Glaucoma
December 2022
by Liz Hillman
Editorial Co-Director
When the term MIGS (microinvasive glaucoma surgery) was first coined more than a decade ago, there were only a few options in the space, and they were often referred to by their brand name, not the mechanism of action. Since then, however, the MIGS space has grown significantly with many options addressing the same outflow pathway. As such, it might be time to start talking about MIGS in terms of procedural categories.
“The MIGS space has expanded throughout the years,” said Brian Francis, MD. “There are some novel mechanisms that are being introduced, but there are also a lot of procedures in the same space. I think it makes sense to talk about the mechanism of action rather than the name of the procedure itself.”
As Robert Noecker, MD, put it, “we’re at critical mass” with multiple entries available in each space, so “it only makes sense to talk about these in categories now.”
“It wasn’t as important before because there were only a couple of things to think and talk about and everyone was on the same page. Now many companies offer multiple strategies and operate in different parts of the MIGS spectrum. It’s important to do this to reduce confusion and help sort out the technologies,” Dr. Noecker said.
Dr. Noecker said MIGS has followed a similar trajectory to glaucoma medications 2 decades ago. “First all we had was [timolol], but now we also have prostaglandins, alpha agonists, rho-kinase inhibitors, CAIs, and others.” There are multiple options, and classifying based on mechanism of action is a way to organize things, he said, adding that when billing and coding a procedure, a brand is not specified, so understanding the procedural category is helpful.

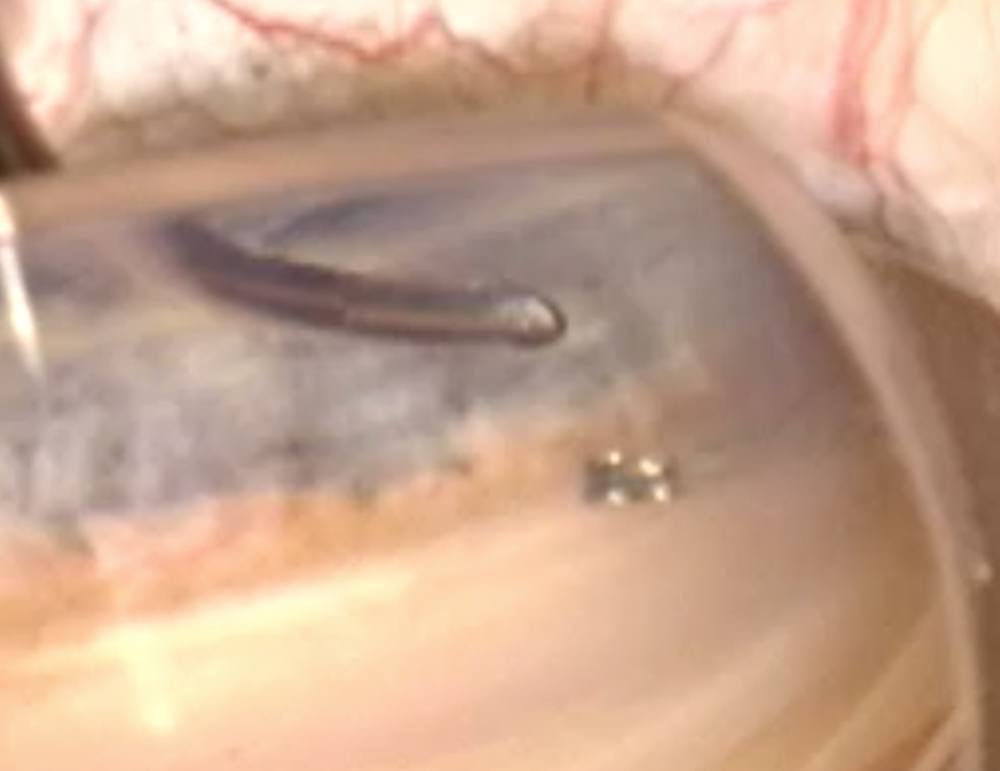

B. Hydrus in place in the canal with adjacent area of goniotomy visible (white area visible is back of Schlemm’s canal)
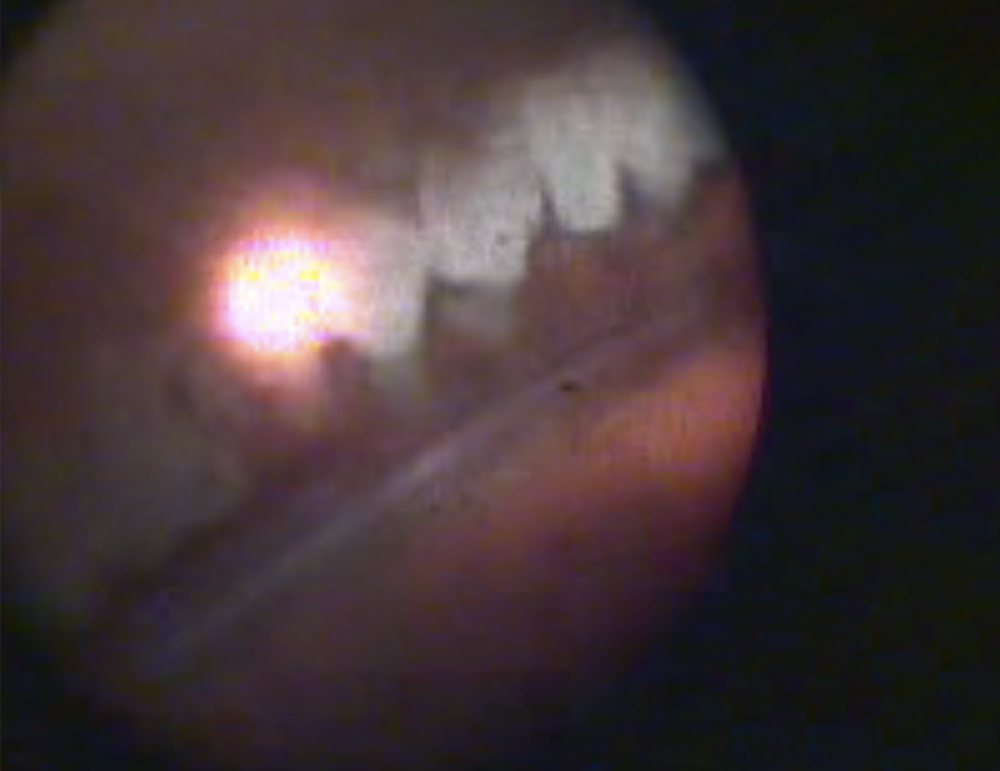
C. Endoscopic view of ciliary processes with ECP laser-treated white processes visible
D. Gonioscopic view of TrabEx performing goniotomy
Source (all): Robert Noecker, MD
MIGS procedural categories
Here is a breakdown of the categories and the different brands available in each.
Trabecular bypass: This category includes iStent (Glaukos), of which there are several generations now, and Hydrus (Alcon, formerly Ivantis). These devices provide a conduit through which aqueous can bypass a dysfunctional trabecular meshwork and flow into Schlemm’s canal.
Ab interno goniotomy/trabeculotomy: This category includes the Kahook Dual Blade/KDB Glide (New World Medical), TrabEx and TrabEx+ (MicroSurgical Technologies), Trabectome (MicroSurgical Technologies), and the goniotomy-assisted transluminal trabeculotomy (GATT) procedure. Dr. Noecker also mentioned iAccess (Glaukos). According to Dr. Noecker, these procedures remove a section of the trabecular meshwork to increase outflow into Schlemm’s canal. “The end result is the opening you leave behind, so that’s why I think it’s important to not specifically talk about devices you use but the end result,” he said. According to Dr. Francis, there is a small distinction within the category of procedures that tear through the trabecular meshwork (GATT) and those that remove trabecular meshwork tissue (the others).
Canal dilation procedures: These include the iTrack Surgical System (Nova Eye Medical) and OMNI Surgical System (Sight Sciences). According to a paper by Riva et al., canaloplasty functions via viscodilation of Schlemm’s canal “as it breaks adhesion inside the canal, stretches the trabecular plates by means of micro-perforations into the inner wall of the trabecular meshwork and separates herniations of the inner wall of the trabecular meshwork into the outer wall collector channels.”1
Goniotomy/trabeculotomy-canaloplasty (hybrid procedures): The OMNI Surgical System performs both trabeculotomy and canaloplasty. The STREAMLINE Surgical System (New World Medical) performs goniotomies in the trabecular meshwork and delivers a small amount of OVD into Schlemm’s canal.
Suprachoroidal access devices: CyPass (Alcon), recalled in 2018 due to the potential for endothelial cell loss, was a device in this space. This device bypassed Schlemm’s canal and the traditional outflow pathway, facilitating outflow directly from the anterior chamber into the suprachoroidal space. Dr. Noecker said there is work being done to bring back a device that uses the suprachoroidal space. Dr. Francis also mentioned the MINIject (iSTAR Medical) and iStent Supra (Glaukos).
Ciliary body procedures: These include endocyclophotocoagulation (ECP) and MicroPulse Laser Therapy (Iridex). These procedures, Dr. Noecker said, contribute to aqueous reduction and may increase uveo-scleral outflow. There is also some evidence that the latter may increase suprachoroidal or trabecular outflow, according to Dr. Francis.
Bleb-forming “MIGS”: The PreserFlo MicroShunt (Santen, not FDA approved in U.S.) and the XEN Gel Stent (Allergan) fall into this category. Dr. Noecker said they’re not quite MIGS because they are a little more invasive with the formation of a bleb and use of mitomycin, but they are still “basically bypass procedures” that are less invasive than traditional filtering procedures.
Why is categorizing helpful?
Dr. Francis said that it’s good to know these general categories, as well as the subtle differences among the procedures within the categories. First, he said, it can help you decide the procedures you want to do on a regular basis.
“You don’t have to become proficient in multiple procedures that are in the same category. It makes more sense to span two or three different categories within your armamentarium,” he said.
Dr. Francis said it’s helpful to know the different categories and what they address to customize choices for patients based on their disease and anatomy.
“You don’t have to become proficient in multiple procedures that are in the same category. It makes more sense to span two or three different categories within your armamentarium.”
Brian Francis, MD
“That can sometimes give you an idea of what procedures might be more successful depending on how they work,” he said. “The categories also help if you’re thinking about combining different procedures. You want to combine procedures that are from a different category. For instance, you might not want to do two trabecular bypass stents. That’s not going to be as helpful as combining a trabecular bypass with something that reduces aqueous humor production or opens up the canal 360 degrees.”
Dr. Noecker said that the variability in eye anatomy influencing MIGS efficacy makes understanding the different categories important. It also highlights the need to have experience across the different categories.
Both Dr. Noecker and Dr. Francis said insurance coverage can play a role in why a surgeon might want to have experience in different MIGS categories as well.
“It’s about having backup options. Some patients don’t want to have a device put in
their eye. It’s nice to have another option,” Dr. Noecker said. “I like to hedge my bets, so I do a lot of combining of these procedures and understanding what makes sense to combine, what complements each other vs. doing the same thing.”
In terms of choosing an option within each category, Dr. Noecker said to go with what you’re good at. “Figure out which one works best in your hands and go with it,” he said. Dr. Francis said without head-to-head data showing which MIGS is better, it boils down to what you’re comfortable with. “Within the same category, generally, they are similar in terms of their mechanism of action and efficacy. I don’t think it matters that much which you choose,” he said.
Dr. Francis said trabecular bypass stents are the first step for most cataract surgeons. As a second step, he advised a goniotomy/trabeculotomy or combined canaloplasty-goniotomy/trabeculotomy procedure.
“The reason those are nice is you can do them without cataract surgery,” he said. “The other category you might want to consider is an aqueous humor reduction procedure. Those can be combined with any procedure along the way.”
Dr. Noecker said that each of these spaces has evolved and gotten better, but there is still room for improvement.
“The techniques got better. The instrumentation got more elegant. It’s all with the goal of decreasing side effects, which in this case is primarily bleeding. I think all of the technologies have improved, but they all could continue to be better,” he said. “There is always room for improvement to [reduce the] chance of sticking a device in the wrong place.”
Dr. Francis said he’d like to see a suprachoroidal stent come back to the market.
“I know there are a couple in the pipeline that are being studied right now; they’re in trials that are ongoing. I think that is an area that will be reopened in the near future. It’s not necessarily better than the other procedures but it’s different. We’re accessing a different outflow pathway than the traditional trabecular outflow,” he said, adding “it can be nice to have access to a different outflow pathway to try to enhance the aqueous outflow rate.”
About the physicians
Brian Francis, MD
Doheny Eye Institute
UCLA David Geffen School of Medicine
Los Angeles, California
Robert Noecker, MD
Ophthalmic Consultants of Connecticut
Fairfield, Connecticut
Reference
- Riva I, et al. Canaloplasty in the treatment of open-angle glaucoma: a review of patient selection and outcomes. Adv Ther. 2019;36:31–43.
Relevant disclosures
Francis: Alcon, Allergan, BVI, Iridex, iSTAR Medical, MicroSurgical Technologies, Santen
Noecker: Allergan, Alcon, Glaukos, Iridex, MicroSurgical Technologies, New World Medical, Nova Eye Medical, Santen, Sight Sciences
Contact
Francis: bfrancis@doheny.org
Noecker: noeckerrj@gmail.com