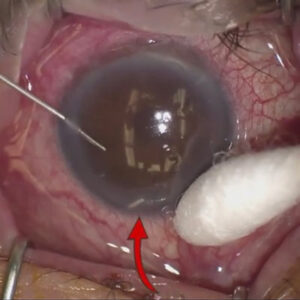
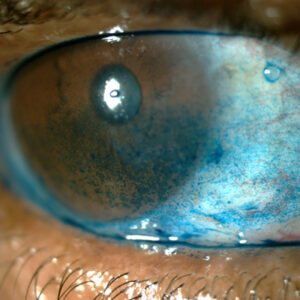
Cornea: Hot topics in ophthalmology
December 2022
by Ellen Stodola
Editorial Co-Director
When treating endothelial dysfunction, surgeons have several options. The current standard of care is endothelial keratoplasty, DSAEK and DMEK, said Edward Holland, MD. “These transplant procedures have been a tremendous surgical advancement,” he said. “However, there are issues that can be problematic. Patients are required to lie flat on their back for 1–2 days postoperatively. Graft detachment is an issue especially in DMEK. And despite a successful procedure, the endothelial cell count can be low, resulting in a shorter life of the graft.”
There has been very little innovation in transplantation in decades, said Elizabeth Yeu, MD. However, she noted that rejection rates have improved in the last 10–15 years because of advances in allograft techniques. “That’s great, but at the same time, that does not allow us to do more than a one-to-one ratio,” she said. “That’s not enough to cure global blindness.”
One new therapy that has been getting a lot of attention is corneal endothelial cell therapy, and Dr. Holland said there has been excellent progress in the last 18 months. This technology was developed by Shigeru Kinoshita, MD, PhD, and colleagues at Kyoto Prefecture University of Medicine in Japan. “Dr. Kinoshita published key findings of his first 11 patients at 2 years postop in the New England Journal of Medicine1 and at 5 years postop in Ophthalmology.2 Those publications were met with tremendous enthusiasm by corneal specialists throughout the world,” Dr. Holland said. “In total, Dr. Kinoshita and colleagues have treated 65 patients in research and clinical studies. Dr. Kinoshita’s exciting innovation was to create a method to reproduce corneal endothelial cells in vitro.”
Dr. Yeu said this is a form of harvesting and culturing, so it allows for one donor to help up to 200 patients. The reason this is so exciting is there is less antigenicity with the greater cell lines that are harvested, she said.
In 2021, the technology was acquired by Aurion Biotech, which has continued to innovate with cell manufacturing advances and treated a total of 67 patients in the last 18 months in OUS trials. Dr. Holland was part of a team of U.S. surgeons who treated those patients. “I think that the preliminary results for safety and efficacy are largely consistent with patients treated in Japan,” he said. “I have high confidence in the technology and its exciting potential.”
Dr. Yeu, John Berdahl, MD, and Matthew Giegengack, MD, also have experience working with the new technology.
Compared to DSAEK and DMEK, Dr. Holland said there are several benefits of corneal endothelial cell therapy: Postop endothelial cell counts are significantly higher than EKs; there is an improved surgical experience for the patient (surgery takes less time, and there is no prolonged positioning); and there is a lower complication rate, as there is no risk of graft detachment. Dr. Holland added that there is also a shorter postop patient recovery. “Corneal endothelial cell therapy involves a single injection,” he said. “Once the procedure is complete, patients lie face down for a couple of hours. Then they are free to go home and live relatively normally. Within weeks, vision recovers.”
Another potential benefit of this new therapy is the number of patients it could treat. “The ability to manufacture corneal endothelial cells will ultimately enable ample supply for patients in need. This, along with the benefits of a simplified surgical procedure, has the potential to dramatically increase accessibility for patients,” Dr. Holland said, although he stressed that this cell therapy is not yet available commercially, and Aurion Biotech must go through clinical trials in the U.S.
“We are lucky in the U.S. in that we have very good treatment options for endothelial dysfunction, DSAEK and DMEK, both of which set a high bar for cell therapy,” Dr. Giegengack said. “For patients in the U.S. who qualify for DMEK/DSAEK procedures, increasingly we are opting for DMEK since patients are generally able to see better and recover more rapidly than with DSAEK. But due to the complexity of surgery, we cannot perform DMEK on all patients, so DSAEK is still a viable option.” Dr. Giegengack said that for cell therapy to be a viable treatment option, it would need to be at least as good as DMEK.
“In my experience with the cell therapy patients I’ve treated (and who I’ve observed my colleagues treat) in the OUS studies, the preliminary findings are promising,” Dr. Giegengack said, noting that corneal edema is reduced, and visual acuity is improved significantly.
He added that cell therapy is a less complex procedure to perform than DMEK, and postop recovery for patients is shorter. “I’m hopeful that cell therapy will ultimately enable ‘DMEK-like’ improvements in vision to a larger group of patients,” Dr. Giegengack said.
This new cell therapy option could also be beneficial on a global scale by enabling easier access worldwide. Globally, corneal tissue supply is a big challenge, Dr. Giegengack said. “Even in the U.S., with an upswing in DMEK procedures, surgeons are requiring more specific donor tissue, so tissue supplies are running short,” he said. “Cell therapy can alleviate these supply challenges. Dr. Kinoshita’s exciting discovery was to get corneal endothelial cells to replicate in vitro (they do not regenerate naturally in vivo).”
Dr. Yeu said that seeing this work in action has been incredibly gratifying. “It’s exciting because it’s just cells plus a formulation of ROCK inhibitor.” It allows for limbus-to-limbus adhesion of cells. With allograft transplants, “we’re only able to replace the central 80%.” As a result, there are problems with peripheral edema, Dr. Yeu said, and those patients with peripheral pathology can’t be treated well.
“So far with the work we’ve done, these patients are able to have corneal thinning that gets them to the same type of results that we see with DSAEK and DMEK by month 1 to month 6,” Dr. Yeu said. She added that being able to get patients off steroids, or at least to minimal steroid use, is another benefit. This helps reduce some issues with ocular hypertension and glaucoma. “Not only are rejection rates lower, but the IOP issues are much lower, and these corneas look incredible,” she said, adding that the possibility for patients to be able to survive on one transplant would be amazing.
Dr. Yeu also commented on the technique used with corneal endothelial cell therapy, noting that it’s even easier than DSAEK and DMEK because instead of a stripping, it’s a polishing to remove residual endothelium using a silicone tip on a cannula. It’s a familiar technique that any anterior segment surgeon can do. “It also opens up the opportunity to treat everything from early corneal edema to severe corneal edema as a first-line therapy,” she said.
Dr. Berdahl agreed that surgical accessibility is an advantage of endothelial cell therapy. Endothelial keratoplasty is a highly technical procedure that’s performed primarily by corneal surgeons, but endothelial cell therapy would be a more accessible technique. It would also likely have a decreased rejection risk because the cells are antigenically more neutral. “The procedure can control exactly how many endothelial cells are injected, the surgical technique is less technical, and we can avoid an air bubble in the anterior chamber and avoid the potential complications of flattening the chamber.”
In addition to Aurion Biotech, Dr. Berdahl mentioned that Emmecell is exploring endothelial cell therapy options.
Other treatments
Another advancement is Descemet’s stripping only (DSO). Corneal endothelial cells will naturally expand to form tight junctions with other corneal endothelial cells, Dr. Giegengack explained, so when we strip away portions of Descemet’s membrane, the remaining endothelial cells will grow and “morph” to fill in the gaps.
Dr. Giegengack uses this procedure and thinks it works well for a small subset of Fuchs patients with focal central guttata and corresponding corneal edema that doesn’t extend out to the periphery of the cornea. “You can remove that central area of guttata and treat with ROCK inhibitor drops,” he said. “Peripheral endothelial cells can expand back into the center and fill in the gap. The advantage of this approach is that patients have the potential to regain vision without the risk of transplant rejection.”
However, he noted that DSO can take a long time to heal, and sometimes patients’ vision isn’t improved, and they do need to undergo a corneal transplant. He added that he’s picky about when he performs DSO.
Dr. Holland also explained that corneal endothelial cells do not naturally regenerate in vivo, and if cells die, the remaining cells will expand and enlarge to form tight junctions with remaining endothelial cells. “Thus, by stripping Descemet’s membrane in the cornea’s central area, the remaining endothelial cells at the periphery will likely enlarge and gravitate to the center,” he said. “However, in some cases, enlarged corneal endothelial cells may cease to maintain their pump and barrier functions, thereby increasing corneal edema and potentially resulting in hazy vision in the long term.” He added that this procedure is limited to those corneas with a small area of central guttata, and there can be a long recovery period.
Dr. Berdahl said it’s unknown exactly how cell redistribution works with DSO. It is likely at least partially driven by contact inhibition. Endothelial cells stop growing when they touch other endothelial cells, and by removing an area of endothelial cells, the endothelial cells migrate to cover the cells that have been removed because there is no longer an adjacent contact.
Dr. Berdahl said that he has not used DSO in clinical practice and thinks the majority of endothelial dysfunction treated surgically is with DMEK or DSAEK, with the exception of some cases where only central guttata are present.
Dr. Yeu also noted that patients have a longer recovery with DSO; it could take up to 8 weeks for vision to recover with a lot of corneal swelling in the interim. However, she does see its potential in the future because it doesn’t have the allograft rejection. “If we could do DSO with a ROCK inhibitor, there may be patients who would consider that versus scraping and cells,” she said.
Moving forward
Dr. Giegengack stressed the potential for cell therapy, not just in the U.S. but also internationally. Noting that he’s done humanitarian work in developing countries, Dr. Giegengack said that corneal transplants tend to have lower success rates there than in the U.S. “I think cell therapy has the potential to decrease that discrepancy,” he said. “Because cell therapy is a less complex procedure, I think it will potentially require less follow-up and have fewer complications. [These are] especially important benefits for patients in underserved parts of the world.”
Dr. Yeu mentioned the possibility of having the option to cryopreserve. This isn’t a foreign idea, she said, noting that it’s used for amniotic membranes. She said it would “change the way we think” to be able to use these cells and defrost them when you need them.
She added that it’s been promising to see patients in studies so far who had significant visual issues, vision worse than 20/40 and up to 20/800, some with worse than 600-micron corneas. “To see these types of cornea patients at the level they’re at is very promising,” Dr. Yeu said.
“It is heartening to know that corneal endothelial dystrophies are now the focus of multiple avenues of research and development,” Dr. Holland said. “I think these innovations will yield safe and efficacious options for patients suffering from corneal endothelial diseases. For example, I think that cell therapy might be used across the entire disease spectrum, which would potentially mean the ability for us to treat patients earlier in the course of their disease. I do think endothelial cell therapy will become the treatment of choice for the majority of patients with endothelial disease.”
ARTICLE SIDEBAR
TTHX1114 growth factor
Another interesting option in this space is TTHX1114 growth factor, currently in studies from Trefoil Therapeutics.
“We know that the eye contains antiproliferative factors that naturally prevent endothelial cell regeneration in vivo,” Dr. Holland said. These factors keep those cells in cell cycle “arrest” mode, which prevents cell regeneration in vivo. Trefoil Therapeutics has a novel approach for injecting growth factor into the anterior chamber of the eye to stimulate endothelial cell reproduction in vivo. This treatment requires weekly injections over a 4-week course. “If this approach works, it would have significant benefits as compared to endothelial keratoplasty,” Dr. Holland said.
This is not the injection of endothelial cells, rather injection of a pharmaceutical growth factor, Dr. Berdahl said. The benefit of this approach is that this pharmaceutical growth factor could increase the effectiveness of the body’s own endothelial cells. This helps to decrease the chances of rejection.
About the physicians
John Berdahl, MD
Vance Thompson Vision
Sioux Falls, South Dakota
Matthew Giegengack, MD
Associate Professor of Ophthalmology
Wake Forest University
School of Medicine
Greensboro, North Carolina
Edward Holland, MD
Professor of Ophthalmology
University of Cincinnati
Cincinnati, Ohio
Elizabeth Yeu, MD
Virginia Eye Consultants
Norfolk, Virginia
References
- Kinoshita S, et al. Injection of cultured cells with a ROCK inhibitor for bullous keratopathy. N Engl J Med. 2018;378:995–1003.
- Numa K, et al. Five-year follow-up of first 11 patients undergoing injection of cultured corneal endothelial cells for corneal endothelial failure. Ophthalmology. 2021;128:504–514.
Relevant disclosures
Berdahl: Aurion Biotech
Giegengack: Aurion Biotech
Holland: Aurion Biotech
Yeu: Aurion Biotech
Contact
Berdahl: john.berdahl@vancethompsonvision.com
Giegengack: mgiegeng@wakehealth.edu
Holland: eholland@holprovision.com
Yeu: eyeulin@gmail.com