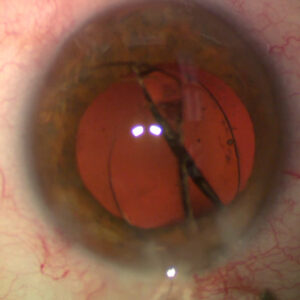
Cataract
July 2021
by Liz Hillman
Editorial Co-Director
When patients see Darrell White, MD, for a cataract evaluation, they all get on the same train, what he calls the refractive cataract train. Dr. White uses this analogy to describe the journey of patients as they seek out a toric and/or presbyopia-correcting IOL.
There are stops along this ride where patients get off the train, either for their own reasons or at the recommendation of the physician.
“In our practice, … we are committed to the premium channel, specifically presbyopia-correcting IOLs,” Dr. White said. “We go in under the assumption that every patient who is in the office for a cataract evaluation is a candidate for a presbyopia-correcting intraocular lens until either we say they’re not or they say they’re not.”
Stop #1: Diagnostic testing and assessment
At this stage, as Dr. White put it, he’s looking for reasons to not offer a presbyopia-correcting IOL.
Every patient in Dr. White’s office gets a macular OCT, and anyone with significant macular pathology gets off the train. Alice Epitropoulos, MD, and Dee Stephenson, MD, also said macular OCT is a must for premium IOL candidates.
They also mentioned topography.
“You don’t want to use these premium IOLs in patients with irregular astigmatism or keratoconus,” Dr. Epitropoulos said, emphasizing later the importance of consistent biometry measurements.
Inconsistent measurements could signal an ocular surface issue. In 2015, Dr. Epitropoulos coauthored a paper that showed patients with hyperosmolarity had significant variability in their average Ks and anterior corneal astigmatism, resulting in differences in IOL power calculations.1
“You have to treat the dry eye. It’s astonishing to me that there are some well-regarded training programs where the attendings don’t, and you have young surgeons coming out who are trained but they’re not emphasizing treating the ocular surface beforehand,” Dr. White said. “You’ll have a meaningful problem at least a third of the time, and you can’t do that in an area where the public relations part is so important.”
Dr. Stephenson said every patient she sees gets homework, which includes using hypochlorous acid lid scrubs, artificial tears, cyclosporine, and/or a topical steroid before they have diagnostic testing performed and measurements taken.
Both Dr. White and Dr. Epitropoulos discussed the importance of identifying the angle kappa and chord mu to ensure optimal IOL centration to achieve maximum optical performance and minimize the risk of dysphotopsia or “waxy vision.”
“We use the IOLMaster 700 [Carl Zeiss Meditec] and like to see the angle kappa (chord length) less than 0.5 mm for patients considering a presbyopia-correcting IOL. A large angle kappa is a relative contraindication for a multifocal lens due to a decrease in optical performance and high percentage of subjective complaints in these patients,” Dr. Epitropoulos said.
As Dr. White put it, most presbyopia-correcting IOLs have bullseye designs. With that design, if the lens doesn’t line up with the optical center of the patient’s visual system, aberrations and reduced contrast sensitivity could be induced, he said.
“It’s like the optic and the focal lens of a telescope. If you don’t have the optic and the optical element lined up, you won’t be able to see with a telescope. The same thing in many ways occurs with a true presbyopia-correcting IOL,” Dr. White said.
Stop #2: Patient personality and expectations
While there are quite a few presbyopia-correcting IOL options in the U.S. market, multifocal, trifocal, extended depth of focus (EDOF), and newer options like Eyhance (Johnson & Johnson Vision) and Vivity (Alcon), patient personality remains an important factor in the selection process.
“We want to make sure that our ever-improving but still imperfect presbyopia-correcting technology is going to be able to match the expectations of our patients,” Dr. White said. “Because of that, you can’t do it without learning a bit about who they are, what makes them tick, what’s important to them, and how flexible are they,” Dr. White said. “You can’t take someone whose happiness in life is driven by how well they see at distance and put a presbyopia-correcting IOL in them that is going to have any negative effect on their distance vision. You still have to do a tiny amount of psychological profiling.”
Dr. Epitropoulos said patients fill out an online questionnaire through software called MDbackline prior to seeing her, which gives her an idea of what their expectations are for their vision.
“Patients who come in wanting to see ‘perfect’ at all distances including good quality vision at night should raise a red flag, highlighting the importance of discussing realistic expectations with patients,” she said. “For doctors new to presbyopia-correcting IOLs, start with cataract patients who are interested in reducing dependence on corrective lenses, have realistic expectations, and have an otherwise healthy eye.”
Dr. Epitropoulos said having family listen in during IOL selection discussions can be helpful.
“It’s important to spend extra chair time with these patients, being transparent and reviewing the pluses, minuses, pearls, and pitfalls of this technology,” she said.
Dr. Stephenson said setting patient expectations is an art; you want to under promise and over deliver. “It’s never going to be what God gave us—a pristine eye that doesn’t have a cataract. You have to be honest with them about their own anatomy. We’re good at hitting our mark, but we don’t have a crystal ball [to see] how the patient heals, how soon they will get fibrosis, where the lens will sit in the eye.”
Closing points
Dr. Stephenson said it’s important to understand how presbyopia-correcting lenses work in your hands. She, a long-time Crystalens and Trulign (Bausch + Lomb) user, said she understands it takes special patient buy-in for the time it will take to optimize outcomes. “These are great for post-refractive patients because they are aspheric IOLs so have zero aberrations,” she said. Dr. Stephenson said she had a harder time gaining success with traditional multifocals and EDOF because of how they split the light but has brought the Vivity and PanOptix trifocal (Alcon) into her practice with success.
“There are quite a few options but whatever technology you use, you’ve got to know how it works in your hands,” she said.
On a similar vein, Dr. Epitropoulos said it’s important to track results and personalize your A constant. She also noted that dissatisfied patients with residual refractive error should be offered a LASIK touch-up, LRI, or IOL exchange when appropriate; patients need to be informed of this possibility preop.
“If someone comes in and they’re unhappy, it’s important to look at the whole picture. Treat any organic problems before telling them they need to get used to it. Let them know you’re going to do what you can to resolve these issues. Pay attention to the ocular surface. Evaluate for macular edema or posterior capsule haze. Treat residual refractive error,” she said.
Dr. White cautioned against considering an EDOF as a bypass for eyes with some issues.
“If you have an eye where there is large angle kappa, an eye with an epiretinal membrane, an eye with a certain amount of macular degeneration, the extended depth of focus lenses are going to allow those patients to still get an anticipated benefit from putting the lens in. The reality is they’re much more forgiving by a full order of magnitude, but they don’t fix the epiretinal membrane. They don’t fix the corneal irregularities.
“While I am absolutely a fan and will switch someone from a bifocal or trifocal to EDOF when I’m concerned about the visual health of the eye, I’m always careful not to get so enthusiastic that I’m putting it in patients who should have a basic IOL or maybe a toric IOL,” he said. “The EDOF lenses are much more forgiving, but they don’t resolve the existing problems the eye has coming into the office.”
About the physicians
Alice Epitropoulos, MD
Ophthalmic Surgeons and Consultants of Ohio
Columbus, Ohio
Dee Stephenson, MD, FACS
Stephenson Eye Associates
Venice, Florida
Darrell White, MD
SkyVision Centers
Westlake, Ohio
Reference
- Epitropoulos A, et al. Effect of tear osmolarity on repeatability of keratometry for cataract surgery planning. J Cataract Refract Surg. 2015;41:1672–1677.
Relevant disclosures
Epitropoulos: Alcon, Bausch + Lomb, Johnson & Johnson Vision
Stephenson: Alcon, Bausch + Lomb
White: None
Contact
Epitropoulos: eyesmd33@gmail.com
Stephenson: eyedrdee@aol.com
White: dwhite2@skyvisioncenters.com