Refractive Surgery
January 2007
by Maxine Lipner
EyeWorld Senior Contributing Editor
Investigators study how autoimmune patients fare with LASIK
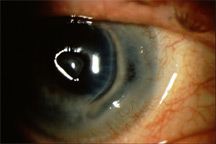
Source: Robert K. Maloney, M.D.
When it comes to LASIK, patients with autoimmune disease have long been on the “do not treat list.” Indeed, due to concerns about wound healing, the Food and Drug Administration (FDA) currently lists LASIK as a contraindication for those with autoimmune disorders. But are these concerns always founded? Not according to results of a study published in the August 2006 issue of the Journal of Cataract & Refractive Surgery. These study results show that LASIK can be a viable alternative for the right autoimmune patients.
Deciding whether or not to treat autoimmune patients is something that every refractive surgeon faces. “We all have patients who come in for refractive surgery consultations who have autoimmune disease,” said Robert K. Maloney, M.D., Los Angeles. “The question we ask ourselves is, ‘Is it safe to do refractive surgery on these patients?’”
Historically the answer has seemed to be a resounding no. The consensus has been that ocular surgery patients with certain autoimmune diseases, such as rheumatoid arthritis, are predisposed to corneal melting. “There are case reports in the literature where after cataract surgery, these patients develop corneal melting, particularly in the area of the corneal wound,” Dr. Maloney said. “Also, patients with certain autoimmune diseases can have spontaneous corneal or scleral melting.” As a result, many practitioners fear that performing refractive surgery in this population will stimulate new cases of corneal melting.
Studying autoimmune LASIK patients
In his own practice, however, Dr. Maloney had found that select autoimmune patients with well-controlled diseases actually had good outcomes with LASIK surgery. With this in mind, he decided to a launch a study to see if these results could be validated. For the study, investigators reviewed approximately 15,000 charts and culled those cases that involved LASIK patients with autoimmune connective tissue disease. They ultimately investigated 49 eyes of 26 patients and considered whether the patients had any of the corneal and scleral complications attributable to autoimmune disease after LASIK. “We got follow up on as many of the cases as we could, and of these 49 eyes, not a single one had autoimmune corneal or scleral melting,” he said.
Investigators concluded that LASIK, particularly in younger patients with well-controlled or inactive autoimmune connective tissue disease, is a reasonable option that appears to be safe.
The study results were in keeping with what Dr. Maloney had come to expect from such cases. “I had dealt with a number of patients with autoimmune corneal melting over the years,” he said. “I had become very comfortable both with managing it and, more importantly, in the understanding that autoimmune corneal melting tends to occur only in elderly patients and occurs almost exclusively in those with extra-articular disease.”
Selecting viable autoimmune candidates
In cases where rheumatoid arthritis only manifests in the joints, patients usually do very well with LASIK surgery. “It would be very unusual to have corneal melting in a patient without extra-articular disease,” Dr. Maloney said. However, such cases do occasionally occur, he said. He cites a study published by C. Stephen Foster, M.D., clinical professor of ophthalmology, Harvard Medical School, Cambridge, Mass., and co-investigators, published in the September–December 2002 issue of Seminars in Ophthalmology that showed that corneal melting following cataract surgery could be the first manifestation of extra-articular disease. These rare cases do not tend to happen out of the blue. “This tends to happen in much older patients,” Dr. Maloney said. “Also, it almost always occurs in patients where the disease is active and not well-controlled.” In general, the patients to whom Dr. Maloney offers LASIK are those who are relatively young, with well-controlled disease and good tear function.
“Another thing that is making LASIK more viable in these patients is the use of Enbrel [etanercept, Amgen/Wyeth, Thousand Oaks, Calif.] and other immune response modulators,” Dr. Maloney said. “This is a new class of drug that has revolutionized the treatment of rheumatoid arthritis.” As a result of these new medications, Dr. Maloney finds that the disease is less damaging and far better controlled than it was a decade or two ago.
In fact, the key to succeed with LASIK in such patients is to make sure that the disease is well-controlled. One way to determine this is by talking to the patient’s rheumatologist. However, it is the patients themselves who can be the most helpful. “Generally, the best way is to find out from the patient that they’re relatively symptom free and that their medication regimen has been stable for some period of time … while they have been under the care of a rheumatologist,” Dr. Maloney said.
Proper informed consent is also crucial. Before allowing any autoimmune patient to undergo LASIK, Dr. Maloney has a frank discussion where he explains that many surgeons consider the disease to be a contraindication for LASIK due to the potential for corneal melting. “I’m very explicit: I say that the cornea can melt through and leak out,” he said. “Then I explain the evidence both ways and allow them to make the decision.” In at least half of cases, patients forgo the procedure after hearing the risks. The remaining patients evaluate the risks themselves and decide to go ahead.
While LASIK can be a good bet for many of these patients, the study results should by no means be extrapolated to PRK, Dr. Maloney stressed. “We didn’t test the safety of PRK in these patients,” he said. “There’s reason to suspect that PRK may be less safe than LASIK in these cases.” Among other concerns, PRK creates a large epithelial defect. As non-healing epithelial defects are a cause of ulceration. There is the concern that such epithelial defects may predispose these patients to ulceration.
The study results also have no bearing on whether or not such patients are at increased risk of dry eye. A prospective study would be needed to determine this, Dr. Maloney said.
Overall, he recommends that practitioners not rule out LASIK surgery pro-forma. “I’d suggest that surgeons keep an open mind about LASIK in patients with autoimmune disease because for many people, it is really a wonderful enhancement to their life, just as it is for people without autoimmune disease,” he said.
Editors’ note
Dr. Maloney is a consultant for Advanced Medical Optics (AMO, Santa Ana, Calif.), Calhoun Vision (Pasadena, Calif.), and Bausch & Lomb (Rochester, N.Y.).
Contact Information
Maloney: 310-208-3937, erussell@maloneyvision.com




