Cataract: Cataract editor’s corner of the world
November 2012
by Jena Passut
EyeWorld Editor

Cataract surgery is now commonly considered refractive surgery due to the abundance of specialty intraocular lenses and the introduction of the femtosecond laser. Although great strides have been made in perfecting the visual outcomes after surgery, the patients are also concerned with the cosmetic appearance of their eyes after surgery. Ptosis, ecchymosis, and conjunctival erythema have long been considered necessary evils of cataract surgery. With the trend away from retro and peribulbar injections and toward topical anesthesia, the risk of ptosis has decreased. However, ptosis still occurs in a significant percentage of patients after intraocular surgery. In this column, we asked two specialists their opinions about the etiologies and treatments for post-op ptosis.
—Bonnie An Henderson, M.D., cataract editor
Despite being somewhat common, post-surgical ptosis is a multifactorial condition that can be minimized or treated, according to oculoplastics specialists who spoke to EyeWorld.
The main culprit that causes droopy eyelids after surgery appears to be the speculum used to pull back a patient’s lids and keep the eye accessible for the procedure, said Erin M. Shriver, M.D., assistant professor of clinical ophthalmology, Bascom Palmer Eye Institute, University of Miami Miller School of Medicine.
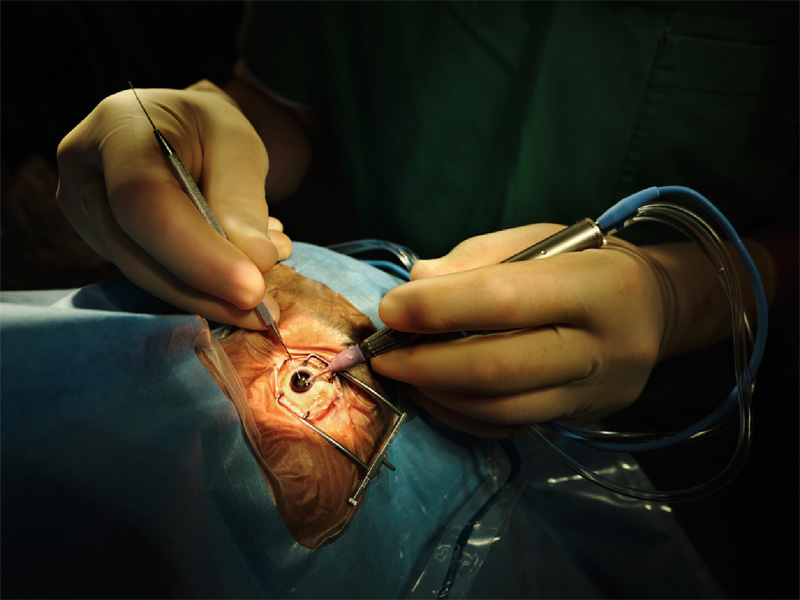
Dr. Shriver said she sees ptosis after all types of ocular surgery including complicated cataract, refractive, corneal, and glaucoma surgery.
Studies differ, but ptosis has been reported to occur in anywhere from 0-21% of patients following surgery.
“We have one rigid eyelid speculum that we have nicknamed the ‘ptosis maker,'” Dr. Shriver said, adding that a good portion of her ptosis referrals are post-surgical patients. “The ‘ptosis maker’ is used for ocular surgeries that require significant conjunctival exposure such as glaucoma-filtering procedures. The benefit in exposure for the procedure is felt to outweigh the risk of ptosis. Although this has not been researched, a more rigid speculum theoretically causes more trauma to the eyelid than a more flexible wire eyelid speculum as it would not yield to the contracting forces of the concentric orbicularis muscle.”
Theories abound about what causes post-surgical ptosis, including the eyelid speculum, a predisposition to the condition, retrobulbar or peribulbar anesthesia, duration of surgery, and eyelid inflammation resulting from corneal sutures.
“If the speculum was weaker and had less give, maybe that would cause less trauma to the muscle than if you have a firm speculum”
Erin M. Shriver, M.D.
“The problem is that no one has looked at each factor alone,” Dr. Shriver said. “It’s not clear cut.”
With the speculum at play, ptosis “could be related to edema or ischemia from the speculum compressing the lid, dehiscence of the levator muscle, or horizontal stretching of the lid,” Dr. Shriver noted.
Anesthesia was also suspected to be an offender potentially causing ptosis.
“In a study by John J. Alpar, M.D., [Amarillo, Texas], there was a 10-fold increase in post-operative ptosis following cataract surgery using a retrobulbar injection vs. general anesthesia, but other studies have found an equal incidence,” said Wendy W. Lee, M.D., associate professor of clinical ophthalmology, Bascom Palmer Eye Institute.
Dr. Shriver said the anesthetic can be both neurotoxic and myotoxic.
“Two percent lidocaine with 1:100,000 epinephrine has been shown to cause degeneration of human muscle within 18 hours of injection,” she said, adding that the epinephrine augments the myotoxic effects. “Degeneration may be ischemic or non-ischemic resulting in weakness of the levator muscle and ptosis. Recovery occurs over an 8-12 week period and results from hypertrophy of remaining muscle fibers and regeneration of muscle fibers.”
With anesthetic, “use only the amount of anesthetic you need and perform surgery with topical anesthesia alone when possible,” Dr. Shriver suggested. “Ocular massage and compression decreases the risk of hematoma and edema but increases the risk of anesthetic effects as it increases its availability.”
Surgeons also can decrease the risk of ptosis following cataract surgery by avoiding bridle sutures, using small, sutureless temporal incisions, and reducing irritation on the ocular surface, Dr. Shriver said.
Duration and treatment
Luckily for surgeons and patients, lid drooping after cataract surgery is often short-lived. “Most transient ptosis resolves by 6 months, but there has been one reported case of spontaneous resolution 11 months post-operatively,” she said. That case was believed to have been caused by a neuropraxia of the oculomotor nerve, Dr. Shriver said.
Ptosis is either classified as transient or persistent, depending on the duration. Transient ptosis, which lasts less than 6 months, often resolves on its own without medical intervention.
Dr. Lee said practitioners, however, may “consider prescribing apraclonidine to achieve up to 2 mm of lift by stimulating Muller’s muscle temporarily as the levator recovers.”
Persistent ptosis lasts more than 6 months and can be treated with surgical interventions such as a levator advancement or conjunctival Mullerectomy.
“Ptosis can be repaired by either an internal or external approach depending on the degree of ptosis response to phenylephrine testing, ocular surface health and integrity, and surgeon preference,” Dr. Shriver said.
Cataract patients should be warned of the risk of ptosis, and ptosis patients with cataracts should be warned that the surgery could exacerbate the condition. Repair of the ptosis also should be postponed until after the cataract surgery, Dr. Shriver said.
When patients develop ptosis after cataract surgery “it is recommended that the patient be observed for at least a 6-month period and that the patient’s eyelid measurements are stable prior to surgery,” Dr. Shriver continued. “If surgery is performed within the first year after intraocular surgery, it has been recommended that the levator be plicated rather than resected in the event that there will be a return of function necessitating a reversal of the ptosis repair.”
Dr. Shriver added that because of the potential effects of cataract surgery on the eyelids, if a patient desires elective eyelid surgery and is going to need cataract extraction within a year, she would recommend postponing the eyelid surgery until after cataract surgery.
Editors’ note
Drs. Lee and Shriver have no financial interests related to this article.
Contact information
Lee: 305-326-6434, wlee@med.miami.edu
Shriver: 561-355-8608, eshriver@med.miami.edu



