Dry Eye and Ocular Surface Disease Bonus Issue
October 2025
by Ellen Stodola
Editorial Co-Director
When considering patients with dry eye, it is imperative for physicians to understand the types of dry eye disease in order to best address a patient’s issues and choose an appropriate treatment. Vincent de Luise, MD, and John Sheppard, MD, discussed in depth dry eye sub-types and their identification.
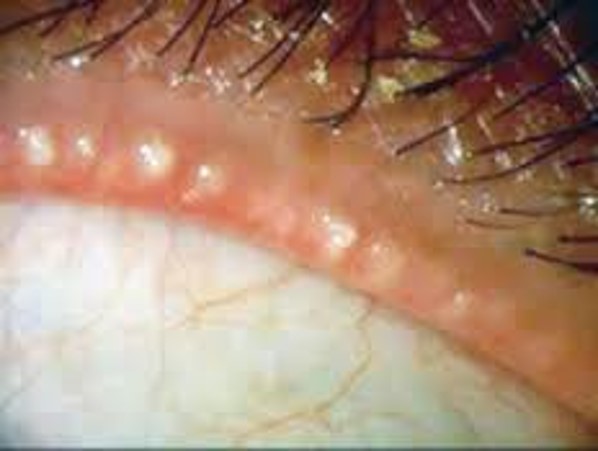
Source: Vincent de Luise, MD
Ocular surface diseases can be referred to by many names, Dr. de Luise said. These include dry eye disease, tear dysfunction syndrome, dry eye syndrome, and keratoconjunctivitis sicca. The 2017 Tear Film and Ocular Surface Dry Eye Workshop II (TFOS DEWS II)1 consensus is that dry eye disease (DED) is an ocular surface condition in which evaporation-induced tear hyperosmolarity is a trigger for a cascade of events leading to ocular surface damage, tear film instability, and inflammation, he said.
There are two basic forms of dry eye disease. Aqueous deficient dry eye (ADDE) disease is a result of reduced basal tear secretion (accessory lacrimal glands), and evaporative dry eye (EDE) disease is the outcome of excessive tear evaporation, most often from meibomian gland dysfunction (MGD) and lipid dysregulation, or from mucin abnormalities from goblet cell dysfunction or exposure, Dr. de Luise said. “There is also a neuropathic aspect to dry eye disease, with dysfunction of corneal nerves being another component.”
While we tend to think of aqueous deficient dry eye disease as inflammatory and evaporative dry eye as mechanical (especially if the underlying cause is meibomian gland dysfunction), it is important to remember that both of these DED types have inflammation as a major part of their underlying etiology, he said. “In addition, DED in any given patient is not uncommonly heterogenous, displaying symptoms and signs of both DED types.”
Furthermore, Dr. Sheppard noted that the TFOS DEWS II report acknowledged the significance of neurosensory abnormalities in the genesis of DED and the importance of afferent trigeminal signals regulating the production of aqueous, lipid, and mucin tear film components.
Dry eye disease is common, Dr. de Luise said, noting that more than 100 million Americans have symptoms referable to DED, about 40 million have been diagnosed with DED, and about 20 million who have been diagnosed are thought to have sufficient insurance coverage to start and stay on a prescription DED medication for a length of time. He mentioned that only about 2.5 million of the 20 million are on an FDA-approved DED medication.
There are several reasons for this disconnect, Dr. de Luise said. First of all, some patients are not aware of treatment options. Other patients are not that symptomatic. These patients may find relief and improved visual quality with relatively simple strategies, such as over-the-counter (ideally non-preserved) artificial tears and gels, environmental modification and ambient humification (cold air humidifiers), hydration, reduction in daily contact lens wear time, and frequent blinking. “Some have found a benefit to altering their diet to include more omega-3 FFAs,” Dr. de Luise said, noting leafy greens and wild-caught salmon. Oral fish oil supplements or oral flaxseed supplements may provide value.
Dr. de Luise said other patients may achieve DED symptom relief from episodic pulse therapy with off-label topical loteprednol etabonate for aqueous deficient DED flares or from topical azithromycin off-label or oral doxycycline or minocycline off-label for evaporative DED.
Most patients with DED have the evaporative type, Dr. de Luise noted. “A majority of patients who are being evaluated for cataract surgery have underlying DED (usually MGD) or another type of ocular surface disease, and many may not even be aware.”
Dr. de Luise said that both aqueous deficient dry eye and evaporative dry eye can present in similar manners, with overlapping symptoms and signs.
Dr. Sheppard agreed that there is frequently overlap between the two types. “It’s pretty rare that a patient is exclusively one or the other,” he said, adding that you need to look at the spectrum. In that spectrum are various levels of dysfunction in the integrated, interdependent components of the ocular surface unit.2
He added that many doctors and clinicians prefer to use the term “ocular surface disease,” which can be confusing to patients. Patients want to hear “dry eye,” and we want them to hear “dry eye disease,” he said, adding that this is not something to be taken lightly. DED is not just a condition. It’s a complex, multifactorial disease that requires astute analysis and data collection, then strategic intervention, Dr. Sheppard said.
In general, Dr. de Luise said that patients with predominantly or purely aqueous deficient dry eye disease present with blurred or fluctuating vision, sometimes with increasing blurriness as the day progresses (due to evaporation), burning, stinging, tired eyes, and foreign body sensation. They may present with lissamine green (or fluorescein) corneal and conjunctival staining, a thin to absent tear meniscus, low Schirmer testing, and an elevated and/or asymmetric tear film osmolarity.
Meanwhile, patients with predominantly or purely evaporative dry eye, which Dr. de Luise said is most commonly meibomian gland dysfunction and less commonly a goblet cell deficiency with mucin quality issues or from exposure changes, often present with blurred or fluctuating vision. Their vision is usually worse in the morning than later in the day due to the overnight action of bacterial lipases, which create a buildup of soapy oils. “There is often a marked decrease in tear film breakup time (normal is >10 seconds), corneal staining, a tear meniscus that even if not thin is often admixed with debris, cheesy to inspissated to caked meibum on lid margin compression, and/or keratinization of the meibomian gland orifices,” he said.
How do you approach these patients?
All types of dry eye require a similar starting point, Dr. de Luise said. He and Dr. Sheppard agreed that a thorough history is crucial.
Once you’ve figured out your global classification, you need to collect a lot of data, Dr. Sheppard said. The entire history is important, he said, emphasizing that patients should share past surgical interventions, like lid or corneal surgery and surgery that involves vital organs. These are all important so you can target your therapy, he said. Other factors like occupation, environmental exposure, heating/AC preferences, allergies, fan use, etc., are also important. Having a great staff can be an asset when it comes to doing this patient workup, Dr. Sheppard said.
In addition to a thorough history, the exam is a crucial piece. This should include evaluating blink rate, knowing if the patient is neurotrophic, if they have rheumatoid arthritis, and looking at the tear film, lids, meibomian gland orifices, and the lacrimal apparatus are all key.
Dr. Sheppard said he also wants to assess the sensation of the corneal nerves, but this test is rarely done on the first visit because the patient has usually had a pressure check and has been given an anesthetic.
Dr. de Luise added that it’s important to ask about topical and systemic medications and any associated systemic diseases, such as Sjögren’s disease.
He finds that ocular surface disease questionnaires can be useful. It’s also important to examine the lids and lashes for the presence of lash base collarettes diagnostic for Demodex mites. “Look at meibomian gland health and meibum quality; assess the meibum on lid compression to see if it is liquid or if there is inspissation and/or orifice plugging/caps and keratinization,” Dr. de Luise said.
All types of dry eye have underlying inflammation as part of their etiology. It might seem intuitive to start an immunomodulator (cyclosporine, lifitegrast) on all dry eye patients, but Dr. de Luise cautioned that while immunomodulators work well for aqueous deficient dry eye patients, they have had mixed results in patients with evaporative dry eye, which is by far the most common type. “With today’s expanded armamentarium of medications and technologies, there is now a new era in DED management: targeting by subtype and symptomatology to better individualize DED treatment.”
It is imperative, Dr. de Luise said, for the clinician to establish the three pillars of the DED treatment paradigm:
- The presence of dry eye (is this DED or a masquerader; see page 28 for more on dry eye masqueraders)
- The type of DED (aqueous deficient, evaporative dry eye, exposure, or combined)
- The severity of DED
Treatment can then be initiated and stratified by DED type, symptomatology, and severity. Dr. de Luise noted various FDA-approved dry eye medications and different mechanisms of action, including immunomodulators, lipolytics, evaporation reducers, cold receptor agonists, and trigeminal nerve agonists, as well as technologies focusing on MGD, thermal pulsation, intense pulsed light therapy, low level light therapy, and punctal plugs.
While Dr. de Luise said there is no fool-proof strategy to effectively treat all types and severities of dry eye, especially the most severe forms that are usually seen in Sjögren’s patients, it is still valid and efficient to treat based on type and severity. “It is useful to consider the DED types as mild, moderate, and severe, and to use a step-wise strategy for treatment, starting with least invasive and proceeding to more invasive strategies,” he said.
Dr. Sheppard stressed the importance of managing the interventions for a patient. “To give a patient too many things to do is unreasonable,” he said. “We should pick out the most obvious therapeutic and the most obvious environmental intervention and move forward.” However, with this strategy, he said you also have to manage how quickly each treatment response will manifest. For example, a pharmaceutical intervention, like lifitegrast or punctal plugs, may be more fast acting than a nutritional/environmental intervention. “If you’re going to have multiple interventions, pick a quick onset and a gradual onset so you know what’s going on,” he said. Additionally, physicians will need to consider if they are trying to prepare a patient for surgery. In these cases, the dry eye may need to be addressed more quickly and aggressively.
Dr. Sheppard also noted the use of warm compresses, but he added that these have to be done chronically. There are also many lid wipes/massages available, and hypochlorous acid can be useful. He finds hypochlorous acid sprays or wipes useful for dry eye and blepharitis, as well as preop surgical preparation.
When the patient has components of both types of dry eye, it can be even more challenging. Dr. de Luise noted that one large study3 found that even though 50% of DED patients had a pure evaporative mechanism and 14% had pure aqueous deficiency, more than a third of patients (36%) had a mixed etiology of both aqueous deficient and evaporative dry eye.
An effective strategy is to determine which of the two major types is most prominent, and address that type first, Dr. de Luise said. “This strategy also makes sense given ongoing challenges in trying to get insurance coverage for a patient to obtain a specific DED prescription, let alone two (or more) DED medications.”
Future products
There are several dry eye medications in the pipeline that could potentially expand the ability to individualize treatment of dry eye based on type, symptoms, and signs. (This is not an exhaustive list and does not represent all dry eye medications currently being researched.)
- Reproxalap (Aldeyra Therapeutics): Aldeyra announced in May that its RASP-inhibitor, reproxalap, achieved statistical significance against vehicle comparator in the primary outcome sign metric of patient-reported ocular discomfort. Reproxalap is also efficacious for allergic conjunctivitis, making this the first agent to simultaneously treat both comorbid conditions other than steroids, Dr. Sheppard said.
- AZR-MD-001 (Azura Ophthalmics): This is a selenium sulfide keratolytic gel meant to be applied twice weekly to dissolve keratin and melt inspissated meibum. The Phase 3 study is looking at AZR-MD-001 in patients with clinical signs and symptoms of MGD, Dr. de Luise said, adding that there is no currently available FDA-approved medication labeled specifically for MGD.
- Lacripep (Tear Solutions): Lacripep is a stable, water-soluble, C-terminal synthetic peptide fragment derived from lacritin tear protein. Lacritin is a foundational ocular surface protein in normal tears that is diminished to absent in the tears of DED patients. Lacripep may also possess neuroregenerative properties and efficacy in neurotrophic keratopathy, a comorbidity often seen in severe cases of DED, Dr. de Luise said, adding that Tear Solutions has completed DED patient enrollment in the setting of Sjogren’s disease.
- OCS-02 (Oculis): This is the TNF-alpha inhibitor licaminlimab, which has anti-inflammatory and regenerative (anti-apoptotic) mechanisms of action, Dr. de Luise said. In the Phase 2b trial, OCS-02 demonstrated symptom improvement as early as 2 weeks.
- PL9643 (Palatin Technologies): According to Dr. de Luise, this is a melanocortin receptor modulator with rapid onset of action and symptom resolution across multiple DED endpoints. The MELODY-1 trial has been completed, and the MELODY-2 and confirmatory MELODY-3 clinical trials are planned. Dr. Sheppard noted that systemic administration of melanocortin receptor immune modulators is indicated for a wide variety of ocular inflammatory diseases, including severe keratitis, uveitis, and scleritis.
- ST-001 vezocolmitide (Stuart Ophthalmics): This is a collagen mimetic peptide that Dr. de Luise said selectively repairs disease-damaged ocular surface collagen and reduces oxidative stress and inflammation. A Phase 2 trial showed rapid relief of symptoms and improvement in tear function within 28 days.
- TP-03 (Tarsus): The acaricide lotilaner is being evaluated for use in meibomian gland dysfunction in ERSA and RHEA trials.
Dr. de Luise also mentioned Visomitin SkQ1 (Mitotech), a mitochondria-targeted antioxidant to treat dry eye disease by scavenging reactive oxygen species and inflammation; SURF-200 (betamethasone in Klarity vehicle, Surface Ophthalmics) for the treatment of acute dry eye disease; and GLK-301 (Glaukos), a topical ophthalmic pilocarpine-based cream for dry eye disease.
Several other companies, such as Kala Pharmaceuticals (KPI-012), Claris Bio (CSB-001), and Krystal Biotech (KB801) are evaluating topical growth factors for neurotrophic keratopathy, a complex corneal condition that can overlap with the corneal changes in severe DED, Dr. de Luise said. The Claris Bio hepatocyte growth factor provides additional potential benefits including anti-fibrosis and anti-apoptosis in the context of ocular surface and corneal healing, Dr. Sheppard noted.
“The DED pipeline has never been more robust, and along with the many DED medications that have been FDA approved over the years, ophthalmologists have an ever-increasing toolkit of effective strategies to begin to individualize DED therapy and target DED by type, symptom, and severity,” Dr. de Luise said.
“Our therapeutic strategies have become far more sophisticated than the early days of this century when topical cyclosporine was the only approved medication for DED,” Dr. Sheppard said. “We now have choices analogous to synergistic therapies for glaucoma or hypercholesterolemia.”
Article Sidebar
Dr. de Luise’s step-wise strategy for treatment
Aqueous deficient dry eye
Mild: Patient education, environmental modification, humidification, reduction in computer and cell phone use, reduction in contact lens wearing time, frequent blinking, dietary modification, and non-preserved eye drops and gels
Moderate: Short courses of a topical ester- based corticosteroid, followed by long-term topical non-steroid immunomodulators; after inflammation is reduced, consider punctal plugs
Severe: Moisture chamber goggles, oral secretagogues, autologous serum tears or allogenic platelet-rich plasma, scleral lenses, PROSE AMT lenses, and lateral tarsorrhaphy
Evaporative dry eye
Mild: Dietary modification to increase omega-3s, ambient humidification, lipid-based eye drops, or home-based eyelid warming
Moderate: MIEBO (perfluorohexyloctane ophthalmic solution, Bausch + Lomb) eye drops, pulsed courses of topical azithromycin, courses of oral minocycline or oral doxycycline, and eyelid warming and compression technologies
Severe: All strategies in moderate level, plus consider intense pulsed light therapy
About the physicians
Vincent de Luise, MD
Assistant Clinical Professor of Ophthalmology
Yale University School of Medicine
New Haven, Connecticut
John Sheppard, MD
Professor of Ophthalmology
Eastern Virginia Medical School
Medical Director
Lions Eye Bank of Eastern Virginia
Norfolk, Virginia
References
- Craig JP, et al. TFOS DEWS II Definition and Classification Report. Ocul Surf. 2017;15:276–283.
- Sheppard JD, Nichols KK. Dry eye disease associated with meibomian gland dysfunction: focus on tear film characteristics and the therapeutic landscape. Ophthalmol Ther. 2023;12:1397–1418.
- Lemp MA, et al. Distribution of aqueous-deficient and evaporative dry eye in a clinic-based patient cohort: a retrospective study. Cornea. 2012;31:472–478.
Relevant disclosures
de Luise: None
Sheppard: AbbVie, Alcon, Bausch + Lomb, Bio-Tissue, Claris Bio, Dompe, Mallinckrodt, Novaliq, Noveome
Contact
de Luise: vdeluisemd@gmail.com
Sheppard: jsheppard@cvphealth.com




