Glaucoma
June 2022
by Ellen Stodola
Editorial Co-Director
Tube shunts still have important applications for glaucoma patients today and are often used for more severe disease. When categorizing tubes shunts, there are valved or non-valved options. Davinder Grover, MD, Leon Herndon Jr., MD, and Thomas Patrianakos, DO, discussed the available non-valved tube implants, particularly how the newer Ahmed ClearPath (New World Medical) compares to older options.
The non-valved options include the ClearPath, Baerveldt (Johnson & Johnson Vision), and Molteno3 (Nova Eye), Dr. Patrianakos said, noting that he uses the non-valved option when he wants IOP to be a bit lower. He also said he uses this option more in end-stage disease where pressure of 16 or 17 mm Hg might not be enough for the patient. He added that the profile of the non-valved option is a bit lower because valved devices are slightly thicker.


Dr. Grover said that the Baerveldt is the most commonly used of the three, with the Molteno3 being the oldest and the ClearPath being the newest. They have different size options—the Molteno3 has a 245 mm2 and 185 mm2, while Baerveldt and ClearPath have 250 mm2 and 350 mm2 options.
The reason for the introduction of the new ClearPath, Dr. Grover said, was the hope that it would have a lower profile and would be easier to put in. Ideally, it could be put in farther away from the muscles, so there would theoretically be a lower risk of double vision and other problems. Dr. Grover has observed this improved safety and efficiency in his experience with the implant over the past 2 years.
The 250 and 350 Baerveldt are put underneath the rectus muscles, typically the superior rectus, Dr. Grover said, and with the 350, the lateral rectus as well because it’s bigger. The 350 ClearPath also goes under both muscles, he said. But the 250 ClearPath does not require this, and the Molteno3 can also be put in without isolating a muscle.
“In my mind, what’s revolutionary about the 250 ClearPath is it does not require you to touch the muscles,” Dr. Grover said. You can slide it in the superior temporal quadrant, which is the most common location, and it doesn’t require any muscle isolation. Dr. Grover added that this is beneficial in terms of patient recovery and comfort.
Double vision is one of the most debilitating and annoying side effects of tube shunts, he said. “You take someone who is young and functional and give them double vision, and it is miserable.”
Dr. Grover noted that he sees a role for all of the tubes, but recently he’s found the 250 ClearPath to be his preferred choice because of its flexibility and ease of implantation.
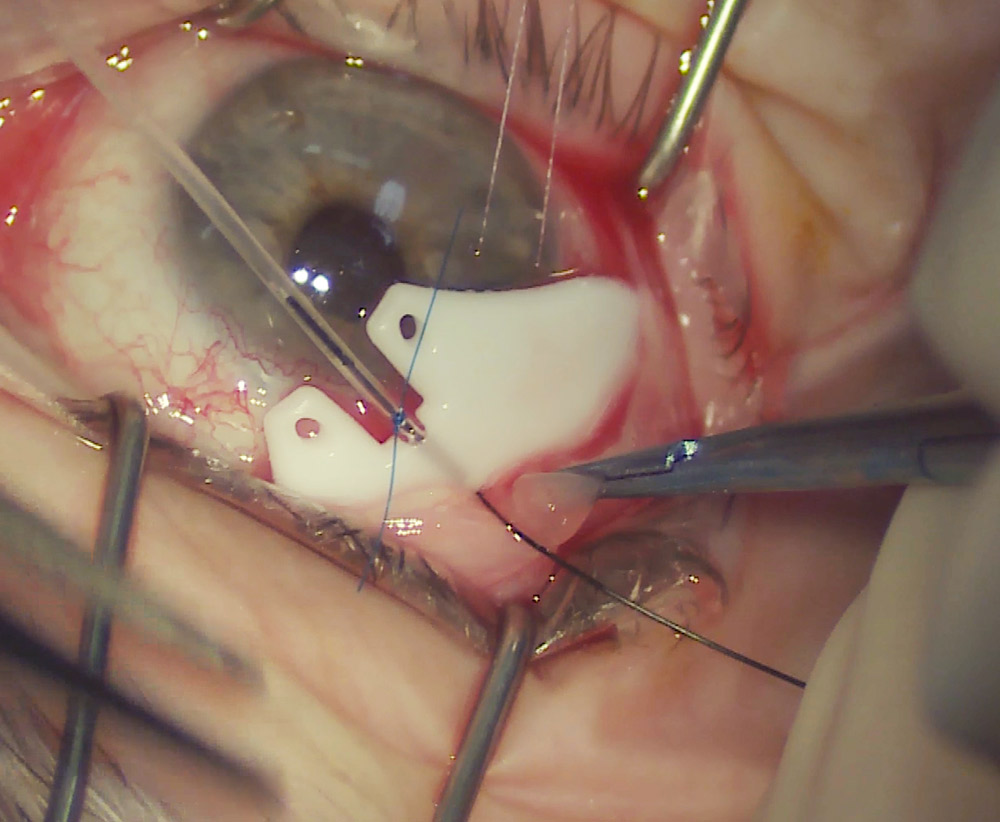
Source (all): Davinder Grover, MD
Comparing the devices
Dr. Grover said it’s important to collect data and compare the newer devices to the more tried and true options. He recently published 6-month data and is in the process of looking at his 1-year data with the ClearPath.1 “It is extremely promising and consistent with my clinical impression that the safety is there, there is less risk of hypotony, and we still have yet to see, with the 250 ClearPath, any cases of double vision in more than 200 cases at our practice.”
Dr. Herndon is currently involved in a study comparing the 350 Baerveldt and the 350 ClearPath. While the study is ongoing, he said that early data suggests that there is no difference between the two products. “We have a handful of patients who have reached the 1-year mark, and we’re looking at the interim data,” he said. While it’s still early, Dr. Herndon noted the similar success and complication rates between the two. There had been no previous head-to-head comparison.
Dr. Herndon noted that some thought the newer ClearPath has features that are more beneficial to patients, causing less diplopia, less pain, quicker recovery, and less surgical time, so the study is a way to look at this.
Dr. Herndon has experience using both devices. ClearPath came to market about 2 years ago, and he had extensive experience with the 250 and 350 before starting the trial.
Dr. Herndon said he thinks it may be surprising the way the 250 has taken off. “Traditionally, with tube surgery, we do think that bigger is better,” he said. There is more data on the 350, and for his more advanced patients, Dr. Herndon is using a 350.
The ClearPath is similar in theory to traditional tubes, but with a different design, Dr. Herndon said. “We wonder if there are some factors with design that will make it better,” he added.
Dr. Patrianakos uses both the ClearPath and Baerveldt devices in his practice, noting that he has been using the ClearPath for about a year and a half. For the most part, he thinks they’re similar in terms of efficacy.
He said there are certain advantages of the ClearPath in patients who have a deep-set orbit where it’s hard to implant or tie down the device through the ostium holes. With the ClearPath, the holes are a little more anterior, and in eyes where it may be a more difficult angle to tie those down, the ClearPath can be a good option, he said.
Dr. Patrianakos also uses the ClearPath over the Baerveldt in eyes with a lot of conjunctival scarring, particularly in those patients who have had previous surgeries, retinal surgeries, etc., because the ClearPath material is more flexible, and it can be “rolled up like a taco” and inserted and unrolled, he said.
He stressed, however, that the ClearPath and Baerveldt are similar. “If you talk to some other doctors, they might say that they prefer the Baerveldt, but in my experience, I’ve had similar results with the two.”
Another thing to consider when comparing the options are the different sizes. Dr. Grover has moved away from the larger implants. “There’s more and more data showing that there’s not a significant difference in outcomes when you compare the 250 and 350 Baerveldt implants,” he said. Given the similarity in outcomes, he tends to think that the smaller option is safer because it’s taking up less room, it’s less invasive, and there is a lower chance of tube-associated hypotony.
One additional reason he likes the 250 ClearPath option is because of patient comfort. When you have to pull on muscles during surgery and put a plate under them, it’s uncomfortable for the patient, and this requires a block, he said. “When you’re not messing with the muscles, you don’t need to do an extensive block, so I’m doing all of my 250 ClearPaths topical without having to block the patient at all, which is safer and more efficient, while still comfortable for the patient.”
He added that this may be potentially beneficial if a patient gets double vision and needs to be referred to a strabismus surgeon for muscle surgery, as that surgeon would have access to all muscles if needed. “While I have yet to experience double vision with the 250 ClearPath, in the rare situation the patient has this, the strabismus surgeon has more flexibility in fixing the problem,” he said.
In terms of IOP lowering, Dr. Herndon said that both the Baerveldt and ClearPath can get to similar levels. In multicenter trials with the 350 Baerveldt out to 5 years, the pressures were 14 mm Hg, he said, adding that he’s seeing 12–15 mm Hg in the ClearPath.
For both devices, Dr. Patrianakos said you can get pressures in the low teens, sometimes high single digits, with the larger surface area options. The larger surface area of the 350 may get the pressure down lower, but there are tradeoffs too, he said. The larger the surface area of the plate, the more chance of complications, so you have to take that into account. “I do think that the larger the surface area, the lower the intraocular pressure, and when I really want to aim for low pressures, I usually will opt for the 350. It may not be that significant, but it does have some effect,” Dr. Patrianakos said.
Dr. Grover said he’s typically seeing pressures in the mid-teens with one IOP-lowering drop. He also mentioned using a diode laser with CPC or ECP. “What’s becoming more of a trend is if a patient has a tube shunt and pressures are not ideally controlled, I can supplement that tube with the low-energy CPC diode, and it allows me to dial down the pressure a bit,” he said.
“It’s our responsibility, as a society of glaucoma specialists, any time a new implant comes out, to prove that it’s safe and successful and look at our data. This is what we are currently doing with the ClearPath,” Dr. Grover said.
About the physicians
Davinder Grover, MD
Attending Surgeon and Clinician
Glaucoma Associates of Texas
Dallas, Texas
Leon Herndon Jr., MD
Director of the Glaucoma Service
Duke Eye Center
Durham, North, Carolina
Thomas Patrianakos, DO
Chair of Ophthalmology
Cook County Health
Chicago, Illinois
Reference
- Grover DS, et al. Clinical outcomes of Ahmed ClearPath implantation in glaucomatous eyes: A novel valveless glaucoma drainage device. J Glaucoma. 2022;31:335–339.
Relevant disclosures
Grover: New World Medical, Nova Eye
Herndon: New World Medical
Patrianakos: None
Contact
Grover: dgrover@glaucomaassociates.com
Herndon: leon.herndon@duke.edu
Patrianakos: tpatrianakos@yahoo.com



