Refractive
Spring 2026
by Liz Hillman
Editorial Co-Director
Attend a session on cataract surgery and astigmatic correction at a medical conference and you’ll hear about the importance of K alignment ad nauseam, but Nicole Fram, MD, said it continues to be a relevant and important point to emphasize.
“1) When K values don’t align, ocular surface disease is a very common cause. 2) I think astigmatic correction is critical to the success of refractive cataract surgery. We’re seeing reimbursements going down, and we’re seeing expectations from patients going up. The first step to getting comfortable with presbyopia-correcting lenses, in my opinion, is knowing how to reliably correct astigmatism. … If you don’t feel comfortable treating astigmatism or knowing when to treat astigmatism, you can never elevate your practice into the presbyopia-correcting world, which is not only what patients want but it’s also what doctors are going to need to survive [financially],” Dr. Fram said.
Dr. Fram and Douglas Koch, MD, discussed the topic of when the Ks don’t align—when misalignment is clinically significant, what can be done about it, and how it impacts lens choices.
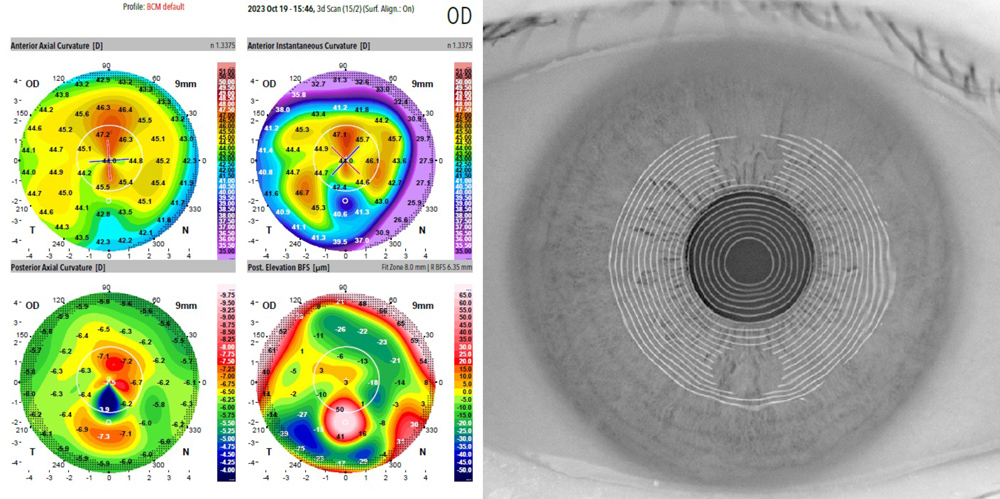
Source: Li Wang, MD, PhD
K discrepancies
Dr. Koch said everyone has their own threshold for K measurements that don’t align, meriting remeasurement and potentially further action.
“For me, it would be any difference in astigmatism magnitude that’s greater than a half or certainly greater than 0.75 D. For astigmatism meridian, in general I would like measurement variations in the steep meridian of no more than 10 degrees,” he said. He provided the accuracy of meridional alignment as a function of the astigmatism magnitude needed to leave the patient with <0.5 D of refractive astigmatism:
- 1 D: ≤14°
- 2 D: ≤7°
- 3 D: ≤4°
- 4 D: ≤3°
For eyes with low amounts of astigmatism, there is some flexibility, but accuracy within even 15 degrees can be a big ask if the magnitude of astigmatism is small, i.e., less than a half diopter. “You might ask why consider correcting 0.5 D? For the patient with against-the-rule astigmatism, not treating 0.5 D on the cornea will lead to up to 1.0 D in refractive astigmatism, and this will increase over time,” Dr. Koch said. “Fortunately, it’s easier to get agreement on the steep meridian when the astigmatism magnitude is greater because it’s a more defined point with increasing magnitudes.”
Dr. Koch mentioned a study that compared the steep meridian difference between two devices—the IOLMaster (Zeiss) and the Lenstar (Haag-Streit)—in the same visit for 129 right eyes. The devices agreed on the location of the steep meridian within 5 degrees 60.5% of the time and within 10 degrees 82.9% of the time. This highlights the importance of taking multiple measurements, he said.
If you only have one device for K measurements, Dr. Koch said you need to think about how to verify the information that device is giving you. “Everyone uses a biometer with LEDs to measure the K readings, and everyone should have a topographer, preferably one with Placido rings because of the detail it gives about the ocular surface,” Dr. Koch said. “Ideally [you should also have] a device that gives you corneal tomography or corneal thickness. One should have a very low threshold for evaluating the mires of the biometer LEDs if the measurements don’t add up.”
If you don’t have multiple devices, Dr. Koch said he and his colleague Li Wang, MD, PhD, developed a formula with Zeiss to help provide central topographic information from IOLMaster 700 measurements, but he noted this is only the central 3–3.5 mm.
“Ideally, you want a topography/tomography and LEDs. Let’s say you have a patient come in, you get a topography, tomography, and maybe on that first visit, if you only have one biometer, get a Lenstar or an IOLMaster 700, then when they come in for the preop visit, repeat the biometry. If it’s consistent with a prior measurement, you’re in good shape. If it’s not, then you have to check the surface,” Dr. Koch said.
Dr. Koch added that if he only had one biometer and one topographer, taking two measurements from each and finding that measurements were consistent with the biometer but different with the topographer, he would rely on the biometer “because those LED measurements are usually very good.” There is a caveat, however. “You need to look at the raw data … the little black dots that are in the printout of the IOLMaster 700, or you can look at the Lenstar device where it shows you what the LED reflections look like. You should verify that these are not smudged—or worse, absent.”
Dr. Fram said she has two biometers in her practice from which she obtains measurements on the same day. She noted that biometry reliability of K readings is getting better and better. “With IOLMaster 700 with Total K, then Lenstar and Argos [Alcon], I think we’re seeing a lot of improvement in our K values,” she said.
After biometry, Dr. Fram also emphasized the utility of topography with Placido imaging is critical. “This can give you a snapshot of the tear film quality.” She said there are different modalities that are allowing physicians to look at the K values. Dr. Fram finds Pentacam (Oculus) with dual Scheimpflug imaging helpful, but it does not give Placido imaging and has limitations in isolation. iTrace ray tracing (Tracey Technologies) is helpful to look at higher order aberration profiles and has Placido imaging. “Anterior OCT imaging has an anterior axial curvature map—3D surface fit generated from 65 radial OCT scans with 16,640 data points over 8 mm. It will also give total corneal power. Finally, something as simple as reviewing patients’ refraction in glasses before cataract development can help guide the surgeon when there is a discrepancy in testing,” she said.
“We want to see at least three of these measurements line up for magnitude and meridian,” Dr. Fram continued. “When you have all of these measurements line up, it’s a home run. When you have three out of the five, you’re still doing pretty well. But you have to figure out in your clinic, what are the three most reliable diagnostics that are going to determine whether you treat astigmatism.”
Dr. Fram said to feel confident in her measurements she needs to see regular Placido imaging on her topographer and quality measurements with good fixation from her biometers. “Whenever I skip a step, that’s when bad things happen. So, I have a very low threshold for bringing someone back before surgery,” she said. “I had a patient who I thought looked OK at first glance, but when I was going over my charts the night before, I had no problem calling the patient and saying, ‘I need you to come back in the morning ahead of your surgery to double check.’ … I never hesitate to bring patients back in for a remeasurement, and sometimes I treat the ocular surface before I bring them back.”
Dr. Fram acknowledged that she has many technologies to take measurements. If you don’t have redundancies among devices, astigmatism can still be accurately measured and treated. “You may want to bring patients back on two different days if you have the same technology. If you have multiple technologies that are redundant and do the same thing, you can do it all at once. If you have one biometer and one topographer, it’s not a bad idea to bring patients back for another measurement if they’re not in complete alignment,” she said. “If you have multiple devices and the readings are all different on each device, there must be an ocular surface or user variability issue going on.”
Ocular surface evaluations and management
The ocular surface is often the cause of inconsistent K measurements, both Dr. Fram and Dr. Koch said.
Dr. Koch said if you find different measurements, it’s time to look at the surface for punctate erosions, rapid tear film breakup, dry eye, or blepharitis; even sitting in front of the device unblinking for too long can affect tear film quality. If the tear film quality is not the cause, the patient could have epithelial basement membrane disease (EBMD) or subepithelial scarring.
Dr. Fram said she needs about 20% of her patients to come back for repeat biometry because she’s not happy with their initial measurements, most commonly due to dry eye and ocular surface issues. In most of these cases (about 80%), she said, a mild steroid like a loteprednol pulse and cyclosporine or lifitegrast can get them on track for surgery. Dr. Fram said she is also looking for and treating Demodex blepharitis to improve the ocular surface for quality measurements as well.
“It’s not enough, however, to say we’ve got you optimized for surgery. We need to keep them optimized after surgery,” Dr. Fram said. “You have to have a system of how to maintain the ocular surface or else you’re not going to have a good outcome.”
For patients who don’t want a superficial keratectomy to treat EBMD or who have conditions that will always cause fluctuations of their ocular surface, Dr. Fram said a monofocal IOL is the best choice, but another creative option to mask up to 1.5 D of astigmatism could be the IC-8 Apthera IOL (Bausch + Lomb). “It’s an interesting option for the non-dominant eye in those patients where you can’t, no matter how many measurements you get, no matter how many times you try and optimize their surface, get them to where they need to be,” she said.
Case example
Dr. Koch described a patient with diffuse punctate corneal erosions who was treated for dry eye preoperatively for 6 months, but her ocular surface never fully recovered even with plasma tears. Dr. Koch said they went forward with a standard surgery at that point because she had narrow angles and her cataract was significant.
“She had a good result of about 20/25 and was very happy. She was certainly not a candidate you would entertain for something like a diffractive or other form of simultaneous vision IOL, either EDOF or trifocal,” he said. “In those cases, I would look at what the refraction was because the refraction often indicates how the patient’s corneal astigmatism contributes to the vision. In this patient, repeated preop refractions were consistent with K readings.”
Take-home messages
Dr. Koch’s take-home message is to avoid trifocal IOLs if you can’t get consistent surface measurements due to severe dry eye. “The dry eye will come back to haunt you postoperatively and impair quality of vision,” he said.
He also advised against a trifocal in patients who have anterior basement membrane dystrophy and who refuse to have it treated before surgery. “You have to treat it and get rid of it in order to have accurate measurements and the best quality of vision,” he said.
If the mires are poor, Dr. Koch would also not implant a toric IOL. “I tell patients they’re better off wearing glasses for astigmatism because you can always adjust glasses.”
One of Dr. Fram’s take-home messages is to avoid under-treating against-the-rule astigmatism. “These are some of my most unhappy patients,” she said. “It used to be that we would say, ‘They have to have a diopter or more or else I’m not going to use a toric lens.’ I think more and more … we are treating against-the-rule astigmatism at the 0.6 D level.” Dr. Fram said that because the total K is verified with the IOLMaster 700 and Pentacam to include the contributions of the posterior cornea, she thinks measurements are becoming more sophisticated and accurate, rather than relying on a nomogram.
Dr. Fram also said that using language in preoperative visits like “we’re going to reduce your astigmatism” instead of “we’re going to correct all of your astigmatism” can be helpful in setting patient expectations. She tells patients that astigmatism can be further fine-tuned, if needed, postoperatively with limbal relaxing incisions or laser refractive surgery.
There are surgical tips to help avoid toric IOL rotation (like making sure all the viscoelastic is removed behind the lens and confirming its removal/lens stability with a balanced salt solution pulse at the end of the case), but Dr. Fram said starting with quality preoperative measurements—knowing what’s reliable and what’s not and what to do to increase accuracy—is most important for gaining confidence with astigmatic correction.
About the physicians
Nicole Fram, MD
Advanced Vision Care
Los Angeles, California
Douglas Koch, MD
Department of Ophthalmology
Cullen Eye Institute
Baylor College of Medicine
Houston, Texas
Relevant disclosures
Fram: Zeiss
Koch: Johnson & Johnson Vision, Zeiss
Contact
Fram: nicfram@yahoo.com
Koch: dkoch@bcm.edu