Cornea: Lessons learned
December 2023
by Liz Hillman
Editorial Co-Director
The topic of ocular allergy and associated conjunctivitis is broad, ranging from seasonal to perennial, acute/episodic to chronic. EyeWorld asked ophthalmologist and ocular surface specialist Esen Akpek, MD, and ocular allergist/immunologist Leonard Bielory, MD, to provide an overview on the topic.


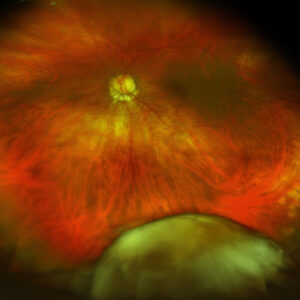
Source: Esen Akpek, MD
Dr. Bielory said the area of ocular allergy is multidisciplinary. He also said it’s important to realize that “for something to be clinically relevant, we all have different tolerances.” He explained that patients have different thresholds where they think an allergy is impacting their quality of life. “When it comes to symptoms, we all have the propensity to develop allergies; 40% complain of them,” he said. “It reaches a level where it breaks through what I call their level of tolerance.”
Once that level is reached, that’s when the patient seeks professional medical help.
Ocular symptoms for most allergies, Dr. Bielory said, are red, itchy, and/or tearing eyes. Depending on what their symptoms are seems to determine what type of medical professional the patient seeks help from first. Dr. Bielory pointed to the Allergies, Immunotherapy, and RhinoconjunctivitiS (AIRS) surveys published in 2014, which found that patients who had itchy eyes were seeking medical treatment from pediatricians, ophthalmologists/optometrists, and nurse practitioners/physician assistants, while nasal congestion as a symptom had patients visiting otolaryngologists, allergist/immunologists, and family medicine physicians.1
While ophthalmologists will see patients who experience ocular allergy, Dr. Bielory said he thinks ophthalmologists will try a few strategies and if those don’t work, refer to an allergist. The chances of allergic symptoms being only in the eyes occurs in 5–10% of cases, Dr. Bielory said. If physicians see and treat only the eyes, they’re not dealing with the whole patient.
“The patient might not be satisfied just taking eye drops when they have sneezing, nasal congestion, and a variety of other conditions. The allergist acts like a medical ophthalmologist because ophthalmologists are primarily surgeons, but they treat symptoms that they see—tear film dysfunction as well as ocular allergy and more severe forms,” he said.
With more severe ocular allergy cases, such as atopic keratoconjunctivitis, vernal conjunctivitis, and giant papillary conjunctivitis, Dr. Bielory said an allergist who might see the patient first needs to work in concert with an ophthalmologist. “The international consensus of treatment on ocular allergy … shows there should be cross fertilization,” he said.
In the ICON paper,2 which explored the diagnosis and management of allergic conjunctivitis, the authors described a “predominance of self-management [that] increases the risk of suboptimal therapy that leads to recurrent exacerbations and the potential development of more chronic conditions that can lead to corneal complications and interference with the visual axis.” The authors wrote that “successful management includes overcoming the challenges of underdiagnosis and even misdiagnosis by a better understanding of the subtleties of an in-depth patient history, ophthalmologic examination techniques, and diagnostic procedures, which are of paramount importance in making an accurate diagnosis of [ocular allergy.” They advocated for “appropriate cross-referral between specialists (allergists and eyecare specialists).”
Whether it’s an allergist or ophthalmologist first seeing the patient experiencing ocular symptoms, Dr. Bielory pointed to Figure 2 in the ICON paper, which leads the physician through an algorithm of the different assessments to be done by the allergist and/or ophthalmologist, followed by diagnoses and severity-based treatment.
Dr. Akpek detailed her process when she has a patient with known ocular surface disease or symptoms of discomfort and blurred vision.
“I do a thorough symptoms evaluation, past medical history, medication history, and review of the system with particular attention to underlying collagen vascular, inflammatory, or allergic diseases, which might be comorbid issues. When a patient is asked about their symptoms, they usually complain of multiple symptoms that could be confusing. That’s when I ask them about the most bothersome symptom,” she said. “Patients with allergy usually complain of itching, although some patients describe it as stinging. Exam findings are also important. Presence of upper tarsal conjunctival papillae is an important finding, but in some severe chronic cases, such as atopic or vernal keratoconjunctivitis, these might not be present and replaced with scarring.”
From a treatment standpoint, Dr. Bielory said he thinks most physicians follow the same consensus, going “from lubricants/antihistamines to multiple action agents. If that doesn’t work, you go to immunomodulators, steroids, cyclosporine, and immunotherapy,” he said. Dr. Bielory said there are studies that show patients can be exposed to 10–100 times more allergens if they’re on the appropriate immunotherapy.
Dr. Akpek said due to the overlap that can occur among the different types of allergic conjunctivitis and sometimes diseases changing from one form to another (such as seasonal allergic conjunctivitis turning into perennial), she thinks it’s best to determine the chronicity and the changes on the ocular surface to determine severity. “Treatment should be tailored according to chronicity and severity of the physician-measured clinical signs,” Dr. Akpek said. “For acute seasonal allergic conjunctivitis, mast cell stabilizer plus antihistamine medications would be helpful. But any chronic allergy should be treated with anti-IL-2 medications, such as tacrolimus or cyclosporine. Steroids should be avoided as much as possible.”
In terms of new options for ocular allergy treatment, Verkazia (cyclosporine ophthalmic emulsion, Santen) was approved in 2021, and also in 2021, Dextenza (dexamethasone ophthalmic insert, Ocular Therapeutix) received approval for ocular allergy as an additional indication. Johnson & Johnson Vision received approval for the first drug-eluting contact lens—ACUVUE Theravision with Ketotifen—in 2022 for treatment of allergic conjunctivitis along with vision correction.
Dr. Bielory regularly reviews advances in therapeutics for ocular allergy.3 He said there is still a large unmet need to serve patients who experience allergic conjunctivitis. Among several active areas of research, Dr. Bielory pointed to a 2022 paper about immunobiologicals and ocular surface disease, which concluded that immunobiologicals can provide “a more directed therapeutic approach to ocular inflammatory disorders” and another recent paper that looked at type 2 cytokine pathways that have impacts on both the skin and the ocular surface, which could help lead areas for immunomodulatory intervention.
As an allergist, Dr. Bielory said his advice to his colleagues in ophthalmology is to think more holistically when they see signs of ocular allergy, recommending to the patient that an allergist get involved if the eye is not the only organ system being affected.
As a lesson learned, Dr. Akpek said that as ophthalmologists treat meibomian gland dysfunction and dry eye, they should not forget about allergy. She also noted that ASCRS recommends the minimal exam to include flipping of the upper lids to look for papillary changes.
About the physicians
Esen Akpek, MD
Bendann Family Professor of Ophthalmology
Wilmer Eye Institute
Johns Hopkins University School of Medicine
Baltimore, Maryland
Leonard Bielory, MD
Professor of Medicine, Allergy, Immunology and Ophthalmology
Hackensack Meridian School of Medicine
Springfield, New Jersey
References
- Bielory L, et al. Ocular and nasal allergy symptom burden in America: the Allergies, Immunotherapy, and RhinoconjunctivitiS (AIRS) surveys. Allergy Asthma Proc. 2014;35:211–218.
- Bielory L, et al. ICON: Diagnosis and management of allergic conjunctivitis. Ann Allergy Asthma Immunol. 2020;124:118–134.
- Bielory L, Schoenberg D. Emerging therapeutics for ocular surface disease. Curr Allergy Asthma Rep. 2019;19:16.
Relevant disclosures
Akpek: None
Bielory: AccuPollen, Blueprint Medicines, Dr. Bielory’s Remedies, Eyevance, Genentech, Regeneron, Santen
Contact
Akpek: esakpek@jhmi.edu
Bielory: drlbielory@gmail.com