Glaucoma: Opening doors
Winter 2025
by Ellen Stodola
Editorial Co-Director
Surgeons who routinely perform cataract surgery could better help patients by learning basic glaucoma procedures and incorporating them into cataract surgery, according to physicians who spoke to EyeWorld. For those who aren’t sure where to start, Rom Kandavel, MD, and Shivani Kamat, MD, discussed how they think cataract surgeons can gain experience with glaucoma procedures and when it makes sense to incorporate them.

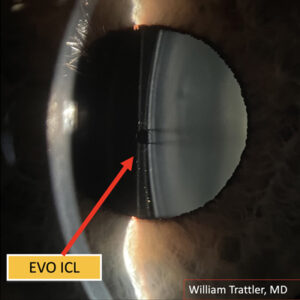
Source: Shivani Kamat, MD
Dr. Kandavel said that if cataract surgery is imminent, it makes sense to consider angle surgery while the patient is already in the OR if the patient has glaucoma and is on treatment or would benefit from lower pressure beyond what the cataract surgery alone could offer. There is minimal risk involved with the additional procedure, he said. “In fact, some may say that not performing an additional glaucoma procedure in a patient who could benefit from the technology is a lost opportunity,” he said. “Adding angle-based surgery is a natural evolution for an anterior segment surgeon who is already comfortable with cataract surgery skills.”
For cataract surgeons interested in expanding into glaucoma procedures, Dr. Kamat said she would recommend starting with procedures that build naturally on their existing surgical skillset, such as MIGS. She offered the following steps to consider:
- Build the foundation in clinic: Perform gonioscopy on every cataract patient for a month; document angle grade, pigment, and the presence of peripheral anterior synechiae (PAS). If you commit to MIGS, commit to gonioscopy.
- Get trained and credentialed: Pick 1–2 MIGS to start (e.g., goniotomy or trabecular bypass). Attend a wet lab, watch surgical videos, and consider having an experienced colleague available for your first cases.
- Set up the room: Ensure your OR is stocked with all the instrumentation you may need, including a gonioprism (Dr. Kamat prefers Swan Jacob gonioprisms because she likes the control offered by the handle, but she noted that a physician could also start with a hands-free gonioprism). “It is also helpful to practice patient positioning and using the goniolens before you have a scheduled phaco-MIGS case. For patients scheduled for cataract surgery alone, I suggest practicing turning the head and scope (~30–45 degrees), ensuring you have a clear en face view of the angle, placing the gonioprism on the eye, and practicing touching the trabecular meshwork with a cannula.” Being comfortable with the maneuvers and having a good view is more than half the battle, she said, adding that practicing can set one up for success.
- Choose straightforward cases at first: Choose phaco candidates with mild to moderate POAG, open angles without PAS, and good corneal clarity.
- Debrief and review video: Record your first several cases, review them with your proctor/mentor, and keep a simple log (procedure, IOP, medications, complications, reoperations). Use it to refine case selection and technique for the best outcomes in your hands.
Add-on procedures during cataract surgery
Dr. Kandavel thinks that the biggest learning curve for the cataract surgeon is mastering the technique for achieving excellent, consistent angle visualization, regardless of which procedure is chosen. “Mastering direct gonioscopy is the best way to get consistency in MIGS procedures and their outcomes,” he said. “Once visualization is achieved, the most straightforward procedure now available, in my opinion, is the implantation of the iDose TR [travoprost intracameral implant, Glaukos]. Placement into the angle is relatively forgiving, and since it is scleral fixated, the target is much larger than the trabecular meshwork. There’s also less risk of obscuring your view with heme, and once in position, it tends to be secure and introduces the surgeon to a trigger-based implantation device. This sets the stage for iStent [Glaukos] implantation as a next step.” He noted that insurance coverage and patient acceptance vary with the patient population, but iDose TR and iStent are the most straightforward entry points to MIGS procedures for the cataract surgeon.
MIGS procedures are a good place to start, Dr. Kamat agreed, and within that category, she said canal-based stenting or goniotomy are likely the most approachable. These include trabecular bypass stents such as the iStent or Hydrus (Alcon) or goniotomy procedures such as the Kahook Dual Blade (New World Medical). “These procedures have a favorable safety profile, comparable postoperative management to cataract surgery alone, and have a similar recovery period as a typical cataract extraction.”
Dr. Kamat said it’s within the wheelhouse of a comprehensive ophthalmologist to master a couple of MIGS techniques. “If one wanted to expand his or her MIGS armamentarium, I would consider viscocanaloplasty, as I personally find that to be a highly effective and useful tool for glaucoma.” She added that while subconjunctival bleb-forming procedures such as the XEN Gel Stent (AbbVie), trabeculectomy, or glaucoma drainage devices are all important in the surgical management of glaucoma, they are not critical for the comprehensive ophthalmologist to master.
Dr. Kandavel encouraged surgeons to formulate their own algorithm for recommending and performing these glaucoma procedures (as standalone procedures or in conjunction with cataract surgery) as they gain experience and as more data is published. But he said surgeons should not feel limited because they can all be learned and mastered by any committed cataract surgeon.
“For instance, we would not prescribe only one medication drop to a patient because we are only comfortable with that drop; rather, we want to be familiar with the benefits of all medications and offer the best combination of medication available,” he said. “Similarly, MIGS procedures should be performed in a logical algorithm and should not be limited by experience or effort.”
Dr. Kandavel agreed with Dr. Kamat that surgeons can start with a limited number of procedures that they are comfortable with and then expand to others as they become more familiar with the techniques.
“At this point in time, we can break down angle-based procedures into the following larger categories: stenting procedures such as Hydrus and iStent, viscodilation and goniotomy procedures, and the last, for now, is pharmaceutical implantation,” he said.
Dr. Kandavel suggested starting with the iDose TR to get the surgeon prepared for angle-based visualization. Then, he suggested expanding to iStent, which he said leverages that same visualization for an angle stenting procedure. “The surgeon will have to be comfortable with retrieving and rethreading the stent for reimplantation in case the first pass is not successful and the target is more narrow,” he said, adding that this is an additional skillset. “Having microsurgical forceps for intracameral use is necessary. However, with practice, rethreading the stent onto the original insertion trocar is most efficient.”
The next step, he said, would be learning to incise and access Schlemm’s canal with a goniotomy. “This can be accomplished with devices such as a Kahook Dual Blade, SION [Sight Sciences], or Trabectome [MicroSurgical Technology],” he said. “These procedures are quick and still have an excellent safety profile, however, they are more dependent on good visualization and identification of anatomical landmarks to avoid complications such as hyphema or cyclodialysis cleft formation.”
From there, Dr. Kandavel said the surgeon can begin to access Schlemm’s canal via a canal threading procedure with viscodilation, such as the Via 360 (New World Medical) or Omni Surgical System (Sight Sciences). “Canalizing Schlemm’s canal and introducing the suture successfully can be challenging without first developing comfort with performing incisional goniotomy. These procedures can be coupled with a goniotomy as the catheter tip can be pulled to create a trabeculotomy up to 360 degrees,” Dr. Kandavel said. Once you’ve tried everything, you can more confidently recommend the appropriate treatment and really make a difference while already in the eye for cataract surgery or start to do standalone procedures, he added.
Pharmaceutical treatments and sustained release
Dr. Kamat said that sustained drug delivery is a great tool for the comprehensive ophthalmologist to offer, whether it is in the form of Durysta (bimatoprost intracameral implant, AbbVie) prior to cataract surgery to optimize the ocular surface disease preoperatively or placing iDose TR in combination with cataract surgery. “Any procedure that can improve IOP as well as diurnal IOP control while decreasing the dependence on topical medications can be hugely beneficial to a glaucoma patient,” she said. “Reducing the cost, treatment burden, compliance issues, and ocular surface disease associated with IOP-lowering drops can significantly improve patients’ quality of life. Furthermore, these interventions tend to be the most effective in mild to moderate disease, which is a common subset of glaucoma patients being managed by comprehensive ophthalmologists.”
Dr. Kandavel thinks a surgical option is a better choice than topical medication for the sake of compliance and efficacy. “One of the best ways to get started with MIGS procedures is to perform standalone iDose TR in pseudophakic patients,” he said. “Choose a patient who has difficulty putting in drops or is noncompliant and has already had SLT.” He added that having the cornea at its clearest and having the smallest incisions possible leads to good chamber stability and the best view.
“The iDose TR is truly a separate treatment modality from all other MIGS and in my opinion, can be added to any MIGS procedure in the appropriate patient,” Dr. Kandavel said. “Currently, I implant iDose TR in any willing patient who is already on a prostaglandin while performing cataract surgery. I’m also looking forward to longer-lasting versions that are on the horizon.”
Additional insights
Dr. Kandavel stressed that visualization is the key to getting comfortable with angle-based surgery. “Getting true en face position is the key,” he said. “For the beginning surgeon, hands-free prisms are light on the cornea, introduce fewer striae, and improve the consistency of the view overall. There are many different versions. It is nice to have a prism that does not compete with entry into the main incision and has a half or elliptical moon shape. These prisms can add cost to the procedure, but prioritizing the view is the key to success and is well justified as a small additional cost of the procedure at current reimbursement rates.”
He also finds that using trypan blue can aid in properly visualizing the trabecular meshwork landmarks, especially if the angle is lightly pigmented during preoperative evaluation. Using a dispersive viscoelastic on the gonioprism improves the view rather than a cohesive, he said. “Having a relatively pressurized eye to maintain chamber stability and reducing the incision size to prevent viscoelastic egress can be helpful as well. Tilt the scope and accentuate the patient’s head rotation away from you. If you use an ORA aberrometer [Alcon], consider taking it off for these procedures until you get used to the angles so as to not interfere with some of the MIGS inserters.” Dr. Kandavel added that watching videos and practicing can help.
About the physicians
Shivani Kamat, MD
Associate Professor
Director of the Glaucoma Fellowship
Glaucoma Service Lead
University of Texas Southwestern Medical Center
Dallas, Texas
Rom Kandavel, MD
Volunteer Clinical Instructor
Jules Stein Eye Institute
Colvard-Kandavel Eye Center
Encino, California
Relevant disclosures
Kamat: AbbVie, Alcon, Bausch + Lomb, Glaukos, Iantrek, New World Medical
Kandavel: Alcon, Glaukos, Tarsus Pharmaceuticals
Contact
Kamat: shivani.kamat@gmail.com
Kandavel: valleyeyedoctor@gmail.com