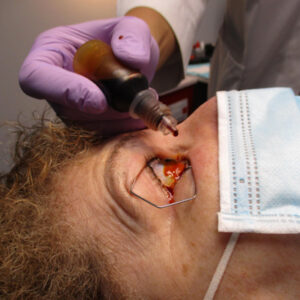
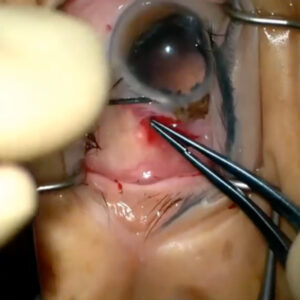
Cataract: YES Connect: Beyond the Routine
Fall 2025
by Ellen Stodola
Editorial Co-Director
Secondary IOL fixation is a hot topic and likely will be for as long as we are continuing to do traditional IOL surgery. It requires skill, patience, steady hands, an innovative mind, and experience to accomplish these effectively. But most of all, it requires a persistent dedication to doing these types of procedures and doing them well. This is because these procedures are at the pinnacle of difficulty in the field of anterior segment surgery. For anyone who has consistently done them, they know what kinds of complications can occur both intraoperatively and postoperatively. A surgeon who does secondary IOLs must be prepared to do multiple surgeries to get the lens just right. They must have a stout heart to prepare themselves for the numerous complications that occur, including ones like retinal detachments or choroidal hemorrhages that can cause a patient to lose vision or even lose the eye. The surgeon must be brilliant enough to figure out a solution to a problem that can occur within a few seconds during surgery and to be able to safely navigate their way out of it and produce an outstanding outcome despite the challenges. And finally, there’s a whole refractive outcome aspect that is equally challenging, and the surgeon must have the clinical acumen and empathy to walk the patient through the proper expectations for this type of surgery.
I have requested that these outstanding surgeons describe their techniques for how and when to successfully fixate a secondary lens when the capsule is either not present or not secure enough for traditional IOL implantation.
–Austin Nakatsuka, MD, YES Connect Guest Editor
Secondary IOL fixation can be used when the IOL is not in the right position, when there isn’t an IOL, or when there isn’t anything to fixate the IOL to in an ordinary way, said John Hart Jr., MD. When to proceed with this option depends on how the patient is functioning and any visual complaints.
Dr. Hart and David Crandall, MD, discussed techniques and lens considerations when choosing to do secondary IOL fixation.
“The most obvious situation for secondary lens implantation is when a patient is sent to me aphakic, most often from trauma or from a surgery that did not go well,” Dr. Crandall said. “These techniques are also valuable during cataract surgery and lens exchange if there is inadequate capsule support for in-the-bag or in-the-sulcus lens placement. Many patients who are aphakic, especially if it’s in one eye, can do well with contact lens correction but over time become intolerant to this approach and desire lens implantation. Some patients know from the get-go that they will not be able to do contacts.”
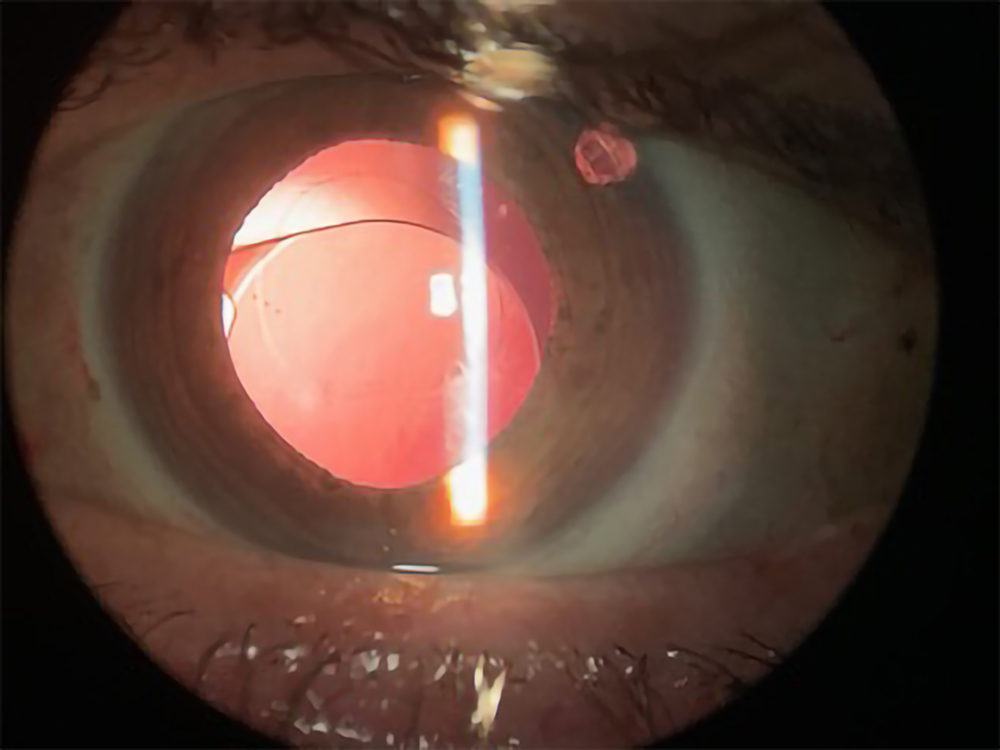
syndrome
Source: John Hart Jr., MD
Techniques
Dr. Crandall said the main secondary IOL fixation techniques that he utilizes are Yamane intrascleral haptic fixation and directly suturing a lens with polytetrafluoroethylene (Gore-Tex) sutures.
For most patients, either technique will work fine, he said. “For patients who have conjunctival scarring, I generally prefer the Yamane technique since that does not require me to open the conjunctiva. This is most common in patients who have had glaucoma surgery or retina surgery,” he said. However, Dr. Crandall noted that he would hesitate to use this technique in very high myopes since the wider distance can put extra tension on the haptics, which can lead to haptic breakage or predispose lenses to rotisserie lens rotation (the lens optic twisting on the haptic). He also said that the scleral passes of the needles need to be of equal length to make sure the entry points are 180 degrees apart. “Before burying the haptics, I like to keep about 1 mm of each haptic outside the eye and check the lens centration. If the lens is well centered but the haptic ends outside the eye are of unequal length, the longer one can be shortened until they are equal,” he said. “This way, the lens will stay centered when the haptics are buried.” Early on, almost everyone makes the bulb of the melted haptic much larger than necessary, he said, adding that it takes very little bulb creation to hold the lens securely. Additionally, a large bulb will be more prone to erosion. “I like to push the bulb in until it is completely flush with the sclera,” Dr. Crandall said. “I also will lift up the conjunctiva and Tenon’s to make sure they are completely free from the bulb.”
For scleral-sutured lenses, Dr. Crandall primarily uses enVista lenses (Bausch + Lomb) with the opening at the base of the haptic or the CZ70BD lens (Alcon) with the eyelet on the haptic. The CZ70BD lens is PMMA, so it requires a large incision. “I will lean toward this lens if I have a large corneal or scleral incision, often either in a patient who requires an extracap or intracap lens removal or a patient who needs an anterior chamber lens removed since they will already have a large incision.” When a toric or multifocal lens is an option, Dr. Crandall said the enVista platform works well as a sutured lens, so there are more lens options for this technique.
It is important not to overtighten the sutures, he added. “I like to use a slip knot, and slowly tighten each side until the lens is sitting in a good position, then lock the knots and bury them. It is critical to completely bury the knot. Any free ends of this material have a very high risk of causing a conjunctival erosion.”
Dr. Crandall also noted advantages of Yamane fixation, particularly minimal conjunctival manipulation, and once you have experience, it is a much quicker technique. Since there are only small needle passes, there is a lower risk of hypotony, he said.
“Advantages of direct scleral fixation are the wider range of lens options, and, in my hands, it has lower rates of tilting or decentration.”
For both techniques it is important to use infusion, Dr. Crandall said, adding that this can be either pars plana or anterior chamber infusion, to make sure the positioning, centration, and tension are right. Marking for lens placement is also critical, he said. The entry points of the haptics/sutures need to be directly 180 degrees apart from each other.
Dr. Hart noted that choosing the right fixation technique could also depend on where the original cataract implant was placed. “If the original lens was placed within the capsular bag, which is where these are FDA approved to be, and the zonules have given out, that’s one issue. That’s an in-the-bag IOL dislocation. That’s the most common thing we see these days, usually due to pseudoexfoliation syndrome or trauma,” he said.
Additionally, he noted the issue of dead bag syndrome, a more recently described term for when the lens capsule doesn’t seal around the implant, and all of the cells that would normally be involved with sealing, the lens epithelial cells, die off. The lens is rattling around inside the capsular bag, Dr. Hart said. When you have a dead bag, the lens can erode through the capsule. If that happens, the lens needs to come out, and you’ll need an entirely new way to fixate it. “Often those lenses with dead bags have bad zonules, so you can’t necessarily depend on the capsule or the bag for continued support.”

Source: John Hart Jr., MD
While Dr. Hart said he has used iris fixation in the past, he doesn’t use this technique as much anymore because of the higher incidence of CME.
“Now, predominantly, if it’s an in-the-bag IOL dislocation, I will suture to the sclera with Gore-Tex right through the capsule to the haptics.” He noted that you could also use 10-0 or 9-0 Prolene, but he finds these more prone to break over time.
Another option is the belt loop technique, Dr. Hart said, adding that this technique was coined by Cathleen McCabe, MD, and the original technique was developed by Sergio Canabrava, MD. This uses 6-0 or 5-0 Prolene to loop the haptics and use cautery.
Dr. Hart said he uses this technique but infrequently because he has concerns about erosion and whether the suture is going to hold up long term. However, when he has done the technique, it works. “It requires a little less dissection of the conjunctiva, but the other issue is the wound leak tends to be more common, and getting the right tension on sutures is more difficult.
“With sutures, Gore-Tex particularly, I’m able to adjust suture tension so the implant is better centered and not too tight and not too loose, which is very important,” Dr. Hart said.
He also noted the Yamane technique of intrascleral haptic fixation from an anterior segment approach and added that some retina colleagues perform a similar technique. This requires a 3-piece lens and haptics brought into the sclera, and the ends of the haptics are cauterized. “If there’s no zonular or capsular support, I do a Yamane technique,” he said.
If there’s adequate capsular or zonular support, putting a lens in the bag is still the way to go or putting it in the sulcus if you can’t put it in the bag, Dr. Hart said.
Dr. Hart said he will generally try to use the lens that’s already been working in the eye, as these problems are usually structural and not the fault of the lens. “Part of the problem is that anything that goes into the ciliary sulcus, you have to use a 3-piece lens because 1-piece lenses can cause UGH syndrome, and you don’t want to leave the patient with a potentially sight-threatening complication that you created,” he said.
To learn these techniques and to keep your skills fresh, Dr. Hart said there are wet labs on secondary IOL fixation at major meetings, including the American Academy of Ophthalmology Annual Meeting and ASCRS Annual Meeting. “Most of the people who do this on a regular basis are willing to teach,” he said.

Source: John Hart Jr., MD
Potential concerns
Dr. Hart said that all of these techniques have risks, including the risk of CME, retinal detachments, or retinal tears. When you’re working through the pars plana or in that area, you always have that risk.
For intrascleral haptic fixation, it’s required that you do a thorough vitrectomy, he said. The recommendation is that you do a pars plana vitrectomy, but you can do an anterior vitrectomy because the implant is going to be dangling into the vitreous cavity, and you don’t want it to be caught up in vitreous.
It’s also very important to be able to recognize dead bag syndrome, he said. If it is a dead bag, the lens and bag should be removed, and you should do intrascleral haptic fixation.
He added that when he first started doing secondary IOL fixation, he saw a lot more cases where there were problems with the lens in the sulcus and the haptics of the sulcus-fixated lens had eroded through the zonules. In those situations, we were suturing to the iris. “The downside is there’s a somewhat higher rate of CME,” he said.
There are all kinds of special circumstances, Dr. Hart said. “Some lenses create more problems than others.” For example, he said if you get Z syndrome with a Crystalens (Bausch + Lomb), it’s difficult to fix. They often need to be explanted, and Z syndrome causes damage to zonules.
He also noted that using a Yamane technique, you may need to look out for the risk of tilted IOLs or rotisserie syndrome (optic twisted on haptic).
“This is definitely a rescue. This is not refractive surgery,” he said. “People come in with multifocal or toric lens, and in those situations, it’s a lot more challenging to properly put that in from an intrascleral haptic fixation standpoint than to suture it in place.”

Source: John Hart Jr., MD
This takes patient counseling, he said. If the patient has a lot of astigmatism, taking out a toric that’s correcting a large portion of that can be a big issue for them. Even with multifocal lenses, people get used to them. There’s no 3-piece alternative to do intrascleral haptic fixation with.
“Since I do all of them, from a technical standpoint, fixation with sutures is easier technically than intrascleral haptic fixation,” Dr. Hart said. “I think for people looking to pick something up, it’s well within their skillset.”
Physicians often want to learn this in case something happens during cataract surgery, he said, adding that he explains that during cataract surgery is not usually when you want to perform this. “The calculations are different. Implants are different. It’s going to take you longer. You want to take your time. It’s not topical anesthesia anymore because it’s going to take longer. For most of these, I like to do general anesthesia so I know the patient is comfortable and will wake up seeing well.”
Dr. Hart added that he usually schedules secondary IOL fixation cases for the first case of the day. “I schedule them for an hour, but that’s counting the fact that I’m using general anesthesia,” he said. “These are things that can be planned. In the past, people were told, ‘Just put in an anterior chamber lens or throw in whatever lens you can after the cataract surgery,’ and I don’t think that’s the way we feel anymore because in a lot of cases, you’re going to be compounding the error.”
About the physicians
David Crandall, MD
Henry Ford Hospital
Detroit, Michigan
John Hart Jr., MD
Associates in Ophthalmology
Farmington Hills, Michigan
Relevant disclosures
Crandall: None
Hart: None
Contact
Crandall: dacrandall@gmail.com
Hart: j.c.hartjr@sbcglobal.net