For a more recent article on this topic, see “Cataract postop regimens examined.”
Cover Feature: Cataract Surgery Pharmaceutical Corner
April 2007
by Michelle Dalton
EyeWorld Contributing Editor
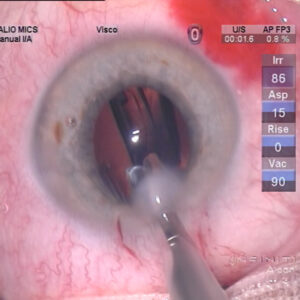
As cataract surgery becomes “gentler,” how will a surgeon’s post-op treatment strategy change?
Ten years ago, a supposition that ocular steroids used in cataract surgery were on the decline would have been laughable. Today, with the advent of cold phacoemulsification, a smaller incision, and more effective nonsteroidal anti-inflammatory drugs (NSAIDs) on the market, the theory is not as radical as once thought. Topical steroids are still needed in today’s uncomplicated cataract surgeries “simply because you can’t predict who is and who isn’t going to have more inflammatory reaction after surgery,” said Stephen S. Lane, M.D., adjunct professor of ophthalmology, University of Minnesota, St. Paul, Minn. Surgeons may perform the same procedure on similar patients with no significant risk factors—one may have minimal or no inflammation post-op; the other may have quite a bit of inflammation, he said. But there are alternatives to using the stronger steroids, Dr. Lane said. “There are steroids available [now]—that I call ‘safe’ steroids. At the head of the class is Lotemax [loteprednol etabonate ophthalmic suspension, Bausch & Lomb, Rochester, N.Y.],” he said. “The efficacy of this particular steroid is very high—almost as strong as prednisolone acetate or phosphate but with far fewer side effects.”
“In cases of more complicated surgery or those that have uveitis or trauma, I find that steroids are imperative to reduce inflammation and improve outcomes,” said Rosa Braga-Mele, M.D., M.Ed., associate professor, University of Toronto, Canada, and director of cataract unit and surgical teaching, Mt. Sinai Hospital, Toronto.
The NSAID effect
Despite the current phaco techniques, “significant inflammation is encountered in a large percentage of eyes following uncomplicated surgery if no medication is used,” said David F. Chang, M.D., clinical professor of ophthalmology, University of California, San Francisco. In the late 1990s, Dr. Chang was an investigator for Surodex, a sustained release steroid delivery system. In the Food and Drug Administration (FDA) trial, there was a placebo control arm that received no medication at all.
“Although some control eyes [in that study] were indeed very quiet in the absence of any anti-inflammatory medication, most patients had significant iridocyclitis, discomfort, and photophobia until a topical steroid was instituted,” Dr. Chang said. Minimizing patient discomfort while suppressing inflammation as rapidly as possible is the key to post-op cataract management, he added. “The synergy of topical steroids and NSAIDs accomplishes these goals and prevents cystoid macular edema [CME]. Even if 80% of patients did well on a topical NSAID alone, I would still routinely use topical steroids to prevent excessive inflammation in the other 20%,” he said.
Samuel Masket, M.D., clinical professor of ophthalmology, Jules Stein Eye Institute, David Geffen School of Medicine, University of California, Los Angeles, conducted a study that looked at post-op change in astigmatism as affected by topical steroids versus topical NSAIDs. (Masket S. Comparison of the effect of topical corticosteroids and nonsteroidals on postoperative corneal astigmatism. J Cataract Refract Surg. 1990 Nov; 16(6):715-8.) “This was before the potent NSAIDs we have today were available,” said Dr. Masket, “In that study, 75% of the patients who were treated with NSAIDs alone did not need a steroid to reduce inflammation. But we couldn’t predict who was going to fall where.”
Dr. Masket has changed his post-op regimen as a result of the “absolute hard evidence” that combining NSAIDs with steroids prevents CME. Dr. Masket now uses a less potent steroid such as Lotemax and typically uses nepafenac as his NSAID of choice.
“NSAIDs are not nearly as potent in their anti-inflammatory effects as steroids, plain and simple,” countered Kevin M. Miller, M.D., Kolokotrones professor of clinical ophthalmology, Jules Stein Eye Institute. “You can’t reasonably treat a cataract patient with NSAIDs alone—too many will develop CME.”
Louis D. “Skip” Nichamin, M.D., Brookville, Penn., said there’s still controversy around the issue. He noted studies that eliminated steroids and used just NSAIDs showed patients did well; other studies have examined weaker steroids (such as Lotemax) that have a better safety profile than prednisolone acetate, and those eyes did well, too. “We don’t have a plethora of prospective studies comparing the NSAIDs to prednisolone acetate,” he said. “We see slightly higher levels of inflammation without using the stronger steroids, but that may be acceptable if there are no complications during surgery,” said Dr. Nichamin. Until a head-to-head comparison between NSAIDs and corticosteroids is performed that involve enough eyes to show statistical significance, Dr. Nichamin will continue to combine the two post-op.
Decreased steroid duration
Dr. Braga-Mele said that by using NSAIDs both pre- and post-op she has been able to effectively use a weaker steroid for a shorter period of time than in previous years, a sentiment echoed by others.
“Using an NSAID adds a protective arm to the inflammatory cascade that a steroid does not inhibit,” Dr. Nichamin said. “Most importantly, this means that NSAIDs help to block CME, which remains one of the last banes of cataract surgery.”
Once he added NSAIDs to his routine treatment regimen, Dr. Nichamin began to experience a noticeable drop in the incidence of CME. His normal routine is to begin the NSAID along with a fourth-generation fluoroquinolone three days prior to surgery. On the day of surgery, a corticosteroid is used every two hours, and then continued four times per day along with the NSAID.
“When combined with a NSAID, tapering patients off of the steroid may begin to take place in two to four weeks instead of a month or two,” he said. In the past, Dr. Lane prescribed prednisolone acetate four times daily for “about four to six weeks post-op.” After adding NSAIDs to his post-op regimen, his dosing changed. He now prescribes loteprednol three times daily for about two to three weeks, or until the 5c bottle runs out,” he said.
The change in prescribing habits is due to three variables that weren’t in play years ago, Dr. Lane said.
“First, you have a safer, gentler surgical procedure. Second, there are newer NSAIDs that work synergistically with steroids. And third, we have very good steroids that although not quite as strong as prednisolone are still very effective, work well in a situation where you don’t need much anti-inflammatory action, and have a much improved safety margin,” he said.
“The only real negative of steroids is intraocular pressure rise,” said Dr. Miller. “If there wasn’t that side effect, no one would reduce the amount of time a patient is on steroids.”
Dr. Miller continues to prescribe a four-week treatment of steroids even when he prescribes NSAIDs because he found eliminating steroid use after just two weeks caused rebound inflammation. “We used to prescribe steroids for six weeks, but now that we’re creating clear corneal incisions, we’ve cut it back to four,” said Dr. Miller, who added that surgeons need to remain vigilant and aggressively treat any side effects. “Ten years ago, I was using prednisolone acetate 1% as a topical steroid of choice, but now I’m using a much less potent one,” Dr. Masket said. “Most physicians tend to discontinue treatment too soon. The scientific evidence suggests the blood aqueous barrier does not reform until about six weeks after surgery.” During the last four weeks of his six-week post-op regimen, Dr. Masket prescribes both NSAIDs and steroids twice daily. Dr. Chang, however, continues to use 1% prednisolone acetate—but at a lower dose.
“The newer NSAIDs are dosed b.i.d. [twice a day] and t.i.d. [three times a day], and I usually prescribe the steroid at this same frequency for the sake of easier compliance,” he said. “Concurrent use of topical NSAIDs generally allows us to stop the steroid drops sooner.”
What the future might hold
Continued advances in pharmacology may lead to more potent NSAIDs that may, in turn, obviate the need for corticosteroids, Dr. Lane suggested. Other advances could lead to even safer steroids or lower dosing than are currently used, he added. “There’s ongoing work with sustained release devices as well—perhaps a steroid that would soak into the lens material and the lens itself might work as a delivery vehicle,” he said.
Dr. Chang said that with the development of more potent steroids and NSAIDs, the possibility of once-daily dosing of both NSAIDs and steroids is not out of reach and that such dosing would help alleviate the patient compliance problem.
“I keep wishing there was a way to combine both in the same bottle,” he said, adding that intraocular sustained release drug delivery systems would be able to eliminate the need to use any topical medications. Those innovations are on the horizon, he noted.
Dr. Nichamin said the future of drug delivery may be “depositing medications intracamerally, either with pellets in the eye or an implant that’s soaked in a cocktail of anti-inflammatory medications.” “Even though we’re using less potent steroids, we cannot forget steroids can—and do—have negative side effects,” Dr. Masket said. “These are potent agents that need to be treated with respect.”
Editor’s note
Dr. Braga-Mele is a consultant for Alcon (Fort Worth, Texas) and Bausch & Lomb (Rochester, N.Y.). Dr. Chang has no financial interests related to his comments. Dr. Lane has a financial interest in Advanced Vision Science (Goleta, Calif.), Alcon, Bausch & Lomb, and other ophthalmic companies. Drs. Masket and Miller are consultants for Alcon. Dr. Nichamin is a medical monitor for Bausch & Lomb.
Contact information
Braga-Mele: (416) 462-0393; rbragamele@rogers.com
Chang: (650) 948-9123; dceye@earthlink.net
Lane: (800) 846-1877; sslane@associatedeyecare.com
Masket: (310) 229-1220; avcweb@aol.com
Miller: (310) 206-9951; kmiller@ucla.edu
Nichamin: (814) 849-6547; ldnichamin@aol.com