Cornea
Summer 2024
by Ellen Stodola
Editorial Co-Director
There are several options for antiviral treatments for HSV. Leela Raju, MD, and Pedram Hamrah, MD, discussed both topical and oral options, when to get patients treated, how quickly the treatment works, and how this can impact the patient in the future.
Dr. Raju said you should incorporate antiviral treatment “from the get-go” if you’re concerned that the patient has a herpes infection. “The best way to treat it is to get them on antivirals as soon as possible,” she said. As to whether you choose topical or oral treatment, Dr. Raju said there are differing opinions on this. Some of the topical options can cause toxicity. “What I find works best for me is that generally trifluridine has been recommended nine times a day, but I do not do it that often. I usually do five times a day, and I taper much faster than prescribed because the idea is to stop the viral replication, which it can do at a lower dose and hopefully you’ll avoid corneal toxicity,” she said.
A lot of people find oral antivirals easier because you don’t have to worry about that. “There is concern about the kidney function when you put them on oral antivirals. You want to make sure you won’t be exacerbating any levels of poor kidney function, but luckily, it’s a very well-tolerated medication,” she said.

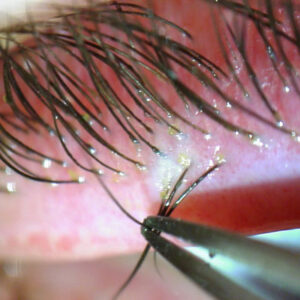
Source: Leela Raju, MD
In addition, there needs to be lubrication of the eye, Dr. Raju said. “We know that this often leads to neurotrophic keratopathy in many patients, so they’re not going to notice how dry their eyes are. People often forget that a great first line for epithelial keratitis is removing the dendrite. Peeling the dendrite off actually reduces the viral shedding.”
When discussing if she would choose topical over oral or vice versa in certain scenarios, Dr. Raju said it’s more about if you think the patient can’t handle the oral. They could have trouble swallowing pills or the frequency could be a problem. If you’re talking about a drop vs. a pill five times a day, sometimes patients want that option, but this is only for epithelial keratitis. With stromal keratitis, you need oral delivery.
The other problem with herpetic keratitis Dr. Raju said is that it often presents so differently in different patients that it may not look like what you’re used to seeing or what’s in a book. “You have to have a high level of suspicion,” she said.
According to Dr. Hamrah, if we see epithelial disease, meaning if there are epithelial dendrites (dendritic epithelial keratitis) that are visualized on exam or geographic epithelial keratitis, typically you need to start these patients right away on antiviral therapy.
In terms of topical treatment, he also mentioned that it can result in epithelial toxicity. The two topical options currently available are trifluridine (which is more toxic) and a ganciclovir gel (less toxic but not always covered by insurance and often requires pre-authorization).
Oral antiviral medication are usually as effective, he said, and they’re typically easier to get covered by insurance, but they may need potential adjustments in the dose depending on the patient’s kidney status.
“I think generally speaking, most practitioners use topical treatments, but others, including myself, prefer oral therapy because of the potential high efficacy, the coverage of insurance, lower chance of toxicity, and better compliance,” Dr. Hamrah said. “The frequency of oral therapy is also less than topical drugs.”
If the patient develops a recurrence, oral treatment is recommended per the Herpetic Eye Disease Study for a year and a half, as this has been shown to decrease the recurrence rate by 70%, but it is not safe to keep patients on topical antivirals for this long. Topical therapy should thus only be used in the acute settings, while oral antivirals can be used chronically, he said.
In very severe cases, Dr. Hamrah said both topical and oral antivirals can be used concurrently. For non-epithelial herpetic flare-ups, some physicians still use oral antivirals as well in order to prevent stromal keratitis or scleritis. Anti-inflammatory therapies can work well, but sometimes the virus may cause persistent inflammation, and unless treated with oral antivirals, the condition does not resolve.
How quickly do the treatments work?
In an acute setting, usually 7–10 days are sufficient in most cases, Dr. Hamrah said. However, he noted that there are always exceptions—for example, if the patient is immunosuppressed. Patients who have atopic disease or autoimmune disease respond differently, so it depends on the comorbidities.
These treatments should also work for patients with persistent herpetic keratitis. But we have seen cases where patients might be resistant to the treatments, Dr. Hamrah said, adding that if they don’t respond, the accuracy of the diagnosis should be reconsidered. Many times, patients with Acanthamoeba keratitis or fungal keratitis can be misdiagnosed as herpetic keratitis.
Dr. Raju said how quickly the treatment works varies between epithelial and stromal keratitis. With epithelial, if you’re doing a topical preparation, you usually see response in a couple of days, which is why she also thinks the course does not have to be as long as originally prescribed for some.
With stromal, it’s not only going to be reducing any viral shedding that’s going on, “it’s also going to reduce the swelling that’s in the cornea, so that often requires topical steroids as well,” Dr. Raju said. “Sometimes it requires a very slow taper on the steroid. You’ll start seeing response in the first week to 2 weeks, but the hard part is how do you make sure they don’t have repeated recurrences. That ends up being much more detrimental to the vision in the long term because the next time they have a recurrence, scarring can form, and that can be what really affects the patient.”
Concerns for future surgery
Dr. Hamrah said antiviral treatment shouldn’t get in the way of other procedures as long as the patient’s disease is under control. If they have a history of herpetic eye disease, they’re at risk for developing it after surgery, he added, noting that a flare-up may occur after refractive surgery.
Dr. Raju said that it is documented that the process after surgery can cause recurrences in herpetic keratitis. “I’ve seen it recur after cataract or cornea surgery, and it can lead to poor healing in corneal surgery,” she said. There are some who think patients with a previous history of herpetic keratitis shouldn’t have refractive surgery, but Dr. Raju thinks it’s possible, knowing how long it’s been and doing prophylaxis. But you should have a long conversation with the patient about this.
For all surgeries, Dr. Raju recommends prophylaxis at least 5 days before and at least a week or longer after. If it’s cornea surgery, she might taper to prophylaxis doses at 1–2 weeks postop but won’t take them off completely. There’s no hard rule on what amount of time is most appropriate. “For a full thickness graft, I might not take them off antiviral or topical steroids, but for cataract surgery, I think you can,” she said. “It also depends if the patient has a scar and you know they’ve had multiple episodes already.”
Dr. Raju again stressed that different patients react differently, so the conversation and explanation to the patient will be very important, particularly why a treatment may be something that they need to do every day. “We’re doing it now so it doesn’t affect their vision later,” she said.
About the physicians
Pedram Hamrah, MD
Professor of Ophthalmology
Vice Chair of Research and Academic Programs
Tufts University School of Medicine
Boston, Massachusetts
Leela Raju, MD
Associate Professor
Department of Ophthalmology
Tulane University
New Orleans, Louisiana
Relevant disclosures
Hamrah: None
Raju: None
Contact
Hamrah: Pedram.Hamrah@tuftsmedicine.org
Raju: rajulv25@gmail.com