For a more recent article on this topic, see “Handling dry eye prior to cataract surgery.”
Cover Feature: Dry eye
March 2012
by Faith A. Hayden
EyeWorld Staff Writer
What to use when all else fails
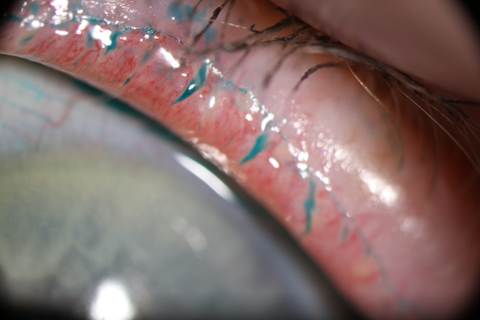
When pharma fails to relieve dry eye in the severest cases, patients still have options. Non-pharmaceutical treatments such as LipiFlow (TearScience, Morrisville, N.C.), autologous serum tears, and intense pulsed light are therapies proven successful for evaporative dry eye caused by meibomian gland dysfunction. Could one of these alternatives be the answer your toughest patients are looking for?
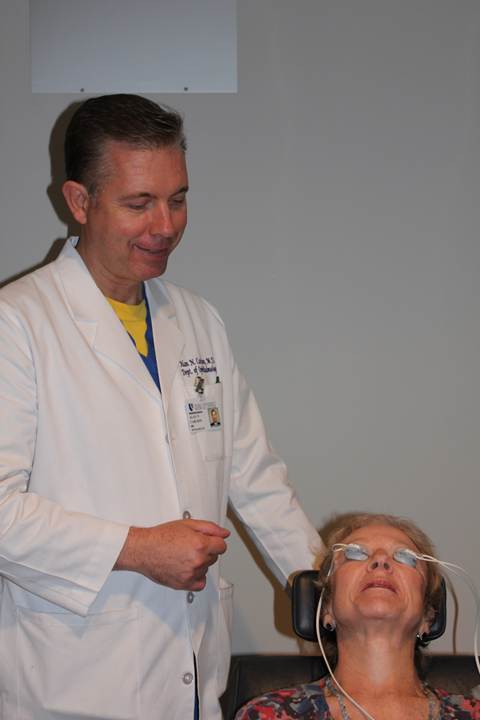
LipiFlow
LipiFlow is a three-part thermal pulsation unit consisting of the LipiView Interferometer, which assesses a patient’s tear film; a Meibomian Gland Evaluator, which evaluates meibomian gland secretions; and the LipiFlow, a disposable, sterile, single-use biocompatible component made up of a lid warmer and eyecup.
“The lid warmer generates heat directed onto both the upper and lower inner eyelid surfaces,” states company literature. “Behind the eyecup, an inflatable bladder pulses against the outer eyelids. The disposable fits under the eyelid, simultaneously delivering heat and pressure to both the upper and lower lids.”
“The initial treatment delivery heats to 42.5 centigrade, which is about 108.5 Fahrenheit, and does so for 8 minutes,” explained Alan N. Carlson, M.D., professor of ophthalmology, chief of corneal and refractive surgery, Duke Eye Center, Durham, N.C. “The initial 8 minutes delivers the thermal aspect of the treatment that liquefies the material hardened and obstructing the gland. The last 4 minutes of the 12-minute overall treatment is a pulsation that has a massaging or milking action on both the upper and lower lids that expresses the glandular material.”
Some patients can benefit from one LipiFlow treatment up to 2 years, while others will need another treatment every 8-12 months. Because LipiFlow is not currently covered by insurance, some patients may need to space out treatments for economic reasons.
“The cost of the equipment is $100,000, and our cost for the disposable unit is $700 per pair,” Dr. Carlson said. “It creates a substantial overhead.”
Dr. Carlson charges patients $1,500 per treatment and treats 6-10 patients a week.
LipiFlow is not recommended for patients with an active ongoing infection, recurrent corneal erosion, or a thin filtering bleb. Side effects include a red, irritated eye for 12 hours after treatment.
AST
Autologous serum tears (AST) can be extremely effective in alleviating dry eye symptoms in some patients, but should be considered a last resort, said David Glasser, M.D., Baltimore.
“The idea of AST is that it contains vitamin A and several growth factors that promote corneal epithelial healing,” Dr. Glasser explained. “Those factors remain stable at refrigerator temperature for a couple of weeks and in the freezer for a couple of months. It’s not simple to make because you have to draw blood, centrifuge it, and get it from the blood collection into a sterile eyedropper bottle without contamination. Those steps aren’t that complicated, but they need to be done in a sterile environment.”
Studies have shown the contamination rate can be upward of 40% for bottles cultured in an outpatient setting. The good news, however, is in those studies the contamination didn’t lead to clinical infection.
Finding someone to make AST can be a bit of a problem. Most compounding pharmacies won’t prepare it because it’s a biologic.
“Patients haven’t been tested for HIV and hepatitis, so most pharmacies are not going to want to touch it,” Dr. Glasser said. “If you’re at an academic center, you can have it done. Sometimes you can ask an eye bank to prepare it for you. [AST] can be helpful, but it’s not used frequently because of the hassle that comes with making it.”
Intense pulsed light
In 2002, Rolando Toyos, M.D., medical director and founder, Toyos Clinic, Memphis, discovered intense pulsed light (IPL), normally reserved for rosacea and skin rejuvenation patients, came with a happy side effect: It reduced the severity of dry eye symptoms.
“We started doing studies in 2004 to look at this further,” he explained. “What we saw in our studies is if we did IPL, patients systematically were getting better and their tear break-up time increased.”
IPL is suitable for patients with moderate to severe meibomian gland dysfunction.
“Essentially what we found when we did IPL on these patients [was] small abnormal telangiectasia that were around the gland were closed off,” he explained. “We found this light was absorbed in the dermal area, so it bypasses the epidermal and goes into the dermas. It melts these thick secretions and dilates the glands so we can do easy gland expression.”
Patients can have some relief from IPL alone, but to get the full effect of the treatment, Dr. Toyos recommended gland expression. Insurance does not cover the full cost of IPL. Dr. Toyos charges $400 a treatment, but other physicians charge up to $800.
Physicians interested in trying IPL for dry eye shouldn’t dust off any old IPL equipment lying around.
“When people read IPL helps with dry eye, they immediately want to take out an old system and try it,” Dr. Toyos said. “The problem is they’ll cause scarring on the face. It took us 7 years to configure an IPL system for dry eye. Most [IPLs] are made for photofacials, which is a lot of energy because you’re trying to stimulate collagen.”
African-American patients cannot have IPL because their skin could burn and lighten. IPL is an ongoing treatment program with patients receiving the therapy once a month until symptoms improve. Maintenance treatments are needed throughout the year.
Dr. Toyos expects to publish 3-year clinical follow-up data for IPL in the near future. Results, he said, are excellent. “More than 90% of patients that get the treatment have symptomatic relief,” he said.
Editors’ note
Dr. Carlson has financial interests with TearScience. Drs. Glasser and Toyos have no financial interests related to this article.
Contact information
Carlson: alan.carlson@duke.edu
Glasser: dbg@comcast.net
Toyos: rostar80@gmail.com