and stabilization). Dr. Greenstein said he has had success with reshaping the cornea (with CTAK or topography-guided PRK) prior to cataract surgery. He sees a role for monofocal and toric lenses and blended vision and monovision options. Drs. Greenstein and Williamson mentioned the utility of an adjustable IOL, like the Light Adjustable Lens (LAL, RxSight), due to the ability to fine tune vision postop. They all mentioned the utility of the IC-8 Apthera IOL (Bausch + Lomb). Dr. Greenstein and Dr. Williamson advised caution when it comes to multifocal lenses with these patients, though Dr. Williamson said some patients might be eligible for Eyhance (Johnson & Johnson Vision) or Vivity (Alcon).
Dr. Williamson said he thinks the LAL in both eyes or the IC-8 Apthera in the non-dominant eye and LAL in the dominant eye are good for patients who have 2–2.5 D of cylinder. If there is more cylinder, like 3–4 D of irregular cylinder, Dr. Williamson said he might use bilateral IC-8 Apthera off-label.
“It can clean up coma and some of the higher order aberrations that you typically see in those post-refractive ectasia patients,” he said.
In addition to selective choice, Dr. Williamson said factors for achieving on-target cataract surgery still apply. These include making sure you have a good informed consent that “gives you plenty of runway to achieve a reasonable result,” using the right tools (accurate measurements with multiple devices confirming degree and power of astigmatism, updated formulas), and appropriate lens offerings.
Monitoring for progression is especially important for patients with keratoconus or post-refractive ectasia. Dr. Trattler said while crosslinking is highly effective at strengthening the cornea, a small percentage of patients can still progress. Known risk factors for progression include continued eye rubbing and advanced ectasia. “The good news is that most patients with ectasia will not progress after a single crosslinking procedure. However, patients need to be seen every year after crosslinking to ensure that their corneal shape is stable or improving,” he said. “In our experience, when progression is identified after a previous crosslinking procedure, a second crosslinking procedure is quite effective at preventing further progression.”
Dr. Greenstein presented 10-year results of crosslinking with patients who had topography-altering surgery (PRK or Intacs) compared to those who didn’t at the 2023 ASCRS Annual Meeting. Overall, there was stability 10 years after crosslinking (76.7% of eyes were stable) with no significant differences in eyes that had subsequent topography-altering surgery. However, eyes with keratoconus that received crosslinking were less likely to progress later compared to eyes that had crosslinking for post-refractive surgery ectasia; 86.7% of eyes with keratoconus that had crosslinking remained stable at 10 years postop compared to 66.6% of eyes that had crosslinking for post-refractive ectasia.
“This is why it’s important to tell those patients: 1) They need crosslinking done to stabilize their cornea now, and 2) they need to be monitored for the rest of their lives to make sure they don’t need repeat crosslinking down the road,” Dr. Greenstein said.
About the physicians
Steven Greenstein, MD
Medical Director
Cornea and Laser Eye Institute
Teaneck, New Jersey
William Trattler, MD
Center for Excellence in Eye Care
Miami, Florida
Blake Williamson, MD
Williamson Eye Center
Baton Rouge, Louisiana
Reference
- Al-Mohaimeed MM. Combined corneal CXL and photorefractive keratectomy for treatment of keratoconus: a review. Int J Ophthalmol. 2019;12:1929–1938.
Relevant disclosures
Greenstein: CorneaGen, Glaukos
Trattler: CXLO, Glaukos, Oculus
Williamson: Glaukos
Contact
Greenstein: sgreenstein@vision-institute.com
Trattler: wtrattler@gmail.com
Williamson: blakewilliamson@weceye.com