Cornea: Changing mindsets
Summer 2025
by Liz Hillman
Editorial Co-Director
For about 7 years, there has been one FDA approved treatment for neurotrophic keratitis (NK): Oxervate (cenergermin-bkbj ophthalmic solution, 0.002%, 20 mcg/mL, Dompe). Before that, there was nothing. Now pharmaceutical options for NK—and persistent corneal epithelial defect (PCED) more generally—in the pipeline number about a half dozen.

Source: John Sheppard, MD
“Oxervate did an amazing job in terms of opening this whole space for the treatment of non-healing ocular surface epithelial defects,” Dr. Farid said. “Since that therapeutic became available, our knowledge in this space has evolved. We’re understanding more about the pathophysiology of the ocular surface intricacies of the interplay between the epithelial cells, the limbal stem cells, the corneal nerves, and this complex interdigitation that creates a smooth corneal surface that’s important for the immunity of the eye as well as vision.”
Dr. Farid said this area has expanded with a lot of other potential mechanisms of action that are being looked at for the management of these ocular surface wounds.
“The interesting thing,” said John Sheppard, MD, “is that with DEWS I, no one mentioned a neurogenic component to dry eye. We like to think that the previous century was the era of tear replacement. The first decade of this century was the decade of inflammation in dry eye and surface disease in general. The second decade was the decade of meibomian gland dysfunction. This decade has become the decade of neurogenic ocular surface disease.”
Dr. Farid and Dr. Sheppard shared their insights and opinions about some of the options in the pipeline for NK and PCED.
But first …
Is NK the only etiology for persistent corneal epithelial defect?
Dr. Farid said the discussion about NK and PCED treatment needs to start with the difference between the two. Dr. Farid said PCED is the larger umbrella definition of many things that can impact corneal healing, and it encompasses neurotrophic keratitis.
“Neurotrophic keratitis is one form of persistent corneal epithelial defect, but there are others. You look at neurotrophic keratitis as a difficulty of the corneal nerves specifically; when you look at persistent corneal epithelial defect, it’s not just about the nerves of the cornea but also the ability of the epithelium to migrate to regenerate the epithelial cells to communicate and interact with each other as well as with stromal fibroblasts and their ability to adhere to the underlying basement membrane of the cornea. Where does the epithelium of the cornea transform into disease of the nerves of the cornea? You need healthy epithelium to release trophic factors to keep the nerves healthy and vice versa; you also need the nerves to release trophic factors to keep the cornea healthy.”
Dr. Sheppard said PCED is “clearly not monolithic in terms of its etiology.” “It’s a multi-factorial situation with many overlapping features,” he said, calling it a significant diagnosis that is actively being pursued. But he called the PCED market “elusive.”
Patients with PCED are “wandering orphans,” and once you find one, you develop a long-term relationship with that patient to help them in their healing journey, he said.
“It’s not like they’re coming in the door all the time, and there are so many companies with high hopes for this,” Dr. Sheppard said. As a cornea specialist, he thinks the space for treatment development is exciting. As an investor, he’s wary. He said he hopes for the best for the companies that are working toward treatments for PCED and NK indications, but he knows getting a product approved and bringing it successfully to the market can be a challenge.
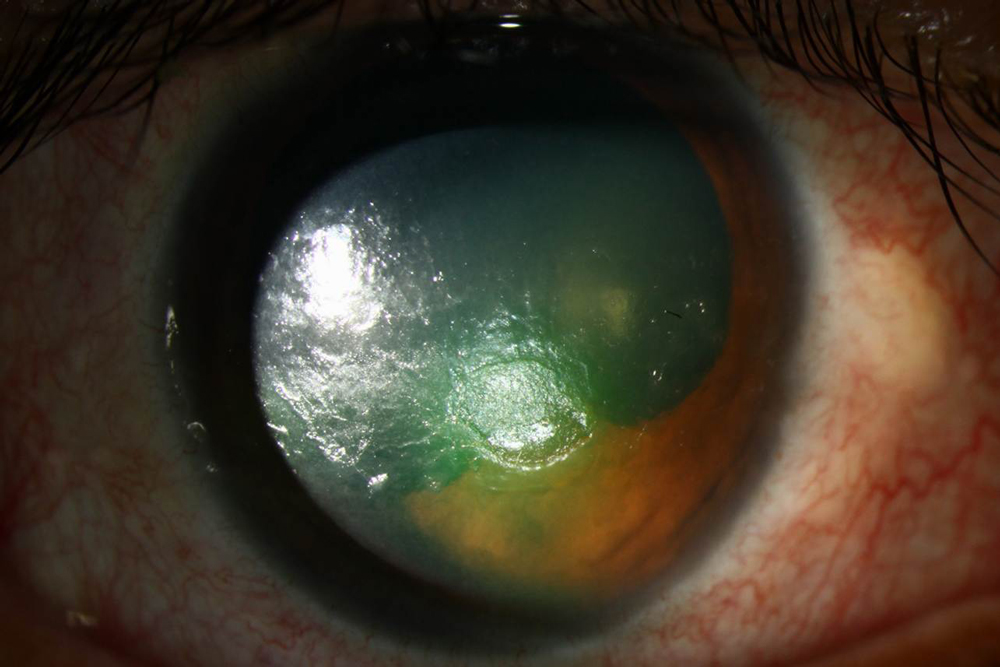
Source: John Sheppard, MD
The ‘Cinderella story’
Dr. Sheppard called Oxervate the “Cinderella story” that motivated other companies to develop their molecules for the indication of PCED and/or NK. “The idea of treating PCED has become more sophisticated in that people are looking for drugs that target a meaningful pathway.”
Oxervate, a recombinant human nerve growth factor, became the first FDA-approved targeted therapy for NK. Dr. Sheppard said it has worked well for these patients, tremendously boosting prescriber awareness of NK, but the expense and prior approvals have been challenges for the drug.
Dr. Farid said Oxervate has been “one of the most impactful therapies for corneal disease” in the last decade, addressing unmet need in regenerating corneal nerves, especially in patients with post-herpetic eye disease and severe diabetes. “It’s the best thing we have right now for a lot of these non-healing neurotrophic ulcers,” she said, but added, “We’ve seen there are areas where it goes beyond the nerves, where there’s limbal stem cell disease, where there’s underlying inflammatory disease, mechanical trauma, where Oxervate may not be 100% effective in these corneas. … I think there is room for therapeutics that offer a broader action to the epithelium and the basement membrane matrix to allow epithelial adhesion, migration, and proliferation.”
Dr. Sheppard said with reasonable patient selectivity, Oxervate can have great success. That being said, patients who are not as severe or who are not appropriate candidates for Oxervate have physicians and pharmaceutical companies “looking for the next echelon of potential success.”

Source: John Sheppard, MD
The PCED, NK pharmaceutical pipeline
What’s great about the pharmaceuticals in the development for PCED and NK, Dr. Farid said, is they all have different mechanisms of action. Some are looking to improve the health of epithelial cells so they can migrate and proliferate better, while others are another human recombinant growth factor that can help with regeneration of nerves/epithelium, and still others are stem cells.
“I think there’s going to be space for all of these therapeutics to work in different types of patients and different etiologies,” Dr. Farid said. “I think some of that is going to need to be worked out in terms of what was the initial inciting problem. Was it an issue with the nerves, was this related to mechanical trauma, was this related to chemical burn of the eye? I think a bit of that is going to get teased out, and we may potentially be able to target different types of etiologies with different medications.”
Here’s a brief look at some of the companies working on a PCED or NK pharmaceutical therapy. (This is not an exhaustive list of every company working on a PCED or NK product.)
Amber Ophthalmics: NEXAGON (lufepirsen ophthalmic gel), an unmodified antisense oligonucleotide, inhibits the protein connexin43, which, according to the company, stops an “exaggerated inflammatory cascade” particularly relevant to chemical burns, and helps restore corneal healing, homeostasis to preserve corneal epithelium, and limbal stem cell function. The drug is currently recruiting patients with PCED for a Phase 2/3 clinical trial.
BRIM Biotechnology: BRM424 is being developed to “[stimulate] the proliferation and differentiation of corneal limbal stem cells to effectively regenerate healthy limbus after extensive limbal layer removal and to speed up the cornea repair process,” according to the company’s website. BRM424 has an Orphan Drug Designation from the FDA for NK and is in a Phase 2 clinical trial. BRIM is also developing BRM423, a synthetic peptide derived from human pigment epithelium-derived factor, targeted to treat severe corneal damage.
Claris Bio: CSB-001 ophthalmic solution 0.1% (oremepermin-α) was in Phase 1/2 clinical trials for patients with Stage 2 or 3 NK. This study began in 2021, and its published planned completion date was within 2024. Oremepermin-α, according to the company, is a five amino acid-deleted variant of hepatocyte growth factor developed by Kringle Pharma with rights to ophthalmic indications licensed to Claris Bio. The mechanism of action augments NGF with potential anti-proptosis, anti-inflammatory, and anti-scarring effects, now under study for corneal defects within 30 days of onset.
Kala Bio: KPI-012, according to the company, has a multifactorial mechanism of action based on human mesenchymal stem cell secretome therapy for the intended treatment of PCED. KPI-012 is in a Phase 2 clinical trial (topline results expected in the second quarter of 2025) and has a Fast-Track Designation from the FDA.
Noveome: ST266 is listed on the company’s website as in a Phase 2 clinical trial. ST266, according to the company, is based on secretome collected from immortalized amnion-derived epithelial cells. This aggregate of more than 500 potentially synergistic proteins may be effective for thermal burns and necrotizing enterocolitis and has been studied in dry eye disease.
RegeneRx: RGN-259 is targeting NK as a thymosin ß4, preservative-free eye drop that promotes cell migration and wound healing and is anti-inflammatory. RGN-259 has an Orphan Drug Designation from the FDA. The company has completed one Phase 3 clinical trial, meeting its primary safety and efficacy endpoint, and is currently conducting two other Phase 3 clinical trials in the U.S.
Dr. Farid thinks that many of the therapies in development will not be a blanket cure for all aspects of PCED or NK but that they each address different components of a disrupted mechanism of the ocular surface. “Down the road, I think we’re going to be able to tease some of that out and figure out what works best and do more targeted medicine,” she said.
‘Epithelial reboot’ procedure vs. pharmaceuticals
Dr. Sheppard said many pipeline pharmaceuticals are intriguing, but he described an “epithelial reboot” procedure that he thinks can, in some cases, accomplish similar results to what some of the pharmaceuticals are aiming for, especially in patients with hereditary or traumatic basement membrane dystrophies.
He said that for these patients, you need to thoroughly remove all of the bad epithelium to give new cells a fresh start to migrate centripetally, heal, and truly adhere to basement membrane. “I’ve had tremendous success, 99% plus, when you remove all the epithelium, polish the basement membrane, and manage them for 3 months, first with an amniotic membrane (which somewhat competes pharmacokinetically with these drugs we’re talking about), then with the serial bandage contact lenses for up to 3 months. They heal, and I never see them for emergencies again.”
Dr. Sheppard said the non-neurotrophic patients can have problems with ring mounted cryopreserved amniotic membrane because they can feel them. However, he said manufacturers have come up with a way to secure the merits of cryopreserved amniotic membrane under a regular bandage contact lens.
Similarly, a retrospective study published earlier this year looked at the use of a decellularized amniotic basement membrane (either single layer or three layer), combined with 24-hour use of an eyelid pressure patch in patients with PCED and reported 100% of cases in the single-layer group and 100% in the three-layer group experiencing corneal staining improvement, suggesting the technique is a “safe and effective approach for healing persistent corneal epithelial defects,” according to the author.1
About the physicians
Marjan Farid, MD
Director of Cornea, Cataract, and Refractive Surgery
Gavin Herbert Eye Institute
University of California, Irvine
Irvine, California
John Sheppard, MD
Professor of Ophthalmology
Eastern Virginia Medical School
Medical Director
Lions Eye Bank of Eastern Virginia
Regional Medical Director
EyeCare Partners
Norfolk, Virginia
Reference
- Linsey K. Use of an eyelid pressure patch concomitantly with a decellularized dehydrated amniotic membrane for ocular surface disease management. Ophthalmol Ther. 2025;14:573–584.
Relevant disclosures
Farid: Kala Bio
Sheppard: Bio-Tissue, Claris Bio, Dompe, Noveome
Contact
Farid: mfarid@hs.uci.edu
Sheppard: jsheppard@cvphealth.com



