Glaucoma: Hot topics in ophthalmology
December 2022
by Liz Hillman
Editorial Co-Director
While glaucoma specialists are likely familiar with MicroPulse Laser Therapy (Iridex) as a non-incisional, non-pharmaceutical glaucoma therapy, Tomas M. Grippo, MD, and Marc Toeteberg-Harms, MD, called it an “ace up your sleeve” and one that can be adopted by any surgeon who treats glaucoma patients.
Drs. Grippo and Toeteberg-Harms shared their thoughts with EyeWorld on the technology, which was initially developed in 2015 and has seen a few updates in the years since.
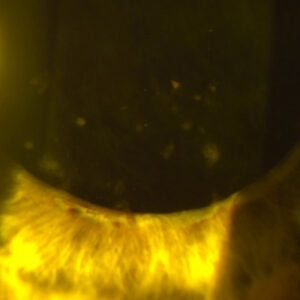
First, they described MicroPulse Transscleral Laser Therapy (MicroPulse TLT) as different from continuous wave transscleral cyclophotocoagulation (CW-TSCPC) and endoscopic cyclophotocoagulation (ECP). The company describes it as “tissue sparing,” and Drs. Grippo and Toeteberg-Harms said that with MicroPulse TLT the laser does not fire continuously. Rather, it “chops up the energy into smaller micropulses,” allowing for more thermal control and less tissue damage. In addition, MicroPulse TLT is non-incisional.
“While the mechanism of action is not fully understood, it is theorized that MicroPulse TLT enhances the natural aqueous outflow pathways of the eye (conventional and non-conventional) as opposed to restricting aqueous production only,” they said. “MicroPulse TLT also focuses the laser energy on a different part of the ciliary body than both CW-TSCPC and ECP. MicroPulse TLT delivers energy to the pars plana portion of the ciliary body or approximately 3 mm back from the surgical limbus.”

Source: Brian Jerkins, MD
They also said that MicroPulse TLT can be performed in many different types of glaucoma and severity levels.
“It is a treatment option in moderate to severe glaucoma, prior to or post-incisional surgery, and in general becomes a surgical option once maximal tolerated pharmacological therapy and trabeculoplasty have failed to control the disease,” they said. “Individual patient characteristics, like the status of the angle, conjunctiva, lens, cornea, if the patient is taking or not taking anticoagulation, are less relevant when performing this procedure, and all of this makes this tool a great addition to our surgical armamentarium.”
In terms of the learning curve, Drs. Grippo and Toeteberg-Harms said it is minimal and that this procedure is generally performed at an ASC. They said that IOP reduction is generally 25–35% if using settings as described in the dosimetry and patient selection guidelines that were published earlier this year (2500 mW, 31.3% duty cycle, and 4 to 5 sweeps at a sweep velocity of 20 seconds each per hemisphere).1
The physicians think that MicroPulse TLT should be considered once the patient has reached maximum tolerated pharmaceutical therapy and other trabeculoplasty options (ALT/SLT/MLT) have failed to adequately control the disease.
“A conservative approach is to use it after MIGS procedures, trabeculectomy, tube shunts, or non-penetrating procedures have become ineffective to fully control the disease. Another scenario could be a patient with moderate to severe open-angle glaucoma or angle-closure glaucoma without prior incisional or filtering glaucoma surgery on maximum tolerated medications,” Drs. Grippo and Toeteberg-Harms said. “Like any glaucoma procedure, it is important to keep in mind that the IOP-lowering effect can diminish over time, or the underlying pathophysiologic disease mechanisms can continue to progress, and the remaining effect may not be enough to control the disease anymore. Therefore, routine checkups need to be performed.”
As a technique pearl, the physicians said it’s important to use a transparent, optically neutral coupling agent, such as lidocaine gel. This offers more effective power transmission. They said to place the footplate of the MicroPulse P3 Device with its “bunny ears” at the limbus or slightly posterior to the limbus if this structure is not well defined. From there, gently compress the conjunctiva for optimal laser transmission. They said to exclude the 3 and 9 o’clock hours.
It’s also important to understand sweep velocity. “Power, duty cycle, sweep velocity, and the number of sweeps all factor into the success of the procedure,” Drs. Grippo and Toeteberg-Harms said. “In the past, sweep velocity has been the least controlled parameter. Think of moving your finger in and out of a candle flame. The slower you move your finger, the higher the induced tissue temperature. This can be compared to MicroPulse TLT; when we slow down, we deliver more laser energy and heating to that tissue. Until recent work was published,2 highlighting the importance of sweep velocity as having a high impact on the success of the procedure, this variable was probably the most under-appreciated and significant factor to consider with MicroPulse TLT. We see correlation between slower sweep duration and greater IOP reduction.”
From a safety standpoint, the physicians noted that most articles in peer-reviewed literature conclude that the MicroPulse TLT procedure is safe and effective, but like any glaucoma procedure, it is not without the potential for side effects.
“Now that we have a better understanding of dosimetry, surgical technique, patient selection, and the availability of the revised probe that allows for more posterior and stable treatment, many side effects can be prevented or minimized,” they said.
In general, postop care is less demanding compared to most glaucoma procedures.
“No cycloplegics or antibiotics are routinely required after MicroPulse TLT. Topical steroids and/or NSAIDs are typically the only medications required,” Drs. Grippo and Toeteberg-Harms said. “Glaucoma medications are typically initially continued after MicroPulse TLT and later tapered based on the IOP-lowering effect.”
They said that the maximum IOP-lowering effect can be expected between 4–6 weeks, but an initial response can be seen within the first week. For a more robust effect or if treatment seems to wear off over time, retreatments are possible.
“MicroPulse TLT is a titratable procedure that can be repeated without limiting the use of other therapies. The possibility to retreat is one of the benefits of this procedure. In the literature, two to three retreatments over time have been reported for some patients,” Drs. Grippo and Toeteberg-Harms said.
About the physicians
Tomas M. Grippo, MD
Founder and Director
Grippo Glaucoma and Cataract Center
Buenos Aires, Argentina
Marc Toeteberg-Harms, MD
Associate Professor
Medical College of Georgia
Augusta University
Augusta, Georgia
References
- TM Grippo, et al. Evidence- based consensus guidelines series for MicroPulse Transscleral Laser Therapy: dosimetry and patient selection. Clin Ophthalmol. 2022;16:1837–1846.
- Grippo TM, et al. MicroPulse® Transscleral Laser Therapy – Fluence may explain variability in clinical outcomes: a literature review and analysis. Clin Ophthalmol. 2021;15:2411–2419.
Relevant disclosures
Grippo: Iridex
Toeteberg-Harms: Iridex
Contact
Grippo: tomasgrippo@yahoo.com
Toeteberg-Harms: MarcToeteberg@aol.com