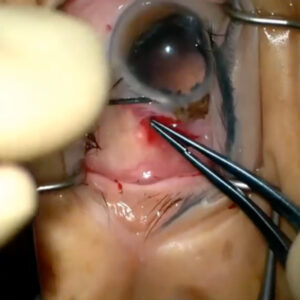
Glaucoma
Fall 2024
by Ellen Stodola
Editorial Co-Director
SLT has gained popularity in the treatment of glaucoma, and there are several new laser technologies and procedures in various stages of development. Richard Lewis, MD, and Inder Paul Singh, MD, spoke with EyeWorld about a few of the newer options and what they’re excited about.

Source: ViaLase
Dr. Lewis said that lasers in glaucoma have been utilized for his entire career for a variety of things including angle closure, YAG, and more. The most common use of laser has been for ALT or SLT, which is treating the trabecular meshwork for open angle glaucoma, Dr. Lewis said, adding that this has been used for around 40 years, evolving from ALT to SLT.
The LiGHT study1 looked at SLT and showed that it could be better and safer than medications because there are no compliance problems and a reduced incidence of side effects compared with incisional procedures. The problem with SLT is that its effect tends to wane over time, Dr. Lewis said, adding that this is why it’s important to follow patients to ensure the pressure is under control.
On the surgical side, there have been efforts for years to do minimally invasive surgery and create a trabeculotomy. “That’s what we’re doing with newer laser applications—such as with the femtosecond—is creating a hole through an area of resistance into the canal,” Dr. Lewis said. “SLT stimulates that tissue; it doesn’t make a hole, but surgically, we do.”
Dr. Singh sees advancements in glaucoma laser procedures as having the potential to help a lot of patients. This can maintain high safety by not having to go into the eye, and providing access to more doctors who aren’t as comfortable doing procedures in glaucoma will allow us to intervene and help more patients early on, he said. “That’s big for me as a glaucoma specialist. We never like to see people coming into our office who are so advanced that we can’t do much. I wish every primary care ophthalmologist was treating glaucoma and trying to get patients off drops. I think these new glaucoma technologies will allow that earlier intervention by non-glaucoma specialists.”
DSLT
“I wish every primary care ophthalmologist was treating glaucoma and trying to get patients off drops. I think these new glaucoma technologies will allow that earlier intervention by non-glaucoma specialists.”
Inder Paul Singh, MD
Discussing a new procedure called direct selective laser trabeculoplasty (DSLT), Dr. Singh said this is done with the Eagle laser (BELKIN Vision, acquired by Alcon). This laser allows the surgeon to perform SLT directly through the limbus, through the sclera, as there’s no gonioprism. The machine looks like an OCT, like a diagnostic machine, he said. The patient looks into the machine, which automatically recognizes the limbus and fires 120 shots externally without any pain in a few seconds. You can control which spots are being applied, he said, adding that it’s fairly automated.
One of the biggest barriers to SLT, Dr. Singh said, is likely due to efficiency and flow; it’s not the data. The LiGHT trial was clear that SLT is a better first-line treatment for glaucoma than drops. Less patients progress over 6 years, less have issues with cost, and less have visual field progression.
Physicians may not be doing the procedure because they are not comfortable viewing the angle, Dr. Singh said. With a gonioprism, you have to be comfortable with the view and knowing where the anatomy is. The cornea might not be clear, so it can be hard to get a good view. Some surgeons may not be comfortable firing the laser, and they may miss some spots, so there’s a lot more variability with SLT with a gonioprism. “I think direct SLT addresses a lot of those concerns. Because you’re not having to use a gonioprism, it doesn’t require you to have a good view through the cornea. It doesn’t require you to have good gonioscopic skills; it doesn’t require you to have the angle perfectly aligned with your aiming beam,” he said. “I think it’s going to allow a lot of doctors to feel more comfortable.”
Dr. Singh sees the efficiency of the procedure as a benefit as well. “Physicians don’t have to struggle to get the gonioprism on the eye and make sure the eye is open enough for the lens to fit.”
The Eagle laser is approved in the U.S. and should be rolling out soon. It’s been approved and launched in the U.K.
FLigHT
Another new, non-invasive approach is ViaLase’s Femtosecond Laser image-guided High-precision Trabeculotomy (FLigHT) procedure, a non-incisional approach where a 500- x 200-micron hole is created without entering the eye using a patient interface. “We can create a well-defined hole in the trabecular meshwork without all the potential problems of having an incision,” Dr. Lewis said. There’s no viscoelastic and no inflammation common with a traditional intraocular surgery.
It has been shown in preliminary studies that the hole stays open for years. This option has a lot of appeal because it’s relatively straightforward, he said. Adoption rates with MIGS have been flat; this could be due to surgeons not being comfortable working in the iridocorneal angle and not understanding the anatomy or because it adds time to the standard cataract procedure, he said. Adoption rates have been 5–6% of patients with cataracts having a MIGS procedure, but closer to 20% could benefit from one. The FLigHT procedure is an option that doesn’t require cataract surgery.
This procedure is not yet FDA approved, so the label isn’t clear, Dr. Lewis continued, but the upside is it will be widely available, and it’s safe, easy, and straightforward. It will be for early and late glaucoma patients, with and without cataracts. The restriction with MIGS is that it has to be done in mild to moderate disease with cataract; the standalone option is essentially not available, he said. Physicians want a standalone procedure and to do it in mild and moderate to advanced disease, but it’s hard to get coverage. This procedure will be not restricted by those labels, he said. In addition, with the FLigHT procedure there is no corneal incision.
Dr. Lewis said that the FLigHT pivotal trial compares the procedure to SLT, which also does not require an incision. SLT is a tough comparison because it’s safe and successful. “The safety and efficacy profile from the pilot study is encouraging, and I think it will be a lot better for the long term because SLT wears out in a year or two. I hope these results will be replicated in the randomized controlled trial that has been fully enrolled,” he said.
The pivotal trial has 152 patients randomized, comparing femto/FLigHT to SLT. It is an outside the U.S. study, with 76 patients in each arm. “We’re extending that study out to 3 years, with the initial data analysis being submitted to the FDA, hopefully in the fall. We hope for clearance sometime in 2025,” Dr. Lewis said.
Dr. Singh called the ViaLase procedure “groundbreaking and paradigm shifting because this is a non-invasive procedure.” You’re performing a trabeculotomy without having to open up the eye, he said, adding that there’s no cutting and no risk of infection.
What’s even more impressive are the diagnostic capabilities, he said. “It has a 360 gonioscopic imaging system, and it also has intraoperative OCT. It can allow us to truly see the angle in high definition better than any gonioscopic view.” Currently, it may be hard to do smaller trabeculotomies temporally by hand. With this, physicians can perform trabeculotomies anywhere in the angle, and they can make a perfect incisional trabeculotomy without having to open up the eye. This can allow physicians to perform trabeculotomies earlier in the disease state. Dr. Singh said the FligHT procedure could be used as a first-line or second-line treatment.
He thinks that this could open up options for physicians to have the same type of precision they’re used to with femtosecond lasers. Docking is similar to that with the femtosecond laser, he said, adding that a lot of cataract/refractive surgeons used to femto will be comfortable with this device.
ELIOS
Dr. Singh also mentioned the laser from ELIOS Vision (not yet approved in the U.S.). Recruitment has been completed for a cataract combination study, and there is currently a standalone study. This laser produces an efficient, clean surgery, he said. It uses an excimer laser with a probe that allows the physician to create 210-micron channels. “You get 10 of these ‘shots on goal’—10 micro channels through the trabecular meshwork into Schlemm’s canal into the nasal angle,” he said. There’s no canal dilating or trying to fit something into the canal. Dr. Singh said it’s very user friendly and efficient in terms of the adoption and learning curve.
The efficacy is similar to what we’d expect with MIGS, he said. You can get the pressure down to the mid to upper teens, and it fits for the mild to moderate patient population at the time of cataract surgery.
The laser has a small footprint, with a small tower that physicians can transport, and the probes are thin.
“I’ve been talking to a lot of comprehensive and cataract and refractive surgeons. I love stenting, but some surgeons say they don’t want to put a stent in and have the risk that it’s not positioned correctly. There’s a little bit of concern using devices that have to stay in the eye,” Dr. Singh said. “With lasers like the ones from ELIOS Vision, ViaLase, and BELKIN Vision, we’re not having to leave a foreign body in the eye. That’s why lasers are beneficial to a lot of physicians who might not feel as comfortable in the angle.”

Article sidebar
Valerie Trubnik, MD, Glaucoma Editorial Board member, shared how she has knocked down clinical and surgical challenges:
One of the biggest postoperative obstacles that I face post-cataract or glaucoma surgery is dry eye disease. A lot of cataract/glaucoma patients have previously undiagnosed ocular surface disease that, if not treated, contributes to patient dissatisfaction post-surgery despite a well-executed surgery. I have become very cognizant of recognizing and treating dry eye ahead of time with an algorithm and combination of drops and lid hygiene. I have also learned to be patient in waiting for those patients to get better before proceeding with surgery (if that’s an option). Once the treatment takes effect, the surgery outcomes and patient satisfaction have drastically improved.
About the physicians
Richard Lewis, MD
Founder
Sacramento Eye Consultants and Capital City Surgery Center
Sacramento, California
Inder Paul Singh, MD
The Eye Centers of Racine and Kenosha
Racine and Kenosha, Wisconsin
Reference
- Gazzard G, et al. Selective laser trabeculoplasty versus eye drops for first-line treatment of ocular hypertension and glaucoma (LiGHT): a multicentre randomised controlled trial. Lancet. 2019;393:1505–1516.
Relevant disclosures
Lewis: ViaLase
Singh: Alcon, BELKIN Vision, ELIOS Vision
Contact
Lewis: rlewismd1@gmail.com
Singh: ipsingh@amazingeye.com