ONLINE EXCLUSIVE
September 2021
by Liz Hillman
Editorial Co-Director
In the beginning of the COVID-19 pandemic, even when non-urgent clinic visits and elective procedures were, for the most part, halted in the U.S., Terrence P. O’Brien, MD, was still seeing 20–25 patients a day for essential care and urgent ocular needs.
“I was afraid of the unknown. I felt like I was a sitting duck against a novel, highly transmissible contagion,” he said, explaining that the up-close nature of ophthalmologists’ examinations with patients makes them particularly vulnerable.1
While many ophthalmologists were donning PPE, fitting slit lamp microscopes with shields, and instituting administrative changes that could reduce the risk and spread of SARS-CoV-2, Dr. O’Brien added another adjunctive preventative measure to his regimen: a dilute povidone-iodine drop for his patients and himself after in vitro studies confirmed virucidal effect against SARS-CoV-2.
“I would place a drop in each eye at the start and at the end of the clinic day. The hope was that enough would contact the ocular surface and migrate into my nose and nasal pharynx to be protective,” Dr. O’Brien said, noting that the eye has been established as a mode of entry for the virus and that it can harbor SARS-CoV-2 in its tissues as a portal for the eye-nasopharynx-lung axis.
While the U.S. has widespread vaccine distribution and adoption, which has resulted in some preventative measures being lifted in communities, Dr. O’Brien said that the use of 2.5% povidone-iodine could be a best practice to continue, not only for SARS-CoV-2 but against other transmissible viruses, like adenovirus, enterovirus, influenza, and even some bacteria.
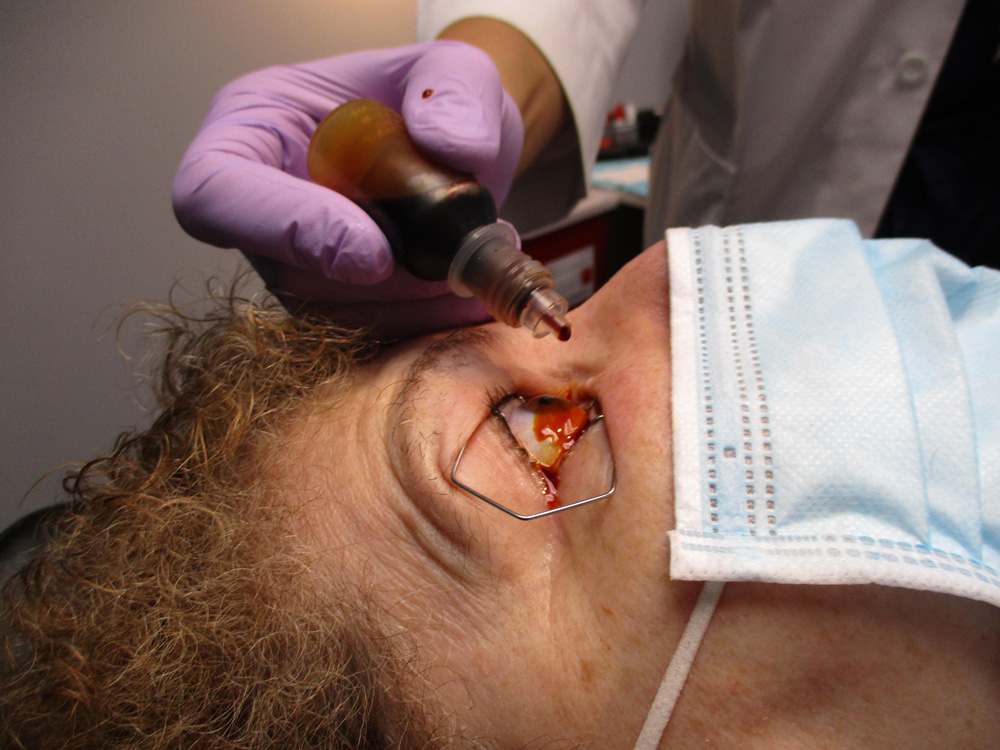
Source: Terrence P. O’Brien, MD
“Could this preventative practice go on even past the current pandemic? Yes, you could think of other viruses that could be thwarted from spreading. It’s such a simple, easy practice that is without significant side effects that even after vaccination one might consider applying it at the beginning of the day, end of the day, or both,” he said, adding that vaccines, though highly effective are not 100%, will have breakthrough cases, and there is still a significant proportion of the population worldwide that is unvaccinated for various reasons.
Dr. O’Brien and Jesse Pelletier, MD, published a perspective in the Asia-Pacific Journal of Ophthalmology on the use of adjunctive povidone-iodine for COVID-19 prevention.2 In the paper, Dr. O’Brien and Dr. Pelletier described the efficacy of povidone-iodine against SARS-CoV-2 and other infectious agents, the safety and other applications of povidone-iodine (such as intravitreal injections), and a recommended protocol for its use during the pandemic.
“… we recommend that 1 drop of PVP-I ophthalmic solution, preferably dilute, is placed on each patient’s eye prior to and after ophthalmic clinic visits, ocular procedures, and surgeries. When [healthcare providers] are unable to don eye protection, we recommend that they adopt the same strategy as well,” they wrote in the paper.
Dr. O’Brien re-emphasized the long track record demonstrating safety and efficacy of povidone-iodine in ophthalmology.
“It has been widely used in ophthalmic surgery for decades but is also used daily in ophthalmic clinics for prophylaxis with the millions of intravitreal injections administered annually. It is also used to prevent infections when removing sutures in the clinic. Many eye clinics have a protocol to use PVP-I with patients having suspected ‘pink eye’ to try to reduce transmission of adenovirus and other transmissible viruses,” he said.
From a cosmetic standpoint, Dr. O’Brien assured that the drops don’t leave an orange tinge in the eye. He also said that it doesn’t affect diagnostic testing or measurements, except perhaps assessment of the tear film and other dry eye metrics, which should be performed before any drops are instilled to the eye.
Dr. O’Brien described povidone-iodine antiseptic drops as a “simple, cost-effective, practical prevention against a potentially lethal occupational hazard.”
About the physician
Terrence P. O’Brien, MD
Professor of Ophthalmology
Charlotte Breyer Rodgers Distinguished Chair
Bascom Palmer Eye Institute
University of Miami
Miller School of Medicine
Palm Beach Gardens, Florida
References
- Kuo IC, O’Brien TP. COVID-19 and ophthalmology: an underappreciated occupational hazard. Infect Control Hosp Epidemiol. 2020;41:1207–1208.
- O’Brien TP, Pelletier J. Topical ocular povidone-iodine as an adjunctive preventative practice in the era of COVID-19. Asia Pac J Ophthalmol. 2021;10:142–145.
Relevant disclosures
O’Brien: None
Contact
O’Brien: tobrien@med.miami.edu