ONLINE EXCLUSIVE
Cornea
August 2023
by Ellen Stodola
Editorial Co-Director
Meibomian gland dysfunction (MGD) is a broad term that covers various types of meibomian gland alterations. In this EyeWorld Online Exclusive, Vincent de Luise, MD, details the meibomian glands, how they differ in MGD, classification of MGD, and treatment options.

Meibomian glands provide the main source of lipids for the human tear film, Dr. de Luise said. “Meibomian glands are large sebaceous glands located as separate gland strands in parallel arrangement within the tarsal plates of the eyelids,” he said. There are, on average, about 30 meibomian glands in the upper eyelid (range of 25–40) and about 25 meibomian glands in the lower eyelid (range of 20–30). Upper eyelid meibomian glands are longer, averaging about 6 mm in length, whereas lower eyelid meibomian glands are shorter, averaging about 2 to 3 mm in length.
Meibum is the lipid secretion of these glands. “These lipids create a hydrophobic barrier and seal off the aqueous portion of the tear film, thus retarding evaporation of water from the ocular surface. This enhances the protective properties of the tear film,” Dr. de Luise said.1,2 In healthy eyelids, the meibomian gland orifices are open, and any expressed meibum is clear at room temperature.
How do the meibomian glands differ in MGD?

One stratification of MGD is into hypersecretory forms and hyposecretory forms, Dr. de Luise said. Whether hypersecretory or hyposecretory, in MGD there is abnormal meibum production, with more rapid evaporation of the tear film during the interblink interval.3 The International Workshop on Meibomian Gland Dysfunction used three parameters to classify MGD: meibomian gland morphology, tear film osmolarity, and Schirmer testing.
MGD is an underdiagnosed and undertreated disease, Dr. de Luise said, with an estimated 70% of Americans over the age of 60 having some degree of MGD.4 “Meibomian glands in MGD differ from normal in that there is an altered lipid composition of the meibomian gland secretions, which in turn destabilizes the tear film. These abnormal secretions can have a direct toxic effect on the ocular surface,” he said.
What are the grades/levels of MGD?
Source (all): Vincent de Luise, MD
The classification system proposed by the International Workshop on Meibomian Gland Dysfunction distinguishes among the subgroups of MGD based on the level of secretions (hypersecretory and hyposecretory) and subdivides those categories by potential consequences and manifestations, Dr. de Luise said. The hyposecretory state is further stratified into hyposecretory or obstructive forms. MGD is the most common type of obstructive hyposecretory dysfunction. Some classification schemes for MGD stratify it into four grades or levels of disease intensity, he said.
Dr. de Luise said that rather than stratifying MGD into four grades or levels, it is easier to remember a three-grade paradigm for diagnosis and therapy.
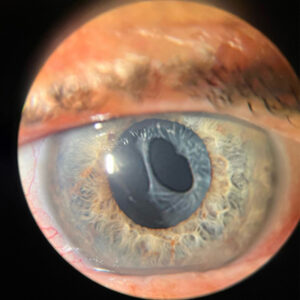
Grade 1 MGD: The meibum is slightly turbid but can be expressed (Figure 1).
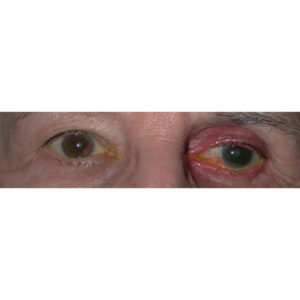
Grade 2 MGD: The meibum is expressible with difficulty and is cheesy, congealed, or inspissated (Figure 2).
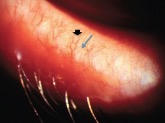
Grade 3 MGD: Meibomian gland orifices are completely epithelialized, with lid margin telangiectasias (Figure 3, blue arrow), and meibum cannot be expressed.
What are the treatment recommendations for each level of MGD?
Dr. de Luise noted that MGD cannot be cured but can be treated and often controlled with the use of heat therapy, combination strategies (such as short courses of topical azithromycin gel), and dietary changes with the addition of more omega-3s. Oral minocycline or doxycycline is another option; however, a 2021 Cochrane analysis found insufficient evidence for efficacy with oral antibiotics.5 MIEBO (perfluorohexyloctane ophthalmic solution, Bausch + Lomb) is a preservative-free eye drop that was recently approved by the FDA. It stabilizes tears and reduces tear evaporation. Patients in a Phase 3 clinical trial experienced a rapid decrease in dryness after using the drops.
In MGD the altered fatty acids and inflammation lead to saponification, a detergent action. Baby shampoo exacerbates this problem, he said, adding that saltwater lid scrubs are better.
Technologies include those to open meibomian glands directly, to heat the meibomian glands to liquefy the congealed meibum, or to apply pressure to the meibomian glands to express them, Dr. de Luise said. He mentioned heating and compressive strategies, such as Bruder Moist Heat Eye Compresses and OCuSOFT lid scrubs, and mechanical devices that provide accurate thermal heat as well as compressive pulsation, such as the LipiFlow (Johnson and Johnson Vision), Systane iLux2 (Alcon), TearCare system (Sight Sciences), and MiBo Thermoflo systems (MiBo Medical). Other heating strategies include intense pulsed light, like the LacryStim IPL (Quantel Medical), OptiLight (Lumenis), and Epi-C Plus (Essilor Instruments).6,7
There are several microblepharoexfoliation devices that mechanically scrub the eyelids, eyelashes, and skin with a gentle mechanical brushing system. These devices are designed to remove eyelid debris gently and can sometimes open blocked meibomian gland orifices.6 Opening capped, keratinized, or epithelialized meibomian gland orifices can be done with Maskin probes, Dr. De Luise added.
Based on the stage of the disease, Dr. de Luise offered the following recommendations:
MGD Stage 1: Change to an omega-3 diet, applying heat and compression to the eyelids.
MGD Stage 2: Use Stage 1 strategies and add technological approaches of thermal pulsation, short courses of topical azithromycin gel.
MGD Stage 3: Use Stage 1 and 2 strategies and add direct opening of capped meibomian gland orifices with Maskin probes; consider a short course of oral minocycline or doxycycline.
MGD pipeline
Dr. de Luise said that there are several companies exploring pipeline products for posterior blepharitis and MGD.
- AZR-MD-001 (Azura Ophthalmics): This is a selenium sulfide keratolytic ointment formulation that prevents protein buildup in meibomian gland ducts. This buildup blocks oil secretion and leads to dryness. Selenium sulfide has a triple mechanism of action in MGD: It decreases the production of keratin, breaks down the bonds between abnormal keratin proteins, and increases meibomian gland lipid quantity. Patients who tested the medication in a Phase 2 trial had healthier amounts of oil and reduced dry eye symptoms.
- AXR-270 (AxeroVision): This is a once daily 2% glucocorticoid cream that is being compared to its excipient placebo in a Phase 2 trial analyzing eye discomfort score, tear breakup time, and total corneal fluorescein staining score.
- XDEMVY (TP-03, Tarsus Pharma): This recently FDA-approved ophthalmic formulation of the acaricide lotilaner is labelled for anterior blepharitis and is now being evaluated in a Phase 2a clinical trial for MGD and a separate trial for oculocutaneous rosacea.
About the physician
Vincent de Luise, MD
Assistant Clinical Professor of Ophthalmology
Yale University School of Medicine
New Haven, Connecticut
References
- Knop N, Knop E. Meibomian glands. Part I: anatomy, embryology and histology of the Meibomian glands. Ophthalmologe. 2009;106:872–883.
- Butovich IA. Lipidomics of human Meibomian gland secretions: Chemistry, biophysics, and physiological role of Meibomian lipids. Prog Lipid Res. 2011;50:278–301.
- Mizoguchi S, et al. Ocular surface inflammation impairs structure and function of meibomian glands. Exp Eye Res. 2017;163:78–84.
- Chader GJ, Taylor A. The aging eye: normal changes, age-related diseases, and sight-saving approaches. Invest Ophthal Vis Sci. 2013;54:ORSF1–4.
- Onghanseng N, et al. Oral antibiotics for chronic blepharitis. Cochrane Database of System Reviews. June 2021.
- Bouchard C. Diagnoses and management of blepharitis. Review of Ophthalmology. Sept. 2022.
- Yan S, Wu H. Efficacy and safety of intense pulsed light therapy for dry eye caused by meibomian gland dysfunction: a randomized trial. Ann Palliat Med. 2021;10:7857–7865.
Relevant disclosures
de Luise: None
Contact
de Luise: vdeluisemd@gmail.com