Cataract
Summer 2025
by Liz Hillman
Editorial Co-Director
Manual marking, digital marking, manual and digital marking—toric IOL alignment methods continue to be an important topic.
“Ten years ago, I’m sure there was an article saying that manual marking was going to be gone, but it’s still around,” said Soroosh Behshad, MD, MPH, who uses both manual and digital marking with his toric cases.
The reason both methods still have a place, Dr. Behshad said, is multifactorial—both have their pros and cons.
Dr. Behshad said he marks the meridians preoperatively using a corneal marker that hooks into his cell phone, then uses the toriCAM app by Graham Barrett, MD, to aid in aligning his marks. In the OR, he has access to a Callisto (Zeiss), which he uses to confirm he is aligning toric IOLs correctly. He said having both gives him confidence in his alignment.

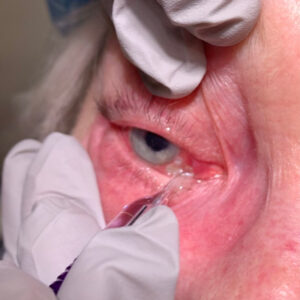
Source: Robert Osher, MD
Some of the main benefits of manual marking, Dr. Behshad said, are that it’s low cost, simple, and quick. To ensure accuracy with manual marking, Dr. Behshad said he talks his patients through what he’s doing every step of the way because they’re sitting up and haven’t had anesthesia yet. In addition, as a cornea specialist, he said regardless of if you mark manually, digitally, or use both for toric alignment, success postop begins preop. He said to look at the ocular surface, manage dry eye, pterygium, anterior basement membrane syndrome, and other pathologies that would affect your preop calculations.
Dr. Osher, like Dr. Behshad, uses a “belt and suspenders” approach, as he put it. Dr. Osher said astigmatic correction at the time of cataract surgery dates to the early 1980s when he introduced astigmatic keratotomy combined with phacoemulsification for the reduction of pre-existing astigmatism. This procedure, he said, was an art. With the invention of the toric IOL in the 1990s by Kimiya Shimizu, MD, astigmatic correction became a science.
Over time, Dr. Osher created a technique called iris fingerprinting to accurately perform manual marking for toric alignment.1 Iris landmarks, unlike blood vessels, don’t change from the preop dilated exam to what surgeons see in surgery. Dr. Osher said he uses a Haag-Streit camera to take a picture of the patient’s iris, and with that photograph, he draws a horizontal line at 0 and 180, followed by the inferior 90-degree mark. “With these, I have three accurate landmarks to guide me in surgery … I hang those photographs on the microscope … and have those right next to me,” he said.
There’s a beauty to having this dual approach, a safe approach, because you never know.
Robert Osher, MD
In surgery, Dr. Osher would make very small, almost imperceptible dots on the conjunctiva with a cautery pen called ThermaDot. “Once I have my ThermaDots, I know I can align that lens perfectly.” In addition to alignment with the manual marks, Dr. Osher uses a circular dial called the Osher-Mendez marker, confirming his correct ThermoDot placement. “I will turn on and register the Callisto. Ninety- nine percent of the time, the target meridian lines up perfectly,” he said.
Dr. Osher acknowledged peer-reviewed studies that have concluded the results with manual vs. digital markers are similar. However, he noted that even a few degrees off on alignment can affect outcomes. Taking a dual approach with precise manual marking that’s confirmed in the OR with a digital marking system does take more time and, with the digital marker, a significant financial investment. Dr. Osher said that if the patient is paying out of pocket for a toric lens and with one shot to get placement right in the OR, it’s worth it.
“I can spend that extra time and invest that extra effort because it satisfies my OCD, and it confirms my conviction that we have one chance in the patient’s entire life to give them the best vision possible,” he said.
Having the manual markings, Dr. Osher added, is also a safety net should the digital marking system fail when needed for whatever reason.
“There’s a beauty to having this dual approach, a safe approach, because you never know,” Dr. Osher said, noting that images might not make it into the medical record, digital systems can freeze, and thumb drives can be lost. “I carry every iris fingerprinting in my briefcase with me every day.”
Both Bryan Lee, MD, JD, and Mitchell Weikert, MD, said they prefer digital marking for their toric IOL cases.
“Digital marking has been shown to be more accurate than manual marking, and it also improves workflow in the preop area and operating room,” Dr. Lee said. “Additionally, if you adjust the axis based on intraoperative aberrometry, you can reposition the digital marker more easily for your final check at the end of surgery.”
The pro of manual marking, Dr. Lee said, is that it is a fallback option if digital images cannot be used, and digital marking is not available 100% of the time. But, he said, “whenever it is, I would always use it.”
Dr. Weikert relies primarily on digital marking and for those where the cost of such a system isn’t an issue, he would say “digital marking all the way.”
“If you are investing in this technology, you need to do a little bit of legwork to make sure that, economically, it makes sense the way you’re handling it,” he said.
Dr. Weikert mentioned the creation of laser capsulotomy marks via the femtosecond laser. This is available on the LENSAR Laser System (LENSAR) and eliminates the issue of parallax error that we have with other digital markers, he said.
But just because you have a digital marking system does not mean you’re out of the woods from using manual marking, Dr. Weikert said. “I had a of couple patients last week where we couldn’t get a quality image. It could be that they have ptosis, or we can’t get them lined up to get a complete image to be able to use the digital marker.”
Dr. Weikert also said that with digital markers, you need to make sure you can reconcile what you’re seeing under the scope with what’s up on the monitor. “Sometimes there’s a little bit of a delay [with digital marking systems],” he said. “I will often mark the eye with the location of the toric lens at the beginning of surgery when I first get my reference, then I’ll look between what I’ve marked on the eye and up at the monitor because the image that you see on the monitor is more static and locked in than the image that you’re looking at under the microscope.”
The discussion of manual and digital marking is still an important one, Dr. Weikert said, especially when you think about it in the context of toric IOL market penetration, which he said is “shockingly low.”
“The penetration of toric lenses was 8.4%,” Dr. Weikert said, citing 2023 data. “Penetration of presbyopia-correcting lenses was 9.1%, so some of those are going to be toric as well. This means that more than 80% of surgeries have a non-toric, monofocal IOL. Why is that? Some of it is cost and the burden of patient expectations, but part of it may be concern about accurate results. Are [surgeons] worried about aligning the lens? What’s the deterrent? If their comfort with aligning the lens is part of it, maybe this is one way to increase the comfort with that.”
About the physicians
Soroosh Behshad, MD, MPH
Associate Professor of Ophthalmology
Gavin Herbert Eye Institute
University of California, Irvine
Irvine, California
Bryan Lee, MD, JD
Altos Eye Physicians
Los Altos, California
Robert Osher, MD
Professor of Ophthalmology
University of Cincinnati
College of Medicine
Medical Director Emeritus
Cincinnati Eye Institute
Cincinnati, Ohio
Mitchell Weikert, MD
Professor, Cullen Eye Institute
Baylor College of Medicine
Houston, Texas
Reference
- Osher RH. Iris fingerprinting: new method for improving accuracy in toric lens orientation. J Cataract Refract Surg. 2010;36:351–352.
Relevant disclosures
Behshad: None
Lee: Zeiss
Osher: None
Weikert: Heidelberg, Zeiss
Contact
Behshad: sbehshad@hs.uci.edu
Lee: bryan@bryanlee.pro
Osher: RHOsher@cvphealth.com
Weikert: mweikert@bcm.edu