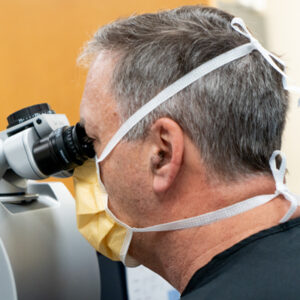
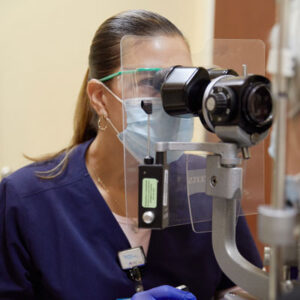
Practice Management
Fall 2025
by Liz Hillman
Editorial Co-Director

A new session at the 2025 ASOA Annual Meeting, “Aii: Building a Blueprint for Success,” gave attendees a strategy for successful adoption, integration, and implementation (Aii) of new technologies in their practice. The session was sponsored by iOR Partners, ModMed, Promptly, and RxSight.
Led by Patti Barkey, COE, a former ASOA president, and Carrie Jacobs, COE, ASOA President, this session provided the roadmap to help practices successfully bring in new technology and procedures.
Infrastructure considerations for successful Aii include staffing, scheduling, revenue cycle expertise, facilities, marketing, and education. The program dove into each of these areas and how they can be factors when adopting, integrating, and implementing a new technology or procedure.
Ms. Barkey said education is an area where many practices hit a roadblock. She said that Frank Bowden III, MD, said, “We’re only as good as the least enlightened person” in the practice. Clarifying, Ms. Barkey said that if that person has a touchpoint with the patient and they don’t understand what the practice is trying to accomplish with a new technology or procedure, they could hamper that product.
The session used real-world practice case studies to showcase successful Aii.
Office-based cataract surgery
Hugh Glatts, COE, Mittleman Eye, spoke about how his practice sought out office-based cataract surgery for several reasons—a growing population, decreased OR time at local ASCs with limited resource availability there, declining reimbursements, and more. Office-based surgery (OBS) not only addressed several limitations that Mittleman Eye was experiencing, but it also provided an opportunity for a new revenue stream, training abilities, and efficiencies that could lead to reduced expenses.
The steps to get a patient from the decision to have surgery to actually having the surgery takes 101 minutes/patient at an ASC, Mr. Glatts said. Several patients were dropping off somewhere in the process before they reached having the surgery. Office-based cataract surgery, conversely, takes 30 minutes.
“We’ve had a dramatic increase in the number of surgeries we’re doing because of our office-based surgery, and we’ve added no people to our employee list or our surgical department,” he said.
When it came to implementing office-based cataract surgery, Mr. Glatts said the first thing is to find the right partner. For Mittleman Eye, this was iOR Partners. From there, the practice considered its projected and future surgical volume to help determine if the practice would need more than one OR. The practice also had to consider bringing in a femtosecond laser (which it did) and the other supplies and lens inventory it would now have to store, determine the space for the OR(s), decide on a surgical equipment vendor, and decide which staff would be trained to work in the office-based OR.
Some of the challenge in implementation was changing the mindset of the doctors who were accustomed to performing surgery at an ASC. For these doctors, education about the benefits of OBS and visiting an established OBS was important.
For integration, Mr. Glatts explained how iOR Partners took the lead. The company took care of the setup, supplies, training, and accreditation. Mr. Glatts said the practice audited all their OBS cases and saw superior safety in this setting compared to the ASC.
Mr. Glatts said they have had OBS for 3 years, completing more than 5,000 cases in this setting. They have had no canceled surgeries, though a few rescheduled. In the time since OBS adoption, implementation, and integration, Mr. Glatts said the practice has experienced an increase in conversions for advanced-technology IOLs and an increase in refractive lens exchange procedures. It has implemented ICL procedures (STAAR Surgical) and has seen an overall increase in surgical volume and patient satisfaction. Additionally, employees being offered new responsibilities and engagement has increased their work satisfaction.

Source: ASCRS
EMR changes
Guido Piquet, MBA, COE, Mann Eye Institute, said that EMR rollouts can be “brutal.” He’s been through two EMR rollouts in his career, but the second one was not like the first.
“After surviving that first EMR system, I swore that I would never change systems again. … But as the years passed, I saw that our current solution was no longer serving our vision,” Mr. Piquet said.
Mann Eye Institute sought to change from its prior EMR system because 1) it couldn’t fit the boutique patient experience the practice wanted; 2) clinical and revenue cycle workflow inefficiencies slowed operations and growth; 3) there were patient-related communication deficiencies creating rework and frustration for patients and staff; and 4) software complexity was a burden and stemmed evolution. “We really needed a partner who could scale with us,” he added later.
When it came to partnering with a new EMR company, the practice knew it needed to work with one that shared its values (one of a growth mindset, for example), that understood that implementation process is critical, and that had interoperability that extends the value of the investment. The practice found these qualities in ModMed.
For implementation, Mr. Piquet said a core team oversaw the change, guided by ModMed. “Super users,” or key players/physician champions, were identified and received additional training so they could be a resource for others during and after go-live. The implementation plan was extensive and detailed.
“Despite everything that we did right on go-live … when we first went live, it was rough. It was probably rougher than the first time we did it. Why? It’s largely because this time, we were about four times the size of when I did it the first time. It’s obvious to say, but when you’re bigger, it’s so much harder to navigate change successfully,” Mr. Piquet said.
There were doctors who were asking to revert to the old system after go-live, Mr. Piquet said, but he knew this time around, it wasn’t about the system. They were afraid.
“Instead of retreating, we leaned in,” Mr. Piquet said, noting that the super users were the “secret ingredient,” providing support and solutions for the doctors who were struggling with the system.
After 3.5 years with ModMed Klara, the practice has seen improved efficiency and patient collaboration, as well as an increase in patients with the same amount of staff. The system has revolutionized its patient communications (no more phone tag) and reduced time to collect payments and introduced new payment methods. Going forward, Mr. Piquet said they are looking into ambient listening tools to help the practice.
In the end, Mr. Piquet said that it’s important to understand that resistance is not defiance, rather fear of loss. “If you give people a clear vision for why the change is necessary, you can lead them through it,” he said.
Humanizing healthcare
Brooke Flint, COE, senior regional director, Eyecare Partners, oversees the Ohio division, which is composed of 11 practices, 140+ providers, in more than 40 locations.
Almost 2 years ago, the team got together to review where they wanted to go operationally and identified areas of need.
“When our team got together, we determined we’re not effectively able to do business, and we’re not making it easy for our patients to do business with us with our current technologies. So we wanted to determine what was the best technology to use for our patient experience,” Ms. Flint said. “We identified the need to change technologies and adopt a new platform.”
Ms. Flint said the practice group was using 4–6 software platforms to perform daily work. This all came with multiple logins, passwords, workflows, integrations, support teams, and subscriptions. Too many workflows, Ms. Flint said, were affecting the patient experience. “Our need was for a better practice workflow software solution,” she said.
In the adoption phase, the team began with a workflow audit, gaining an understanding of what was and was not working, measured what matters, and consulted with peer practices they trusted. To implement a change based on what they learned, Ms. Flint said they knew they needed a partner platform that would work across multiple practices with complex workflows. “We needed some ability to configure to keep it specialized to our practices and make it feel like it was still local to the brand but to have something that’s easy to be duplicated,” she said.
After identifying Promptly as a solution, the practice group’s implementation included creating a cross-functional team of super users who would champion the project. “Once you implement into one practice and it goes really well, pulling that team into the next group, they become your champions at that next site or location,” she said.
She said continued education for the staff on the “why” behind the project and an emphasis on defining success by stages (progress, not perfection) was also helpful.
At the integration stage, Ms. Flint said it’s important to ask the hard questions early and learn the support process. It’s also important to collaborate with partners to create detailed process documents to help the team integrate new workflows. In addition, the team built feedback loops with practice users.
Since adopting, implementing, and integrating Promptly, Ms. Flint said the regional practice group consolidated 6 platforms, resulting in an expected $500,000+ in savings in 2026. Manual work was reduced by 25% or more through automated workflow tools. In addition, no-show appointments were reduced by 50%. The practice expects to gain 50% more functionality, save more than 5 minutes per patient at check-in, and it negotiated a better credit processing rate.
“Technology should make things easy for patients, convenient for staff, and the right technology can improve the staff and patient experience,” Ms. Flint said.
‘Bringing Light to Life’
As the title of her presentation, “Bringing Light to Life,” suggests, Kasey Gantz, COO, Alliance Vision Institute, said this is what the Light Adjustable Lens (LAL, RxSight) did for her practice a couple of years ago.
“We believed the lens technology was aligned with the practice’s mission and the mission of our surgeon, and that was to bring the newest technology in a state-of-the-art way and obviously have clinical efficacy and safety behind it,” Ms. Gantz said.
Their adoption of the LAL was done with minimal disruptions, but Ms. Gantz said the adoption was done very strategically, staged, and slowly because they wanted to make sure they were getting the outcomes they wanted for these patients.
“We are a practice that comanages care with external OD offices, so initially we didn’t comanage these lenses. The reason we chose to do that was because we wanted the ability to watch the surgical outcome and manage the adjustment period for a patient,” she said, noting this was done for the first 10 patients before they developed a comanagement strategy.
During the adoption phase, there were clinical flow nuances in the postop period that required attention. She said RxSight’s support team was invaluable with ideas to help with clinic flow. Ms. Gantz also emphasized the importance of whole-team education for success of onboarding a new technology.
In the integration phase, Ms. Gantz said it was important to be patient during workflow optimization, and both ODs and MDs were trained to perform the Light Delivery Device adjustments.
The decision to adopt through full capability with the LAL, Ms. Gantz said, was between 90 and 120 days. “Within the first year we gained hundreds of happy patients. It quickly became the top lens that we were converting,” she said.