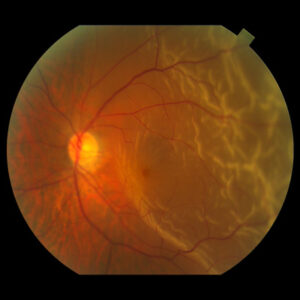
Glaucoma
September 2021
by Ellen Stodola
Editorial Co-Director
ASCRS co-sponsored a session at the 2021 virtual meeting of the American Glaucoma Society (AGS) that covered topics relating to patients with controlled glaucoma but visually significant cataracts.
John Berdahl, MD, discussed options for refractive IOLs in glaucoma patients. He asked two questions: Do patients with glaucoma deserve to have astigmatism corrected? Do they deserve to have presbyopia corrected? The answer is, of course, yes. These patients should be informed of premium IOLs as an option, in addition to glasses or contact lenses, Dr. Berdahl said. When looking at the options, it’s about patient goals, considering what the patient is hoping for and how they want to use their eyes. You have to make sure it’s the right eye and the right technology, he added.
Premium IOLs can be options for patients with milder forms of glaucoma as opposed to severe glaucoma eyes, Dr. Berdahl clarified.
There is an array of astigmatism-correcting and presbyopia-correcting IOLs available, Dr. Berdahl said, highlighting the Light Adjustable Lens (RxSight) and Vivity (Alcon).
He also discussed considerations for glaucoma patients: contrast sensitivity, pupil size, refractive stability, and potential for glaucoma progression.
Newer presbyopia-correcting IOLs cause little decrease in contrast sensitivity compared to older options. He mentioned the PanOptix trifocal (Alcon), which has very little decrease in contrast sensitivity; the Symfony (Johnson & Johnson Vision), which has minor loss in contrast sensitivity; and the Vivity, which has some decline in contrast sensitivity but likely not clinically significant. Monovision has a much higher decrease in contrast sensitivity because of the blur induced by monovision eyes, Dr. Berdahl said.
Pupil size matters most at the extremes, Dr. Berdahl noted. Pupil size doesn’t matter as much with newer generation lenses, he added, but it does matter with the Light Adjustable Lens.
In terms of refractive stability, Dr. Berdahl stressed the importance of a well-centered IOL, symmetric capsulotomy, stable zonular support, and a healthy ocular surface.
If you think the patient will progress despite your best efforts, Dr. Berdahl said that a presbyopia-correcting lens isn’t the right option, and it’s better to correct with glasses.
When considering which option he would want for himself, Dr. Berdahl said if he had mild glaucoma, he’d choose a multifocal IOL. If he had moderate glaucoma, he would likely choose an extended depth of focus lens in combination with a MIGS procedure.
Davinder Grover, MD, presented “No Medications: Cataract Surgery Combined with MIGS.”
When it comes to angle surgery in POAG, Dr. Grover said to use the desired degree of IOP lowering to help choose surgery. For example, in a patient with mild POAG/OHTN controlled on one medication, you might want to consider an iStent (Glaukos) or Hydrus (Ivantis). For a patient with mild POAG/OHTN controlled on two to three medications or moderate POAG on one to two medications, you might consider a Hydrus or goniotomy. For a patient with mild POAG/OHTN controlled on three or more medications or moderate POAG on two or more medications, Dr. Grover suggested Hydrus/goniotomy or a GATT.
For a patient with moderate to advanced disease on several medications, Dr. Grover said he wants to get the “biggest bang for my buck.” He will consider GATT if there was uncomplicated phaco, the patient has normal angle anatomy, and the patient doesn’t have severe disease. He will consider XEN (Allergan) if the anatomy is favorable, if the patient has moderate to advanced disease, if the patient is not able to tolerate many drops, and if the patient’s lifestyle is compatible with subconjunctival filtration.
Another factor to consider when looking at surgical options is the patient’s use of blood thinners. He will avoid GATT in patients who can’t be taken off blood thinners or who have to restart use quickly. He would consider iStent or Hydrus instead, depending on the degree of IOP lowering needed. He also said to consider XEN if the patient needs significant IOP lowering.
If the patient has had a prior tube shunt, Dr. Grover said that cilioablation works extremely well. He recommended CPC or ECP.
Dr. Grover also mentioned angle closure disease, secondary OAG, and the health of the cornea as important factors to consider. For those with angle closure disease, he recommended phaco alone or possibly phaco and goniotomy, depending on the IOP and stage of the disease. For those with secondary OAG, Dr. Grover said these patients tend to do better with goniotomy or ab interno trabeculotomy. He also noted that if the patient has endothelial dysfunction and may need some form of corneal replacement, you may want to consider a tube shunt.
For patients with “real” disease who are not able to use drops appropriately, Dr. Grover said he considers subconjunctival MIGS to maximize the chance of a lower IOP, or he may consider phaco/Hydrus or phaco/goniotomy first, with a possible standalone XEN at a later time.
It’s very important to manage patient expectations, Dr. Grover said. In general, the greater the IOP lowering, the greater the risk of surgery. The main goal of MIGS in most cases of moderate to advanced glaucoma, Dr. Grover said, is to decrease the dependence on drops. He rarely promises to get a patient off all drops.
Tak Yee Tania Tai, MD, presented on cataract surgery in patients with primary angle closure glaucoma.
When considering cataract extraction in patients with shallow anterior chamber, Dr. Tai said that a good preoperative evaluation should be performed, assessing for zonular dehiscence and secondary causes of shallow AC. Gonioscopy is also useful for determining if any angle procedure should be done, she said. Endothelial cell count is helpful for surgical planning.
Even without other preexisting factors, operating in the limited space of a shallow AC is challenging, she said. There is increased risk of endothelial compromise and Descemet’s detachment. Difficulty maintaining a deep AC may allow the lens to move forward, and the posterior capsule may be harder to avoid. Aqueous misdirection and suprachoroidal hemorrhage may also be more common.
Dr. Tai said it’s important to have a game plan for these cases. Her five steps include:
- Control the pressure. This starts preoperatively with topical and oral medications. Make sure the speculum is not tight or resting on the eyeball.
- Make the patient comfortable. Don’t be stingy on anesthesia.
- Deepen the chamber (but not too much). You only need a few seconds to deepen.
- Take advantage of technology. Dr. Tai suggested using the femtosecond laser to assist.
- Stay in the bag. Try not to do supracapsular cataract extraction in a shallow AC.
Shakeel Shareef, MD, discussed cataract surgery in patients with pseudoexfoliation. He said to assume all patients have pseudoexfoliation, noting that it might not be evident during an office exam and might come up for the first time in the OR.
Some of the preoperative signs of zonulopathy include asymmetry of the anterior chamber and angle depth, lens subluxation, phacodonesis, iridodonesis, and poor dilation, among others.
“We can decrease the risk of late subluxation by taking steps to respect the zonules intraoperatively,” Dr. Shareef said.
He said that it’s important to minimize side-to-side and up-and-down movements, maintain a stable anterior chamber, perform careful hydrodissection/delineation, and perform tangential phaco and I/A vs. radial forces.
Dr. Shareef also discussed the possibility for a small pupil in these cases and said it’s important to enlarge to gain access. This can be done with cohesive viscoelastic or with mechanical options. He added that it’s “vital to create an optimal anterior capsulorhexis.” The optimal size is about 5–6 mm; too small of a rhexis could lead to damage to the zonules during lens rotation. He added that hydrodissection/hydrodelineation is an essential step for separating the lens from the capsule zonular complex.
When sculpting, don’t push. “Let the phaco handpiece lead you, like a dog pulling his owner on a leash” to avoid stress on the zonules, Dr. Shareef said.
He also gave tips for maintaining a stable anterior chamber, especially when transitioning from phaco to I/A and from I/A to lens implantation. Before pulling out the phaco handpiece, inject balanced salt solution simultaneously while turning off the continuous irrigation, and gently pull out the phaco handpiece. Prior to removing the I/A handpiece, turn off continuous irrigation while simultaneously injecting viscoelastic into the capsular bag, then remove the I/A handpiece.
Dr. Shareef highlighted the role of capsular tension rings, which help with centration with less than 3 clock hours of zonulopathy. But he said they do not prevent late lens subluxation or capsular bag contraction (phimosis).
Erin Boese, MD, discussed cataract surgery in patients with an over filtering trabeculectomy. In cases of an over filtering trabeculectomy, Dr. Boese said preoperative planning for cataract surgery is an important step, with some questions to ask.
First, how long has your patient been hypotonus? If it has been more than 6 months to a year, they may have some irreversible components to the hypotony.
Second, how much IOP increase do you need? You have to decide if you should fix the over filtration before, during, or after cataract surgery. With significant hypotony, Dr. Boese suggested addressing it prior to cataract surgery.
One reason has to do with IOL calculations. With an increasing IOP, the axial length may increase, leading to myopic surprise, Dr. Boese said.
She added that keratometry readings may also shift significantly, so be wary of placing toric lenses.
There are a number of techniques to increase the IOP depending on how much increase you need, including surgical revision, fewer postop steroids with cataract surgery, and a blood patch.
Surgical revision of the trabeculectomy should be addressed before cataract surgery. With revision, you are looking to significantly increase the IOP by slowing down flow through the scleral flap by replacing the interrupted nylon flap sutures. If it’s an old trabeculectomy, you may need to use additional techniques, she added.
Reducing postop steroids following cataract surgery is an easy technique, Dr. Boese said. Post-trabeculectomy phacoemulsification causes small blebs and increased IOP. When she’s trying to keep a bleb working, Dr. Boese counteracts with frequent steroids. However, if she’s looking to increase the IOP in the case of an over filtering trabeculectomy, she will use fewer or no postoperative steroids to use the inflammation from cataract surgery to promote scarring.
The blood patch option is another nice tool, Dr. Boese said. With this technique, the patient’s blood is drawn and immediately used to inject into the bleb using a 27-gauge needle. It’s easy and quickly done in the clinic, but physicians should expect a small IOP increase.
Dr. Boese mentioned several intraoperative considerations for cataract surgery in an over filtering bleb, specifically lowering the bottle height and being careful not to nick the conjunctiva with the clear corneal incision. She doesn’t find that fluidics change much with a mature bleb.
Wrapping up the presentations, Arsham Sheybani, MD, spoke about new surgical technology on the horizon.
He mentioned treatment to the trabecular meshwork, highlighting excimer laser trabeculostomy (ELT). This is non-thermal laser removal of TM. There is less overall tissue removal than goniotomy, and it does not create a flap of TM, he said.
Dr. Sheybani discussed iDose (Glaukos), a small titanium implant with a reservoir of travoprost that is inserted into the trabecular meshwork through a clear corneal incision. It involves travoprost elution at two different rates.
In the suprachoroidal space, Dr. Sheybani mentioned the iStent Supra (Glaukos), which has a titanium sleeve. While similar to other suprachoroidal devices, he said there are differences in material and flexibility. He also mentioned the MINIject (iSTAR Medical), which has a porous silicone material, not as long as prior suprachoroidal devices and very flexible. The green ring on the device helps with ideal implantation, he added.
About the physicians
John Berdahl, MD
Vance Thompson Vision
Sioux Falls, South Dakota
Erin Boese, MD
Clinical Assistant Professor of Ophthalmology and Visual Sciences
University of Iowa
Iowa City, Iowa
Davinder Grover, MD, MPH
Attending Surgeon and Clinician
Glaucoma Associates of Texas
Dallas, Texas
Shakeel Shareef, MD
Professor
Case Western Reserve University School of Medicine
Cleveland, Ohio
Arsham Sheybani, MD
Associate Professor of Ophthalmology and Visual Sciences
Washington University in St. Louis
St. Louis, Missouri
Tak Yee Tania Tai, MD
Associate Professor of Ophthalmology
New York Eye and Ear Infirmary of Mount Sinai
New York, New York
Relevant disclosures
Berdahl: Alcon, Allergan, Carl Zeiss Meditec, Glaukos, Johnson & Johnson Vision, New World Medical
Boese: None
Grover: Aerie, Allergan, New World Medical, Santen
Shareef: None
Sheybani: Alcon, Allergan, Ivantis, New World Medical, Santen
Tai: None
Contact
Berdahl: john.berdahl@vancethompsonvision.com
Boese: erin-boese@uiowa.edu
Grover: dgrover@glaucomaassociates.com
Shareef: shklshrf@gmail.com
Sheybani: arsham.sheybani@gmail.com
Tai: ttai@nyee.edu