Cataract: Hot topics in ophthalmology
December 2022
by Ellen Stodola
Editorial Co-Director
Four surgeons discussed the importance of ergonomics in ophthalmology, including their personal experiences and how they arrange their clinics and ORs for better ergonomics.
Michael Snyder, MD

Source: Michael Snyder, MD
Dr. Snyder’s attention to ergonomics began more than 25 years ago when he heard a lecture from Bruce Wallace, MD. “He gave a talk on ergonomics and how young people should pay attention so we didn’t run into issues with back and spine disease,” Dr. Snyder said. At that time, he was advocating for tilting the microscope and the patient’s head about 30 degrees. The oculars are then farther lateral to the eye, so the surgeon does not have to lean into the microscope, Dr. Snyder said. The surgeon can sit with an upright spine rather than leaning forward. This also elevates the patient’s head relative to the floor, allowing the surgeon’s hands to be a little higher and their elbows to drop down. “When our elbows fall toward our sides, we’re not using any of the neck muscles to lift our shoulders,” he said. That’s more comfortable and puts less strain on the cervical spine.
Dr. Snyder said he learned these initial tips from Dr. Wallace’s lecture; they are fundamental and cost nothing to implement. Dr. Snyder also began tilting his foot pedals. Some prototypes have been created for this, but pedal tilt can be achieved by taping something to the bottom side of the far end of the foot pedal. “The advantage of tilting the foot pedals is that now the feet, rather than being in full extension of the ankles, are in the midpoint of the joint’s range of motion, the most sensitive position for any joint. When the feet are not in full extension, it also puts less stress on the lumbar spine.”
Next, Dr. Snyder turned his attention to the OR chair. Most surgical chairs don’t have great lumbar support, and the backs of the chair are often too wide, so they end up bumping the elbows of the sterile gown and contaminating the elbows. Dr. Snyder has been working with Haag-Streit to design a new surgical chair that has center back support that follows the contours of the lumbar spine and goes up into the thoracic spine.
Chair height is also important. “The surgeon should set their own chair height … and take the extra 3 seconds to raise or lower the patient so the bed in the OR and the slit lamp in the clinic are at a comfortable height,” he said. “Most ophthalmologists either lean down a little or lean up a little.” While this might be fine for a few minutes, Dr. Snyder said it becomes a problem when you’re doing it 50–100 times a day several days a week, decade after decade. Some operative microscopes and slit lamps have attachments that allow the surgeon to change either the angle of viewing or the distance the oculars extend laterally. When it comes to the slit lamp, Dr. Snyder said its basic design has been around for 150 years and it’s time for an update.
When considering heads-up microscope technology, Dr. Snyder mentioned several potential downsides that hopefully technology can overcome. These include the footprint and fixed positioning of the screen, the tower of the microscope sitting right in front of the eye (the surgeon has to look around the stack of the microscope, which requires them to either tilt their spine or turn their head), latency delays in the display system, and the dynamic range of the camera not being quite as good as the human eye.
Dr. Snyder mentioned Beyeonics, which pairs virtual reality glasses that are partially transparent with a microscope system. The Beyeonics technology avoids the issue of having to look around the stack of the microscope because the stack could be right in front of you and you can still see fine since the image is in the goggles-based headset, he said.
Jonathan Rubenstein, MD
Dr. Rubenstein has experienced firsthand the necessity of making changes due to progressive neck problems, which began more than a decade ago. He eventually developed a herniated cervical disc and needed a cervical discectomy and cervical fusion in 2008.
Ergonomics, he said, is an issue that’s getting more attention now than it has in the past. The slit lamp is one problem because you’re often in a position where you’re putting tension on your neck, he said. Additionally, the use of the microscope in the OR has the potential to cause neck and back issues. It is common for ophthalmologists to develop these neck and back issues, he said.
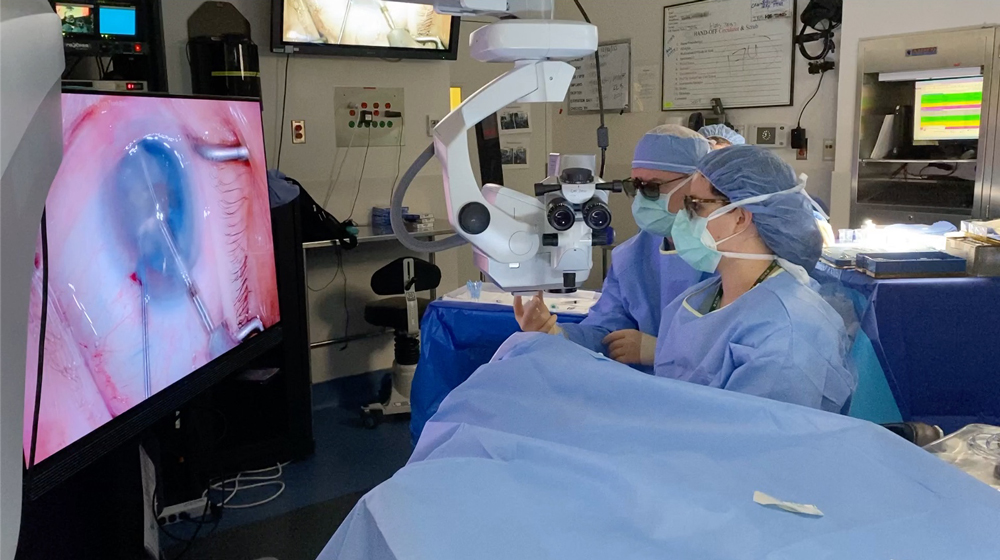
Source: Jonathan Rubenstein, MD
Dr. Rubenstein said his neck issues likely built up over time during his more than 30 years in practice. “I remember when I went to physical therapy, I thought I had good posture,” he said, adding that the physical therapist showed him the correct posture to realign his back and neck. “Therapy did not obviate the need for surgery, but it taught me [what to do] after surgery and how to maintain proper posture,” he said.
“I knew I had pain, but I didn’t think it was a big deal,” Dr. Rubenstein said. “I saw a neurosurgeon, and he tested the strength in my arms. I lifted my arms up, and he said, ‘Don’t let me pull your arm away.’ He then easily pulled one arm down as I was trying to resist, demonstrating a definite loss of strength.” As an ophthalmologist, you cannot risk motor problems affecting your arms and hands, he said.
Dr. Rubenstein started using the 3D heads-up microscope, which he thinks helped lessen his neck strain, but he also acknowledged that even heads-up microscopes have issues. They present other issues with posture, he said, because you tend to sit back like you’re in an easy chair, and although you’re relaxed, you might not have good posture. It’s not perfect, but he thinks it’s considerably less stress on the back and neck than a traditional microscope. He noted that there are a couple of options available in this space, the NGENUITY (Alcon) and the ARTEVO 800 (Carl Zeiss Meditec).
The heads-up technology provides a great intraocular view, Dr. Rubenstein said, and it’s good for teaching. “Everything the surgeons sees, everyone else in the operating room can see,” he said.
The disadvantages, however, are that there is more equipment that needs positioning in the operating room. The setup can be clumsy initially, and there is a learning curve for the surgeon and the OR staff. The extra HD monitor also tends to restrict access for anesthesia.
Dr. Rubenstein said there will likely be a number of advances in the future to improve heads-up microscope technology, including smaller monitors that can be mounted on the microscope stand. He also said there will be more components visible on the 3D screen and potentially virtual reality goggles that may obviate the need for the monitor.
Deepinder Dhaliwal, MD
Dr. Dhaliwal also has firsthand experience with posture problems from years of practicing ophthalmology. In 2015, she developed a disc herniation and a ruptured disc in her back. “I was actually in the OR and slipped on some water, and that was the final blow,” she said. “Two neurosurgeons and an orthopedic surgery were ready to do my discectomy.” However, Dr. Dhaliwal decided to take a more conservative approach after she was told by a radiologist that results after a year with conservative treatment versus surgery are the same.
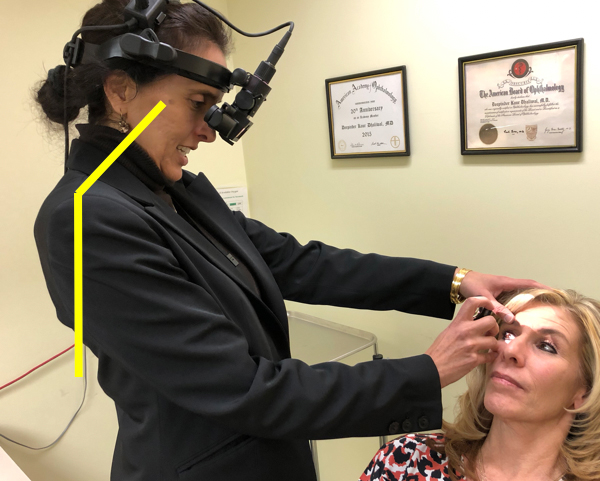
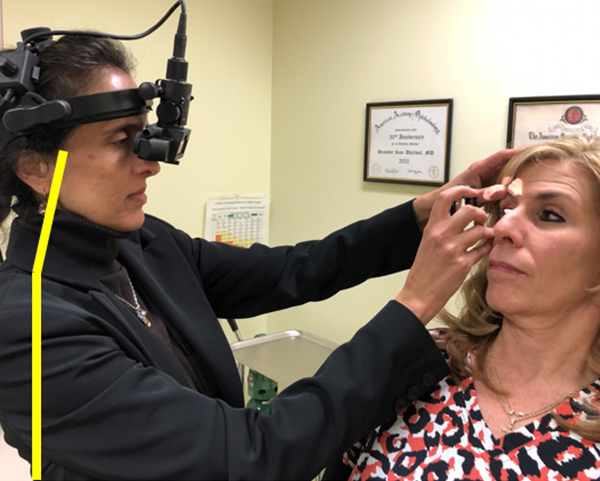
Source: Deepinder Dhaliwal, MD
“I started doing physical therapy, acupuncture, meditation, and I had to stop working because I was getting weakness in my right leg,” she said. “It was scary because I thought I was going to be disabled. This made me stop being a doctor, so it was a total wakeup call.” After doing therapy and other modifications, Dr. Dhaliwal said her symptoms gradually started to dissipate.
Dr. Dhaliwal still does physical therapy, and she said she wishes someone had taught her these things when she was a first-year resident. “The bottom line is that we all need to be mindful about our posture, about our instrumentation, about what we’re doing as we deliver care,” she said. “We’re so concerned about patients’ comfort and health, and over the years and decades, the toll that it takes on our necks and backs adds up.” The critical thing is to do an overhaul of the office, in terms of how you see patients, how you do surgery, and how you use certain instruments, she said.
One of the most important things, she said, is to work on having the neck over the shoulders over the hips and having a straight spine. In the office, when Dr. Dhaliwal is at the slit lamp, she has the patient move to the edge of their seat so she can keep her back straight. She then raises the exam chair and rolls her stool under the platform for their feet.
Sitting can get you into trouble with bad posture, Dr. Dhaliwal said. When sitting, you’re putting 200 times more pressure on the discs than when lying down; standing only puts 100 times more pressure on them. Dr. Dhaliwal said she tries to take “micro breaks” between every case. This involves extending her arms and shoulders back to reverse the posture she was in during surgery.
Dr. Dhaliwal emphasized the need for a good chair with lumbar support. She noted that she brings a lumbar support pillow everywhere she goes.
Dr. Dhaliwal has also tried the heads-up microscope technology but said she used an older version that was not comfortable for her neck. She said that she’s not as comfortable wearing the glasses needed for the heads-up microscope technology and prefers to make the chair and microscope modifications. However, she plans to try the technology again in the future.
She noted the focus in training on ergonomics. “I think people realize that you don’t want to stop practicing due to a disability.”
Jeffrey Marx, MD
While Dr. Marx has not had neck or back issues himself, he factored ergonomics into his career early. “My journey with ergonomics started when I was a junior faculty member at Lahey Hospital & Medical Center, and I was one of two retina specialists,” he said. “My partner, the other retina specialist, was out for a month for his first carpal tunnel surgery and a couple months later for a second surgery.” This prompted Dr. Marx to talk to his partner’s physical therapist about how he could avoid injuries, and he started working with physical therapists and other specialists to reduce his risk for problems.
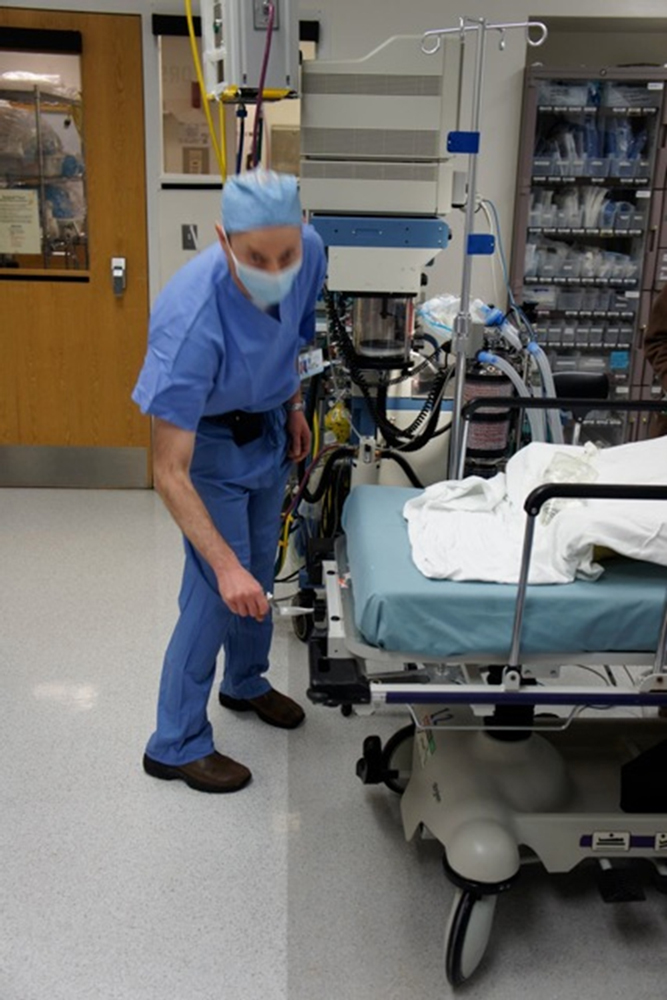
Source: Jeffrey Marx, MD
Dr. Marx said equipment is important and noted that one challenge is the size of the operating rooms and clinics and how much equipment needs to be positioned.
In terms of necessities, he always uses an elbow support. “It’s important to support the upper extremities when using lenses,” he said.
Dr. Marx is also very aware of the “competition” between the patient and the physician. “The patient wants us to move everything forward to them so that they don’t have to lean forward, and we want the patient to sit on the edge of the chair and lean forward so we can maintain upright posture,” he said. The back support of the chair is incredibly important, Dr. Marx added. “I look at all my chairs before I start the day and make sure that they’re for me,” he said, adding that he likes a certain chair for his laser procedures that many other colleagues don’t prefer.
While Dr. Marx said his practice hasn’t bought much new equipment, he did insist on ergonomic arms for the computer monitors.
In the OR, Dr. Marx said he has access to the NGENUITY system, but he prefers to use the traditional microscope. “I haven’t had neck pain in years after operating, and after a few times operating with the NGENUITY as the assistant, I didn’t like it,” he said. “I think it’s great and there are ergonomic benefits, but I personally don’t use it,” he said.
Dr. Marx uses a microscope from Carl Zeiss Meditec with extended oculars, which help him maintain a neutral posture with back support. It comes down to neutral posture, back support, and positioning yourself appropriately, he said. Pain is the warning sign that something in your daily life is causing you to potentially have problems down the road. Decreasing that risk at work is incredibly important, and the flip side of that is taking care of yourself outside of work as well. This includes factors like exercise, diet, good sleep, reducing stress, and building strength in various muscles so you can withstand the rigors of a long day.
About the physicians
Deepinder Dhaliwal, MD
Professor of Ophthalmology
University of Pittsburgh
School of Medicine
Pittsburgh, Pennsylvania
Jeffrey Marx, MD
Lahey Hospital & Medical Center
Burlington, Massachusetts
Jonathan Rubenstein, MD
Chairman
Department of Ophthalmology
Rush University Medical Center
Chicago, Illinois
Michael Snyder, MD
Professor of Ophthalmology
University of Cincinnati
Cincinnati, Ohio
Relevant disclosures
Dhaliwal: Haag-Streit
Marx: None
Rubenstein: Alcon
Snyder: Beyeonics, Haag-Streit
Contact
Dhaliwal: dhaliwaldk@upmc.edu
Marx: Jeffrey.L.Marx@lahey.org
Rubenstein: Jonathan_Rubenstein@rush.edu
Snyder: Msnyder@CVPHealth.com