Refractive
December 2021
by Ellen Stodola
Editorial Co-Director
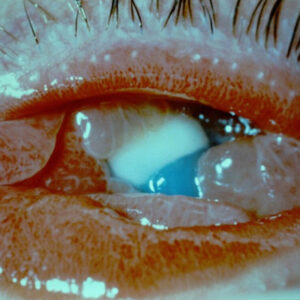
Epithelial basement membrane dystrophy (EBMD) can be seen in patients both prior to cataract surgery and after cataract surgery. Kourtney Houser, MD, said this is one of the more frequently diagnosed causes of blurry vision before or after cataract surgery, and it can be the result of long-term dry eyes.
While common, EBMD is often missed, so it’s important to look for it. “In all of my cataract evaluations, for people coming in with blurry vision, I always look for it, she said. “If I see it in the central 3 mm of the cornea, causing irregular astigmatism on topography, or see it in the center, I always treat before cataract surgery,” she said, noting that patients might not notice a benefit when they still have a cataract. It helps the surgeon to know how much astigmatism to treat with cataract surgery, making patients happier postop, especially when using presbyopia-correcting lenses, Dr. Houser said.
In addition to treating EBMD prior to cataract surgery, Dr. Houser said she gets a number of referrals for patients with blurry vision after cataract surgery. “I think a large percentage of people have undiagnosed EBMD and had a toric lens or multifocal put in and the quality of their vision is not good.” Unfortunately, Dr. Houser said that outcomes of treatment for EBMD following cataract surgery may not be as good as if it was treated prior because “if you correct astigmatism with the irregular cornea, it’s not always the right astigmatism.”
According to Amir Marvasti, MD, most patients with EBMD are asymptomatic. “Those who do present with vision quality complaints typically present for fluctuation in vision, double vision, or are sometimes being referred for a second or third opinion for dry eyes,” he said. “It’s crucial to have a high degree of suspicion for this condition for anyone who complains of blurry vision or fluctuation in their vision.”
Vance Thompson, MD, also encounters this epithelial blur problem frequently when dealing with EBMD patients. “The most powerful focusing element of the eye is the air/tear interface,” he said. “In a normal cornea, the epithelium is relatively smooth, which promotes a smooth tear film and makes for a smooth air/tear interface and crisp vision. If the epithelium is irregular, the tear film is irregular and light rays are focused irregularly, and it creates reduction in image quality.”
Other symptoms
Dr. Marvasti noted that patients with EBMD who are symptomatic can be divided into two groups: those who have vision quality issues (double vision, blurry vision, etc.) and those with episodes of pain and irritation from corneal erosion. “In my practice, this condition is most commonly diagnosed as an incidental finding during a routine eye exam, a refractive or cataract consultation, or those who present for ‘dry eye’ evaluation,” he said.
Dr. Houser agreed that EBMD can often present with subtle findings, and patients may not have symptoms. If there are a lot of changes, the cornea looks a little bumpy and irregular on the surface, she said, as well as the tear film. “If you have peaks and valleys in the epithelium where there are a lot of changes, there can be some corneal erosion over the changes, so those patients can present with dry eye symptoms, like watering or burning,” she said.
Diagnosing
Dr. Thompson noted that this is not always a problem that will be detected before surgery. Often changes in the epithelium can be seen at the slit lamp, but sometimes they can’t. “If a patient has reduced image quality and you do a refraction and can’t make the image clear, do a gas permeable contact lens over refraction, and if it gets clear, we know the surface is the cause,” Dr. Thompson said, adding that epithelial mapping may help with a diagnosis as well. “We can now map the epithelium and prove that it is the issue,” he said.
When diagnosing, Dr. Houser said she routinely will use corneal topography and a slit lamp exam. She noted that she doesn’t generally use epithelial mapping but said it can be a valuable technology to help identify EBMD.
“Corneal topography can help tell you how much it’s changing the shape of the cornea and in what part of the cornea,” she said. “But I still find that the best way to diagnose this is the slit lamp because you can have irregular topography from so many causes.”
Dr. Houser also likes to use corneal dye, but she said that it’s important to only use a little dye, applied with a strip. “I find if I use a combo of fluorescein and numbing drop, I can miss it because there’s so much drop in the eye that it will overwhelm the cornea,” she said. “If I put just a little dye from a strip in, I can see negative staining and find it so much easier.”
Dr. Marvasti said you don’t necessarily need any imaging device to diagnose EBMD, and he will often look for the characteristic map, dot, and fingerprint lines. He agreed that these findings will become more apparent with negative staining when a minimal amount of fluorescein dye is used.
“I do use imaging modalities, like topography and epithelial mapping, to document the refractive effects of this condition and to assess the effectiveness of treatment,” he said. “For example, I would capture topography before and after epithelial debridement to judge the success of the procedure.”
Lastly, Dr. Marvasti said he finds that showing patients an abnormal topography or epithelial map of their eye is an effective way to explain how the condition is affecting their vision.
Gas permeable lens over refraction
Dr. Thompson said that a soft contact drapes the irregular surface and does not help with the diagnosis, but a gas permeable lens is rigid and maintains its smooth shape. The tear film fills in between the contact and the cornea; then the air/tear interface is smooth because of the contact. “Since there is still refractive error, you put them behind the phoropter and do a ‘better #1 or #2’ manifest refraction, and if it gets crisper than when you refracted them with the contact in place, you know it is corneal surface related,” Dr. Thompson said.
Specialty contact lenses have both a therapeutic and a diagnostic role, Dr. Marvasti said. “In my practice, we mainly take advantage of the diagnostic aspect.”
A gas permeable lens over refraction can help narrow down the source of limitation in vision and either identify or rule out the cornea as the main site of pathology, he said. For example, in a patient with irregular astigmatism (ectasia, corneal scar, Salzmann’s nodule, etc.) and other ocular pathology (cataract, macular degeneration, etc.), he said a gas permeable lens over refraction will identify what the vision potential would be if the corneal shape and astigmatism were regular. “This will help us in counseling the patient and recommending the best next treatment modality,” Dr. Marvasti said.
Dr. Houser said she wants to know the potential of the patient’s eye, whether that patient is having cataract surgery or not. “Gas permeable or scleral lenses over refraction are useful to determine what the eye can see beyond the irregular cornea,” she said. “Whether the corneal changes are from EBMD or another disease, you can put a hard contact lens on, do refraction, and know what the potential of the eye is if you could fix the cornea and tear film.” Dr. Houser uses this before cataract surgery because it helps tell her how much of the vision change is due to the cornea.
Healing time and waiting before surgery
Dr. Houser said she likes to wait about 6 weeks after treating EBMD before proceeding with cataract surgery. Treatment like superficial keratectomy may be used in these cases.
“I tell patients 4–6 weeks, but usually I like to wait 6 weeks for the cornea to fully remodel,” she said, adding that some physicians may choose to wait 2–3 months. She also alerts patients that if they still have irregularity on topography, the wait may be longer.
Dr. Houser added that this is also a condition that can recur, though she said patients usually don’t need retreatment for some time. “It’s rare that I have to do retreatments within several years,” she said.
Dr. Thompson added that after doing epithelial scraping or PTK, it can take about 3 months for best vision to be restored.
Dr. Marvasti said for a patient with EBMD with multiple recurrences of corneal erosion or those with the dystrophy affecting the visual axis, he will typically recommend epithelial debridement with diamond burr polishing. “This treatment has worked the best for my patients, especially after failing other more conservative options,” he said. “The healing time can range from weeks to 1–2 months.”
Generally, Dr. Marvasti said he starts with more conservative treatment options, which can include ocular surface optimization with ocular lubricants, nighttime lubricating ointments, serum tears, amniotic membrane, hypertonic saline solution or ointment, bandage contact lens, and topical antibiotics for corneal erosions.
Surgical options, he said, include epithelial debridement with or without diamond burr polishing, PTK, and stromal micro-puncture. He again stressed that he typically uses epithelial debridement with diamond burr polishing for someone who has failed with more conservative options.
Dr. Marvasti noted that recurrence after surgical intervention is low, adding that he has not personally seen someone with recurrent corneal erosions after a thorough epithelial debridement with diamond burr polishing.
“The main point is always having a high degree of suspicion for EBMD in someone with fluctuation in vision, monocular diplopia, or anyone seeking to have cataract or refractive surgery,” Dr. Marvasti said. “As one of my mentors told me, ‘You’ll miss it if you don’t look for it.’”
About the physicians
Kourtney Houser, MD
Duke University
Durham, North Carolina
Amir Marvasti, MD
Coastal Vision Medical Group
Irvine, California
Vance Thompson, MD
Vance Thompson Vision
Sioux Falls, South Dakota
Relevant disclosures
Houser: None
Marvasti: None
Thompson: Alcon, Bausch + Lomb, Carl Zeiss Meditec, Johnson & Johnson Vision
Contact
Houser: kourtney.houser@gmail.com
Marvasti: amarvastimd@gmail.com
Thompson: vance.thompson@vancethompsonvision.com