Glaucoma
September 2009
by Tony Realini, M.D.
A new parameter to estimate the rate of visual field loss over time
The goal of glaucoma therapy is to slow or halt progression of the disease, with the ultimate aim of preserving visual function throughout the lifetime of the patient. Progressive glaucomatous changes can occur with both structural and functional assessments of the optic nerve. Presently, there is little consensus among glaucoma specialists regarding the optimal method of detecting progressive changes of either the optic nerve or the visual field. In the absence of accepted methodology for the detection of progression, the identification of patients with progressive glaucoma represents a significant clinical challenge.
At the May 2009 annual meeting of the Association for Research in Vision and Ophthalmology in Ft. Lauderdale, Fla., several research groups investigated the clinical utility of the new parameter—the visual field index (VFI)—to detect progression of the visual field over time.
What is the VFI?
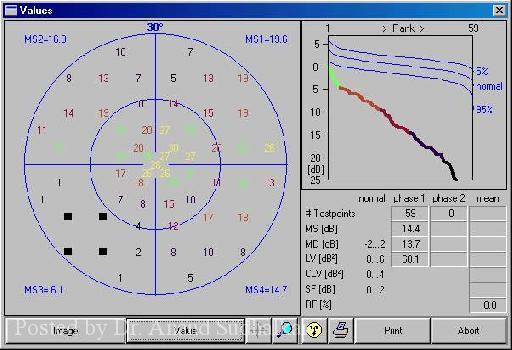
“The VFI is a new global metric that represents the entire visual field as a single percentage of normal,” said Richard Madonna, O.D., SUNY State College of Optometry, New York. “It is based largely on the pattern deviation and weighs central points more than peripheral ones.”
He added, “A full visual field has a VFI of 100% while a perimetrically-blind visual field has a VFI of 0%.”
Correlating VFI with other visual field indices
“Establishing the rate of progression is important in glaucoma,” said Frank May, M.D., Paris. “Knowing the rate of progression provides information on what will happen in the future, and therefore allows us to adapt therapeutic management to preserve visual function in our glaucoma patients.”
There are two strategies for evaluating progression of glaucoma: event-based analysis and rate-based analysis. In event-based analysis, progression is suspected or confirmed based on the occurrence of pre-specified events. In one form of event-based analysis, Glaucoma Progression Analysis (GPA), individual test locations in the visual field are flagged as possibly, likely, or probably progressed from baseline if the retinal sensitivity at that location has changed by an amount expected in fewer than 5% of stable glaucoma patients (for example: P<0.05) on one, two, or three consecutive visual fields, respectively.
Event-based analysis has the disadvantage of providing no information on the rate at which progression is occurring. Rate-based analysis, in contrast, not only identifies the presence of progression but also provides an estimate of the rate at which the visual field is deteriorating.
When followed over time, the VFI provides both rate-based and event-based information. The rate of change of the VFI over time characterizes the rate of progression, while a statistical analysis of this rate generates a p-value indicating whether or not the rate of change is significantly different from zero.
Dr. May and colleagues compared the new VFI parameter to GPA analysis in detecting glaucomatous progression. Their retrospective analysis consisted of eyes at various stages of disease: ocular hypertension and early, moderate, and advanced open-angle glaucoma. “Each subject performed an average of 10 SITA-Standard visual field tests over a mean of 6.5 years,” he said. For each stage, the VFI and GPA2 outputs were compared.
“Among the ocular hypertensive eyes, 100% had a stable VFI and 96% had no ‘possible’ or ‘probable’ progression using GPA2,” Dr. May said. The correlation between VFI and GPA2 in these eyes was 97%.
In the early, moderate, and advanced open-angle glaucoma eyes, stability was established in 88%, 39%, and 33% of eyes by VFI and in 76%, 54%, and 36% of eyes by GPA2. “The correlation of VFI and GPA2 in eyes with glaucoma ranged from 85 to 87%,” he said. Based on his findings, Dr. May said that the VFI appears to be comparable to GPA2 in distinguishing between stable and progressing patients. “However, when the visual field defects are deep and extensive, GPA2 has a diminished capacity to generate progression alert signals,” he cautioned. “In these cases with very advanced defects, VFI appears to be more useful and provides information on progression rates.”
Correlating VFI with structural changes
To determine the relationship between the VFI and the extent of structural damage to the retinal nerve fiber layer, Harmohina Bagga, M.D., and colleagues, University of California, San Diego, conducted a strength of association analysis comparing nerve fiber layer measurements obtained with both the Stratus OCT (Carl Zeiss Meditec, Dublin, Calif.) and the Heidelberg Retina Tomograph (HRTII, Heidelberg Engineering, Vista, Calif.) to three global visual field indices: mean deviation (MD), pattern standard deviation (PSD), and VFI.
In this study, the square of the Pearson correlation coefficient (r2) was used to assess the strength of association between the structural and functional status of the nerve fiber layer (NFL). The r2 parameter, called the coefficient of determination, has values ranging from 0 to 1, with 0 representing no correlation and 1 representing perfect correlation.
Drawing data for this post hoc analysis from two ongoing prospective, longitudinal glaucoma studies, Dr. Bagga found that “the structure-function relationships at one point in time using VFI were comparable to those of MD and PSD.” The coefficients of determination correlating HRT-derived NFL thickness and MD, PSD, and VFI ranged from 0.08 to 0.10, while those correlating OCT-derived NFL thickness and MD, PSD, and VFI ranged from 0.26 to 0.28.
“Despite the fact that all of these coefficients of determination were statistically significantly greater than zero, the strength of association of VFI, MD, and PSD with functional measurements using Stratus OCT and HRTII was uniformly weak,” Dr. Bagga said.
Correlating VFI with global visual function
Dr. Madonna conducted a prospective study to evaluate the association between VFI scores and global visual function using the NEI VFQ-25 Questionnaire.
“The National Eye Institute Visual Function Questionnaire is a validated 25-question measure of visual function that has been shown to be correlated with the degree of visual field loss in glaucoma,” said Dr. Madonna. “The questionnaire provides a global score and has a number of subscales, including general health, general vision, ocular pain, near acuity, distance acuity, social functioning, mental health, role difficulties, dependency, driving, and peripheral vision.”
After performing visual fields and administering the questionnaire to 80 glaucoma patients and suspects, Dr. Madonna said, “We found significant correlation between the VFI and all VFQ subscales except ocular pain and color vision.” He added that the driving subscale was not included in their analysis because “the majority of the subjects with lower VFI scores had already stopped driving.”
VFI was not uniquely correlated to those aspects of visual function, he said. “Statistically significant correlations were also found between VFQ subscales and the other visual field metrics, MD and PSD.”
“Based on our findings, the VFI may have the potential to represent a measure of functional disability in the management of glaucoma,” Dr. Madonna said. However, “our results do not indicate that the VFI is any better correlated with future disability as measured by the NEI VFQ-25 than are the conventional visual field metrics MD and PSD.”
The NEI VFQ-25 is not specific to glaucoma and reflects decreased visual function from any cause, such as cataract. Similarly, MD and PSD are affected by cataract and other ocular pathologies, not specifically by glaucoma. “The VFI is relatively independent of the effects of cataract and other media opacities and thus better reflects localized damage from glaucoma,” said Dr. Bagga.
This distinction between the VFI and the MD and PSD parameters may be important, said Dr. Madonna. “Further evaluation of the VFI in comparison with glaucoma-specific visual function tools may serve to distinguish VFI from MD and PSD as a gauge of glaucoma-related functional disability,” he said.
Editors’ note
Dr. Madonna has no financial interests related to his comments. Drs. May and Bagga did not indicate any financial interests related to their comments.
Contact information
Bagga: harmohina@yahoo.com
Madonna: rmadonna@sunyopt.edu
May: ophtimum@aol.com