Cataract
December 2021: Complicated cases
by Liz Hillman
Editorial Co-Director
Iris prolapse can occur at any time during cataract surgery when the pressure inside the eye is higher than the pressure outside and when there is an open wound, said Michael Snyder, MD. There are certain conditions, he explained, that increase the potential for iris prolapse: light blue iris, poor dilation, short axial length, shallow anterior chamber, too short of a wound, too posterior of an internal incision, and/or excessive pressurization of the globe with too much OVD.
How commonly (or uncommonly) iris prolapse occurs is surgeon dependent, Dr. Snyder said.
“Mild prolapse may occur in double-digit percentages for some, while others may encounter this problem in only a fraction of a percentage. It is all about wound construction and attentiveness to micro-pressure gradients. As with so many things, prevention is the best management,” he said.

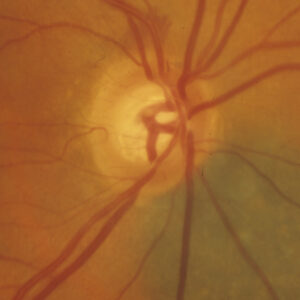
Source: Naveen Rao, MD
A case in point
Naveen Rao, MD, presented an example of a difficult iris prolapse case in nanophthalmic eyes. He followed up this difficult case with the second eye where he applied lessons learned from his experience with the first.
The case presented during the ASCRS Young Eye Surgeons Clinical Committee Complications by Proxy symposium at the 2021 ASCRS Annual Meeting involved a 75-year-old woman who was hyperopic, had shallow anterior chambers, prior laser peripheral iridotomy, and a BCVA of 20/80 in her right eye and 20/100 in her left.
Her first eye’s axial length was 20.24 mm with an anterior chamber depth of 2.02 mm. Dr. Rao said he used topical and intracameral lidocaine, but as soon as he made the paracentesis and injected “the tiniest bit of lidocaine, the eye turned rock hard.” There was iris prolapse through the paracentesis.
Dr. Rao tried to burp out some of the fluid, but the iris was plugging the incision. He said he was worried about the high pressure causing a CRAO, so he made a rapid temporal corneal incision to decompress the eye as soon as possible. It was a uniplanar incision, and immediately, iris prolapse occurred again due to the shallow anterior chamber and the architecture of the incision.
“Every time I would sweep the iris back in using a cyclodialysis spatula, it would come right back out,” he said.
He phacoed through the incision and said, in retrospect, he should have put an iris hook posterior to hold the iris subincisionally. He was able to phaco successfully but found IOL insertion difficult because the iris kept trying to prolapse through the incision.
He abandoned that incision, created a new incision superiorly, and successfully inserted the lens. Even when he was trying to suture the temporal incision at the end of the case, the iris continued to prolapse as he tried to pass the needle. A Sheets glide to hold the iris back was unsuccessful. In the end, there was significant iris atrophy temporally, which was later repaired with pupilloplasty.
Dr. Rao applied the lessons he learned in this case to the second eye, which had an axial length of 20.08 mm and an anterior chamber depth of 2.01 mm. This time he used general anesthesia and intravenous mannitol preop. There was less squeezing and posterior pressure from the patient at the start of the case. As he made the incision and inserted a little viscoelastic, the iris began to prolapse. He left the iris alone at this point, abandoned the original incision, and made a supero-temporal incision instead. He was able to phaco and put the lens in through this separate incision. This time he said he was able to sweep the iris back in with a blunt I/A tip. He said sometimes tapping on the roof of the incision can coax the iris back in when there is mild prolapse.
Leela Raju, MD, on the panel for the session, told Dr. Rao that switching to the other wound was a great idea.
“It feels like you’re failing but you’re not; you’re making it easier for yourself,” she said.
How to prevent iris prolapse
Whenever an eye is at risk for iris prolapse, Dr. Snyder said to stop irrigation and let the chamber shallow before removing the phaco or I/A tip. While this might sound counterintuitive, especially in shallow chambers, he said that if there is no pressure gradient for flow to occur out of the wound, the iris will not follow if there is no flow.
Other advice Dr. Snyder gave was to make sure the wound is carefully constructed with a slightly more anterior internal entry into the chamber and a longer tunnel. He also advised intravenous mannitol preop in eyes with short axial lengths and mentioned use of iris hooks to dilate and stabilize the pupil with one hook under or adjacent to the wound, which was described by Thomas Oetting, MD.1
“If the iris is tethered internally peripheral to and under the wound, it cannot prolapse out,” Dr. Snyder said.
What to do when the iris emerges
It’s first important to determine why the iris has prolapsed.
If it occurs due to a significant IOP increase from a suprachoroidal hemorrhage (SCH), Dr. Snyder said no action should be taken at the wound. In this case, he said, “the iris should be left plugging the wound and the SCH and underlying cause(s) should be identified and managed. The iris becomes secondary.”
If the cause of the prolapse is not due to an occurrence in the posterior segment, Dr. Snyder said the surgeon should reduce pressure in the anterior chamber before attempting to put the iris back.
“This can be done by aspirating aqueous or OVD from a paracentesis, giving intravenous mannitol, or rarely, converting to general anesthesia, if patient cooperation is the origin,” he said.
If/when the anterior chamber pressure has returned to at least somewhat below normal, Dr. Snyder said tapping on the roof of the corneal tunnel will usually drop the iris back in without any direct contact. However, in stubborn cases, he said the iris can be pulled into the anterior chamber with microforceps through a paracentesis on the other side. Gently grasp the iris internally and pull it into the AC, he said.
Dr. Snyder said pushing the iris with an instrument through the same wound as the prolapse is less effective and can cause more stromal or pigment loss.
Finally, he said another strategy when there is minimal prolapse after the chamber is depressurized is to use a gentle squirt of balanced salt solution external to the wound ostium. This can create an internally directed flow gradient and “blow” the iris in, he explained.
article sidebar
Continue the conversation
Share on ASCRS social platforms your tips/pearls for handling iris prolapse.
About the physicians
Naveen Rao, MD
Assistant Professor of Ophthalmology
Tufts University
School of Medicine
Boston, Massachusetts
Michael Snyder, MD
Professor of Ophthalmology
University of Cincinnati
Cincinnati, Ohio
Reference
1. Oetting TA, Omphroy LC. Modified technique using flexible iris retractors in clear corneal cataract surgery. J Cataract Refract Surg. 2002;28:596–598.
Relevant disclosures
Rao: None
Snyder: None
Contact
Rao: naveen.k.rao@lahey.org
Snyder: Msnyder@cvphealth.com