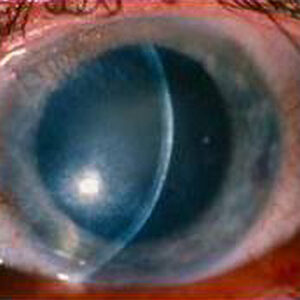
Glaucoma
April 2023
by Liz Hillman
Editorial Co-Director
There is a significant focus on stopping progression of optic nerve damage and subsequent vision loss in glaucoma, but what about patients who have already reached a point of vision loss? What modern visual rehabilitation technologies and services are available to them?

Source: Omar Mohiuddin, OTR/L, CLVT
According to a review article published in the journal Eye in 2022, “relatively little effort has been focused on the practical question of how to maximize visual ability (perform every day, visually-mediated tasks) and minimize the effects of impairment in persons with glaucoma, particularly those with advanced disease.”1 Compared to other medical specialties, the authors of this paper wrote that in ophthalmology, “significant barriers exist in the integration of rehabilitation into glaucoma care,” including visual changes being gradual and fluctuating, the need for multiple conversations with patients, limited time for the primary glaucoma specialist to guide patients in visual rehabilitation and/or limited visual rehabilitation specialists in their area, and difficulty getting patient commitment and/or trust in the visual rehabilitation process.
Mona Kaleem, MD, said that even if patients experience problems with their vision, some don’t bring it up with their care providers. She also said that the physician, in general, doesn’t spend a lot of time talking to patients about their functional deficits, focusing more on IOP, testing, and visual acuity.
She said that asking three questions could help ophthalmologists determine if a patient would benefit from a vision rehab consult: 1) Do you have problems reading? 2) Do you have difficulty walking? 3) Have you fallen in the past 6 months? If they answer yes to any of these, a referral is recommended. “If there is VA of 20/50 or worse, any contrast sensitivity loss, any field loss or scotoma, you should start having conversations with your patients about vision rehab,” Dr. Kaleem said.
“Vision loss is both a spectrum and a journey, with some people experiencing improvements and declines in their vision over time,” said Omar Mohiuddin, OTR/L, CLVT. “When vision loss first begins to impact a person’s ability to do functional tasks a referral to vision rehabilitation services is recommended. Vision rehabilitation specialists will first evaluate to see if glasses maybe help improve vision before visual aids are introduced.”
Traditional aids
Mr. Mohiuddin said that while most people immediately think of magnifiers as visual aids, the first thing he recommends is proper lighting and glare control measures.
“Simple sunglasses or blue light-blocking filters may help reduce glare, and certain color temperature lighting positioned in the right place may help illuminate a task or environment that may allow a person to see their best,” he said. “Common complaints we hear from patients with glaucoma when they notice changes in their vision include increased sensitivity to glare, everything appearing dimmer, or trouble seeing in low light conditions. Later in their vision loss, complaints may include total loss of vision or loss of peripheral vision creating challenges walking around and navigating environments safely.”
Mr. Mohiuddin said he regularly demonstrates conventional and electronic magnifiers, handheld options, and glasses-mounted telescopic devices, as well as specialty filters for glare control and photosensitivity. He said there are a number of non-optical modifications as well, such as using contrasting tape to mark the edges of stairs and no-cut gloves or chopping aids, as a couple of examples.
He said that he does not demonstrate high tech wearables, such as smart glasses and augmented reality headsets, frequently because there is often a learning curve.
“I find that lighting solutions are often the most important thing I can recommend, and while my recommendations are individual, an LED gooseneck task lamp with adjustable brightness and color temperature and a Lil Larry flashlight are versatile tools that help many people with low vision see to complete different tasks,” Mr. Mohiuddin said.
From a contrast standpoint, Dr. Kaleem said making things brighter can be helpful, as can something as simple as switching the background setting on a phone, making it have a dark background with white text instead of white background with black text.
Bathrooms, Dr. Kaleem said, are often a location for falls, in part due to contrast issues. Many bathrooms have white tubs, white floors, and white sinks, making it difficult for people with contrast sensitivity issues. She recommends using high contrast, bright colors for bathmats on the floor near the step for the tub.
Smart technology solutions
Mr. Mohiuddin said that while the range of available assistive technologies has come a long way in the last few decades to help the visually impaired, the greatest difference has been the introduction of smartphones. “Our smartphones are capable of not only taking calls and photos but come equipped with digital assistants to help tell the time, weather, compose text messages through dictation, and accessibility features, such as voiceover, and may allow users to access emails and information on the web and different apps,” he said.
Mr. Mohiuddin said there are apps that now use machine learning and AI that can help users identify objects, barcodes, and read print materials with text-to-speech (optical character reading) capabilities.
“As technology improves and things become lighter weight, less conspicuous, and more affordable, that should help with the adoption and use of devices,” he said. “I find that my patients are more open to adopting and using mainstream technologies, such as smartphones and tablets, rather than proprietary low vision devices as they are more readily available and easier to learn to operate.
No one size fits all
While new technologies are always rolling out, Mr. Mohiuddin cautioned that no technology is one size fits all.
“Not every new aid is going to help everyone, as it depends on their familiarity with technology, their level of vision, and what goals or tasks they are looking to accomplish,” he said. “When recommending aids and technologies, it’s important to understand that it’s often the low tech solutions that are easiest to adopt, and it depends on the individual and what tools they are most comfortable with learning to use and adopting to help do what it is they need to do.”
Jullia Rosdahl, MD, PhD, also spoke about how personalized visual aid recommendations need to be. She stressed early referrals to vision rehabilitation services. Dr. Rosdahl offered a few simple helpful elements for patients depending on their stage of vision.
For patients at an earlier stage of vision loss, she said it’s helpful for glasses prescriptions to be kept up to date, with lined bifocals or separate single-vision glasses being used instead of progressive lenses. Tints can be used to reduce glare and improve contrast, and attention should be paid to ocular surface optimization. Dr. Rosdahl said task lighting at this stage can be useful.
For patients with more advanced vision loss, especially if the vision loss is in the inferior visual fields where falls could be more of an issue, Dr. Rosdahl said a walking stick might be needed, and it’s important for the physician to review strategies for the patient to move their head and neck instead of just their eyes when walking around.
Dr. Rosdahl, Dr. Kaleem, and Mr. Mohiuddin mentioned the resources on Hadley.edu, which is a website with learning opportunities for patients dealing with vision loss or blindness. Topics on the website cover daily living, technology, adjusting to vision loss, working, and more.
About the sources
Mona Kaleem, MD
Associate Professor of Ophthalmology
Wilmer Eye Institute
Johns Hopkins University
Baltimore, Maryland
Omar Mohiuddin, OTR/L, CLVT
Occupational Therapist
Duke Eye Center
Duke University
Durham, North Carolina
Jullia Rosdahl, MD, PhD
Associate Professor of Ophthalmology
Duke Eye Center
Duke University
Durham, North Carolina
Reference
- Deemer AD, et al. Approaching rehabilitation in patients with advanced glaucoma. Eye. 2022. Online ahead of print.
Relevant disclosures
Kaleem: None
Mohiuddin: None
Rosdahl: None
Contact
Kaleem: mkaleem1@jhmi.edu
Mohiuddin: omar.mohiuddin@duke.edu
Rosdahl: jullia.rosdahl@duke.edu